Progressive Formation of Germinal Centers with Multiple Nodule in The Lung
Ahmet Dumanli1*, Gürhan Öz1, Adem Gencer2, Çi?dem Özdemir3, ?ule Çilekar4, Ayd?n Balc?4
1Afyonkarahisar Health Sciences Universty, Department of Chest Surgery, Afyonkarahisar, Turkey
2Afyonkarahisar Public Hospital, Department of Chest Surgery, Afyonkarahisar, Turkey
3Afyonkarahisar Health Sciences Universty, Department of Patology, Afyonkarahisar, Turkey
4Afyonkarahisar Public Hospital, Department of Pulmonology, Afyonkarahisar, Turkey
*Corresponding Author: Ahmet Dumanli, Afyonkarahisar Health Science University, Departman of Chest Surgery, Turkey
Received: 08 April 2020; Accepted: 21 April 2020; Published: 24 April 2020
Article Information
Citation: Ahmet Dumanli, Gurhan Oz, Adem Gencer, Cigdem Ozdemir, Sule Cilekar, Aydin Balci. Progressive Formation of Germinal Centers with Multiple Nodule in The Lung. Journal of Surgery and Research 3 (2020): 075-081.
View / Download Pdf Share at FacebookAbstract
Enlarged lymph nodes in the head, neck, and axillary region are a common cause for patients to contact doctors. The most common cause of lymphadenopathy is infection and usually regresses with treatment. In the differential diagnosis of chronic lymphadenopathies, infection, lymphoproliferative diseases and progressive transformation of germinal centers should be considered. In this article, we aimed to discuss the patient with bilateral widespread nodular appearance in the cervical, supraclavicular, axillary, mediastinal lymph node and lungs. A 43-year-old female patient was referred for her mass in the neck and bilateral axillary region. Biopsy from the cervical region in the outer center was evaluated as an infection. In radiological imaging, lymph nodes were observed in the left cervical 15*11 mm, right supraclavicular 24*11 mm, left supraclavicular 18*11 mm, right axillary 11*21 mm, left axillary 27*18 mm, mediastinum 24*15 mm. In addition, extensive nodular lesion, the largest of which was 15 mm, was observed in both lungs. Excisional biopsy was performed from the left axillary region. Pathologically, progressive transformation of germinal centers was diagnosed. In the presence of lymphadenopathies that do not pass with medical treatment, an excisional biopsy should be performed and the diagnosis should be clarified for a definitive diagnosis.
Keywords
<p>Germinal, Center, Transformation, Surgery, Lymph node</p>
Article Details
1. Introduction
Enlarged lymph nodes in the head and neck area are a frequent reason for patients to refer to doctors [1]. The most common cause of lymphadenopathies (LAP) is infections and regress with treatment [1]. However, if LAP is permanent, excisional biopsy may be required for diagnosis [1]. In differential diagnosis, progressive transformation of infection, lymphoproliferative diseases and germinal centers should be considered [1]. In addition, it should be kept in mind that nonhodgkin lymphomas with cervical and axillary lymphadenopathies can also be found in chylothorax [2]. Castleman disease, one of the lymphoproliferative diseases and the most common causes of LAP should not be forgotten [3]. Progressive transformation of the germinal centers (PTGC) is associated with the presence of chronic LAP and germinal centers [1]. Histologically, the mantle zone region is characterized by the expansion of lymphocytes into both adjacent sinusoids and germinal centers [4]. It was first described by Lennert and Müller-Hermelink in 1975 [1]. It is a clinicopathological condition that is 3-4 times larger than reactive lymphoid hyperplasia [1]. It is typically seen in the head and neck region [5]. PTGC is a common, benign and asymptomatic condition [6]. It is 3 times more common in men [7]. Approximately 50% cervical, 25% inguinal, 22% axillar are located [8]. Approximately 3.5-10% of patients presenting with painless, persistent lymphadenopathy are diagnosed with PTGC [9]. Often, nodular lymphocyte-rich Hodgkin lymphoma (NLPHL) can be confused with malignant processes such as follicular lymphoma [10]. In some previous studies, they found 16-35% of PTGC related to NLPHL [7, 11, 12].
In our study, we aimed to discuss the patient with cervical, supraclavicular, axillar, mediastinal lymph node and widespread nodular appearance in the lungs.
2. Case Presentation
A 43-year-old female patient applied bilaterally due to LAP palpated in the neck and axillary. LAP biopsy was performed from the cervical region in the hospital where he went before, and medical treatment was given in favor of infection. The patient, who did not shrink in the lesions with medical treatment, applied to our clinic. On physical examination, a nodular lesion was palpated in the bilateral axillary, cervical and supraclavicular region. The patient did not have any complaints and previous illnesses. Vital findings were normal. Radiologically in thorax CT imaging; widespread LAP in the cervical and mediastinum, and bilateral widespread nodular lesion in the lung parenchyma were observed (Figure 1). In PET-CT, the larger of the left cervical is 15*11 mm (SUVmax: 8.7), the right supraclavicular is 24*11 mm (SUVmax: 8.9), the left supraclavicular is 11*8 mm (SUVmax: 2.6), the largest is the right axillary 21*21 mutiple LAP with mm, left axillary 27*18 mm (SUVmax: 14.6) was observed. Multiple LAP with the largest 24*15 mm (SUVmax: 6.4) were observed in the mediastinum. Multiple nodular lesions with scattered localization, 15 mm in diameter (SUVmax: 7.1), were observed in both lung parenchyma (Figure 2). The patient underwent excisional biopsy from the left axillary region and was diagnosed pathologically (in the immunohistochemical study, marginal zone lymphocytes infiltrating germinal centers) were diagnosed (Figure 3, 4).
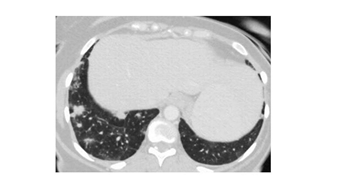
Figure 1: Preoperative thorax CT.
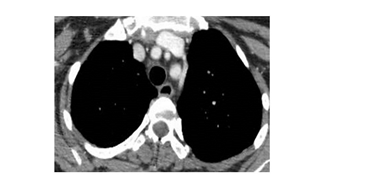
Figure 2: Preoperative thorax CT.
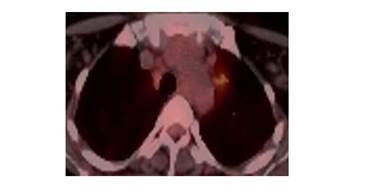
Figure 3: Preoperative PET-CT.
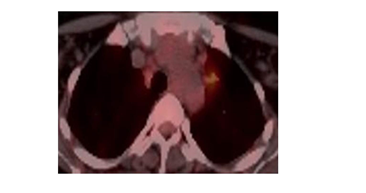
Figure 4: Preoperative PET-CT.
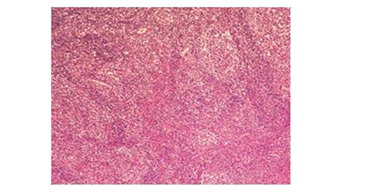
Figure 5: Small lymphocyte clumps trying to enter the germinal centers (x40HE).
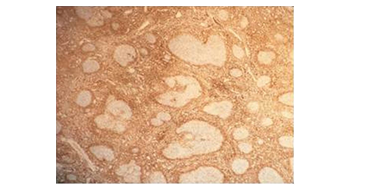
Figure 6: In the Bcl-2 immunohistochemical study, marginal zone lymphocytes infiltrating germinal centers.
3. Discussion
Enlarged lymph nodes in the head and neck region are a common reason for patients to refer to doctors [1]. The most common cause of LAP is infections and treatment regresses [1]. However, if LAP is permanent, excisional biopsy may be required for diagnosis [1]. In differential diagnosis, infection, lymphoproliferative diseases and progressive transformation of germinal centers should be considered [1]. It is well known that progressive transformation of germinal centers can mimic nodular lymphocyte dominant Hodgkin lymphoma both clinically and histologically [10].
Ta?asiewicz K, et al. They examined 2 patients with lymph node swelling. The first case; A 32-year-old male patient who underwent surgery for pancreatic cancer 4 years ago, who had painless submandibular and cervical lymphadenopathy. She was a 65-year-old female patient who was under observation for primary sclerosing cholangitis and celiac disease and had a single, painless mass in the submandibular region [13]. Bailey CE, et al. They examined a 39-year-old woman with right neck lymphadenopathy and a parotid mass on the same side. They have previously learned that ipsilateral parotidectomy and neck dissection were performed in another institution [6]. Abo AY, et al. They examined a 60-year-old female patient who underwent thyroid ca operation at the age of 48 and suffered from submandibular swelling at the age of 59 [4]. Chian A, et al. They examined a 67-year-old male patient who had no previous complaints due to acute shortness of breath and chest discomfort [14]. We also examined a 43-year-old woman with bilateral swelling in the neck and axillary region. Our case was compatible with the literature as a location. Ta?asiewicz K, et al. on physical examination in the first patient; they detected enlarged lymph nodes. Laboratory tests found erythrocyte sedimentation rate (ESR) 22 mm/1 hour [1-15] and beta-2-microglobulin 1.96 mg/L (0.7-1.8). In the second patient; detected an enlarged, rounded and well-shaped submandibular lesion. Increased beta-2-microglobulin was detected in laboratory tests and other findings were found to be insignificant [13]. Bailey CE, et al. they detected a mass on the right neck. There has been fatigue and weight loss for 4 years [6]. Abo AY, et al. They detected a nodule in the submandibular region in a 60-year-old woman. There were no symptoms such as fever and weight loss [4]. Chian A, et al. They detected acute shortness of breath and chest discomfort in the patient who did not have any problems and did not smoke. There was no family history of malignancy. On examination, the pulse was 110/minute, TA 130/80 mmHg, the respiratory rate was 16/minute and no fever was detected [14]. In our physical examination, palpable nodules were found in the bilateral neck and axillar region. The patient had no complaints. Vital findings were normal. The findings were consistent with the literature.
As a diagnostic procedure; Ta?asiewicz K, et al. in the first patient; They performed fine needle aspiration biopsy on the lymph node with USG. Pathologically, LCA (+) and CD56 (-) arrived. These findings indicated reactive lymphadenopathy and low-grade lymphoma. They had PET-CT due to the patient's suspicion of lymphoma and saw cervical lymph nodes with SUVmax 8.9. Then they performed surgical excisional biopsy and PTGC was diagnosed by seeing giant irregularly shaped germinal centers. In the second patient; In USG, they found hypoechoic lymph node 10 × 17 mm in size with abundant vascularization. An FNAB was made from the lesion and cytopathology came as a reactive lymphadenopathy. It was suggested to perform a biopsy again. Magnetic resonance was taken to exclude other pathological findings in the head and neck region. Enlarged submandibular lymph node with increased contrast was detected. The patient underwent excisional biopsy. The pathological report supported follicular lymphoid hyperplasia with PTGC [13]. Bailey CE, et al. No malignancy was detected pathologically in the patient who had previously performed ipsilateral parotidectomy and neck dissection in another institution. However, the patient was directed to an oncologist. Recurrent right parotid mass and neck lymphadenopathy developed after a four-year symptom-free break. The facial nerve was bilaterally intact. Recurrences in the parotid gland and lymph node area suggested the possibility of malignancy. Repeated parotid and lymph node FNAB pathology was negative in terms of malignancy. It was reported as PTGC as a result of reexamination of pathologies obtained from previous surgery. Excisional neck lymph node biopsy was performed. Pathology supported NLPHL in a portion adjacent to PTGC areas. In postoperative PET/CT, hypermetabolic lymphadenopathy was detected in the right neck, parotid and right groin areas. The patient was successfully treated with chemotherapy [6]. Abo AY, et al. CT showed deep cervical and right axillar lymph node. Lymph node biopsy was performed and reported as hodgkin lymphoma that developed pathologically on the basis of PTGC. The patient was given chemotherapy. After 9 months, PET was evaluated, relapsed in the axilar lymph node, and chemotherapy was given again and the patient was treated [4]. Chian A, et al. the patient suspected pulmonary embolism and the diagnosis was confirmed by pulling thorax CT. Abdominal USG and CT, taken during the treatment, detected a 4.9** 3.0 cm age mass in the mesenteric root, without necrosis and calcification. The patient who did not accept the treatment was followed up. In the PET-CT taken during follow-up, a single mass with SUVmax = 6.6 was detected at the mesenteric root. The patient refused treatment again. In PET-CT, which was taken again after 6 months, SUVmax: 8.5 and a non-changing mass was observed. The patient was convinced of the possibility of malignancy and laparoscopy was performed. Pathologically irregular edged, large-sized follicles with an increased number of enlarged, significantly enlarged follicles along the lymph node along with germinal centers. Follicular lymphoma was excluded due to the apparent infiltration and accumulation of mantle region lymphocytes in larger follicles in CD79a stain with BCL2 negativity. There were no L&H cells and classic Reed-Sternberg-like cells. Based on these findings, a diagnosis of PTGC was made [14]. In our patient; radiologically in thorax CT imaging; Widespread LAP in the cervical and mediastinum, and bilateral widespread nodular lesion in the lung parenchyma. In PET-CT; the larger of the left cervical is 15*11 mm (SUVmax: 8.7), the right supraclavicular is 24*11 mm (SUVmax: 8.9), the left supraclavicular is 11*8 mm (SUVmax: 2.6), the largest is the right axillary 21*21 mm, left axillary 27*18 mm (SUVmax: 14.6) LAP was observed. Multiple LAPs with the largest 24*15 mm (SUVmax: 6.4) were observed in the mediastinum. Multiple nodular lesions with scattered localization, 15 mm in diameter (SUVmax: 7.1), were observed in both lung parenchyma. The patient underwent excisional biopsy from the left axillary region and was diagnosed pathologically (in the immunohistochemical study, marginal zone lymphocytes infiltrating germinal centers) were diagnosed. The patient was also offered biopsy from nodules in the lungs and did not accept. The patient was followed up.
Consequently, in the presence of persistent LAPs that do not pass with medical treatment, excisional biopsy may be required for a definitive diagnosis. In differential diagnosis, infection, lymphoproliferative diseases and PTGC should be kept in mind.
Conflict of Interest
Authors Ahmet Dumanli, Gürhan Öz, Adem Gencer, Çi?dem Özdemir, ?ule Çilekar, Ayd?n Balc? declare that they have no conflict of interest.
Financial Support
No financial support was received for the study.
Author Contributions
A.D. conceived and designed the study. G.Ö, A.G, performed clinical assessments. Ç.Ö, ?.Ç, A.B. performed experiments, and contributed to data acquisition, analysis and interpretation. All authors contributed to critical revision of the manuscript for intellectual content and final approval of the manuscript.
References
- Ikinciogullari A, Koseoglu S, Cetin MA, et al. Boyunda lenfadenopati: Germinal merkezlerin progresif transformasyonu. Kulak Burun Bogaz Ihtis Derg 23 (2013): 307-311.
- Cansiz KA, Tug T, Konuk S, et al. A Case with Tumor, Tuberculosis and Chylothorax. Archives of Clinical and Medical Case Reports 2 (2018): 68-74.
- Bayram Metin, Ahmet Dumanli, Olgun Kadir Aribas. Castleman Hastal???. Turkiye Klinikleri J Thor Surg-Special Topics 7 (2016): 95-100.
- Yashima-Abo A, Satoh T, Shimosegawa K, et al. Classical Hodgkin Lymphoma Occuring in Association with Progressive Tranformation of Cerminal Center. H Clin Exp Hematop 54 (2014).
- Kojima M, Nakamura S, Motoori T, et al. Progressive transformation of germinal centers: a clinicopathological study of 42 Japanese patients. International Journal of Surgical Pathology 11 (2003): 101-107.
- Bailey CE, Jung F, Addicks B, et al. Nodular Lymphocyte-Predominant Hodgkin Lymphoma in Progressive Transformation of Germinal Centers. Hindawi Case Reports in Otolaryngology (2017).
- Hicks J, Flaitz C. Progressive transformation of germinal centers: review of histopathologic and clinical features. International Journal of Pediatric Otorhinolaryngology 65 (2002): 195-202.
- Guzzo M, Locati LD, Prott FJ, et al. Major and minor salivary gland tumors. Critical Reviews in Oncology/Hematology 74 (2010): 134-148.
- Miller MW, Gatter KM, Cannady SB, et al. Progressive transformation of germinal centers (PTGC) in the head and neck. Laryngoscope 120 (2010): S168.
- Smith LB. Nodular lymphocyte predominant Hodgkin lymphoma diagnostic pearls and pitfalls. Archives of Pathology and Laboratory Medicine 134 (2010): 1434-1439.
- Chang CA, Kumar B, Nandurkar D. A case report of high 18F-FDG PET/CT uptake in progressive transformation of the germinal centers. Medicine 94 (2015): e412.
- Ozkan MC, Ozsan N, Hekimgil M, et al. Progressive transformation of germinal centers: single-center experience of 33 Turkish patients. Clinical Lymphoma Myeloma and Leukemia 16 (2016): 149-151.
- Konrad Ta?asiewicz, Aleksandra Czachowska, Katarzyna ?mia?ek-Kania, et al. Progressive transformation of germinal centers: an illustration of two clinical cases. Annals of Hematology 97 (2018): 1081-1083.
- Chian A Chang, Beena Kumar, Deepali Nandurkar. A Case Report of High 18F-FDG PET/CT Uptake in Progressive Transformation of the Germinal Centers. Medicine 94 (2015).


 Impact Factor: * 4.2
Impact Factor: * 4.2 Acceptance Rate: 72.62%
Acceptance Rate: 72.62%  Time to first decision: 10.4 days
Time to first decision: 10.4 days  Time from article received to acceptance: 2-3 weeks
Time from article received to acceptance: 2-3 weeks 