Development of Myofibrosarcoma after Removal of Longstanding Chemotherapy Port
Christopher P. Rice1, Aaron Wyble2, Suimin Qiu2, Michael Silva1, Douglas Tyler1, Linda Phillips1 and Celia Chao1*
1Departments of Surgery, University of Texas Medical Branch, Galveston, Texas, USA
2Departments Surgical Pathology, University of Texas Medical Branch, Galveston, Texas, USA
*Corresponding Author: Dr. Celia Chao, Departments of Surgery, University of Texas Medical Branch, Galveston, Texas, USA
Received: 12 January 2018; Accepted: 02 February 2018; Published: 07 February 2018
Article Information
View / Download Pdf Share at FacebookAbstract
We present a case report of a patient who developed a myofibrosarcoma after removal of a left-sided chemotherapy port which was place ten years prior for the treatment of a right sided-breast cancer. The patient developed a new left-sided breast cancer and after surgical resection of the left breast cancer, she presented with a rapidly growing mass; a high grade sarcoma was diagnosed after definitive resection. We also review the literature in foreign body- associated sarcomagenesis.
Keywords
Sarcomagenesis, Foreign body, Fibrosarcoma
Sarcomagenesis articles, Foreign body articles, Fibrosarcoma articles
Sarcomagenesis articles Sarcomagenesis Research articles Sarcomagenesis review articles Sarcomagenesis PubMed articles Sarcomagenesis PubMed Central articles Sarcomagenesis 2023 articles Sarcomagenesis 2024 articles Sarcomagenesis Scopus articles Sarcomagenesis impact factor journals Sarcomagenesis Scopus journals Sarcomagenesis PubMed journals Sarcomagenesis medical journals Sarcomagenesis free journals Sarcomagenesis best journals Sarcomagenesis top journals Sarcomagenesis free medical journals Sarcomagenesis famous journals Sarcomagenesis Google Scholar indexed journals Foreign body articles Foreign body Research articles Foreign body review articles Foreign body PubMed articles Foreign body PubMed Central articles Foreign body 2023 articles Foreign body 2024 articles Foreign body Scopus articles Foreign body impact factor journals Foreign body Scopus journals Foreign body PubMed journals Foreign body medical journals Foreign body free journals Foreign body best journals Foreign body top journals Foreign body free medical journals Foreign body famous journals Foreign body Google Scholar indexed journals Fibrosarcoma articles Fibrosarcoma Research articles Fibrosarcoma review articles Fibrosarcoma PubMed articles Fibrosarcoma PubMed Central articles Fibrosarcoma 2023 articles Fibrosarcoma 2024 articles Fibrosarcoma Scopus articles Fibrosarcoma impact factor journals Fibrosarcoma Scopus journals Fibrosarcoma PubMed journals Fibrosarcoma medical journals Fibrosarcoma free journals Fibrosarcoma best journals Fibrosarcoma top journals Fibrosarcoma free medical journals Fibrosarcoma famous journals Fibrosarcoma Google Scholar indexed journals Myofibrosarcoma articles Myofibrosarcoma Research articles Myofibrosarcoma review articles Myofibrosarcoma PubMed articles Myofibrosarcoma PubMed Central articles Myofibrosarcoma 2023 articles Myofibrosarcoma 2024 articles Myofibrosarcoma Scopus articles Myofibrosarcoma impact factor journals Myofibrosarcoma Scopus journals Myofibrosarcoma PubMed journals Myofibrosarcoma medical journals Myofibrosarcoma free journals Myofibrosarcoma best journals Myofibrosarcoma top journals Myofibrosarcoma free medical journals Myofibrosarcoma famous journals Myofibrosarcoma Google Scholar indexed journals Chemotherapy articles Chemotherapy Research articles Chemotherapy review articles Chemotherapy PubMed articles Chemotherapy PubMed Central articles Chemotherapy 2023 articles Chemotherapy 2024 articles Chemotherapy Scopus articles Chemotherapy impact factor journals Chemotherapy Scopus journals Chemotherapy PubMed journals Chemotherapy medical journals Chemotherapy free journals Chemotherapy best journals Chemotherapy top journals Chemotherapy free medical journals Chemotherapy famous journals Chemotherapy Google Scholar indexed journals Cancer articles Cancer Research articles Cancer review articles Cancer PubMed articles Cancer PubMed Central articles Cancer 2023 articles Cancer 2024 articles Cancer Scopus articles Cancer impact factor journals Cancer Scopus journals Cancer PubMed journals Cancer medical journals Cancer free journals Cancer best journals Cancer top journals Cancer free medical journals Cancer famous journals Cancer Google Scholar indexed journals Sentinel lymph node biopsy articles Sentinel lymph node biopsy Research articles Sentinel lymph node biopsy review articles Sentinel lymph node biopsy PubMed articles Sentinel lymph node biopsy PubMed Central articles Sentinel lymph node biopsy 2023 articles Sentinel lymph node biopsy 2024 articles Sentinel lymph node biopsy Scopus articles Sentinel lymph node biopsy impact factor journals Sentinel lymph node biopsy Scopus journals Sentinel lymph node biopsy PubMed journals Sentinel lymph node biopsy medical journals Sentinel lymph node biopsy free journals Sentinel lymph node biopsy best journals Sentinel lymph node biopsy top journals Sentinel lymph node biopsy free medical journals Sentinel lymph node biopsy famous journals Sentinel lymph node biopsy Google Scholar indexed journals Malignancy articles Malignancy Research articles Malignancy review articles Malignancy PubMed articles Malignancy PubMed Central articles Malignancy 2023 articles Malignancy 2024 articles Malignancy Scopus articles Malignancy impact factor journals Malignancy Scopus journals Malignancy PubMed journals Malignancy medical journals Malignancy free journals Malignancy best journals Malignancy top journals Malignancy free medical journals Malignancy famous journals Malignancy Google Scholar indexed journals Mastectomy articles Mastectomy Research articles Mastectomy review articles Mastectomy PubMed articles Mastectomy PubMed Central articles Mastectomy 2023 articles Mastectomy 2024 articles Mastectomy Scopus articles Mastectomy impact factor journals Mastectomy Scopus journals Mastectomy PubMed journals Mastectomy medical journals Mastectomy free journals Mastectomy best journals Mastectomy top journals Mastectomy free medical journals Mastectomy famous journals Mastectomy Google Scholar indexed journals Tumor articles Tumor Research articles Tumor review articles Tumor PubMed articles Tumor PubMed Central articles Tumor 2023 articles Tumor 2024 articles Tumor Scopus articles Tumor impact factor journals Tumor Scopus journals Tumor PubMed journals Tumor medical journals Tumor free journals Tumor best journals Tumor top journals Tumor free medical journals Tumor famous journals Tumor Google Scholar indexed journals
Article Details
1. Introduction
Foreign-body (FB) associated sarcomagenesis is rare. To our knowledge, we report the first case of a myofibrosarcoma developing after the removal of a long-term implanted device. We present this interesting case report and review the literature involving FB-associated sarcomagenesis.
2. Methods
A retrospective review of the clinical case was ascertained via electronic medical records. A PubMed search was used to review the literature published from 1956 to 2016 using the keywords: implant, myofibrosarcoma, myofibroblast, sarcoma, long-term, surgery, heal, growth factor.
3. Results
In 2007, a 57-year-old female with locally advanced infiltrating ductal carcinoma of the right breast underwent neoadjuvant chemotherapy via an implanted portacath inserted into her left internal jugular vein. After surgery and radiation, she was followed by medical oncology while on hormonal therapy. Despite a plan to remove the port at least 2 years prior, it was not removed until 10 years after insertion. One month after an uneventful port removal, the patient was diagnosed with a new left infiltrating ductal carcinoma which was treated and staged with left total mastectomy and sentinel lymph node biopsy, respectively.
Three weeks after the left total mastectomy, her physical examination was notable for a small, mobile, soft tissue nodule at the previous port site on the left anterior chest wall inferior to the clavicular head. Two months later, the nodule was noted to be 3 cm in diameter. Despite a benign percutaneous biopsy result, the subcutaneous mass continued to grow rapidly to 7 × 4 cm with overlying skin ulceration within the following 2 weeks. A wide local excision of the mass was performed and pathological diagnosis revealed a “high grade sarcoma, favoring myofibrosarcoma” (Figure 1, 2 and 3). All margins were widely negative except a region near the posterior margin near the fibrous sheath of the previous port. The patient subsequently underwent surgical excision of the prior port fibrous sheet en bloc with a small portion of the internal jugular vein. The final pathology revealed no residual malignancy.
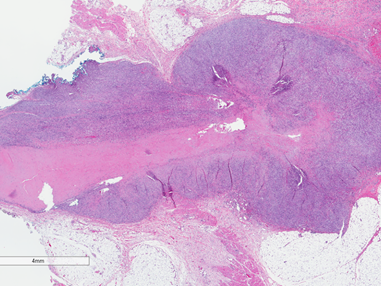
Figure 1: Low magnification of the surgical resection shows the fibrous tract from where the foreign body was removed. Surrounding this fibrous tract is a hypercellular mass with pushing infiltration into the surrounding subcutaneous fat and soft tissues. (Hematoxylin and Eosin Stain).
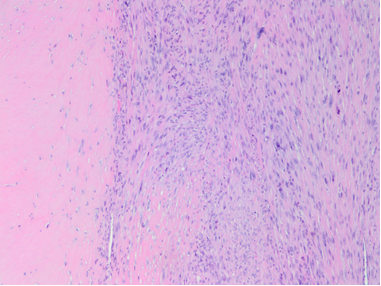
Figure 2: Medium magnification of the surgical resection at the interface of the fibrous tract and the hypercellular mass shows a spindle cell lesion with short fascicles. (Hematoxylin and Eosin Stain at 4x Magnification).
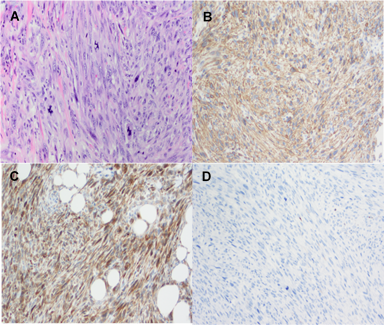
Figure 3: High magnification of the surgical resection in the hypercellular areas show high grade sarcoma highlighted by malignant spindle cells that show pleomorphic cellular and nuclear size, irregular nuclear contours, vesicular chromatin pattern, and abnormal mitoses (A). Immunohistochemistry shows the malignant cells are diffusely positive for Alpha Smooth Muscle Actin (B) and Calponin (C) and negative for Desmin (D). Not shown are negative stains for S100, SOX-10, CD34, and Caldesmon; and focal positivity for AE1/AE3, EMA, and CD31. These findings favor a myofibroblast cell origin. (Magnification 200 x).
4. Discussion
A review of the literature suggests a possible association between foreign bodies retained for a prolonged time frame and sarcomagenesis. However, the mechanism of FB-associated tumor development is not known, but many types of sarcomas have been described in the literature. To our knowledge, however, our case is the first to report a longstanding FB-associated myofibrosarcoma developing after FB removal followed by a major surgical intervention.
One published review of 40 case studies [1] of FB sarcomagenesis from 1956-1988 demonstrated an average latency of 14.12 years. Another published review of 22 case reports from 1956 to 1991 demonstrated an average latency of 10.89 years for soft tissue sarcomas associated with orthopedic implants [2]. Interestingly, however, these authors also performed a case-control study on 816 men diagnosed with a soft tissue sarcoma and found no significant relationship between implants and the diagnosis of a sarcoma, suggesting that other events may be involved in tumor development.
We hypothesize that tumor initiation and growth may accelerate post-surgery via growth factors related to wound healing. It is widely recognized that inflammation is an essential component of tumor development [3]. Tumor growth may be initiated via inflammatory responses in the body such as that involved in wound healing or surrounding an implanted foreign body [4, 5]. Thus, acute inflammation and wound healing mechanisms incited by a recent surgical intervention at the site of a long-standing implanted foreign body may be sufficient to initiate sarcomagenesis.
Based on this report and literature review, the differential diagnosis for a mass forming at the site of a current or previous implantation should include FB-associated sarcoma, especially with a recent history of surgery. Case reports infer a long latency period after placement of implanted devices, supporting prompt removal of unused devices. Patients who have a medical need for their device long term should be monitored and educated on the signs and symptoms of FB-associated sarcomagenesis.
References
- Jennings TA, Peterson L, Axiotis CA, et al. Angiosarcoma associated with foreign body material. Cancer 62 (1988): 2436-2444.
- Morgan R. Artificial implants and soft tissue sarcomas. J Clin Epidemiol 48 (1995): 545-549.
- Grivennikov SI, Greten FR, Karin M. Immunity, Inflammation, and Cancer. Cell 140 (2010): 883-899.
- Ceelen W, Pattyn P, Mareel M. Surgery, wound healing, and metastasis: Recent insights and clinical implications. Crit Rev Oncol Hematol 89 (2014): 16-26.
- Segatto I, Berton S, Sonego M, et al. Surgery-induced wound response promotes stem-like and tumor-initiating features of breast cancer cells, via STAT3 signaling. Oncotarget 5 (2014): 6267.


 Impact Factor: * 4.2
Impact Factor: * 4.2 Acceptance Rate: 72.62%
Acceptance Rate: 72.62%  Time to first decision: 10.4 days
Time to first decision: 10.4 days  Time from article received to acceptance: 2-3 weeks
Time from article received to acceptance: 2-3 weeks 