Lateral Trans-malleolar Approach for Posterior Malleolar Fractures of the Ankle for Articular and Syndesmosis Reduction: A Retrospective Study
Masanori Taki1*, Kosuke Suzuki1, Naohiro Hio2, Atsushi Hasegawa2
1Foot and Ankle Surgery, Seirei Hamamatsu General Hospital, Shizuoka, Japan
2 Orthopaedic Surgery, Higashi Maebashi Orthopaedic Hospital, Gunma, Japan
*Corresponding author: Masanori Taki, Foot and Ankle Surgery, Seirei Hamamatsu General Hospital, 2-12-12 Sumiyoshi, Naka-ku, Hamamatsu, Shizuoka 430-8558, Japan
Received: 08 December 2021; Accepted: 14 December 2021; Published: 23 December 2021
Article Information
Citation:
Masanori Taki, Kosuke Suzuki, Naohiro Hio, Atsushi Hasegawa. Lateral Trans-malleolar Approach for Posterior Malleolar Fractures of the Ankle for Articular and Syndesmosis Reduction: A Retrospective Study. Journal of Surgery and Research 4 (2021): 796-803.
View / Download Pdf Share at FacebookAbstract
Background
The lateral transmalleolar approach (LTA), a surgical approach for posterior malleolar fractures (PMFs), provides direct visualization of the articular surface of the posterior malleolus, though temporarily disrupting the syndesmosis. It is still unclear whether this fibrous joint can be effectively reconstructed afterward to prevent complications. We report the clinical results and computed tomography (CT) findings for articular and syndesmosis reduction status after surgery with LTA for PMF.
Methods
Sixteen patients who underwent PMF reduction with LTA with a follow-up of at least 1 year were evaluated retrospectively. Per the AO Foundation/Orthopaedic Trauma Association classification, the fracture type was 44B in 13 patients and 44C in three patients. The Haraguchi classifications of PMF were type 1 in six cases and type 2 in 10 cases. The American Orthopedic Foot and Ankle Society Ankle-Hindfoot Scale (AOFAS) score, post-surgical complications, and reduction status of PMF and syndesmosis on CT were investigated.
Results
The mean AOFAS score was 93.0 ± 5.2 points. Post-operative complications were observed in one case of superficial infection and one case of delayed fibular union. The articular step-off seen on CT improved significantly after surgery (5.9 ± 2.9 mm preoperatively vs. 0.6 ± 0.8 mm post-operatively). Syndesmosis malreduction was seen in three cases, including two high fibular fractures and one comminuted fibular fracture with osteoporosis.
Conclusions
The LTA provided favorable clinical results and effective reduction of intra-articular PMFs. However, surgeons should
Keywords
<p>Posterior Malleolar Fracture, Lateral Trans-malleolar Approach, Trimalleolar Fracture, Intra-articular fracture, Surgical approach, Syndesmosis, Fibular fractures, Syndesmosis malreduction</p>
Article Details
List of abbreviations
AO/OTA: AO Foundation/Orthopaedic Trauma Association
AOFAS: American Orthopedic Foot and Ankle Society Ankle-Hindfoot Scale
LTA: lateral transmalleolar approach
PMFs: posterior malleolar fractures
TFL: tibiofibular line
1. Introduction
Posterior malleolar fractures (PMFs) of the ankle are relatively common [1,2]; however, the treatment guidelines for PMFs are still controversial. In recent years, as the importance of PMF repair has been recognized, the surgical indications expanded, and the reduction goals became more demanding [3]. Since the PMFs are intra-articular fractures, surgeons should reconstruct the articular congruity properly. One report highlighted the need for reduction of the PMF intra-articular step-off to less than 1 mm [4]. By contrast, the current most common approaches for PMFs such as the posterior lateral [5] or posterior medial [6] approaches are extra-articular, lacking a direct visualization of the intra-articular fracture. Only a few methods [7,8] can provide direct intra-articular visualization for PMFs; one method is the lateral transmalleolar approach (LTA). With the LTA, surgeons can perform a more accurate intra-articular fracture reduction. However, as LTA temporarily disrupts the syndesmosis, it is unclear whether this fibrous joint can be effectively reconstructed afterwards. Thus, in this study, we retrospectively reviewed data of patients with trimalleolar ankle fractures, including PMFs, who underwent surgery with the LTA. Herein, we report the clinical results and computed tomography (CT) evaluations of articular and syndesmosis reduction following surgery via the LTA for PMFs.
2. Methods
2.1 Patients
Between April 2013 and January 2018, 19 patients had undergone surgery with the LTA for the reduction of trimalleolar PMFs at Seirei Hamamatsu Hospital. The inclusion criteria for this study were as follows: surgery was performed via the LTA for trimalleolar fractures, including PMFs, pre- and post-operative CT images were available, and cases followed up for at least 1 year after surgery. All patients provided informed consent, and this study was approved by the Institutional Ethics Review Board of Seirei Hamamatsu Hospital (Trial registration no. 3613; 19 May 2021). The study was conducted in accordance with the principles of the Declaration of Helsinki. Three patients were excluded from this study because two were lost to follow-up and one lacked post-operative CT. Finally, 16 (nine male and seven female) patients (median age, 52.6; range, 21-81 years) were enrolled in this study. The fracture type was 44B in 13 cases and 44C in three cases, based on the AO Foundation/Orthopaedic Trauma Association (AO/OTA) classification. In the CT classification of PMFs by Haraguchi [9], six cases were type 1 and 10 cases were type 2. Additionally, 10 patients had one or more extra fracture fragments, which are potential obstacles to fracture reduction. The study was conducted retrospectively, and the American Orthopedic Foot and Ankle Society Ankle-Hindfoot Scale (AOFAS scale), bone healing status, and presence of surgical complications were evaluated. In the CT evaluations of LTA outcomes, the articular step-off was evaluated in sagittal views pre- and post-operatively, and the post-operative syndesmosis reduction was assessed in axial views by measuring the tibiofibular clear space (TFCS; normal value: -0.8 to 5.8 mm), fibula rotation (normal value: 0.5–29.5°) [10], and tibiofibular line (TFL; normal value: < 2 mm) [11]. Statistical analysis was performed using the Welch’s t-test, with a significance level of p < 0.05.
2.2 Surgical procedure
PMF surgery using the LTA was performed in the supine position under general anesthesia; a tourniquet was placed on the patient’s thigh. A longitudinal skin incision was performed over the fibula, and the fibular fracture was exposed. Then, the ligaments and periosteum surrounding the distal fibula were dissected distally, and the lateral malleolus was gradually inverted distally. These soft tissue dissections are usually performed as minimum as necessary to expose the intra-articular fracture of the PMF; however, in these patients, the anterior aspect of the fibula was dissected till the anterior talofibular ligament. The interosseous membrane was dissected, and the posterior aspect of the fibula was dissected till approximately half of the posterior inferior tibial ligament. With this method, the lateral malleolus was inverted, and the intra-articular fracture was exposed (Figure 1). Subsequently, intra-articular dissection of the PMF and reduction or removal of the third fragment were performed, followed by articular reduction of the PMF under direct visualization. Then, large bone reduction forceps were inserted through the small anterior incision and the lateral fibular incision and held between the anterior tibial cortex and posterior tibial cortex of the PMF. The PMF was fixed via an anterior incision using several screws. Thereafter, the lateral malleolus was reduced to its original position, and the fibular fracture was fixed with a plate. Finally, the medial malleolus fracture was fixed with several screws. After surgery, a non-weight-bearing cast was used to immobilize the patients for 3 weeks; then, a patellar tendon-bearing brace was used until the PMF union.
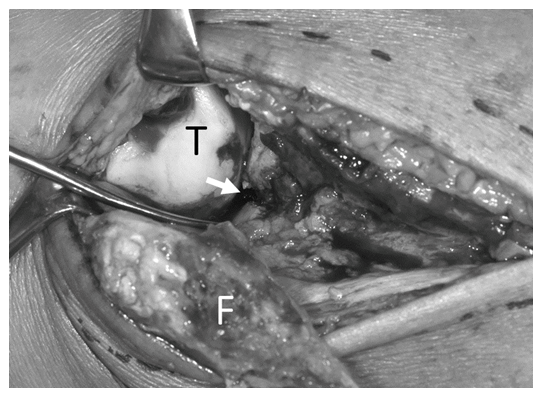
Figure 1: Intra-articular posterior malleolar fracture (PMF) visualized using the lateral transmalleolar approach (LTA). The LTA clearly shows the lateral side of the PMF. T, talus; F, inverted fibula; white arrow, intra-articular PMF
3. Results
The mean follow-up period was 17.0 ± 4.6 months (mean ± standard deviation). The post-operative AOFAS score was 93.0 ± 5.2 points. In the post-operative bone healing process, bone union was obtained within 3 months from surgery, although one case of AO/OTA type 44C presented delayed union of the fibula, achieved after 10 months. No serious complications, such as osteonecrosis of the fibula, were observed in the post-operative period. The pre- and post-operative articular step-offs in the CT sagittal view were 5.9 ± 2.9 mm and 0.6 ± 0.8 mm, respectively (Figure 2), showing a significant improvement (p = 0.0000017). However, three cases had post-operative articular step-off > 1 mm, including two Haraguchi type 2 PMFs (Figure 3a). In the CT examinations for syndesmosis reduction, the TFCS was 1.1 ± 1.6 mm, within the reference range in all cases. The fibula rotation was 6.3 ± 6.4°, deviating from the reference values in two cases, and the TFL was 1.6 ± 1.8 mm, exceeding the reference values in three cases. Overall, three cases demonstrated syndesmosis malreduction, including two AO/OTA type 44C and one 44B, which was a case of comminuted fibular fracture with underlying osteoporosis (Figure 3b).
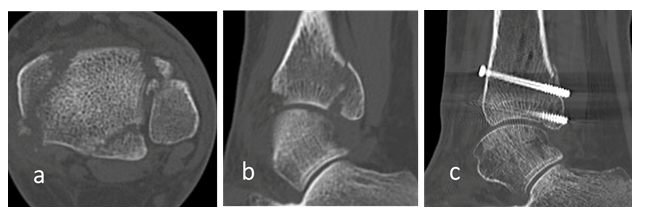
Figure 2: A 42-year-old woman with AO Foundation/Orthopaedic Trauma Association type 44B trimalleolar fracture and Haraguchi type 1 posterior malleolar fracture: (a) pre-operative computed tomography (CT) axial view; (b) pre-operative CT sagittal view; (c) post-operative CT sagittal view
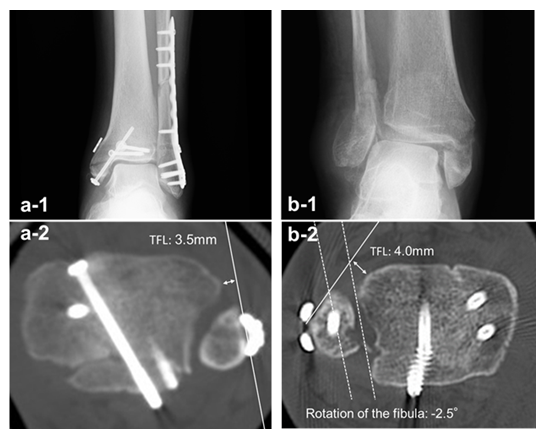
Figure 3: Syndesmosis malreduction cases after lateral transmalleolar approach: (a-1) A 76-year-old man with AO Foundation/Orthopaedic Trauma Association (AO/OTA) type 44C trimalleolar fracture and Haraguchi type 2 posterior malleolar fracture. Post-operative X-ray image shows a high fibular fracture fixed with a plate and a syndesmosis fixation using a suture button. (a-2) Post-operative computed tomography (CT) shows syndesmosis malreduction with tibiofibular line (TFL) of 3.5 mm. (b-1) A 70-year-old woman with type AO/OTA 44B trimalleolar fracture, a comminuted fibular fracture with underlying osteoporosis. (b-2) Post-operative CT shows syndesmosis malreduction with fibula rotation of -2.5° and TFL of 4.0 mm due to unsuccessful fibular reduction.
4. Discussion
This study showed that the intra-articular step-off was reduced to ≤ 1 mm in 13 of 16 cases via the LTA for PMFs. Moreover, syndesmosis reduction after LTA was successful in 13 of 16 cases. Overall, LTA offered good results in PMF treatment in terms of fracture reduction and clinical outcomes. However, some important considerations emerged when surgeons chose LTA for PMFs. The major advantage of the LTA is that it allows direct visualization of the tibial plafond articular surfaces. This capability could provide an opportunity for surgeons to perform more accurate intra-articular fracture reductions. Ankle fractures with PMFs have a worse prognosis than without PMF [12,13]. Articular step-offs > 2 mm are conventionally an indication for surgery [14,15]. In 2015, Drijfhout van Hooff et al. [4] reported that articular surface step-offs ≥ 1 mm frequently result in arthritic changes and recommended carefully repairing the posterior articular surface. However, the process for obtaining a successful articular reduction is challenging. Currently, the most common surgical approaches to PMFs are the posterior lateral [5] and posterior medial [6] approaches. However, with these techniques, it is impossible to perform surgery with direct observation of the articular surfaces affected by PMFs. Given the local anatomy, only a few approaches provide direct intra-articular visualization of PMFs [7,8]; the LTA is one of these approaches. Kim et al. [16] reported 36 cases of PMFs treated with the LTA that presented good clinical results. It is a versatile approach for ankle intra-articular pathology, established by a long history. We believe that the LTA is a useful approach for reducing intra-articular PMFs, expected to offer improved clinical results. However, there are still some surgical limitations associated with the LTA. It can only visualize the lateral side of the PMF, not the medial side, affected by fractures such as Haraguchi type 2 medial extension. Therefore, these fractures require X-ray fluoroscopy. Conversely, the LTA requires wide dissection of undamaged soft tissues, including the ligaments comprising the syndesmosis. Therefore, one significant concern is whether the syndesmosis can be anatomically reconstructed at the end of the surgery. In the CT evaluation for this study, syndesmosis malreduction emerged in three patients; two patients had AO/OTA type 44C fractures and one had a type 44B fracture. In the two cases of AO/OTA type 44C fractures, the injury included a high fibular fracture, and syndesmotic fixation was performed. These types of injuries are the most common causes of syndesmotic malreduction. By contrast, the type 44B case could be considered an LTA-induced syndesmotic reduction failure. The risk of syndesmotic malreduction is usually low in patients with type 44B fracture. This patient had a comminuted fibular fracture with underlying osteoporosis, complicating the fracture reduction. Therefore, we believe that the poor reduction of the fibula led to the syndesmosis malreduction. LTA use should be carefully considered when fibular reduction is assumed to be complicated, such as in AO/OTA type 44C, comminuted, and osteoporotic fractures. Additionally, because of the extensive dissection, LTA may lead to pseudoarthrosis or necrosis of the fibula [16]. Although no case of peroneal necrosis due to the LTA has been reported to date, we observed a delayed fibular union in a case of AO/OTA type 44C fracture. This delay could be due to the more extensive dissection required to perform the LTA for a high fibular fracture. Therefore, indications for the LTA should be carefully considered in patients with high fibular fractures or insufficient blood circulation in the lower extremities. The main limitations of this study were its retrospective design, inclusion of a small number of cases, and a short follow-up period. However, in our experience, the LTA is a useful approach for performing intra-articular fracture reduction in PMFs. Further research and development of surgical techniques are required.
5. Conclusions
The LTA provides direct visualization of the intra-articular PMFs and is an effective approach for PMF treatment. However, even with the LTA, it is challenging to confirm a proper fracture reduction in Haraguchi type 2 PMFs. In addition, surgeons should be aware of the possibility of syndesmosis malreduction in cases of high or comminuted fibular fractures.
Acknowledgments
We thank Editage (www.editage.com) for English language editing.
Funding
The authors did not receive support from any organization for the submitted work.
Ethics approval and consent to participate
This study was approved by our Institutional Ethics Review Board, Seirei Hamamatsu Hospital. Trial registration number: 3613. 19 May 2021 retrospectively registered. All patients provided informed consent for participating in this study.
Consent for publication
All patients provided informed consent for the publication of their images and data.
Availability of data and materials
The datasets analyzed in the current study are available from the corresponding author on reasonable request.
Competing interests
The authors have no relevant financial or non-financial interests to disclose
Authors Contributions
Kosuke Suzuki, Naohiro Hio, Atsushi Hasegawa, and Masanori Taki were involved in the study design and data interpretation. All authors critically revised the report, commented on drafts of the manuscript, and approved the final report.
References
- Court-Brown CM, McBirnie J, Wilson G. Adult ankle fractures- an increasing problem? Acta Orthop Scand 69 (1998): 43-47.
- Xu HL, Li X, Zhang DY, et al. A retrospective study of posterior malleolus fractures. Int Orthop 36 (2012): 1929-1936.
- Bartonícek J, Rammelt S, Tucek M. Posterior malleolar fractures: Changing concepts and recent developments. Foot Ankle Clin 22 (2017): 125-145.
- Drijfhout van Hooff CC, Verhage SM, Hoogendoorn JM. Influence of fragment size and postoperative joint congruency on long-term outcome of posterior malleolar fractures. Foot Ankle Int 36 (2015): 673-678.
- Talbot M, Steenblock TR, Cole PA. Posterolateral approach for open reduction and internal fixation of trimalleolar ankle fractures. Can J Surg 48 (2005): 487-490.
- Neufeld AJ. Trimalleolar fractures: A convenient medial approach for surgical reduction. Calif Med 93 (1960): 297-298.
- Gatellier J, Chastang P. Access to fractured malleolus with piece chipped off at back. J Chir 24 (1924): 513.
- Gonzalez TA, Watkins C, Drummond R, et al. Transfibular approach to posterior malleolus fracture fixation: Technique tip. Foot Ankle Int 37 (2016): 440-445.
- Haraguchi N, Haruyama H, Toga H, et al. Pathoanatomy of posterior malleolar fractures of the ankle. J Bone Joint Surg Am 88 (2006): 1085-1092.
- Dikos GD, Heisler J, Choplin RH, et al. Normal tibiofibular relationships at the syndesmosis on axial CT imaging. J Orthop Trauma 26 (2012): 433-438.
- Gifford PB, Lutz M. The tibiofibular line: An anatomical feature to diagnose syndesmosis malposition. Foot Ankle Int 35 (2014): 1181-1186.
- Jaskulka RA, Ittner G, Schedl R. Fractures of the posterior tibial margin: Their role in the prognosis of malleolar fractures. J Trauma 29 (1989): 1565-1570.
- Odak S, Ahluwalia R, Unnikrishnan P, et al. Management of posterior malleolar fractures: A systematic review. J Foot Ankle Surg 55 (2016): 140-145.
- Berkes MB, Little MT, Lazaro LE, et al. Articular congruity is associated with short-term clinical outcomes of operatively treated SER IV ankle fractures. J Bone Joint Surg Am 95 (2013): 1769-1775.
- Gardner MJ, Streubel PN, McCormick JJ, et al. Surgeon practices regarding operative treatment of posterior malleolus fractures. Foot Ankle Int 32 (2011): 385-393.
- Kim MB, Lee YH, Kim JH, et al. Lateral transmalleolar approach and miniscrews fixation for displaced posterolateral fragments of posterior malleolus fractures in adults: A consecutive study. J Orthop Trauma 29 (2015): 105-109.
- Giebel GD, Meyer C, Koebke J, et al. The arterial supply of the ankle joint and its importance for the operative fracture treatment. Surg Radiol Anat 19 (1997): 231-235.


 Impact Factor: * 4.2
Impact Factor: * 4.2 Acceptance Rate: 72.62%
Acceptance Rate: 72.62%  Time to first decision: 10.4 days
Time to first decision: 10.4 days  Time from article received to acceptance: 2-3 weeks
Time from article received to acceptance: 2-3 weeks 