Inflammatory Fibroid Polyp of ileum causing Ileo-Ileal intussusception in a 38 year old female : A case report
Utpal Baruah*, Subbarao, Azharuddin
Department of General Surgery, Nemcare Hospital Private Limited, Guwahati, Assam, India, 781005
*Corresponding author: Utpal Baruah, Department of General Surgery, Nemcare Hospital Private Limited, Guwahati, Assam, India, 781005
Received: 29 May 2021; Accepted: 07 June 2021; Published: 10 June 2021
Article Information
Citation: Utpal Baruah, Subbarao, Azharuddin. Inflammatory Fibroid Polyp of ileum causing Ileo-Ileal intussusception in a 38 year old female: A case report. Journal of Surgery and Research 4 (2021): 308-314.
View / Download Pdf Share at FacebookAbstract
Adult intussusception is a rare entity that is almost always associated with a demonstrable lead point. There has been a notable association between adult intussusception and inflammatory fibroid polyp (IFP) or Vanek’s tumour. These polyps are benign tumours arising from submucosa, comprising of mesenchymal cells like fibroblasts and numerous variably prominent small blood vessels along with chronic inflammatory cells commonly eosinophils. Inflammatory fibroid polyps are uncommon; moreover, these polyps causing secondary intussusception in an adult is still rarer. Clinical manifestations of IFP vary based on size and location within the GI tract. Here, we report a case of inflammatory fibroid polyp of ileum, presented as acute on chronic pain abdomen in a 38-year-old woman. The rareness of the disease made it a clinical challenge to subject the patient to laparotomy. However this patient underwent resection of the intussuscepted small bowel with primary anastomosis. The rareness of non-malignant condition being the cause for adult ileo-ileal intussusception and the clinical challenge associated with it makes it a case worth reporting.
Keywords
Inflammatory Fibroid Polyp, Ileo-Ileal intussusceptions, Vanek's Tumor
Inflammatory Fibroid Polyp articles; Ileo-Ileal intussusceptions articles; Vanek's Tumor articles
Inflammatory Fibroid Polyp articles Inflammatory Fibroid Polyp Research articles Inflammatory Fibroid Polyp review articles Inflammatory Fibroid Polyp PubMed articles Inflammatory Fibroid Polyp PubMed Central articles Inflammatory Fibroid Polyp 2023 articles Inflammatory Fibroid Polyp 2024 articles Inflammatory Fibroid Polyp Scopus articles Inflammatory Fibroid Polyp impact factor journals Inflammatory Fibroid Polyp Scopus journals Inflammatory Fibroid Polyp PubMed journals Inflammatory Fibroid Polyp medical journals Inflammatory Fibroid Polyp free journals Inflammatory Fibroid Polyp best journals Inflammatory Fibroid Polyp top journals Inflammatory Fibroid Polyp free medical journals Inflammatory Fibroid Polyp famous journals Inflammatory Fibroid Polyp Google Scholar indexed journals Ileo-Ileal intussusceptions articles Ileo-Ileal intussusceptions Research articles Ileo-Ileal intussusceptions review articles Ileo-Ileal intussusceptions PubMed articles Ileo-Ileal intussusceptions PubMed Central articles Ileo-Ileal intussusceptions 2023 articles Ileo-Ileal intussusceptions 2024 articles Ileo-Ileal intussusceptions Scopus articles Ileo-Ileal intussusceptions impact factor journals Ileo-Ileal intussusceptions Scopus journals Ileo-Ileal intussusceptions PubMed journals Ileo-Ileal intussusceptions medical journals Ileo-Ileal intussusceptions free journals Ileo-Ileal intussusceptions best journals Ileo-Ileal intussusceptions top journals Ileo-Ileal intussusceptions free medical journals Ileo-Ileal intussusceptions famous journals Ileo-Ileal intussusceptions Google Scholar indexed journals Vanek's Tumor articles Vanek's Tumor Research articles Vanek's Tumor review articles Vanek's Tumor PubMed articles Vanek's Tumor PubMed Central articles Vanek's Tumor 2023 articles Vanek's Tumor 2024 articles Vanek's Tumor Scopus articles Vanek's Tumor impact factor journals Vanek's Tumor Scopus journals Vanek's Tumor PubMed journals Vanek's Tumor medical journals Vanek's Tumor free journals Vanek's Tumor best journals Vanek's Tumor top journals Vanek's Tumor free medical journals Vanek's Tumor famous journals Vanek's Tumor Google Scholar indexed journals primary anastomosis articles primary anastomosis Research articles primary anastomosis review articles primary anastomosis PubMed articles primary anastomosis PubMed Central articles primary anastomosis 2023 articles primary anastomosis 2024 articles primary anastomosis Scopus articles primary anastomosis impact factor journals primary anastomosis Scopus journals primary anastomosis PubMed journals primary anastomosis medical journals primary anastomosis free journals primary anastomosis best journals primary anastomosis top journals primary anastomosis free medical journals primary anastomosis famous journals primary anastomosis Google Scholar indexed journals Inflammatory fibroid polyps articles Inflammatory fibroid polyps Research articles Inflammatory fibroid polyps review articles Inflammatory fibroid polyps PubMed articles Inflammatory fibroid polyps PubMed Central articles Inflammatory fibroid polyps 2023 articles Inflammatory fibroid polyps 2024 articles Inflammatory fibroid polyps Scopus articles Inflammatory fibroid polyps impact factor journals Inflammatory fibroid polyps Scopus journals Inflammatory fibroid polyps PubMed journals Inflammatory fibroid polyps medical journals Inflammatory fibroid polyps free journals Inflammatory fibroid polyps best journals Inflammatory fibroid polyps top journals Inflammatory fibroid polyps free medical journals Inflammatory fibroid polyps famous journals Inflammatory fibroid polyps Google Scholar indexed journals Adult intussusception articles Adult intussusception Research articles Adult intussusception review articles Adult intussusception PubMed articles Adult intussusception PubMed Central articles Adult intussusception 2023 articles Adult intussusception 2024 articles Adult intussusception Scopus articles Adult intussusception impact factor journals Adult intussusception Scopus journals Adult intussusception PubMed journals Adult intussusception medical journals Adult intussusception free journals Adult intussusception best journals Adult intussusception top journals Adult intussusception free medical journals Adult intussusception famous journals Adult intussusception Google Scholar indexed journals
Article Details
1. Introduction
Adult intussusception is relatively rare, constituting only 1-5% of patients with bowel obstructions [1]. Adult intussusceptions represent 5% of all intussusceptions, as most cases occur in the pediatric population.The cause of intussusception in children differs from that of adults. Adult intussusception is mostly caused by tumors and 80- 90% of the tumors associated with small bowel intussusception are benign [2]. Lipoma is the most common benign tumor in intussusception. Inflammatory fibroid polyps rarely cause ileal intussusception. Clinical manifestations of IFP depend largely on size and location, but most commonly include intestinal obstruction, abdominal pain, intussusception, and rarely GI bleeding. Here, we report an unusual case of Ileo-ileal intussusception caused by an inflammatory fibroid polyp. Inflammatory fibroid polyp (IFP) is a rare benign solitary lesion that arises from the submucosa of the gastrointestinal tract (GIT) [3]. In 1949, Vanek first described the lesion as an eosinophilic submucosal granuloma [4]. The occurrence of IFP along the GIT is as follows: 66-75% of the cases occur in the gastric antrum; 18-20% of the cases occur in the small intestine; 4-7% of the cases occur in the large intestine; 1% occurs in the duodenum, esophagus, and gallbladder; and less than 1% involves the appendix [4,5]. However, the ileal segment is the most common site where these polyps cause intussusceptions [6]. IFPs can be found in all age groups, but peak incidence is between the sixth and seventh decades with a slight preponderance in males [3-5]. The estimated incidence of IFP in the general population is 0.3 to 0.5% [7].
2. Case Presentation
A 38 year old female presented to our hospital with complaints of pain in the epigastric region on and off for the last 2 months and also complains of pain in the left pelvic region occasionally. Patient was apparently well 2 months ago when she experienced the first episode of pain in the epigastric region, which is mild aching in character and non radiating. There is no history of vomiting & fever. H/O of intermittent constipation present. No history of bleeding per rectum and no alteration in stool consistency. she is a known case of hypothyroidism on irregular medication, stopped 2 months back, not diabetic, not hypertensive, no past history of bronchial asthma & Pulmonary TB LMP -Irregular cycles, & Menorrhagia +nt On Per abdominal examination
- On Inspection there is no obvious distention, no visible peristalsis
- On palpation abdomen was soft, tenderness on deep palpation in right lower quadrant with a palpable mass & a well defined mobile lesion with smooth surface was noted in the left pelvic region
- On auscultation increased bowel sounds were
The provisional diagnosis was Mass in RLQ with Left Ovarian Cyst USG Abdomen revealed a large Left Ovarian Cyst and soft tissue lesion in distal ileal segment
CT of the abdomen and pelvis with intravenous contrast revealed (Figures 1 and 2)
- Well defined left ovarian cystic lesion with internal septations
- Lobulated soft tissue lesion in ileal loops with associated intussusception & soft tissue stranding in the adjacent omentomesentery - ? Malignant
No nidus or lead point for the intussusception could be clearly identified on imaging.
3. No evidence of ascites or retroperitoneal adenopathy
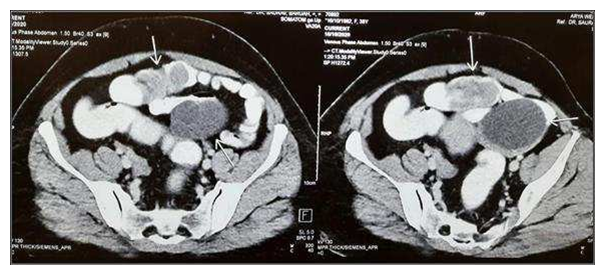
Figure 1: Axial CT revealing Intussusception & Left Ovarian cyst
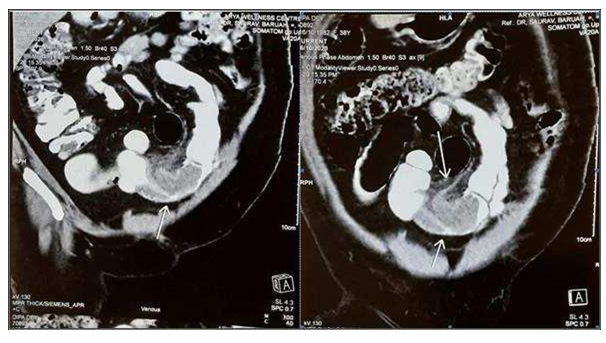
Figure 2: Coronal CT revealing Intussusception & Left Ovarian Cyst
2.1 Treatment
Patient was given conservative management by keeping nil per oral, IV fluids as per requirement, basic antibiotics and analgesics. As the pain did not get relieved and CT abdomen revealed a suspected malignant lesion associated with intussusception & a ovarian cyst, patient was taken up for exploratory laparotomy.
2.2 Intra operative findings
- A well encapsulated Ovarian cyst with smooth outer surface of about 8×6 cm size was noted in Left ovary, This cyst was resected by ovariotomy
- Ileo-ileal intussusception about 60 cm away from the ileocecal .
- No evidence of enlarged mesenteric lymph nodes
- The resected part was cut open which showed a single polyp measuring about 5×5×3cm was
2.3 On Histopathological examination
2.3.1 Gross Examination
- Specimen 1: ovarian cyst measures 8*6*4 cm, it is well encapsulated with smooth outer surface. Cut section shows unilocular acvity filled with clear
- Specimen 2: segment of ileum shows polypoid mass measuring 5*5*3 cm.overlying mucosa is ulcerated. It is connected to bowel wall by athich stalk. Rest of the bowel mucosa is grossly unremarkable
2.3.2 Microscopic examination
- Specimen 1: sections show fibrocollagenous cyst wall focally lined by single layer of low columnar to cuboidal No atypia is seen.
- Specimen 2: shows a polypoidal submucosal lesion composed of bland spindle to stellate shaped cells set in a myxoid and vascularised the stroma also shows infiltrates of lymphocytes and numerous eosinophills. No atypia is seen.overlying mucosa is ulcerated at places the lesion is involving the bowel wall transmurally. Resected margins are with in normal limit.
The above findings are consistent with serous cystadenoma of ovary & inflammatory fibroid polyp of ileum
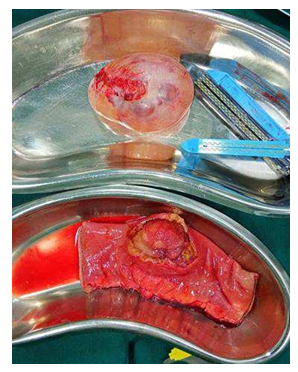
Figure 3: Ovarian Cyst after Ovariotomy & Intraluminal Tumour in the resected segment of ileum
3. Discussion
In 1949, Vanek first described the lesion as an eosinophilic submucosal granuloma. Whereas the term IFP was first proposed by Helwig and Ranier in 1953 for gastric polyps; since then, it has gained acceptance for similar lesions throughout the GIT [4,8]. For a couple of decades, IFPs have been considered as reactive changes of the lining mucosa of the GIT. The discovery of PDGFRA mutation signatures in IFPs has helped to unveil their neoplastic nature [9]. IFPs are always asymptomatic, and they remain silent for a long time without being diagnosed. Incidentally, they may be diagnosed during laparoscopic or endoscopic examination due to other underlying gastrointestinal (GI) medical conditions. If the lesion is symptomatic, it typically presents during the 6th or 7th decade, but there have been reports of young adults with chronic manifestations such as weight loss and intermittent constipation [21]. As they become clinically detectable, the signs and symptoms usually depend on two factors: location and size of the tumour [10]. Studies have shown that IFPs that involve stomach present with abdominal pain, whereas those with small bowel involvement often present with intussusception and obstruction [11]. Moreover, vomiting, diarrhea, tenesmus, and alterations in bowel habits are also seen although their frequencies are low. Larger polyps tend to erode and ulcerate superficially and lead to bloody stool. Patients with IFPs in the small bowel are most likely to present with chronic episodes of colicky abdominal pain, lower GI bleeding, anemia, and, more rarely, intestinal obstruction due to episodes of intestinal intussusception and rarely with necrosis and perforation [12]. Although malignant diseases represent the major causes of intussusceptions in adults, there are few reports of intestinal obstruction and perforation caused by IFPs. Preoperative diagnosis of intussusceptions is rare but can occur in finding a palpable mass on the abdomen with the use of imaging techniques. The etiopathogenesis of IFPs is unknown. Hypotheses have been postulated in the attempt to explain the cause of IFPs such as foreign body, parasites, and chronic H. pylori infection which have been suggested but remain unsupported [13]. Localized variant of eosinophilic gastroenteritis is another proposed aetiology due to frequent observation of a marked eosinophilic infiltration in most cases [9]. It was not possible to ascertain the predisposing factors that were associated with the development of this ileo- ileal IFP in our case. Our case indicates that this condition has to be considered not only in elderly patients with features of chronic abdominal pain, vomiting, and frequent distension of the abdomen, but also in adult patients with acute on chronic pain abdomen. Abdominal CT is currently considered the most sensitive imaging diagnostic technique to show the polyp or to confirm intussusception [14]. Most IFPs can be resected endoscopically. Only rarely surgery is needed. IFPs arising below the Treitz ligament can present with an acute abdomen usually due to intussusception. Exploratory laparoscopy or laparotomy is frequently recommended as the best treatment for intussusceptions caused by IFP. The operation should be performed as early as possible in order to prevent the intussusceptions from leading to ischemia, necrosis, and subsequent perforation of the invaginated bowel segment [15]. Most IFPs are positive for CD34, whereas about 10%-20% of cases show focal reactivity for SMA and desmin. C-KIT (CD117), DOG1, and S-100 are consistently negative [16]. Although IFPs are biologically regarded as benign and noninvasive lesions [17], few cases have been observed to invade the muscularis propria layer [18]. With regard to gastric IFPs, only three invasive cases have been reported in the literature described in 2015 [19,20].
4. Conclusion
Although Vanek's tumor is a rare entity, it should be considered as a differential diagnosis in every case of intussusception in an adult. This case report demonstrates the possibility of benign inflammatory lesion causing secondary intussusception. IFP of small intestine is not fatal and patients remain asymptomatic in their daily life except for intussusception or bowel obstruction. Also, deligent clinical evaluation still determines the decision of subjecting the patient to surgery.
Ethical approval
Institutional and international research regulations were observed during the time of interacting with the patient and the preparation of the manuscript.
Consent
A written informed consent was obtained from the patient for the case details to be published, and it has been kept by the corresponding author.
Conflicts of interest
The authors declare that there are no conflicts of interest regarding the publication of this article.
References
- Azar T, Berger Adult intussusception. Ann Surg. 226 (1997): 134-138.
- Yakan S, Caliskan C, Makay O, et Intussusception in adults: clinical characteristics, diagnosis and operative strategies. World J Gastroenterol 15 (2009): 1985-1989.
- Jan JU, Muslim M, Ullah Vanek's tumor as an unusual cause of ileo-ileal intessuception - A unique case report. Annals of medicine and surgery 32 (2018): 14-17.
- Van Gastric submucosal granuloma with eosinophilic infiltration. The American journal of pathology 25 (1949): 397-411.
- Talukder MRH, Alam MNA, Uddin Jejunal inflammatory fibroid polyp: a rare cause of intussusception. Ibrahim Medical College Journal 9 (2015): 58-60.
- Zinkiewicz K, Zgodziñski W, Browski AD, et Recurrent inflammatory fibroid polyp of cardia: a case report. World journal of gastroenterology 10 (2004): 767-768.
- Jabar MF, Prasannan S, Gul Adult intussusception secondary to inflammatory polyps. Asian Journal of Surgery 28(2005): 58-61.
- Daum O, Hatlova J, Mandys V. Comparison of morphological, immunohistochemical, and molecular genetic features of inflammatory fibroid polyps (Vanek's tumors). Virchows Archiv 456 (2010): 491-497.
- Nonose R, Valenciano JS, da Silva CMG, et Ileal intussusception caused by Vanek's tumor: a case report. Case Reports in Gastroenterology 5 (2011): 110-116.
- Tabrizian P, Nguyen SQ, Greenstein A, et al. Significant parameters for surgery in adult Surgery 147 (2010): 227-232.
- Huss S, Wardelmann E, Goltz D, et Activating PDGFRA mutations in inflammatory fibroid polyps occur in exons 12, 14 and 18 and are associated with tumour localization. Histopathology 61 (2012): 59-68.
- Cawich S, Gibson T, Mitchell D, et al. Adult intussusception from an inflammatory fibroid polyp: a case report and review of the The Internet Journal of Pathology 7 (2008) 1-10.
- Wysocki P, Taylor G, Windsor Inflammatory fibroid polyps of the duodenum: a review of the literature. Digestive Surgery 24 (2007) 162-168.
- Rehman S, Gamie Z, Wilson TR, et Inflammatory fibroid polyp (Vanek's tumour), an unusual large polyp of the jejunum: a case report. Cases journal 2 (2009): 7152.
- Rubin BP and Hornick Mesenchymal tumors of the gastrointestinal tract, in practical soft tissue pathology: a diagnostic approach. Elsevier 214 (2019): 459-498.
- Matsushita M, Hajiro K, Okazaki K, et Endoscopic features of gastric inflammatory fibroid polyps. American Journal of Gastroenterology 91 (1996) 1595-1598.
- Tajima S, Koda Locally infiltrative inflammatory fibroid polyp of the ileum: report of a case showing transmural proliferation. Gastroenterology report 6 (2016): 144-148.
- Zhang C, Cui M, Xing J, et al Massive gastrointestinal bleeding caused by a giant gastric inflammatory fibroid polyp: a case report. International Journal of Surgery Case Reports 5 (2014): 571-573.
- Lee JH, Yoo JS, Jung HY, et al. A case of invasion of muscularis propria of gastric inflammatory fibroid polyp. The Korean Journal of Helicobacter and Upper Gastrointestinal Research 15 (2015): 254-257.
- Rais M, Chahdi H, Elfahssi M, et An unusual cause of intestinal obstruction in a young adult patient: Inflammatory fibroid polyp. Case Rep Surg 36 (2017): 5-8.


 Impact Factor: * 4.2
Impact Factor: * 4.2 Acceptance Rate: 72.62%
Acceptance Rate: 72.62%  Time to first decision: 10.4 days
Time to first decision: 10.4 days  Time from article received to acceptance: 2-3 weeks
Time from article received to acceptance: 2-3 weeks 