A Case Report of Endografting Using a Long Sheath under the Assistance of a Through-and-Thorough Wire Technique for an Extremely Tortuous Aortic Anatomy
Sachito Minegishi*, Yusuke Inaba, Hidehito Endo, Hiroshi Kubota
The Department of Cardiovascular Surgery, Kyorin University Hospital, Japan
*Corresponding author: Sachito Minegishi, The Department of Cardiovascular Surgery, Kyorin University Hospital, Japan.
Received: 20 August 2022; Accepted: 25 August 2022; Published: 01 September 2022
Article Information
Citation: Sachito Minegishi, Yusuke Inaba, Hidehito Endo, Hiroshi Kubota. A Case Report of Endografting Using a Long Sheath under the Assistance of a Through-And-Thorough Wire Technique for an Extremely Tortuous Aortic Anatomy. Journal of Biotechnology and Biomedicine 5 (2022): 148-150.
View / Download Pdf Share at FacebookAbstract
Abstract Introduction: Despite its rapid technological development and widespread uptake for thoracic aortic disease, an extremely tortuous aortic anatomy is considered a contraindication for thoracic endovascular aortic repair procedure. We report a case of a successful thoracic endovascular aortic repair using techniques to straighten an extremely tortuous aorta friendly. Methods: A 78-year-old man with frequent surgical history of aortic repair was admitted to our outpatient clinic because of dyspnea and back pain. Enhanced computed tomography scan revealed type Ib endoleak, acute enlargement of the remnant native aorta and an extremely tortuous aorta. We successfully performed a thoracic endovascular aortic repair using a Gore DrySeal 65 cm sheath, combined with a Gore C-Tag device under the assistance of a through-and-thorough wire technique in the distal descending aorta. Conclusions: Using all the available techniques, thoracic endovascular aortic repair can be performed even in the most
Keywords
<p>Case report; Tortuous aorta; TEVAR; Through-and-thorough wire technique; Long sheath</p>
Article Details
1. Introduction
The Thoracic Endovascular Aortic Repair (TEVAR) procedure is challenging in cases of an extremely tortuous aorta [1]. Herein, we describe a case of a successful TEVAR performed in an extremely tortuous S-shaped thoracoabdominal aorta (TAA), which was a result of the open repair for the Thoracoabdominal Aortic Aneurysm (TAAA) and dense adhesions around the remnant native aorta, using techniques with a unique use of Gore DrySeal long sheath to straighten the vessel friendly.
2. Methods
A 78-year-old man was admitted to our outpatient clinic because of dyspnea and back pain. He underwent an emergency Total Aortic Arch Replacement (TAR) by means of the homemade open stent graft installation for DeBakey type I acute aortic dissection 16 years before the clinic visit. Two years after the TAR, infra-renal abdominal aortic aneurysm was repaired with a 20-mm bifurcated Gelsoft graft (Vascutek Ltd., Inchinnan, United Kingdom), and 6 years after the open abdominal aortic repair, TEVAR using Zenith TX2 2P-38-202 (proximal) and 2P-32-140 (distal) (Cook Medical, IN, USA) was performed to treat descending aortic aneurysm, using the previous homemade open stent graft as a proximal landing zone. Seven years after the TEVAR, he underwent thoracoabdominal aortic replacement using a 24-mm Coselli thoracoabdominal graft (Vascutek Ltd., Inchinnan, United Kingdom) via a left lateral thoracotomy. This procedure was complicated by strikingly dense adhesions around the TAA near the diaphragm, resulting in a 40 mm long remnant native TAA. These adhesions are considered to be due to diffuse large B-cell lymphoma involving mesenteric and retroperitoneal lymph nodes, which was treated by surgery and chemotherapy 6 years before the TAAA repair. Although he remained well one year after the open repair for the TAAA, he presented to our clinic with dyspnea and back pain. He has medical history of hypertension and hyperlipidemia. He has no family history and psycho-social history. Enhanced Computed Tomography (CT) scan revealed type Ib endoleak and acute enlargement of the remnant native aorta around the distal end of the Zenith TX2 2P-32-140 (Figure 1a,1b). He was found to have a significant S-type bend in thoracoabdominal native and aortic grafts, which was a result of the open repair for the TAAA (Figure 1c,1d).
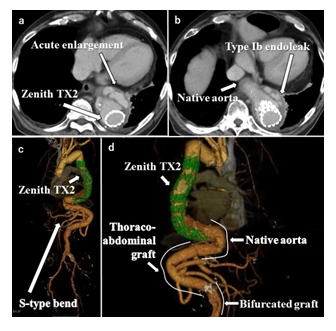
Figure 1: Computed tomography scan with enhancement in the axial (a and b) view demonstrates type Ib endoleak and enlargement of the remnant native aorta. Front (c) and rear (d) views of a 3-dimensional reconstruction of the dynamic computed tomography scan demonstrate the extremely tortuous aorta.
Laboratory tests suggested a white blood cell count of 4.800/μL, hemoglobin of 11.5 g/dL, a C-reactive protein level of 8.85 mg/dL (normal range < 0.14), creatine of 1.59 mg/dL, procalcitonin of 0.08 ng/mL (normal range < 0.5) and Fibrin/Fibrinogen Degradation Products (FDP) of 49.2 μg/mL (normal range < 10). Because of his frequent surgical history of aortic repair and dense adhesions around the remnant native aorta which was observed during the previous open TAAA repair, we chose to pursue an urgent TEVAR. Under general anesthesia, with endobronchial intubation and mechanical ventilation, redo surgical cut-down was made on the right common femoral artery. First, a 0.035-inch hydrophilic guidewire was inserted to the ascending aorta from the right femoral artery, following which a 65-cm-long 22 French introducer sheath (DrySeal; W.L. Gore & Associates, Flagstaff, AZ, USA) was inserted. But, due to the extremely sigmoid bend, we could not insert the 65-cm-long sheath even to the descending aorta. Therefore, the guidewire in the ascending aorta was snared by a EN Snare® Endovascular Snare System (Merit Medical System, South Jordan, UT, USA) from the right brachial artery (Figure 2a) and the pull through was made. We snared the guide wire in the ascending aorta, considering the risk of embolization.
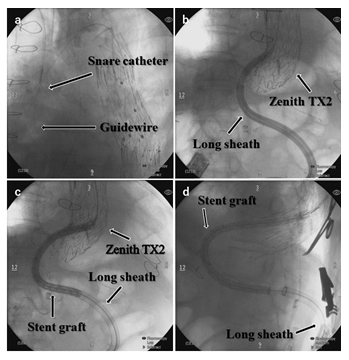
Figure 2: (a) Fluoroscopy image (left anterior oblique projection) demonstrating the guidewire and the snare catheter in the ascending aorta to accomplish through-and-through wire technique. (b) Fluoroscopy image (anterior posterior projection) demonstrating the long sheath inserted in the Zenith TX2. (c) Fluoroscopy image (anterior posterior projection) demonstrating the stent graft advanced within the long sheath. (d) Fluoroscopy image (left anterior oblique projection) demonstrating the long sheath being withdrawn and the stent graft in the appropriate location.
Using this through-and-through wire technique, the long sheath was advanced until it was positioned 5 cm proximal to the distal end of the Zenith TX2 2P-32-140 (Figure 2b). A pull on the catheter was required to straighten the S-type shape. A GORE TAG conformable stent graft with active control (CTAG with AC; diameter 37 mm, length 20 cm; W.L. Gore & Associates, Flagstaff, AZ, USA) was then advanced within the long sheath under fluoroscopic monitoring to the appropriate location (Figure 2c). The long sheath was withdrawn gently (Figure 2d), and the stent graft was deployed. After that, a CTAG with AC (diameter 37 mm, length 10 cm) was advanced and deployed covering 4 cm of the distal end of the proximal CTAG with AC (diameter 37 mm, length 20 cm) and 4 cm of the proximal end of the previous TAA graft. There was no endoleak observed. The patient’s post-operative course was uneventful. Post-operative CT taken before discharge demonstrated no endoleak or embolic events. He is doing well 19 months after the surgery without any complications including neurological disfunction, and the aneurysm is shrunk. Laboratory tests suggested FDP of 32.2 μg/mL (normal range < 10).
3. Results
We performed a successful TEVAR for an extremely sigmoid TAA patient using techniques to straighten the vessel friendly.
4. Discussion
After the introduction of TEVAR [2], it has gradually become popular for treatment of thoracic aortic lesions due to its lower perioperative mortality and morbidity compared with open surgery. But high tortuosity is thought to increase the occurrence of deployment failure and endoleak [3]. Although through-and-through wire technique potentially increases the risk of micro emboli formation, resultant cerebral infarction, and aortic dissection in the brachiocephalic and iliac artery, this procedure is one of effective methods to deliver stent grafts in patients with tortuous aortas [4]. In our technique, a 65-cm-long sheath, which is more flexible than low profile devices such as Zenith TX2, is advanced at first, and then a main stent graft is advanced within the long sheath. We straighten the tortuous aorta friendly in stages. Combined with through-and-through wire technique, we can provide exceptional access to challenging anatomies like this case. We do not choose double wire technique because of the low flexibility of the previous TAA graft which must make double wire technique ineffective. A 65-cm-long sheath has hydrophilic coating which offers flexibility and kink resistance, and this can minimize damages to delivery route [5]. In addition, we advance main stent grafts within the long sheath which allows main grafts to remain “covered” while crossing an extremely sigmoid aorta, therefore, we can deliver stent grafts safely. This case is an unconventional example of a TAVAR using a Gore DrySeal 65 cm sheath, and the length of the sheath is not long enough to allow a TEVAR in the zone 1 or 2. It also has a possibility to be combined with other stent grafts. The novelty of this case should be taken in the context of the patient’s general condition and complicated surgical history.
5. Conclusions
We describe a case of a successful TEVAR being performed through an extremely sigmoid TAA using techniques to straighten the vessel friendly. Using all the techniques available, TEVAR can be performed in the most challenging patients.
Acknowledgments
SM, YI and HK conceived and designed research. SM, YI and HE conducted experiments. SM wrote the manuscript. All authors read and approved the manuscript.
Declarations
Funding and Conflicts of Interests/Competing Interests
The authors declare they have no funding source or interests.
Ethic approval
Ethic approval was granted by the Ethics Committee of Kyorin University (October 1, 2021/No. R03-113).
Consent to participate and Consent for publication;
Informed consent was obtained from the patient for participation and publication of this case.
Availability of data and material, Code availability and Authors' contributions
References
- Grabenwöger M, Alfonso F, Bachet J, et al. Thoracic Endovascular Aortic Repair (TEVAR) for the treatment of aortic diseases: a position statement from the European Association for Cardio-Thoracic Surgery (EACTS) and the European Society of Cardiology (ESC), in collaboration with the European Association of Percutaneous Cardiovascular Interventions (EAPCI). Eur J Cardiothorac Surg 42 (2012): 17-24.
- Dake MD, Miller DC, Semba CP, et al. Transluminal placement of endovascular stent-grafts for the treatment of descending thoracic aortic aneurysms. N Engl J Med 331 (1994): 1729-1734.
- Chen CK, Liang IP, Chang HT, et al. Impact on outcomes by measuring tortuosity with reporting standards for thoracic endovascular aortic repair. J Vasc Surg 60 (2014): 937-944.
- Kanaoka Y, Ohki T, Maeda K, et al. Multivariate Analysis of Risk Factors of Cerebral Infarction in 439 Patients Undergoing Thoracic Endovascular Aneurysm Repair. Medicine (Baltimore) 95 (2016): e3335.
- Fukuda T, Tan W, Sadeghi S, et al. Utility of the long DrySeal sheath in facilitating transcatheter pulmonary valve implantation with the Edwards Sapien 3 valve. Catheter Cardiovasc Interv 96 (2020): E646-E652.


 Impact Factor: * 5.3
Impact Factor: * 5.3 Acceptance Rate: 75.63%
Acceptance Rate: 75.63%  Time to first decision: 10.4 days
Time to first decision: 10.4 days  Time from article received to acceptance: 2-3 weeks
Time from article received to acceptance: 2-3 weeks 