Double-Crossed Knotless Suture Anchor Repair of Quadriceps Tendon Rupture
Waqas Ali1, Javaid Iqbal2, Talat Mahmood2, Liam Leonard2, Paul O'Grady3
1Registrar Trauma & orthopaedic, Cork University Hospital, Wilton, Co. Cork, Ireland
2Mayo University Hospital, Castlebar, Co. Mayo, Ireland
3Hon Personal Professor in Surgery, National University of Ireland, Galway, Consultant Trauma & Orthopaedic Surgery, Mayo University Hospital, Co.Mayo Ireland
*Corresponding Author: Waqas Ali, Department of Trauma and orthopaedic, Registrar Trauma & orthopaedic, Cork University Hospital, Wilton, Co. Cork, Ireland.
Received: 08 March 2022; Accepted: 16 March 2022; Published: 29 March 2022
Article Information
Citation: Waqas Ali, Javaid Iqbal, Talat Mahmood, Liam Leonard, Paul O'Grady. Double-Crossed Knotless Suture Anchor Repair of Quadriceps Tendon Rupture. Journal of Surgery and Research 5 (2022): 173-184.
View / Download Pdf Share at FacebookAbstract
Quadriceps tendon rupture is an uncommon injury but may result in long term disability if not adequately repaired. Many techniques are described for repair of acute quadriceps tendon rupture, including tendon-to-tendon repair, trans-osseous tunnels, synthetic augmentation, tendon plasty and the use of suture anchors. There is no single accepted surgical treatment. This study's objective was to assess the efficacy of a double-crossed suture anchor repair in the management of quadriceps tendon rupture.
Materials and methods
85 patient attended our institute for surgical management of quadriceps tendon rupture over eight years (2012-2019). Twenty patients were treated with the use of a double-crossed suture anchor fixation. These patients were allowed to weight bear in a hinged knee brace for six weeks following surgery. Eighteen out of twenty patients had one or more predisposing comorbidities, including obesity, diabetes, renal failure, quinolone and steroid use.
Results
Clinical and functional outcomes were recorded during follow up visits prospectively for a mean of one year (10-14 months). The mean knee flexion was 124 degree (120-130). All patients were able to return to activities of daily living (ADL) with a mean of 2 months (1.5-3 months) and return to work at a mean of 6 months (4-8 months). The mean Tegner, Cincinnati and Lysholm score at the latest follow up were 2.8 (0-5), 79.2 (60-88) and 90 (70-100), respectively. There were no early complications. There was no re-tear reported at the latest follow up.
Conclusion
The double-crossed suture anchor fixation is a safe and effective treatment option in managing quadriceps tendon ruptures.
Keywords
<p>Quadriceps repair; Tendon rupture; Knotless technique; Suture anchor; Double-crossed suture</p>
Article Details
1. Introduction
Quadriceps tendon ruptures are uncommon but may result in long term disability if not adequately repaired [1-3]. Clayton and Court-Brown reported the incidence of distal quadriceps tendon avulsion as 1.37 cases per 100,000 per year with a mean age of 50.5 in men and 51.7 in women [4]. The aetiology of quadriceps tendon rupture includes reduced blood supply, repetitive microtrauma, diabetes mellitus, renal failure, steroid use [5-9,24] and previous knee surgery [9,14]. A direct blow injury or forceful eccentric quadriceps contraction may cause tendon rupture in younger patients; the force applied across the tendon exceeds its tensile strength causing it to tear. This commonly occurs in the mid-substance of the tendon or at the Musculo-tendonous junction [13,24]. Rupture may also occur spontaneously and bilateral simultaneous quadriceps tendon rupture has also been described. In these tears the aetiology is less certain. Spontaneous tendon rupture may be an end-state manifestation of a chronic degenerative process in the tendon tissue. Poor vascularity at the osseous tendon junction may result in local tissue hypoxia. Chronic medical conditions, chronic inflammation and certain medications can impair tendon healing, and the ability of the tenocytes to repair is overwhelmed, and tendon failure is inevitable [5-9,15]. A rupture in this situation usually occurs at the osseous tendon interface. In these cases, simple suture or end to end tendon repair is limited by the poor vascularity of this zone. Tendon ends are already pathological, and in conjunction with a poor host, optimal healing is difficult. Initial mechanical stability following primary suturing is compromised by a short distal stump and poor biomechanical strength of the suture configuration relative to the extensor mechanism's pull. Prolonged protection or immobilisation may result in quadriceps muscle atrophy and knee stiffness. Partial-thickness or small tears may resolve with conservative management. Full-thickness tears or high-grade partial tears often required operative repair [5,9]. Many surgical techniques described in the literature, including primary suturing of tendon ends, suture through patellar bone tunnels, repair augmentation with looped sutures proximally, autograft, allograft, suture or wires [13] . Maniscalco et al. were the first to describe the use of suture anchors for Achilles tendon repair, and their use has been expanded to quadriceps tendon repair [11,16]. The quadriceps muscle comprises the rectus femoris, vastus medialis, vastus lateralis, and vastus intermedius. The rectus femoris tendon widens distally to about 3-5 cm as it approaches the superior aspect of the patella. It continues over the superior aspect of the patella and becomes contiguous with the patellar tendon distally. The quadriceps tendon is a coalescence of the four muscles rather than four distinct layers. Quadriceps tears often extend medially and laterally through the patellar retinaculum, and these need to be included in the repair. The vastus intermedius inserts directly on the patella and is separate from the rectus femoris more proximally [28]. Three vascular arcades, medial, lateral, and peripatellar, provide blood supply to the quadriceps tendon. A hypo-vascular zone exists about 1-2 cm superior to the patella [25]. Yepes et al. has divided the Quadriceps tendon according to the zones of rupture. Zone 1 is within 1cm of the patellar, Zone 2 is between 1 and 2 cm, and Zone 3 is above this [25]. It is Zone 1 injuries that are technically difficult to repair and have poor healing, and this provides the focus of our study. We endeavoured to develop a technique using a strong small diameter suture with minimal biological reaction. Using a low profile whip stitch through the quadriceps tendon maximises proximal strength and utilises suture anchors in the patella as distal fixation. Angled anchor placement with the double-crossing of the sutures may optimise pull out strength. Crossover of the sutures may enhance biological repair across the patellar footprint. Secure fixation would facilitate early mobilisation and enhanced recovery. This study's objectives were to assess a double-crossed suture anchor technique's effectiveness in quadriceps tendon repair of acute Zone 1 injuries.
2. Materials and Methods
85 patients attended our institution for quadriceps tendon repair over an eight year period (2012-2019). All patients underwent ultrasound scanning of the extensor mechanism. The mean age was 56 with a range of 48 to 64 years. The male to female ratio was 8:1. Unilateral quadriceps tendon rupture was found in 98% of patients and mostly involved the non-dominant limb. The most common site of rupture was at the insertion of the tendon to the patella in Zone 1. Over 70 % of patients had co-morbidities, including diabetes mellitus, renal failure, obesity, gout, steroid and quinolone use. Over 60% of patients had a BMI of 28 or more. Twenty patients were included in the study. All patients had acute full-thickness tears in Zone 1 of the tendon. Exclusion criteria included Zone 2 or 3 tears and all partial tears. Previous knee surgery or arthroplasty, or a neuromuscular condition that may impact rehabilitation were also excluded.Post-operatively all patients participated in an accelerated rehabilitation protocol. The patients were followed up to one year post-operatively, and the follow-up visits were planned at 1,3,6 and 12 months. The patient demographics, clinical and radiological data and functional scores werecollected at each follow-up visit up to one year.
2.1 Case series
Twenty patients with isolated distal quadriceps tendon rupture were treated using a double-crossed suture anchor technique. All of them were male, with a mean age of 57. Mode of injury was eccentric forceful contraction of the quadriceps during a fall. The delay between the injury and surgery was a mean of 8.71 days (1-21 days). The body mass index (BMI) was a mean of 28.5 (23-32). Eighteen out of twenty patients had one or more predisposing factors: obesity, diabetes, chronic renal failure, corticosteroids and quinolone use. All patients had Plain X-Rays and Ultrasonography to confirm the diagnosis.
2.2 Surgical technique
The patient is painted and draped in a standard fashion with Chlorhexidine 2% and an Ioban 3M drape is used. A tourniquet is applied but not inflated. An 8 cm midline incision is made over the superior patella and quadriceps tendon with a size 22 blade. The haematoma is evacuated, and the tendon edge is freed up. Care is taken to identify the medial and lateral extension of the tear. A Krackow suture is placed into the lateral edge of the quadriceps tendon from distal to proximal with a single limb of a 2 Fibre wire (Arthrex) for a distance of 6 cm. The suture is then brought out distally through the tendon to finish in the midline. This is then repeated on the medial aspect of the tendon. One end of each suture is crossed over to the other side and clipped in place (Figure 1). The patella's superior edge is prepared, and two 2.4mm guide pins are drilled into the proximal patellar corners at an angle of 45 degrees to the midline to a depth of 25mm (Figure 2). The two guide pins are over drilled with a 4.5mm cannulated reamer to a depth of 25mm. The free ends of the Krackow sutures on each side are crossed over and passed through the eyelet of a 4.75mm SwiveLock and the suture/anchor is pushed into a drill hole until the eyelet is fully seated.
(Arthrex). Each side of the repair, medial and lateral has one suture tail in each of the two anchors.
Therefore, even if one anchor fails, the remaining anchor still retains the fixation of both sides.
The repair is tested for stability by knee flexion and the suture ends are trimmed (Figure 3).
The wound is closed in layers and the knee is immobilised in a hinged brace (Don Joy).
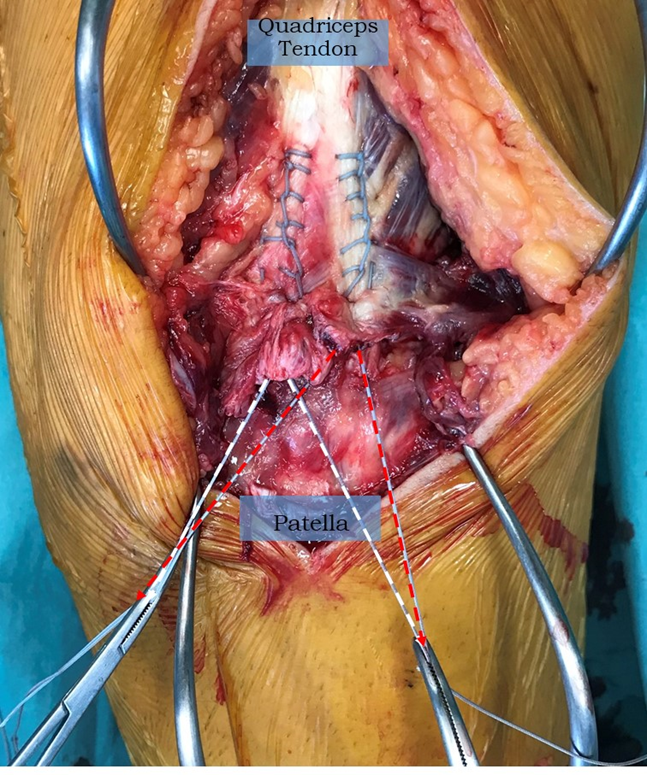
Figure 1: A Krackow suture (2 Fibrewire) has been passed up and then back down the medial aspect quadriceps tendon for 6 cm. The free ends are shown in white. This is repeated on the lateral side with another suture, the ends of which are shown in red. One suture end from each side is crossed over to join its twin.
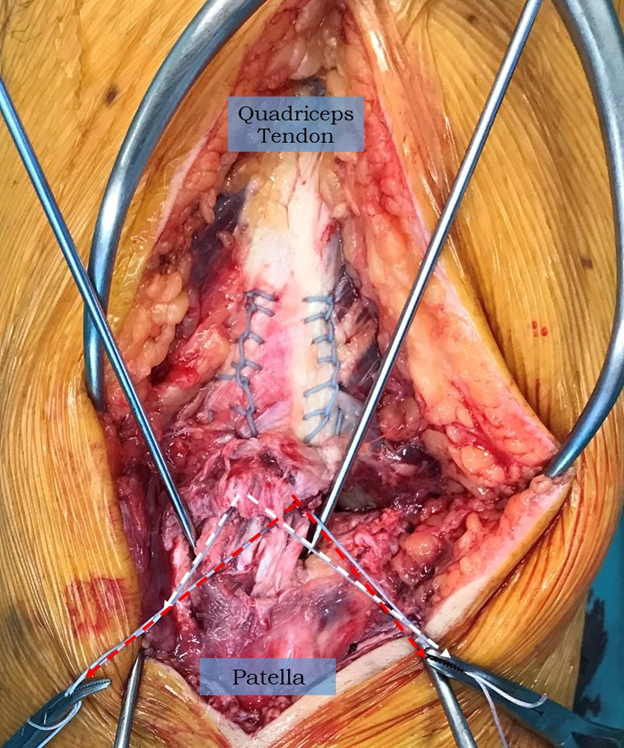
Figure 2: Two 2.4mm drill tip guides are placed on the superior aspect of the patella at a 450 angle to the coronal plane to a depth of 25mm. The two guide pins may then over drilled with a 4.5mm cannulated reamer to facilitate anchor fixation.
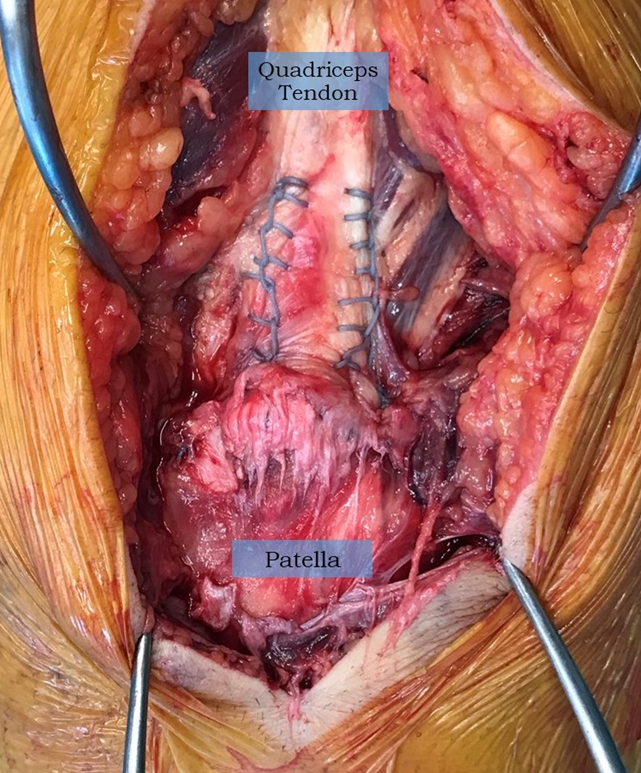
Figure 3: The completed repair with suture tails cut flush with the bone as part of knotless fixation. Each side of the repair, medial and lateral, has one suture tail in each of the two anchors. Therefore, even if one anchor fails, the remaining anchor still retains the fixation of both sides.
2.3 Rehabilitation protocol
Immediate protected weight-bearing was allowed post-operatively while using the splint. Isometric strengthening of the quadriceps started on the first post-operative day. Passive knee flexion 0-300 in the first two weeks and then increased to 0-600 in the next two weeks, and flexion range increased to 900 at six weeks. Partial to full weight-bearing was allowed at 8-10 weeks. Patients were allowed to return to work after three months and could participate in non-contact sports as desired. None of the patients played any contact sport.
2.4 Assessment method
The patient's overall subjective satisfaction, pain (VAS), knee range of motion and time to resume activities of daily living (ADL) were calculated at each follow-up visit. The Tegner [17], Cincinnati [18,19] and Lysholm scores were calculated.
3. Results
The mean operative time was 57 min (45-70 min). The average length of stay was three days. (2-3) There were no significant post-operative complications reported. The mean age was 56 (48-64), and they were all male. All twenty patients were followed prospectively for a mean of 12 months (10-14months). The mean active knee flexion was 1240(120-130). All patients were able to return to activities of daily living (ADL) with a mean of 2 months (1.5-3 months) and return to work at a mean of 06 months (4-8 months). (Table 1). The mean Tegner score at the latest follow up was 2.8 (0-5) versus 2.9 (0-5) before the rupture. The mean Cincinnati score was 79.2 (60-88) at the latest follow up versus 80.2 (62-90) before the rupture. The mean Lysholm score was 90 (70-100) at the latest follow up versus 95.2 (84-100) before the rupture. There was no re-tear reported at the latest follow up. (Table 2)
|
Enrolled Patients |
20 |
|
Age (mean) |
57.7 |
|
Gender |
Male |
|
BMI (kg/m2) |
28.5 |
|
Time to surgery |
8.71 days (1-21 days) |
|
Mean operative time |
57 min |
|
Average length of stay |
3 days |
|
Average Follow-up |
12 months |
|
Range of motion |
124 (120-130) |
|
ADL restarted |
2 months (1.5-3 months) |
|
Sports resumed |
6 months (4-8months) |
BMI: Body mass index
Table 1: Summary of patient characteristics
|
Scores |
Before injury |
Latest follow-up |
|
Tegner |
2.9 (0-5) |
2.8 (0-5) |
|
Cincinnati |
80.2 (62-90) |
79.2 (60-88) |
|
Lysholm |
95.2 (84-100) |
90(70-100) |
Table 2: Functional scores before the injury and last follow-up
4. Discussion
Quadriceps tendon rupture has an incidence of 1.37% per 100,000 per year [4], but there has been an increase in quadriceps tendon rupture treated surgically. The Finnish National Hospital discharge register reports the incidence of quadriceps tendon rupture increased by 411% from 0.55 to 2.82 per 100,000 people/year from 1997 to 2014. Surgical repair is required in complete full-thickness tears. Surgical complications include reduced knee flexion, quadriceps muscle atrophy, decreased patellar mobility, patellar stiffness and persistent pain [20]. Acute quadriceps tendons repair with the use of sutures through trans-osseous patellar bone tunnels is well established technique [3,21]. Maniscalco et al. published the first report of quadriceps tendon repair with suture anchors with mean knee flexion 0-1200 at two years follow up [12]. Richards and Barber reported a Lysholm score of 88 and a Tegner score of 2 in one patient after an 11-month follow-up with a mean knee flexion 00-1250 [11]. Bushnell et al. reported the mean knee flexion of 0-1300 with an 80% complete return to activities of daily living (ADL) [16]. Kerin et al. reported a complete return to sports activity after 8 months [23]. F. Mille et al. reported Tegner score of 2.8 and Cincinnati score of 79.5 with a return to daily activities (ADL) at 1.7 months and sports at 4.5 months [13]. (Table 3) Petri M and Dratzidis A et al.5 showed that suture anchor repairs of quadriceps tendon ruptures showed less gap formation during cyclic loading and sustained higher ultimate failure loads than trans-osseous suture repairs [5]. Ethibond sutures are commonly utilised, with an average diameter of #5 [20], and 5-throw knots optimise square knot security [27]. The knotted sutures can irritate the soft tissues and may loosen over time. The larger needle makes large holes in the native tendon. There is little evidence of osseointegration of the suture material in the bone tunnels, which may increase the risk of patellar fracture [22]. We used a smaller diameter suture with comparable strength to Ethibond, so a #2 fibre wire (Arthrex) was selected. This has high tensile strength and minimises tissue damage compared to ethibond [3]. The addition of a suture anchor for fixation allows for knotless technique and has been shown to have good to excellent pull out strength compared to trans-osseous repair [5]. A second suture with knotless anchor fixation provides additional strength to the repair and may facilitate early mobilisation and loading of the quadriceps mechanism. The fact that the sutures are crossed over means that failure of one anchor does not mean failure of the entire construct as each anchor contains a suture limb form both sides of the tendon. This is a technique that is popular in shoulder surgery [29]. As compared to the trans-osseous technique, the double suture anchor fixation involves smaller skin incision and less tissue trauma, shorter operative time, less soft tissue stripping and disruption of surrounding blood supply and improved healing rates [3]. Besides, there is a decreased risk of major complications, including patella fracture [11,22,24]. These potential advantages must be weighed against the cost-effectiveness of the procedure, which is in favour of the trans-osseous technique [11]. We evaluated the use of a knotless, crossed, double suture anchor fixation in quadriceps tendon repair. It is a safe and effective technique, and the clinical and radiological results are consistent with published studies.
|
References |
Number |
Follow-up (months) |
Score |
Range of motion |
ADL |
Sports |
|
Maniscalco et al. |
1 |
24 |
0-120 |
Yes |
Yes |
|
|
Richards and Barber |
2 |
11 |
L 88T 2 |
0-125 |
Yes |
|
|
Kerin et al. |
1 |
8 |
Complete |
8 months |
||
|
Bushnell et al. |
5 |
10.6 |
0-130 |
80% complete return |
||
|
Mille F et al. |
13 |
15 |
T 2.8 |
0-125 |
1.7 months |
4.5 months |
|
C 79.5 |
||||||
|
L 89.7 |
||||||
|
Current study |
20 |
12 |
T 2.8 |
0-124 |
2 months |
6 months |
|
C 79.2 |
||||||
|
L 90 |
L Lysholm, T Tegner, C Cincinnati
Table 3: Summary of the published studies where suture anchors were used to repair quadriceps tendon
Limitations
The small sample size and the lack of a control group are the main limitations of our study.
5. Conclusion
The double suture anchor fixation is a safe and effective novel treatment option in managing quadriceps tendon ruptures. Proposed benefits may include less tendon damage due to smaller diameter suture (2 Fibre wire). Crossing over the ends of the Krackow suture allows two anchor points for each side, medial and lateral. The 45-degree angle of the suture anchors may increase pull-out strength and facilitate enhanced recovery. The knotless technique may lessen knot irritation and reduce wound complications. Further studies are required to validate this hypothesis.
References
- Boublik M, Schlegel TF, Koonce RC, et al. (2013) Quadriceps tendon injuries in national football league players. Am J Sports Med 41 (2013): 1841-1846
- Boudissa M, Roudet A, Rubens-Duval B, et al. (2014) Acute quadriceps tendon ruptures: A series of 50 knees with an average follow-up of more than six years. Orthop Traumatol Surg Res 100 (2014): 213-216.
- Clayton RAE, Court-Brown CM. The epidemiology of musculoskeletal tendinous and ligamentous injuries. Injury 39 (2008):1338-1344.
- Petri M, Dratzidis A, Brand S, et al. Suture anchor repair yields better biomechanical properties than transosseous sutures in ruptured quadriceps tendon. Knee Surg Sports Traumatol Arthrosc 23 (2015): 1039-1045.
- Omar M, Haas P, Ettinger M, et al. Simultaneous bilateral quadriceps tendon rupture following long-term low-dose nasal corticosteroid application. Case Rep Orthop 12 (2013): 657-845
- Kazimoglu C, Yagdi S, Karapinar H, Sener M. Bilateral quadriceps tendon rupture and coexistent femoral neck fracture in a patient with chronic renal failure. Acta Orthop Traumatol Turc 41 (2007): 393-396.
- Kim BS, Kim YW, Song EK, et al. Simultaneous bilateral quadriceps tendon rupture in a patient with chronic renal failure. Knee Surg Relat Res 24 (2012):56-59.
- Herbort M, Raschke MJ. Ligament ruptures of the lower extremity in the elderly. Unfallchirurg 114 (2011): 671-680.
- Muratli HH, Celebi L, Hapa O, et al. Simultaneous rupture of the quadriceps tendon and contralateral patellar tendon in a patient with chronic renal failure. J Orthop Sci 10 (2005): 227-232.
- Richards DP, Barber FA. Repair of quadriceps tendon ruptures using suture anchors. Arthroscopy 18 (2002): 556-559.
- Maniscalco P, Bertone C, Bonci E. Titanium anchors for the repair of distal Achilles tendon ruptures: preliminary report of a new surgical technique. J Foot Ankle Surg 37 (1998): 96-100.
- Mille F, Adam A, Aubry S, et al. Prospective multicentre study of the clinical and functional outcomes following quadriceps tendon repair with suture anchors. Eur J Orthop Surg Traumatol 26 (2016): 85-92.
- Lynch AF, Rorabeck CH, Bourne RB. Extensor mechanism complications following total knee arthroplasty. J Arthroplasty 2 (1987): 135.
- Shah MK. Outcomes in bilateral and simultaneous quadriceps tendon rupture. Orthopedics 26 (2003): 797-798.
- Bushnell BD, Whitener GB, Rubright JH, et al. The use of suture anchors to repair the ruptured quadriceps tendon. J Orthop Trauma 21 (2007): 407-413.
- Howe TE, Dawson LJ, Syme G, et al. Evaluation of outcome measures for use in clinical practice for adults with musculoskeletal conditions of the knee: a systematic review. Man Ther 17 (2012): 100-118.
- Cincinnati Score-Orthopaedic Scores (2014).
- Agel J, LaPrade RF. Assessment of differences between the modified Cincinnati and International Knee Documentation Committee patient outcome scores: a prospective study. Am J Sport Med 37 (2009): 2151-2157.
- West JL, Keene JS, Kaplan LD. (2008) Early motion after quadriceps and patellar tendon repairs: Outcomes with single-suture augmentation. Am J Sports Med 36 (2008): 316-323.
- Ciriello V, Gudipati S, Tosounidis T, et al. Clinical outcomes after repair of quadriceps tendon rupture: a systematic review. Injury 43 (2012): 1931-1938.
- Lighthart WA, Cohen DA, Levine RG, et al. Suture anchor versus suture through tunnel fixation for quadriceps tendon rupture: a biomechanical study. Orthopedics 31 (2008): 441
- Kerin C, Hopgood P, Banks AJ. Delayed repair of quadriceps using the Mitek anchor system: a case report and review of the literature. Knee 13 (2006): 161-163.
- Harris JD, Abrams GD, Yanke AB, et al. Suture anchor repair of quadriceps tendon rupture. Orthopedics 37 (2014): 183-186.
- Yepes H, Tang M, Morris SF, et al. Relationship between hypovascular zones and patterns of rupture of the quadriceps tendon. J Bone Joint Surg Am 90 (2017): 2135-2141.
- Aleksi R, Juha P, Ville M, et al. The Increasing Incidence of Surgically Treated Quadriceps Tendon Ruptures. Knee Surg Sports Traumatol Arthrosc 27 (2019): 3644-3649.
- Omer AI , Shiraz AY, David MHo, et al. Security of Knots Tied With Ethibond, Fiberwire, Orthocord, or Ultrabraid.Am J Sports Med 36 (2008): 2407-2414.
- Reider B, Marshall JL, Koslin B, et al. The Anterior Aspect of the Knee Joint J Bone Joint Surg Am 63 (1981): 351-356.
- Connelly TM, Shaw A, O'Grady P. Outcome of open massive rotator cuff repairs with double-row suture knotless anchors: case series Int Orthop 39 (2015): 1109-1114.


 Impact Factor: * 4.2
Impact Factor: * 4.2 Acceptance Rate: 72.62%
Acceptance Rate: 72.62%  Time to first decision: 10.4 days
Time to first decision: 10.4 days  Time from article received to acceptance: 2-3 weeks
Time from article received to acceptance: 2-3 weeks 