Cost-utility Analysis-Comparison between with and without using Intraoperative Neuromonitoring in Spinal Surgery for Adolescent Idiopathic Scoliosis Patients
Chaiwat Lorphongphaiboon, Anand Sachamuneewongse, Thanita Panya-amornwat*, Athikom Methathien, Yongyot Laungwitchajareon, Sukrom Cheecharern
Rajavithi Hospital, College of Medicine Rangsit University, 2, Phayathai Road, Ratchathewi District, Bangkok, Thailand
*Corresponding Author: Thanita Panyaamornwat, Orthopaedics Department, Rajavithi Hospital, 2 Rajavithi Road, Ratchathewi District, Bangkok, 10400, Thailand
Received: 24 May 2020; Accepted: 18 June 2020; Published: 25 June 2020
Article Information
Citation: Chaiwat Lorphongphaiboon, Anand Sachamuneewongse, Thanita Panya-amornwat, Athikom Methathien, Yongyot Laungwitchajareon, Sukrom Cheecharern. Cost-utility Analysis-Comparison between with and without using Intraoperative Neuromonitoring in Spinal Surgery for Adolescent Idiopathic Scoliosis Patients. Journal of Surgery and Research 3 (2020): 171-176.
View / Download Pdf Share at FacebookAbstract
Introduction: Nowadays, Intraoperative Neuromonitoring (IONM) techniques are used in complex spinal surgery to improve surgical outcome by reducing the risk of iatrogenic neural injury. But the cost of the device does not included by National Heath Security Care system of Thailand.
Objective: To compare cost-utility between with and without using IONM in spinal surgery for Adolescent Idiopathic Scoliosis (AIS) patients.
Methods: A retrospective review of prospectively collected data in 40 Adolescent Idiopathic Scoliosis patients after 6 months post operation at Rajavithi hospital. EQ-5D-5L (Thai version) questionnaires and medical record review were administered.
Results: Conventional surgery cost 681,746.57 Baht or $ 20,647.10 more than surgery with IONM (Conventional surgery 1,061,405.75 Baht or $ 32,145.30, using IONM 379,659.18 Baht or $11,498.20). The quality-adjusted life years (QALYs) in conventional surgery was 0.878 and is surgery with IONM was 0.9.
Conclusion: Spinal surgery with using IONM in AIS patients is cost-effective strategy than conventional surgery.
Keywords
<p>Adolescent Idiopathic Scoliosis, Cost-utility, Intraoperative Neuromonitoring</p> <gdiv></gdiv>
Article Details
1. Introduction
Adolescent Idiopathic Scoliosis (AIS) is the most common form of abnormal spinal curvature with unknown etiology affecting children over the age of 10 until skeletal maturity, more commonly noticed affecting girls. Treatment options for children with AIS can be classified and into Operative and Non-operative treatment. There are many factors affecting the choice of treatment include age, curve type and curve magnitude. The goal of operative treatment is to correct the abnormal curvature of the spine and to prevent progression of deformity, but most importantly is to prevent surgical related complications such as spinal cord injury. Current technique of using Intraoperative Neuromonitoring (IONM) to assess spinal cord function has been known to improve surgical outcome by preventing intraoperative spinal cord injury, which can lead to permanent disability. However the cost of the device used to monitor AIS patients during surgery is not covered by the National Health Security Care of Thailand.
There were 53 AIS patients underwent surgery at Rahavithi Hospital from 2009 to 2015. The cost of using IONM should outweigh the cost of health care for any of these patients with spinal cord injury and other medical complications secondary to spinal cord injury.
1.1 Objective
The purpose of this study was to evaluate the cost-effectiveness of spinal surgery in AIS patients with the use of IONM compared with conventional surgery without monitoring.
2. Methods
Literature review was done to design an appropriate cost effective analysis using Decision tree (Figure 1). A study by John M. Flynn [1] showed using intraoperative monitoring can reduce neurological complications from 4% to 0.55%. In this retrospective study, a prospectively collected data regarding quality of life in 40 Adolescent Idiopathic Scoliosis patients after 6 months of corrective surgery at Rajavithi hospital from 2011 to 2017 using EQ-5D-5L (Thai version) questionnaires was reviewed, informed consent was obtained by all the participants and their guardians to allow the use of clinical data for research purposes. Exclusion criteria were scoliosis patients classified as non idiopathic (congenital scoliosis, neuromuscular scoliosis) and AIS patients with pre-existing neurological symptoms. Cost analysis from a societal perspective includes
- Direct medical cost such as medication costs and consumables costs
- Indirect medical cost such as patients’ traveling cost, meal costs and accommodation costs
- Non medical cost such as opportunity costs.
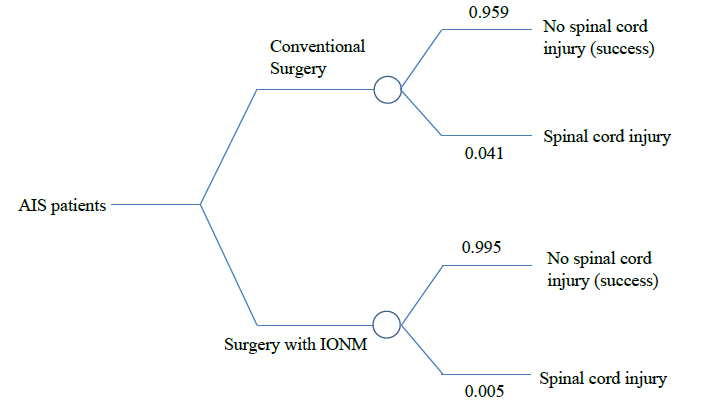
Figure 1: Decision Tree model used in the analysis.
Costs data were collected by reviewing medical records and interviewing patients underwent surgery in Rajavithi hospital from 2009 to 2017 and their guardians. The purpose of medical records review was to calculate the direct medial cost for patients received surgical treatment with and without IONM, and the purpose of the interview was to calculate indirect medical cost and non medical cost which was an actual cost that patients spent during treatment. Opportunity cost during treatment includes patients’ and their family member’s workday losses (maximum 8 hours per day) multiplied by average wage (Thailand average wage in 2015 was 26,915 Baht or $815.14 per month), the remaining time were multiplied by minimum wage (Thailand minimum wage in 2017 was 300 Baht per day). Unemployed patients and family members were excluded. We use the currency exchange rate by the Bank of Thailand on 5th January 2015, 1 US dollar ($) is 33.019 Baht. AA Kawu et al. [2] tried to determine the cost of acute phase injury among spinal cord injured patients treated conservatively in Nigeria, the study showed the direct medical cost was 7,884.28 Baht or $238.78 , the indirect medical cost was 52,773.94 Baht or $ 1,598.29 and non medical care cost was at 21,219,528.3 Baht or $ 642,646 [3], with the mean age of patients at 45.4 years.
3. Results
3.1 Demographic data
A total of 40 participants were included in the analysis (20 participants for each type of surgery), with the mean age of 16.21 years in conventional surgery and 20.2 years in surgery with IONM (Table 1).
3.2 Cost of treatment in AIS patients
We reviewed the data of 40 AIS patients received surgical treatment in Rajavithi hospital (20 patients in conventional surgery group and 20 patients in surgery with IONM group) to calculate treatment cause and quality of life postoperative. Direct medical cost was found to be higher in surgery with IONM (265,946.38 Baht or $8,054.34) compared to conventional surgery (182,118.95 Baht or $5,515.58). However, the indirect medical cost (896,236.57 Baht or $27,143.06 in conventional surgery and 106,004.91 Baht or $3210.42 in surgery with IONM) and the non-medical cost (10,050.23 Baht or $304.38 in conventional surgery and 7,707.89 Baht or $233.44 in surgery with IONM) were lower in patients underwent surgery with IONM. Complications such as spinal cord injury in conventional surgery were found to be 8 times higher (0.041%) than surgery with IONM (0.005%).
3.3 Cost-utility analysis
When applying the data from Table 2 and Table 3 into the decision tree model, it shows that the total cost (direct and indirect medical costs) of conventional surgery was 681,746.57 Baht or $20,647.10 more than surgery with IONM (conventional surgery 1,061,405.75 Baht or $32,145.30 and surgery with IONM 379,659.18 Baht or $11,498.20) (Table 4), which is the amount that the government has to pay more for each conventional surgery. Quality-adjusted life years (QALYs) for patients underwent conventional surgery was 0.878, while in patients underwent surgery with IONM, the QALYs was at 0.90. The cost-utility analysis of having a surgery with IONM for AIS patients yields a cost per QALYs ratio of 30,988,480.45 Baht or $938504.51 per QALY.
|
Parameters |
Surgery with IONM (%) (20) |
Conventional surgery (%) (20) |
|
Sex |
||
|
Male |
3 (15) |
1 (5) |
|
Female |
17 (85) |
19 (95) |
|
Education |
||
|
Highschool |
15 (75) |
17 (85) |
|
Bachelor degree |
4 (20) |
3 (15) |
|
Others |
1 (5) |
0 |
|
Domicile |
||
|
Bangkok |
11 (55) |
12 (60) |
|
Others |
9 (45) |
8 (40) |
|
Occupation |
||
|
Students |
18 (90) |
19 (95) |
|
Workers |
2 (10) |
1 (5) |
|
Treatment Scheme |
||
|
Social Security |
2 (10) |
0 |
|
Universal Coverage |
17 (85) |
17 (85) |
|
Government Officers |
1 (5) |
3 (15) |
|
Age Mean (SD) |
16.21 |
20.2 |
|
Weight Mean (SD) |
47.69 |
52.4 |
|
Height Mean (SD) |
160.46 |
164.2 |
Table 1: Demographic Data.
|
Probability |
Distribution |
Mean |
Standard Deviation |
References |
|
Conventional surgery without complication |
β |
0.90059 |
0.1918 |
1 |
|
Conventional surgery with complication |
β |
0.041 |
0.0082 |
1 |
|
Intraoperative monitoring without complication |
β |
0.90095 |
0.199 |
1 |
|
Intraoperative monitoring with complication |
β |
0.005 |
0.001 |
1 |
Table 2: Probability for each type of surgery.
|
Costs |
Conventional Surgery |
Surgery with IONM |
||
|
Mean |
Standard Errors |
Mean |
Standard Errors |
|
|
Direct Medical Costs |
182,118.95 |
36,423.79 |
265,946.38 |
53,189.27 |
|
Non-medical Costs |
10,050.23 |
2,010.04 |
7,707.89 |
1,541.57 |
|
Indirect Medical Costs |
896,236.57 |
179,247.31 |
106,004.91 |
21,200.98 |
Table 3: Cost-effectiveness analysis model Input.
|
Parameters |
Conventional Surgery |
Surgery with IONM |
Incremental |
|
Costs |
1,061,405.75 |
379,659.18 |
681,746.57 |
|
QALYs |
0.878 |
0.900 |
0.022 |
|
Cost per QALY |
30,988,480.45 |
||
Table 4: Cost-utility analysis.
4. Discussion
The people in the management office are mostly concerned with the cost of treatment, which usually in direct conflicts with the physicians who are more focused on the results. Because of that the Thai government issued that cost-effective study has to be done before any treatment or medication can be covered by the National Health Security Care system of Thailand. As demonstrated in our study, the direct medical cost of treatment for AIS patients underwent correction surgery with IONM was more than conventional surgery, because it required more equipment and resources. However, the indirect medical cost and non medical cost, which include the health care cost and opportunity cost following postoperative spinal cord injury was found to be higher in conventional surgery group. A study with similar results was published in 2013 by John P. Ney et al. [4], which showed that performing surgery with IONM reduced intra-operative complications and the cost by $ 23,189. A WHO report on macroeconomics and health suggested that for a developing countries, the cost of investment in healthcare should be less than 3 times of National income (NI) [5]. Thailand NI per capita in 2016 was 147,088 Baht or $4,454.65, so the cost should not be more than 441,264 Baht or $13,363.94. Data from the cost utility analysis showed that by using IONM, we reduced the risk of intra-operative spinal cord injury and yielded a cost per QALYs ratio of 30,988,480.45 Baht or $938504.51 per QALY. If the cost of the device used for intra-operative monitoring were to be covered by the National Health Security Care System of Thailand, the additional cost of the device should outweigh the cost of health care for patients with permanent disabilities following surgery. The limitation of this study is that, we do not have a record of spinal cord injury following surgery in Rajavithi Hospital, so the data on costs and quality of life were based on other studies.
5. Conclusion
For AIS patients underwent corrective surgery, using intra-operative monitoring was more cost-effective than conventional surgery.
Disclosure
The authors have no personal or financial conflict of interest in any materials or devices mentioned in this article.
References
- Flynn JM, Sakai DS. Improving safety in spinal deformity surgery: advances in navigation and neurologic monitoring. European spine journal: official publication of the European Spine Society, the European Spinal Deformity Society, and the European Section of the Cervical Spine Research Society 22 (2013): 131-137.
- Kawu AA, Olawepo A, Salami AOO, et al. A cost analysis of conservative management of spinal. International Spinal Cord Society 49 (2011): 1134-1137.
- Spinal Cord Injury Facts and Figures at a Glance. National Spinal Cord Injury Statistical Center, Birmingham, Alabama (2012).
- John P Ney, David N van der Goes, Jon H Watanabe. Cost-Benefit Analysis: Intraoperative Neurophysiological Monitoring in Spinal Surgeries. Journal of Clinical Neurophysiology 30 (2013): 280-286.
- Committee on Macroeconomic and Health. Macroeconomics and health: investing in health for economic development. Geneva: World Health Organization (2001).


 Impact Factor: * 4.2
Impact Factor: * 4.2 Acceptance Rate: 72.62%
Acceptance Rate: 72.62%  Time to first decision: 10.4 days
Time to first decision: 10.4 days  Time from article received to acceptance: 2-3 weeks
Time from article received to acceptance: 2-3 weeks 