The Impact of COVID-19 on Surgical Education: A Monocentric Survey of Residents Training in Surgical Specialties
Nicolas Tasse*, Etienne Auger-Dufour
Department of Surgery, Université Laval, Canada
*Corresponding Author: Nicolas Tasse, Department of Surgery, Université Laval, Canada
Received: 25 November 2021; Accepted: 06 December 2021; Published: 04 January 2022
Article Information
Citation:
Nicolas Tasse, Etienne Auger-Dufour. The Impact of COVID-19 on Surgical Education: A Monocentric Survey of Residents Training in Surgical Specialties. Journal of Surgery and Research 5 (2022): 1-9.
View / Download Pdf Share at FacebookAbstract
Background
This study aims to identify the effects of the COVID-19 on surgical resident education at University Laval during first wave of the pandemic of spring 2020.
Methods
We conducted a web-based survey study to all residents training within one of the ten surgical specialties at University Laval, Quebec City. The survey focused on clinical teaching hours, appreciation of activities and novelties experienced and the impacts of virtual teaching. Descriptive statistical analysis was performed to summarize the data.
Results
There were 48 surgical residents who responded to our survey. There were participants from ten specialties. During the pandemic the mean number of weekly teaching hours dropped from 4.31 to 3.69 hours. The most appreciated activity was teaching sessions lead by a staff surgeon. More than 80% of respondents reported having partaken in other activities at some time during an online class while over 70% expressed retaining less when material was taught online rather than in person.
Conclusion
Our survey provides insight for surgical programs to improve resident teaching and illustrates the necessity to optimize teaching schedules rapidly in times of pandemic. Even though the appreciation of virtual learning seems unsatisfactory by certain residents, trainees still require and appreciate teaching by their mentors.
Keywords
<p>Surgery, Medical education, Survey, Resident, COVID-19</p>
Article Details
Background
The World Health Organization (WHO) officially declared the SARS-CoV2 global pandemic in spring of 2020 [1]. The coronavirus disease 2019 (COVID-19) has impacted and destabilized surgical residencies notably with reduced operating time and diminished surgical exposure across all fields [2,3]. During peak outbreaks, limiting the numbers of residents on medical wards resulted in reduced teaching opportunities and significant restructuring [4]. These containment measures have had important ramifications on the training of future surgeons [5]. This situation was not different at University Laval in Québec City (Canada). Residents throughout all surgical specialties experienced important decreases in operating room time leading to diminished clinical exposure from the alterations of usual operations and changes of available humans and material resources. During spring of 2020, the university policy at our institution recommended that resident numbers in hospitals be minimized to reduce contact as required by public health recommendations [6]. This unpreceded event required resident trainees and program directors to restructure the delivery of medical education. Many surgical curriculums have moved since then to complete online platforms to prevent gatherings [7]. The impact of these modifications and repercussions is still ongoing. To learn more about how the pandemic is affecting resident training, we aim to utilize a survey to gain greater insight on resident perspectives regarding clinical teaching at our center.
2. Materials and Methods
2.1 Survey development and distribution
An anonymous 17-question multiple choice and short answer survey was developed using RedCaps, an online survey platform. All surgical residents training during spring 2020 at Laval University were invited to participate. Excluded residents were those on sick leave or partaking in time off clinical duties for research. A link to the survey was emailed to all 85 surgical specialty residents. The emails of residents were obtained through respective postgraduate medical education secretaries. Reminder emails to encourage participation were distributed weekly for a period of 4 weeks. The survey questions were developed and drafted in French. The questions were tested to ensure clarity and consistent interpretation with 4 junior residents who did not partake in final survey. The survey was then adjusted after incorporating feedback. Surveyed period occurred in February 2021. Prior to completing the survey, an informed consent was obtained. The survey questioned resident demographics, clinical teaching hours, appreciation of activities and novelties experienced as well as views of online teaching during the period of the first wave pandemic in spring 2020. Demographic information included clinical post graduate year (PGY), training program type and gender. Changes in clinical and operative activities during COVID period were assessed as well as estimated number of teaching hours before the studied period. Residents were asked to list their three most appreciated teaching activities as well as a least valued activity. Each listed activity was graded according to its listed position. Three points were given for first ranking activities, two for second and one for third position. Activities were grouped into categories. The categories included were: (1) formal teaching activities lead by staff surgeon, (2) teaching sessions lead by senior residents, (3) oral mock exams, (4) morbidity and mortality (M&M) rounds, (4) journal clubs, (5) ultrasound courses (6) tumor boards. They were also required to list any new activities developed by their program during this period. Finally, we assessed the residents’ opinions of online virtual teaching. The detailed survey is found in appendix 1. Descriptive statistical analysis was performed to summarize the data.
2.2 Outcomes measured
The primary outcome was to determine which weekly activities were most appreciated by residents during this period and list new teaching activities/strategies that could be of interest to implement during times of pandemic. Secondary outcomes were to: (1) evaluate the impact of reduced clinical activities on teaching hours prior and during COVID-19 pandemic and (2) obtain the opinions of residents regarding virtual teaching.
3. Results
3.1 Resident information
Forty-eight surgical specialty residents completed the survey. Global participation was estimated at 56%. At least one respondent from each of the ten surgical programs at our institution participated in the survey. Most respondents were residents from general surgery (35%), obstetrics and gynecology (17%) and urology (13%). There was a relatively even distribution of respondents across PGY (between 8 and 12 respondents per year). The gender of respondents was equal (50%) within the group. Table 1 highlights the described demographics of respondents.
|
Q1. Current year of clinical training |
|
|
PGY1 |
19% |
|
PGY2 |
19% |
|
PGY3 |
25% |
|
PGY4 |
20% |
|
PGY5-6 |
17% |
|
Q2. Gender |
|
|
Male |
50% |
|
Female |
50% |
|
Not specified |
0% |
|
Q3. Training program |
|
|
Cardiac surgery |
4% |
|
General surgery |
35% |
|
Plastic surgery |
4% |
|
Orthopedic surgery |
8% |
|
Vascular surgery |
2% |
|
Obstetrics and Gynecology |
17% |
|
Neurosurgery |
4% |
|
Ophthalmology |
2% |
|
Oto-rhino-laryngology |
11% |
|
Urology |
13% |
Table 1: Resident demographics (n =48)
3.2 Surgical training and teaching hours
Respondents answered with a majority of 92% a reduction of clinical and operative activities during the pandemic first wave. None noted an increase. The reminder 8% noted no change. Teaching activities were reported to have increased according to 38% of respondents while 20% experienced no change and 42% stated having experienced a decrease in teaching opportunities. When asked to estimate the weekly number of hours of teaching prior to the pandemic the mean number of reported hours was of 4.31 hours (SD 1.57). During the pandemic the mean dropped to 3.69 hours (SD 2.95). Residents were asked to include all formal or informal teaching activities when estimating the weekly teaching hours. Figures 1 and 2 illustrate the differences between both time periods. Eleven respondents (23%) answered having received no clinical teaching during the pandemic first wave.
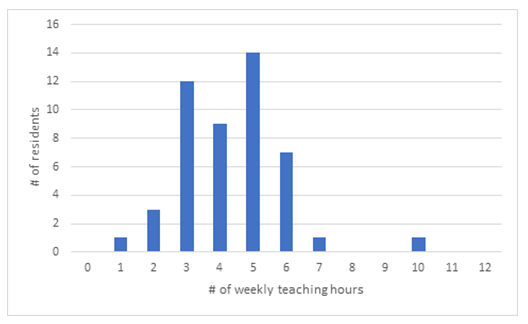
Figure 1: Average teaching hours prior to COVID 19 pandemic according to surgical residents
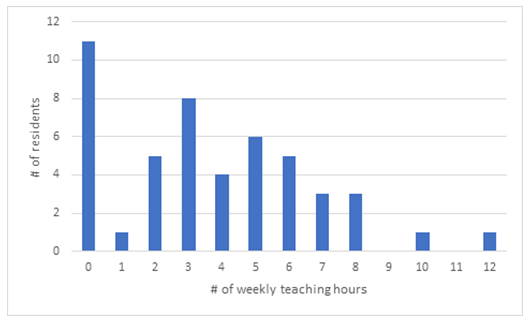
Figure 2: Average teaching hours during COVID 19 pandemic according to surgical residents
3.3 Activities and novelties
Respondents were asked to list their top three most appreciated teaching activities during the first wave. The final count established that the most appreciated activities were (1) formal teaching lectures lead by staff surgeon followed by (2) teaching activities lead by senior residents and (3) oral mock exams. The least appreciated activity was journal clubs. No new teaching activities other than a transition to online platforms were reported by respondents. Over 80% of respondents acknowledge that clinical teaching sessions should be obligatory time off clinical duties even during times of pandemic.
3.4 Virtual class appreciation
Over 80% of recorded teaching activities with this survey were reported being conducted online. The importance of social interactions during previously in
person classes were considered important by all but one respondent. More than half of respondents reported learning opportunities to be limited with the use of online platforms. Most participants disagreed that online teaching sessions are more interactive than in person classes and disagreed that didactic online session are preferable to in person classes. When respondents were questioned if they ever partook in other activities at some time during an online class, only 15% responded “no”. Finally, respondents with a majority disagreed to the statement that the material taught during online classes are better retained than in person classes. A detailed breakdown of the results can be found in table 2.
|
Q12. Importance of social interaction during in person classes |
|
|
Strongly agree |
69% |
|
Agree |
29% |
|
Neutral |
2% |
|
Disagree |
0% |
|
Strongly disagree |
0% |
|
Q13. Learning opportunities limited with the use of online platforms |
|
|
Strongly agree |
17% |
|
Agree |
41% |
|
Neutral |
23% |
|
Disagree |
17% |
|
Strongly disagree |
2% |
|
Q14. Online teaching sessions are more interactive than in person classes |
|
|
Strongly agree |
0% |
|
Agree |
0% |
|
Neutral |
10% |
|
Disagree |
52% |
|
Strongly disagree |
18% |
|
Q15. Didactic online sessions are preferable to live in person classes |
|
|
Strongly agree |
0% |
|
Agree |
0% |
|
Neutral |
30% |
|
Disagree |
45% |
|
Strongly disagree |
25% |
|
Q16. Partook in other activities at some time during an online class |
|
|
Yes, always |
8% |
|
Yes, occasionally |
46% |
|
Yes, rarely |
31% |
|
No |
15% |
|
Q17. Content of online classes are better retained than in person classes |
|
|
Strongly agree |
0% |
|
Agree |
2% |
|
Neutral |
25% |
|
Disagree |
48% |
|
Strongly disagree |
25% |
Table 2: Online teaching
3. Discussion
This survey identified most valued teaching activities. It also assessed the effects of COVID-19 during the first wave on resident teaching hours. Finally, it gathered the opinions of residents with the use of online teaching. Many surgical curriculums are now completely online [8,9]. The impact of this important change is ongoing. A United States National Survey of general surgery residents reported that over 30% of trainees noted a decrease of educational didactics during the pandemic while another survey conducted in West Scotland reported 75% of surveyed trainees not attending any teaching [9,10]. The diminished teaching hours recorded at our institution during the first wave pandemic is thought to be attributable to important restructuring by programs. This period was marked by reduced staff availability, cancellation of case discussions, increased online departmental meetings and cancellations of conferences all to respect social distancing measures. This possibly explains the diminished mean number of teaching hours and increased standard deviation. Interestingly other institutions managed to rapidly develop during the same pandemic period a schedule that addressed the increasing loss of teaching hours and some managed to double teaching hours [8-11]. The COVID-19 pandemic illustrates the importance that programs must be prepared and have educational contingency plans readily available if similar events are to occur. Novelties in medical education have emerged during this time. However, none were reported with our survey. We suppose that the transition and adjustment to the online platforms may have blunted the implementation of additional new academic activities. However, the literature does state certain novelties with regards to medical education strategies. A systemic review by Dedeillia and al. reports that programs having adopted a “flipped classroom” and active learning facilitated the transition to online formats [12]. Although described for preclinical setting, with proper residency level learning objectives, such activities could be implemented and could lead to greater interactions. This systematic review also lists the use of online atlases, podcast and social media as means to optimize clinical teaching. Other novelties to minimize viral transmission all while acquiring new surgical skills is the use practice surgical kits [13]. Some programs have also implemented usage of live camera footage in operating rooms to palliate the limited number of trainees within surgical theaters [14]. The top three listed activities by our group of residents have a common characteristic. They have the possibility of being interactive and can result in active discussions between the professor and the trainee. Our survey shows that these interactions are appreciated by trainees and possibly lacking with virtual classes. The diminished exchanges may explain why residents are possibly partaking in other activities while an online activity is ongoing. This may also be one of many factors explaining why residents report diminished retainment of teachings. However, other studies are needed to validate these proposed associations.
3.1 Limitations
Our study has limitations related to survey-based studies. Firstly, even though the survey link was emailed weekly for a month the response rate of 56% of our small population of 85 residents is considered low. Small sample sizes are common in surgical research. This resulted in a descriptive analysis. In attempt to minimize this effect we included participants from all surgical specialties at our institution. The high volume of emails sent through the university email system during this period might have dissuaded certain residents to participate. Also, the lower responses from the PGY5&6 group might be due to email not reaching these ex-residents. To complete the survey the ex-trainees were required to still be using and monitoring their university email during the time. The limited number of responses did not allow us to perform sub-categorical comparisons. A selection bias may also have resulted from the fact that this survey was on voluntary participation and may have overrepresented participants with strong opinions pertaining to teaching during this period. Resident reported teaching hours may also be biased by possible distorted recollection. Finally, this survey is limited by the fact that it is monocentric and is illustrates views of an urban setting. It may not exemplify the experiences of rural programs nationwide. Despite some limitation our hope is that our study improves the understanding of surgical education and stimulate further discussion to improve resident education.
4. Conclusion
The coronavirus 2019 pandemic has prompted unparalleled changes to healthcare as well as the methods in which we are training surgeons of tomorrow. The data presented can provide insight of residents needs to surgical programs to improve training. When a pandemic occurs, surgical programs must be ready optimize teaching schedules to minimize lost teaching hours. Even though the appreciation of virtual learning seems unsatisfactory by residents, trainees still require and appreciate teaching by their mentors and coworker, may it be in person or on a computer screen. Future studies will be needed to assess the impact theses educational changes on long-term trainee performance.
References
- Organization WH. Coronavirus disease 2019 (COVID-19) Situation Report - 51. World Health Organization (2020).
- Coleman JR, Abdelsattar JM, Glocker RJ. COVID-19 Pandemic and the lived experience of surgical residents, fellows, and early-career surgeons in the American College of Surgeons. J Am Coll Surg 232 (2021):119-135.
- Adesunkanmi AO, Ubom AE, Olasehinde O, et al. Impact of the COVID-19 Pandemic on surgical residency training: Perspective from a low-middle income country. World J Surg 45 (2021): 10-17.
- Nassar AH, Zern NK, McIntyre LK, et al. Emergency restructuring of a general surgery residency program during the coronavirus disease 2019 pandemic: The University of Washington experience. JAMA Surg 155 (2020): 624-627.
- Ostapenko A, McPeck S, Liechty S, et al. Impacts on surgery resident education at a first wave COVID-19 epicenter. J Med Educ Curric Dev 7 (2020): 23-28.
- Université Laval - Faculté de médecine- Vice-décanat aux études médicales postdoctorales. Algorithme de redéploiement des résidents et résidents Pandémie COVID-19 (2020).
- White EM, Shaughnessy MP, Esposito AC, et al. Surgical education in the time of COVID: Understanding the early response of surgical training programs to the novel coronavirus pandemic. J Surg Educ (2020).
- Gawad N, Towaij C, Stuleanu T, et al. Prioritizing resident and patient safety while maintaining educational value: emergency restructuring of a Canadian surgical residency program during COVID-19. Can J Surg 63 (2020): E302- E305.
- Aziz H, James T, Remulla D, et al. Effect of COVID-19 on surgical training across the United States: A national survey of general surgery residents. J Surg Educ 78 (2021): 431-439.
- Khan KS, Keay R, McLellan M, et al. Impact of the COVID-19 pandemic on core surgical training. Scott Med J 12 (2020): 36-43.
- Kilcoyne MF, Coyan GN, Aranda-Michel E, et al. The impact of coronavirus 2019 on general surgery residency: A national survey of program directors. Ann Med Surg 65 (2021): 102-105.
- Dedeilia A, Sotiropoulos MG, Hanrahan JG, et al. Medical and surgical education challenges and innovations in the COVID-19 Era: A Systematic Review. In Vivo 34 (2020): 1603-1611.
- Okland TS, Pepper JP, Valdez TA. How do we teach surgical residents in the COVID-19 era? J Surg Educ. 77 (2020): 1005-1007.
- Chao Tiffany NT. Creation of an interactive virtual surgical rotation for undergraduate medical education during the COVID-19 Pandemic. Journal of Surgical Education (2020).


 Impact Factor: * 4.2
Impact Factor: * 4.2 Acceptance Rate: 72.62%
Acceptance Rate: 72.62%  Time to first decision: 10.4 days
Time to first decision: 10.4 days  Time from article received to acceptance: 2-3 weeks
Time from article received to acceptance: 2-3 weeks 