What’s New in the Management and Treatment of Carotid Body Tumors
Chapman SC*
Department of Vascular Surgery, University of Pittsburgh Medical Center, Pennsylvania, USA
*Corresponding Author: Chapman SC, Department of Vascular Surgery, University of Pittsburgh Medical Center, Pennsylvania, USA
Received: 05 August 2019; Accepted: 22 August 2019; Published: 26 August 2019
Article Information
Citation: Chapman SC. What’s New in the Management and Treatment of Carotid Body Tumors. Journal of Surgery and Research 2 (2019): 139-146.
View / Download Pdf Share at FacebookAbstract
Carotid body tumors (CBT) are a rare, hypervascular tumor involving the carotid bifurcation. CBT represent the majority of paragangliomas of the head and neck region. Despite over a century of experience, we continue to advance our knowledge in its management and treatment.
Keywords
<p>Carotid body tumors, Neoplasm, Paragangliomas</p>
Article Details
1. Introduction
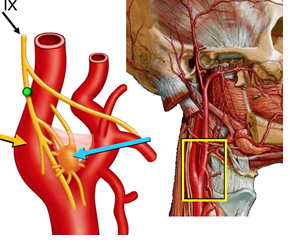
The carotid body is a specialized chemoreceptor located within the semi-adventitial tissue of the carotid bifurcation. It is stimulated by conditions that induce hypoxia, hypercapnia, and acidosis and controls the body’s response to these conditions with changes in blood pressure, heart rate, and respiratory rate by release of catecholamines [1]. The carotid body receives its blood supply through glomus arteries traversing Mayer’s ligament from the common carotid artery and the ascending pharyngeal arterial branch of the external carotid artery, and its innervation derives off a small branch of the glossopharyngeal nerve (Figure 1) [2-4]. CBT (paragangliomas) are a rare neoplasm originating in the neural crest cells at the carotid bifurcation. The incidence of CBT is estimated to be 1-2 per 100,000 and represent two thirds of head and neck paragangliomas of the head and neck [5]. The majority of these neoplasms are sporadic while 10-15% are familial or hyperplastic. The hyperplastic type is most common in populations living in high altitudes (>5000 feet above sea level). Most patients will present in the 4th to 5th decade of life with a slightly earlier onset in the hereditary group [6]. 10% of CBT are bilateral, and only 5% of CBT are considered malignant in nature with metastatic disease on presentation. Historically, the mortality and stroke rate associated with surgical resection was 6% and 23%, respectively [7]. Advancement of preoperative planning, multidisciplinary collaboration, and surgical technique has reduced mortality rate to less than 1% and stroke rate to 1-2%.
2. Initial Evaluation
Majority of patients with CBT present with a painless neck mass (around 65%) anterior to the sternocleidomastoid muscle. The pathognomonic sign on exam is a fixed mass in the vertical axis while mobile on the horizontal axis (Fontaine sign). Approximately 10% of patients will present with hoarseness, dysphagia, pain, winged-scapula, or Horner’s syndrome consistent with nerve involvement. The remaining patients with CBT will be diagnosed incidentally during carotid duplex exam or cervical axial imaging. Fine needle aspiration should not be performed given the vascularity of the neoplasm and high risk for hemorrhage.
A careful history is required to identify patients with a genetic predisposition for CBT and other paragangliomas (e.g. pheochromocytoma). Approximately 10-30% of patients have CBT associated with at least one germline mutation in a subunit of the succinate dehydrogenase (SDH) gene which has vital role encoding mitochondria’s role in the Krebs cycle. Deactivation of SDH promotes dysregulation of hypoxia-induced genes and growth factors [8]. Genetic counseling may be of benefit for patients and their family members that present at a younger age, with a positive family history, or having bilateral location or multiple paragangliomas [9].
3. Radiographic Evaluation
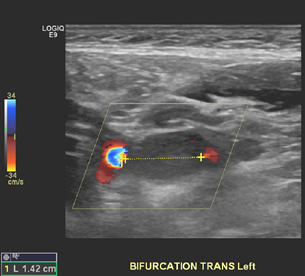
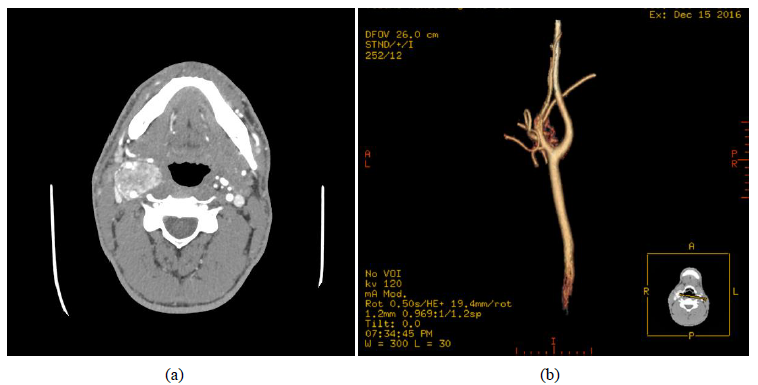
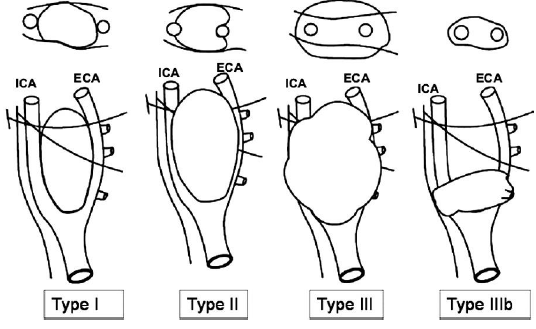
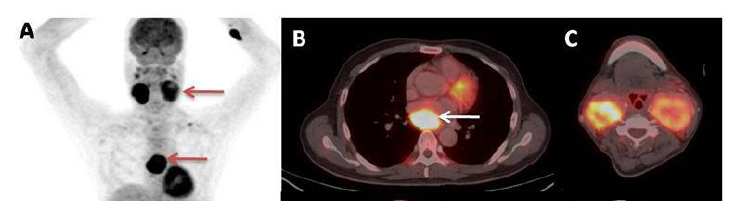
Duplex ultrasonography is the first-line diagnostic modality for evaluation of CBT. It permits identification of any concomitant carotid artery disease and the vascularity of the neck mass (Figure 2). Digital subtraction angiography was once considered the “gold standard” for diagnosing CBT. It has been replaced by cross-sectional imaging. CT angiography (Figure 3a and 3b) and/or MR angiography provide diagnostic as well as preoperative staging of CBT into the appropriate Shamblin classification (figure 4) [10]. Shamblin classification is an important predictor of neurovascular morbidity with Group 3a and 3b carrying the highest risk of nerve injury or requirement of vascular reconstruction. In cases of suspected metastasis or multicentric tumors, 18F-fluorodeoxyglucose positron emission tomography-computed tomography (FDG PET-CT) provides high specificity and sensitivity for detection (Figures 5a, 5b, and 5c) [11].
4. Preoperative Evaluation
CBT are infrequently hormonally active, but it is recommended to perform biochemical testing for plasma metanephrines or 24-hour urine collection for catecholamines and metanephrines. If the paraganglioma is functional, phenonxybenzamine 10mg two times daily should be initiated 7-10 days prior to surgery. Beta blocker is started only after achieving adequate alpha blockade with phenoxybenzamine. Patients presenting with history of previous neck surgery or new hoarseness should undergo a preoperative otolaryngology evaluation of the vocal cords. Depending on local expertise, collaboration of otolaryngologists and vascular surgeons may facilitate surgical planning and improve outcomes. Patients with bilateral CBT should have a staged surgical resection with an intermediate assessment of the vocal cords.
Preoperative embolization of the feeding vessels to CBT is controversial related to lack of evidence of improved outcomes and procedural stroke risk. Some studies have shown decreased blood loss associated with embolization while others have found no difference. If embolization is performed, surgical resection should be planned within 48 hours to avoid the secondary inflammatory reaction [12-14]. Vein mapping of the greater saphenous vein may be beneficial for larger CBT when vascular reconstruction is expected.
5. Treatment
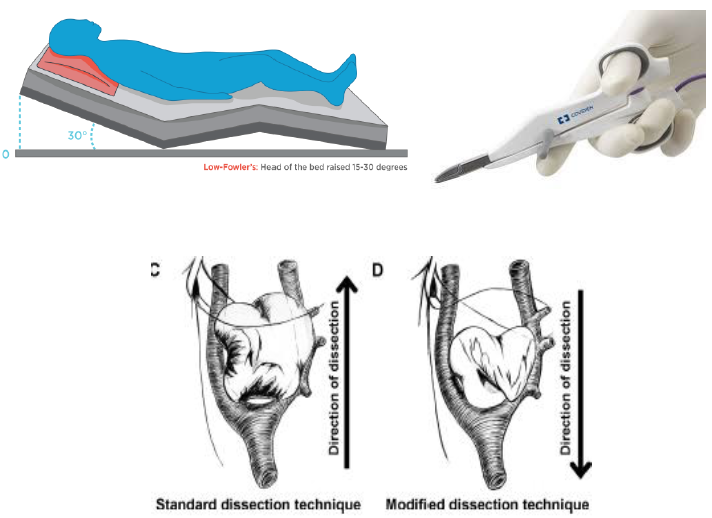
CBT remains a surgical disease. That being said, there may be a role for observation for small CBT (<2 cm) in certain populations as demonstrated by Muno in Bogota (elevation >2000 meters above sea level) [15]. Radiation therapy is available for elderly patients that may be high risk for surgery or patients who present with local recurrence or metastasis [16]. An important but often overlooked step of the operation is patient positioning. After our anesthesiologist achieves satisfactory intravenous access and arterial line monitoring, the patient is placed in a relaxed, semi-fowler position (lawn chair) (Figure 6A) with both arms tucked. The patient’s head is slightly externally rotated to the contralateral side. Some surgeons place a small roll under the shoulder blades to accentuate the neck hyperextension. We monitor EEG waveforms during the procedure in case carotid artery cross-clamping is required, and the EEG technician will establish the patient’s baseline prior to draping and incision. During draping, anatomic landmarks are clearly visible such as the ear lobe, mastoid process, angle of mandible, clavicle and sternal notch. The use of a portable ultrasound to map and mark a segment of greater saphenous vein is beneficial prior to prepping and draping this segment of the upper thigh. We apply an IobanTM (3M, St. Paul, MN) to the neck and thigh surgical sites to prevent drape migration.
The incision may be made obliquely along the medial border of the sternocleidomastoid muscle or transverse following the natural neck lines (Langer’s line). Either incision will provide adequate exposure. Ligation of the facial vein facilitates lateral retraction of the internal jugular vein and access to the common carotid artery and its bifurcation. Early identification of the vagus nerve and the hypoglossal nerve are important steps in their preservation. The vagus nerve is located in the carotid sheath, and the hypoglossal nerve may be identified by tracing the ansa cervicalis nerve superiorly to its attachment to the hypoglossal. The ansa cervicalis may be sacrificed to simplify access to the carotid bifurcation. The next step is the precautionary use of Rummel umbilical tape tourniquets for vascular control of the carotid and its main branches as well as the additional benefit provided by them for vascular shunt stabilization, if required.
The major tenets of surgical resection of these highly vascularized neoplasm is early identification and preservation of the nerves, maintaining a bloodless field to facilitate the former, and a subadventitial plane along the carotid arteries to ensure complete excision. Bipolar diathermy (Figure 6B) provides an efficient, safe technique for maintaining hemostasis during excision and is similarly used by endocrine surgeons for thyroidectomies for smaller vessels. Van der Bogt and Hamming, et al. were one of the first to describe a cranial to caudal dissection technique which permitted early identification of vital neurovascular structures and demonstrated an associated reduction in surgical morbidity (Figure 6C and 6D) [17]. This technique simplifies the more tedious dissection on the ventral surface of the tumor. The most common nerve injury occurs during the ventral dissection to the superior laryngeal nerve. An injury to this nerve results in the alteration of pitch of the patient’s voice and can make it difficult for the patient to yell or be heard in loud areas. A high vagal nerve injury is associated not only with hoarseness but high risk for aspiration and possible need for a PEG tube. In the case of Shamblin 3, with proximal extension, the accessory spinal nerve can be involved and lead to weakness of the trapezius muscle producing a drooping shoulder and a winging of the scapula [18].
Postoperative care involves an overnight hospitalization for observation due to risk of bleeding and nerve injury or palsy. The complication risk directly correlates to the size of the neoplasm, the cranial extent of resection, and the Shamblin classification. Postoperative life-long surveillance is required for patients with hereditary paragangliomas or identified SDH genetic mutation.
6. Conclusion
CBT are a rare neoplasm but the most common paraganglioma of the head and neck. Advancement of radiographic imaging techniques has reduced the role and associated risk of preoperative angiography. Molecular genetics have assisted the identification of patients and their family members who may benefit from genetic counseling, comprehensive preoperative imaging, and postoperative surveillance. We continue to refine surgical technique to reduce neurovascular morbidity associated with resection.
References
- Kaife FE, Freischlag JA. Carotid body tumors: The role of preoperative emobolization. Ann Vasc Surg 15 (2001): 237-242.
- Najibi S, Terramani TT, Brinkman W, et al. Carotid body tumors. J AM Coll Surg 194 (2002): 538-539.
- Hallett JW, Nora JD, Hollier LH, et al. Trends in neurovascular complications of surgical management for carotid body and cervical paragangliomas: a fifty-year experience with 153 tumors. J Vasc Surg 7 (1988): 284-291.
- Weber EC, Vilensky JA, Carmichael SW, et al. Netter’s Concise Radiologic Anatomy (2nd Edn). Philadelphia (PA): Elsevier (2014).
- Sevilla Garcia MA, Liorente Pendas JL, Rodrigo Tapia JP, et al. Head and neck paragangliomas: revision of 89 cases in 73 patients. Acta Otorrinolaringol Esp 58 (2007): 94-100.
- Jani P, Qureshi AA, Verma S, et al. Familial carotid body tumors: is there a role for genetic screening? J Laryngol Otol 122 (2008): 978-982.
- Shamblin WR, ReMine WH, Sheps SG, et al. Carotid body tumor (Chemodectomy): clinicopathologic analysis of ninety-cases. Amer J of Surg 122 (1971): 732-739.
- Martin TPC, Irving RM, Maher ER. The genetics of paragangliomas: a review. Clinical Otolaryngology 32 (2007): 7-11.
- Davila VJ, Chang JM, Stone WM, et al. Current surgical management of carotid body tumors. J Vasc Surg 64 (2016): 1703-1710.
- Arya S, Rao V, Juvekar S, et al. Carotid body tumors: objective criteria to predict the Shamblin group on MR imaging. Amer J Neuroradiology 29 (2008): 1349-1354.
- Prabhu M, Tupalli A, Venkataramarao SH, et al. Multiple paragangliomas at unusual sites detected on 18F-FDG PET CT. ScholArena Case Report 5 (2018): 203.
- Zhang TH, Jiang WL, Li YL, et al. Perioperative approach in the surgical management of carotid body tumors. Ann Vasc Surg 26 (2012): 775-782.
- Abu-Ghanem S, Yehuda M, Carmel NN, et al. Impact of preoperative embolization on the outcomes of carotid body tumor surgery: a meta-analysis and review of the literature. Head Neck 38 (2016): 2386-2394.
- Cobb AN, Barkat A, Daungjaiboon W, et al. Carotid body tumor resection: just as safe without preoperative embolization. Ann Vasc Surg 45 (2018): 54-59.
- Muno A. FT22. Is surgery the best option for small carotid body tumors of high altitudes? J Vasc Surg 61 (2015): 22-23.
- Valdagni R, Amichetti M. Radiation therapy of carotid body tumors. Am J Clin Oncol 13 (1990): 45-48.
- Van der Bogt KEA, Vranken Peeters MP, Van Baalen JM, et al. Resection of carotid body tumors: results of an evolving surgical technique. Ann Surg 247 (2008): 877-884.
- Sajid MS, Vijaynagar B, Singh P, et al. Literature review of cranial nerve injuries during carotid endarterectomy. Acta Chir Belg 107 (2007): 25-28.


 Impact Factor: * 4.2
Impact Factor: * 4.2 Acceptance Rate: 72.62%
Acceptance Rate: 72.62%  Time to first decision: 10.4 days
Time to first decision: 10.4 days  Time from article received to acceptance: 2-3 weeks
Time from article received to acceptance: 2-3 weeks 