A Hybrid Approach for a Minimally Invasive Resection of a Gastrointestinal Stromal Tumor
Frey Sébastien1,2*, Maubert Alexandre1,2, Benizri Emmanuel1,2
1Côte d´Azur University, Nice, France
2Department of Digestive Surgery, University Hospital Center of Nice, Nice, France
*Corresponding Author: Frey Sébastien, Côte d´Azur University, Nice, France
Received: 01 June 2020; Accepted: 10 June 2020; Published: 18 June 2020
Article Information
Citation: Frey Sébastien, Maubert Alexandre, Benizri Emmanuel. A Hybrid Approach for a Minimally Invasive Resection of a Gastrointestinal Stromal Tumor. Journal of Surgery and Research 3 (2020): 160-162.
View / Download Pdf Share at FacebookAbstract
Intragastric laparoscopic surgery has been described for the resection of gastric benign tumor located near the gastroesophageal junction. We describe here the resection of a benign tumor using a multiport intragastric laparoscopic approach. The surgery was safe and effective. Post-operative follow-up was uneventful.
Keywords
<p>Gastrointestinal Stromal Tumor, Intragastric laparoscopic</p> <gdiv></gdiv>
Article Details
Case Report
A 54-year-old male underwent, in our digestive surgery department, a gastrointestinal stromal tumor (GIST) resection performed with a multiport laparoscopic intragastric approach. A 3 cm tumor was diagnosed after a full check-up (CT-scan, upper endoscopy and endoscopic ultrasound) for chronic abdominal pain, located on the lesser curvature near the esogastric junction (Figure 1).
During the procedure, the patient was placed in a dorsal decubitus position and the lead surgeon stood on its right side. Open laparoscopy showed no local invasion nor secondary lesion. We then performed a 5 cm medial laparotomy by extending the camera port incision. An Alexis® retractor was inserted. We were able to palpate the tumor and confirm its endogastric development. Laparoscopic intragastric access was then performed using a camera port of 10 mm, a 5 mm exposure port and a 12 mm working port (Figure 1). Resection was done using an Endo-GIA stapler with two 45 cartridges after mucosal dissection (Figure 2).
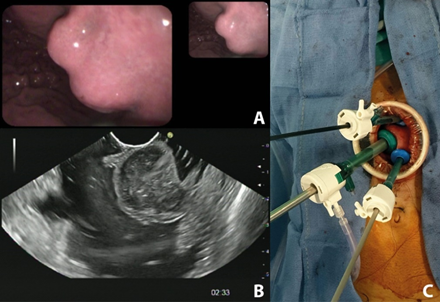
Figure 1: (a) Upper endoscopy view and (b) endoscopic ultrasound view of the tumor; (c) Per-operative view of intragastric trocar placement.
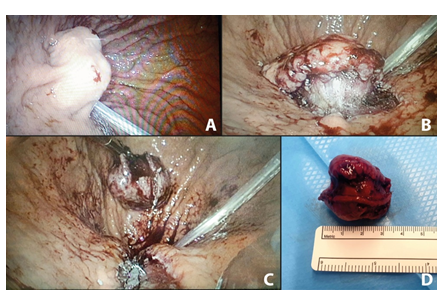
Figure 2: Per-operative endogastric view: (a) at the introduction of scope; (b) after mucosal dissection; (c) after stapling; (d) Tumor resected measuring 32 mm.
The success of this hybrid technique is due to the excellent visibility along with the possibility for a safe and a full-thickness resection. Post-operative follow-up was uneventful and discharge was authorized at day 2. Pathological examination confirmed a GIST with a clear margin. Since the first description of intragastric laparoscopic surgery in 1995, more technical and tactical advancements have been described [1, 2]. Its use for benign gastric lesions resection is now part of the surgeon arsenal, especially for tumor located near the esogastric junction (EGJ). In more recent years, the laparoscopic and endoscopic cooperative approach has been well accepted [3]. However, the endoscopic technical platform is not always accessible and the present case illustrate an easy and efficient alternative. Additionally, surgical site infection is not uncommon during full intragastric laparoscopic procedures. In our case, an Alexis® was used, offering a great exposure but also conferring a protective role of the abdominal wall. All in all, since its first description, intragastric laparoscopic surgery can be considered feasible and represents a great alternative for benign intragastric tumor resection.
Funding/Support
None of the authors has any financial interest or support to report.
Conflict of Interest/Disclosure
All authors declare that they have no conflict of interest or financial relationships, direct or indirect, with other people or organizations that could potentially and inappropriately influence the work and conclusions.
Acknowledgement
No funding was received for this study.
References
- Conrad C, Nedelcu M, Ogiso S, et al. Techniques of intragastric laparoscopic surgery. Surg Endosc 29 (2015): 202-206.
- Boulanger-Gobeil C, Gagné J-P, Julien F, et al. Laparoscopic Intragastric Resection: An Alternative Technique for Minimally Invasive Treatment of Gastric Submucosal Tumors. Annals of Surgery 267 (2018): 12-16.
- Hiki N, Nunobe S, Matsuda T, et al. Laparoscopic endoscopic cooperative surgery: Present and future aspects of LECS. Digestive Endoscopy 27 (2015): 197-204.


 Impact Factor: * 4.2
Impact Factor: * 4.2 Acceptance Rate: 72.62%
Acceptance Rate: 72.62%  Time to first decision: 10.4 days
Time to first decision: 10.4 days  Time from article received to acceptance: 2-3 weeks
Time from article received to acceptance: 2-3 weeks 