Incidence of Neoplasms after Appendectomy in a Cohort of 1197 Patients
Stravodimos C1, Greiber A1, Riemenschneider F1, Popp A1, Schön MR1, Justinger C1,2
1Department of Surgery, Staedtisches Klinikum Karlsruhe, Karlsruhe, Germany
2Albert-Ludwigs-University Freiburg, Freiburg i.Br. Germany
*Corresponding Author: Justinger Christoph, Department of Surgery, Staedtisches Klinikum Karlsruhe, Karlsruhe, Germany
Received: 12 February 2021; Accepted: 19 February 2021; Published: 02 March 2021
Article Information
Citation: Stravodimos C, Greiber A, Riemenschneider F, Popp A, Schön MR, Justinger C. Incidence of Neoplasms after Appendectomy in a Cohort of 1197 Patients. Journal of Surgery and Research 4 (2021): 72-79.
View / Download Pdf Share at FacebookAbstract
Objective: Appendectomy is the gold standard in the treatment of acute appendicitis. The objective of this study was to investigate the incidence of unexpected histopathological findings after appendectomy in a large cohort of patients.
Methods: We retrospectively analyzed the demographic and histopathologic data of 1197 patients, who underwent an appendectomy in order to treat an initially diagnosed acute appendicitis between January 2012 and December 2017. Patients undergoing an appendectomy during other surgical procedures as well as patients under 18 years of age were excluded from the study.
Results: Out of 1197 patients in total who underwent an appendectomy, 1124 (93.9%) received a laparoscopic procedure and 73 (6.1%) underwent a conventional appendectomy. The obtained specimen presented with the following histopathological findings: 103 (8.6%) cases of catarrhal inflammation, 722 (60.3%) cases of suppurative acute appendicitis and 217 (18.1%) of gangrenous acute appendicitis. Furthermore, in 28 (2.3%) cases there were unexpected histopathological findings. Here, neoplasms were found in 25 (2.1%) cases: 16 cases of LAMN (low grade appendice
Conclusions: Unexpected histopathological findings in appendectomy specimens including neoplasms are not rare (2.3%). Histopathological assessment allows early diagnosis and treatment of these incidental findings.
Keywords
<p>Appendectomy; Appendicitis; Neoplasm</p>
Article Details
1. Introduction
Appendicitis is one of the most common causes in patients admitted to the emergency department with lower abdominal pain [1, 2]. The lifetime prevalence is 8.6% for males and 6.7% for females [3]. The prevailing cause leading to an inflammation of the appendix is the luminal obstruction. Provoking factors can be fecalith plugs, lymphoid hyperplasia, as well as other causing clinical symptoms and leading the patient to the emergency department [4]. The therapy of choice remains the laparoscopic or open appendectomy, allowing the subsequent histopathological examination of the specimens [4]. In the vast majority of cases, the operation leads to a fast and full recovery of the patient with low morbidity and mortality. In the recent years though, there is an open discussion regarding whether the antibiotic treatment and its effectiveness may be an alternative healing approach in case of uncomplicated acute appendicitis [5, 6]. However, underestimated causes for acute appendicitis are the appendiceal neoplasms including malignant diseases. Most of them are diagnosed unexpectedly after appendectomy for acute appendicitis. The number of these incidental findings including mucinous neoplasms, carcinoid tumor, adenocarcinoma, granulomatous diseases, enterobiasis, taeniasis, ascariasis, diverticulitis, primary or secondary adenocarcinoma, lymphoma and neurogenic appendicopathy is unclear, but is relevant due to the large number of appendectomies being performed.
In addition, the incidental finding of a malignant neoplasia can have considerable consequences for the patient´s prognosis and the further treatment strategy.
This study was designed to investigate the incidence of unexpected appendiceal neoplasms after appendectomy in a large cohort of patients undergoing surgery due to acute appendicitis.
2. Materials and Methods
We retrospectively analyzed the demographic and histopathologic data of 1197 patients, who underwent appendectomy to treat an initial diagnosis of acute appendicitis at the Karlsruhe State Hospital between January 2012 and December 2017. Patients, undergoing appendectomy during other surgical procedures as well as patients under 18 years of age, were excluded from the study.
Surgical treatment was performed as open or laparoscopic appendectomy.
Tissue from surgical resections was fixed in formalin. Representative samples were collected from the fixed tissue. The sections were stained with haematoxylin and eosin (HE) and mounted on microscope slides using standard techniques.
According to the histopathological examination, the specimens were classified either as positive or negative for acute appendicitis. The specimens were further classified according to the grade and severity of the inflammation. Neoplasms were classified according to the tumor entity and grading. Patients with neoplasms were further classified according to age, ASA classification, performed imaging such as ultrasound or computed tomography prior to surgery.
3. Results
Between January 2012 and December 2017, 1197 patients with clinical signs of an acute appendicitis were treated at the Department of Surgery of the State Hospital Karlsruhe. The patient´s characteristics are shown in table 1.
|
Characteristic |
Number |
|
Gender male/ female |
675 (56.4%) / 522 (43.6%) |
|
Age |
67.5 (18 – 86) |
|
BMI |
24.8+/- 2.7 |
|
ASA-Score |
2.2+/-1 |
|
Type of operation |
|
|
Conventional appendectomy |
73 (6.1%) |
|
Laparoscopic appendectomy |
1124 (93.9%) |
|
Perforated appendicitis |
187 (15.6%) |
|
Appendiceal neoplasm |
25 (2.1%) |
Table 1: Characteristics of 1197 patients who underwent appendectomy between January 2012 and December 2017.
Intraoperatively, one hundred eighty-seven patients (15.6%), showed a perforation of the appendix and 67 of those showed a generalized peritonitis. 1124 (93.9%) operations were performed laparoscopically and 73 (6.1%) patients underwent a conventional appendectomy.
3.1 Histopathological analysis
The histopathological examination of the specimens showed unexpected findings in 28 patients (2.3%) (3 benign lesions and 25 neoplasms). One hundred three patients (8.6%) had a catarrhal appendicitis, 217 patients (18.1%) a gangrenous appendicitis and 722 patients (60.3%) a suppurative appendicitis, while 155 patients (12.9%) had histopathological findings of a chronic appendicitis with signs of fibrosis or no signs of an inflammation. Figure 1 shows the severity of appendicitis according to the histopathological findings.
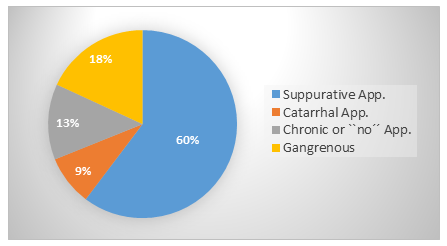
Figure 1: Histological type and severity of acute appendicitis of the 1197 patients.
3.2 Neoplasms of the appendix
Neoplasms were found in 25 (2.1%) cases (Figure 2): 16 cases of LAMN (low grade appendiceal mucinous neoplasms), 7 neuroendocrine tumors, 1 lymphoma, 1 adenocarcinoma. The characteristics of the patients with neoplasms are shown in table 2. Statistically there was no significant difference between male and female patients and most patients were classified ASA II (9), with a mild systemic disease.

Figure 2: Histologic types of unexpected neoplasms of the appendix.
|
Characteristic |
Number |
|
Gender male/ female |
13-Dec |
|
Age |
|
|
<30 years |
1 |
|
30-50 years |
7 |
|
50-70 years |
6 |
|
>70 years |
11 |
|
ASA II |
9 |
|
Acute abdomen |
19 |
|
Pre-surgery CT scan |
3 |
Table 2: Characteristics of the 25 patients with unexpected histopathological findings after appendectomy.
It is noteworthy that neoplasms were diagnosed in patients of all ages: One of the 25 patients was younger than 30 years, 7 patients between 30-50 years of age, 6 patients between 50-70 years and 11 patients were over 70 years old.
Nineteen of the patients with appendiceal neoplasms were admitted with clinical symptoms of an acute abdomen, while all patients showed intraoperative signs of an acute appendicitis.
In three cases a computed tomography was performed prior to surgery, after a suspicious conglomerate was detected during sonographic examination of the abdomen. The computed tomography confirmed our primary diagnosis.
4. Discussion
Acute appendicitis is one of the most common causes leading patients with abdominal pain to emergency departments [2-10]. The lifetime prevalence is 7% and appendectomy is one of the most common performed operations worldwide [3-11]. In Germany about 130.000 appendectomies are performed annually, with our department performing about 200 each year [12]. The lifetime incidence of appendicitis for males is estimated to be 8.6% and 6.7% for females, while the incidence of appendectomy for females is estimated around 12% and for males 23% [13, 14, 15].
Appendicitis is diagnosed and the indication for surgery is based on the patient’s medical history, clinical examination and laboratory findings. A helpful diagnostical tool is the abdominal ultrasound, and sometimes the computed tomography, the magnetic resonance tomography and the diagnostic laparoscopy [17, 18]. This allowed a reduction of diagnostical errors and enabled an optimized therapeutical approach regarding the underlying cause of the disease. Nevertheless, the rate of appendectomies in which no signs of inflammation are found in histological specimens are estimated to be between 9% and 35% [13, 14, 15, 16]. In the current study 12.9% (155 patients) of the appendiceal specimens showed no signs of acute appendicitis or signs of a chronic appendicitis.
While surgery with the resection of the inflamed appendix is the standard therapy for acute appendicitis, there is an increasing discussion, whether the antibiotic treatment and its effectiveness could be an alternative treatment in case of uncomplicated acute appendicitis [5, 6]. Various arguments certainly play a role in the discussion about the conservative therapy of appendicitis. Even though appendectomy is a safe standard procedure, every surgical procedure is associated with a certain morbidity and mortality (in hospital mortality of appendectomies in Germany: 0.2% [19]). Arguments for the surgical therapy of acute appendicitis are the recurrence rates after a conservative treatment (approximately 15%) [20]. Furthermore the results presented in this study should be taken into account. In our study population, 25 patients were diagnosed with unexpected appendiceal neoplasms (2.1%).
The majority of these patients presented with typical signs of an acute appendicitis. It is remarkable, that appendiceal neoplasms were found in patients of all ages. This is important, as the unexpected histopathological findings might pose a therapeutic challenge. In literature appendiceal tumors have been reported in <3% of all appendectomy specimens [21]. In the current study 25 patients with appendiceal neoplasms (2.1%) were detected. All patients showed intraoperative signs of an acute appendicitis. In the following, the histopathological findings are presented in detail.
- Sixteen of the patients (1.3%) have been diagnosed with a low grade appendiceal mucinous neoplasm. Appendiceal neoplasms are rare, accounting for <1% of all cancers. Appendiceal mucinous neoplasms rarely develop metastases outside the peritoneal cavity. They are differentiated according to the American Joint Committee on Cancer according to their histological grade (high or low) [22]. Their clinical course depends on the stage of disease at diagnosis, with well differentiated mucinous neoplasms having a better prognosis than the poorly differentiated ones. In the current study all patients showed a well-differentiated appendiceal mucinous neoplasm. The therapy of choice is the appendectomy, the ileocecal resection or a hemicolectomy with performance of an additional intraperitoneal hyperthermic chemoperfusion (HIPEC), depending on the presence of a pseudomyxoma peritonei [23]. In our cohort, five out of 16 patients (31.2%) with mucinous neoplasms showed a perforated appendix. Two patients with the presence of pseudomyxoma peritonei underwent a right hemicolectomy with additional HIPEC, while 3 patients with no affected margins or lymphatic invasion underwent a close clinical follow up.
- Seven patients (0.58%) were diagnosed with a neuroendocrine tumor. Neuroendocrine tumors of the appendix account for almost 60% of all appendiceal neoplasms. According to the literature, 70-95% of the cases are <1cm and are found at the tip of the appendix [4]. The therapy of choice for tumors <1cm is the appendectomy, while the recommended therapy for tumors >2cm is the right hemicolectomy [4, 7]. Six of our patients with a neuroendocrine tumor of the appendix underwent a right hemicolectomy, while one patient with a tumor <1cm at the tip of the appendix underwent an appendectomy combined with a close clinical follow up.
III. One patient was diagnosed with a lymphoma. It was specified as a mantle cell lymphoma and the patient had no prior history of lymphoma. Thirty percent of extranodal non-Hodgkin lymphomas can occur in the gastrointestinal system. Mantle cell lymphomas can occur in around 25% [24, 25].
- One patient was diagnosed with an adenocarcinoma of the appendix classified as colonic type arising from preexisting adenomas. Adenocarcinoma is thought to be the most common type of primary appendix cancer, constituting for 60% of the cases [26].
In summary, our data underlines the importance of the histological examination of surgical specimens following appendectomy. Even if unexpected findings of malignant appendiceal tumors seem to be rare, their number is relevant due to the high number of patients operated for acute appendicitis annually. Because patients with appendiceal neoplasms do not develop specific symptoms, they present a diagnostic challenge that every surgeon should be aware of.
5. Conclusion
Unexpected histopathological findings including neoplasms in appendectomy specimens are not rare (2.3%). Histopathological assessment allows an early diagnosis and therapy of these incidental findings.
References
- Fagerstrom A, Paajanen P, Saarelainen H, Ahonen-Siirtola M, Ukkonen M, Miettinen P, et al. Non- specific abdominal pain remains as he most common reason for acute abdomen: 26-year retrospective audit in one emergency unit. Scand J Gastroenterol 52 (2017): 1072-1077.
- Cervellin G, Mora R, Ticineci A, Meschi T, Comelli I, Catena F, et al. Epidemiology and outcomes of acute abdominal pain in a large urban emergency department: retrospective analysis of 5340 cases. Ann Transl Med 4 (2016): 362-370.
- Addiss DG, Shaffer N, Fowler BS, Tauxe RV. The epidemiology of appendicitis and appendectomy in the United States. Am J Epidemiol 132 (1990): 910-925.
- Akbulut S, Tas M, Sogutcu N, Arikanoglu Z, Basbug M, Ulku A, et al. Unusual histopathological findings in appendectomy specimens: a retrospective analysis and literature review. World J Gastroenterol 17 (2011): 1961-1970.
- Prechal D, Post S, Pechlivanidou I, Ronellenfitsch U. Feasibility, acceptance, safety, and effectiveness of antibiotic therapy as alternative treatment approach to appendectomy in uncomplicated acute appendicitis. International Journal of Colorectal Disease.
- Sallinen V, Akl EA, You JJ, Agarwal A, Shoucair S, Vandvik PO, et al. Meta-analysis of antibiotics versus appendicectomy for non-perforated acute
- Duzgun AP, Moran M, Uzun S, Ozmen MM, Ozer VM, Seckin S, et al. Unusual findings in appendicectomy specimens: Evaluation of 2458 cases and review of the literature. Indian J Surg 66 (2004): 221-226.
- Harminder Singh, Ananda S, Koomson, Kathleen M, Decker Jason Park, Alain Demers. Continued increasing incidence of malignant appendiceal tumors in Canada and the United States: A population-based study.
- Daniel John Doyle, Amandeep Goyal, Pankaj Bansal, Emily H. American Society of Anesthesiologists Classification
- Prechal D, Damirov F, Grilli M, Ronellenfitsch U. Antibiotic therapy for acute uncomplicated appendicitis: a systematic review and meta-analysis. Int J Color Dis 34 (2019): 963-971.
- Podda M, Cillara N, Di Saverio S, Lai A, Feroci F, Luridiana G, et al. Antibiotics-first strategy for uncomplicated acute appendicitis in adults is associated with increased rates of peritonitis at surgery. A systematic review with meta-analysis of randomized controlled trials comparing appendectomy and non-operative management with antibiotics. 15 (2017): 303-314.
- Büchler MW, Wente MN. Current surgical value of diagnostics and therapy standards. Der Chirurg 80 (2009): 577-578.
- Zdichavsky M, Gögele H, Blank G, Kraulich M, Meile T, von Feilitzsch M, Histological characterization of appendectomy specimens with intraoperative appearance of vascular injection. Surg Endosc 27 (2013): 849-853.
- Khairy G, Acute appendicitis: is removal of a normal appendix still existing and can we reduce its rate? Saudi J Gastroenterol 15 (2009): 167-170
- Seetahal SA, Bolorunduro OB, Sookdeo TC, Oyetunji TA, Greene WR, Frederick W. Negative appendectomy: a 10 year review of a nationally representative sample. Am J Surg 201(2011): 433-437.
- Chandrasegaram MD, Rothwell LA, An El, Miller RJ. Pathologies of the appendix: a 10 year review of 4670 appendicectomy specimens. ANZ J Surg 82 (2012): 844-847.
- Brown MA. Imaging acute appendicitis. Semin Ultrasound CT MR 29 (2008): 293-307.
- Jain RK, Jain M, Rajak CL, Mukherjee S, Bhattacharyya PP, Shan MR. Imaging in acute appendicitis: a review. Indian J Radio Imaging 16 (2006): 523-532.
- Baum P, Diers J, Lichthardt S, Kastner C, Schlegel N, Germer CT, et al. Mortality and Complications Following Visceral Surgery: A Nationwide Analysis Based on the Diagnostic Categories Used in German Hospital Invoicing Data. Dtsch Arztebl Int 116 (2019): 739-746.
- Kaminski A, Liu IL, Applebaum H, Lee SL, Haigh PI. Routine interval appendectomy is not justified after initial nonoperative treatment of acute appendicitis. Arch Surg 140 (2005): 897–901.
- Yilmaz M, Akbulut S, Kutluturk K, Sahin N, Arabaci E, Ara C, Yilmaz S Unusual histopathological findings in appendectomy specimens from patients with suspected acute appendicitis. World J Gastroenterol 19 (2013): 4015-4022.
- Kaitlyn J. Management of appendix cancer. Clin Colon Rectal Surg 28 (2015): 247-55.
- Foster JM, Gupta PK, Correan JH, Grotz TE, Blas JV, Right Hemicolectomy is not routinely indicated in Pseudomixoma peritonei. Ann Surg78 (2012): 171-177.
- D’Amore F, Brincker H, Gronbaek K, Thorling K, Pedersen M, Jensen MK, et al. Non-Hodgkin’s lymphoma of the gastrointestinal tract: a population-based analysis of incidence, geographic distribution, clinicopathologic presentation features, and prognosis. Danish Lymphoma Study Group. J Clin Oncol 12 (1994): 1673- 1684.
- Romaguera JE, Medeiros LJ, Hagemeister FB, Fayad LE, Rodriguez MA, Pro B, et al. Frequency of gastrointestinal involvement and its clinical significance in mantle cell lymphoma. Cancer 97 (2003): 586-591.
- McCusker ME, Coté TR, Clegg LX, Sobin LH. Primary malignant neoplasms of the appendix: a population-based study from the surveillance, epidemiology and end-results program, 1973-1998. Cancer 94 (2002): 3307-3312.


 Impact Factor: * 4.2
Impact Factor: * 4.2 Acceptance Rate: 72.62%
Acceptance Rate: 72.62%  Time to first decision: 10.4 days
Time to first decision: 10.4 days  Time from article received to acceptance: 2-3 weeks
Time from article received to acceptance: 2-3 weeks 