Clinicopathological Characteristics and survival analyses of Primary Mucosal Malignant Melanoma: An Experience from a Cancer of Pakistan
Masood Ur Rehman*, Osama Shakeel, Uzma Khalid, Raheem Dhanani, Hannan Ali, Abdul Wahid Anwer, Awais Amjad Malik, Shahid Khattak, Aamir Ali Syed, Raza Hussain
Department of Surgical Oncology, Shaukat Khanum Memorial Cancer Hospital and Research Centre, Johar town, Lahore, Pakistan
*Corresponding Author: Dr. Masood Ur Rehman, Department of Surgical Oncology, Shaukat Khanum Memorial Cancer Hospital and Research Centre, Johar town, Lahore, Pakistan
Received: 17 April 2021; Accepted: 23 April 2021; Published: 29 April 2021
Article Information
Citation: Masood Ur Rehman, Osama Shakeel, Uzma Khalid, Raheem Dhanani, Hannan Ali, Abdul Wahid Anwer, Awais Amjad Malik, Shahid Khattak, Aamir Ali Syed, Raza Hussain. Clinicopathological Characteristics and survival analyses of Primary Mucosal Malignant Melanoma: An Experience from a Cancer of Pakistan. Journal of Surgery and Research 4 (2021): 278-287.
View / Download Pdf Share at FacebookAbstract
Introduction: Mucosal malignant melanoma (MMM) can arise from the ocular mucosal membranes, and mucosal membranes of respiratory tract, gastrointestinal and genitourinary tract. They are rare and aggressive cancers with poor prognosis. The cornerstone of management is surgical resection along with chemotherapy and radiotherapy. The aim of the study is to analyze the clinicopathological factors and survival analyses of MMM from Pakistan population.
Methodology: During 1st January 1995 to 31st December 2018, patients presented with histological diagnosis of Primary MMM at Shaukat Khanum Memorial Cancer Hospital and Research Centre (SKMCH&RC), Pakistan were selected. It is a retrospective study with convenience sampling. Calculations were performed with Statistical Package for the Social Sciences (SPSS 20) for Windows version 20.
Results: During the span of two decades, 269 patients presented with the histological diagnosis of MMM. 163 (60.5%) patients had cutaneous malignant melanoma, 98 (36.4%) patients had MMM, five (1.8%) patients had ocular malignant melanoma and 3 (1.1%) had visceral malignant melanoma. Of all the MMM, anal canal (59.1%) was the most prevalent site, followed by mucosal melanoma of head and neck region (19.4%) and then female genital track (14.1%). One male patient also had malignant melanoma of urethra. Mean age at the diagnosis of mucosal malignant melanoma was 53 years (23-97). Median duration of symptoms was 8 months (3-36). Genital malignant melanoma had the most favorable survival outcomes of 25 months, followed by anorectal MM (22 months). The worst survival outcomes were noticed among patients with melanoma of mucosal origin from head and neck region (10 months). Median overall survival after mucosal malignant melanoma was 19 months (3-97).
<p>Mucosal malignant melanoma, Malignant melanoma, Genital melanoma, Anorectal malignant melanoma, Pakistan</p> Malignant melanomas are derived from melanin producing cells- melanocytes which are derivatives of neuroectodermal cells. Malignant melanoma frequently arises from cutaneous surfaces although they can rarely originate from mucosal ocular membranes, mucosal membranes lining respiratory tract, gastrointestinal tracts and genitourinary tracts, leptomeningeal surfaces and scarcely from internal organs [1]. Primary functions of melanocytes are pigment production in cutaneous epithelium and protection of skin from ultraviolet (UV) sun rays. The antimicrobial and immunological functions of melanocytes have been studied and their relation with innate immunity has been established [2,3]. Malignant melanomas of non-cutaneous origin are rare, non-specific, aggressive cancers and they show poor prognosis [4]. Overall survival rate and incidence of disease is low, and most of the patients report at very late stages of disease with locally advanced and metastatic disease [5] which curb the formulation of specific treatment for the disease. Therefore to circumvent current problem, it is important to make diagnosis as early as possible because prognosis gets worse with time [6]. Currently locoregional control of disease is done with surgical resection following adjuvant chemo and radio therapy which is effective but does not help with better prognosis [7]. Detailed study of clinicopathological characteristics, epidemiological factors and site specific prognostic factors is prerequisite to control disease progression as well as prompt diagnosis. These factors are not well established in cases of mucosal malignant melanoma (MMM). This study will provide the missing part of puzzle because data as well as studies on MMM from this region are scarce. Considering diverse nature of disease, it is important to know demographic details, clinicopathological characteristics, management of disease and survival outcomes for better understanding and management of this type of malignancy. During 1st January 1995 to 31st December 2018, patients presented with histopathological and radiological diagnoses of Primary MMM at Shaukat Khanum Memorial Cancer Hospital and Research Centre (SKMCH&RC), Pakistan were selected. It is a retrospective study with convenience sampling. Patients with history of cutaneous malignant melanoma or its metastatic disease at presentation were excluded. The ethical approval was sought from Institutional Review Board (IRB) of SKMCH&RC. Data was collected through human information system (HIS), electronic database of SKMCH&RC. Variables recorded were age, gender, pre surgery histopathology, clinical staging, management of disease, surgical findings, post-operative complications, and survival outcomes were recorded. As per the local guidelines of the hospital, extensive pre-operative workup was performed including baseline labs, Computed Tomography (CT) scan, Magnetic Resonance Imaging (MRI) scan and Positron Emission Tomography (PET) scan where indicated. All patients were discussed in the multi-disciplinary team (MDT) meeting. We are a paperless hospital and all patient data is put real time into a computerised Hospital Information System (HIS) by all cadres including nurses, allied health professionals and doctors. The hospital has a unique in-house developed computerised patient management system (HIS) that collects all patient information in real time including patient demographics, investigations, MDT discussions, nursing assessments, outpatient, operative notes and post- operative outcomes. As the data is collected in real time and stored, it allows for accurate retrospective review of the data. Calculations were performed with Statistical Package for the Social Sciences (SPSS 20) for Windows version 20. Data was described using median with minimum and maximum value for skewly distributed quantitative variables. For categorical variables, number of observations and percentages were reported. Kaplan Miere method was utilized for determination of survival and prognosis of disease. The study is complied with the SKMCH&RC guidelines on research involving human subjects. During the span of two decades, 269 patients presented with the histological diagnosis of malignant melanoma. 163 (60.5%) patients had cutaneous malignant melanoma, 98 (36.4%) patients had mucosal malignant melanoma, 5 (1.8%) patients had ocular malignant melanoma and 3 (1.1%) had visceral malignant melanoma. Of all the mucosal malignant melanoma, anal canal (59.1%) was the most prevalent site, followed by mucosal melanoma of head and neck region (19.4%) and then female genital track (14.1%). One male patient also had malignant melanoma of urethra. Mean age at the diagnosis of mucosal malignant melanoma was 53 years (range 23-97). 52 patients were from Punjab, 25 patients from Khyber Pakhtun Khwah (KPK), 3 were from Sindh and 2 from outside Pakistan. Males were predominantly more affected than females. Almost fifty percent of the patients with anorectal mucosal malignant melanoma presented with painless bleeding per rectum. The commonest presentations in patients with melanoma of head and neck were epistaxis and mass in the nasal cavity. In the cohort of female patients with genital MM, per-vaginal discharge and mass in the vagina were the commonest symptoms. Median duration of symptoms was 8 months (range 3-36). Genital malignant melanoma had the most favorable survival outcomes of 25 months, followed by anorectal MM (22 months). The worst survival outcomes were noticed among patients with melanoma of mucosal origin from head and neck region (10 months). Median overall survival after mucosal malignant melanoma was 19 months (range 3-97) [Figure 1, Table 1]. Figure 1: Percentages of cases on five years basis Gastrointestinal tract Head and neck Gynecologic tract Percentage 58 (59.1%) 28 (28.6%) 12 (12.2%) Age (years) 55 (23-94) 48.5 (20-85) 60 (30-70) Gender Male (61%) Male (57.1%) Female (100%) Location Anal canal (58%) Nasal cavity (42.1%) Vagina (75%) Rectum (42%) Paranasal sinus (36.8%) Vulva (25%) Oral cavity (21.1%) Symptoms Per rectal bleeding (46.2%) Epistaxis (36.8%) Per-vaginal discharge (41.7%) Altered bowel habits (30.8%) Mass (36.8%) Mass in vaginal tract (33.3%) Perineal pain (23.1%) Swelling (15.7%) Per-vaginal bleeding (16.7%) Pain (10.7%) Pain (8.3%) Treatment Surgery (44.8%) Combination (63.2%) Combination (58.3%) Palliative chemo-radiation (50%) Radiation (31.6%) Surgery alone (16.6%) Surgery alone (5.3%) Recurrence Yes (38.5%) Yes (26.3%) Yes (41.6%) Metastases Yes (61.5%) Yes (57.9%) Yes (75%) Lungs (26.9%) Cervical LNs (31.6%) Lungs (38.3%) Liver (42.3%) Spine (15.8%) Liver (20.1%) Brain (7.7%) Liver (10.5%) Brain (8.3%) Bone (7.7%) Brain (10.5%) Distant lymph node (8.3%) Median follow up 22 months (3-96) 10 months (5-16) 25 months (2-75) Table 1: Clinicopathological characteristics Primary MMM are among rare cancers when comparing them to their cutaneous counterparts. Biologically cutaneous and mucosal melanomas are two different entities despite their common origin which is from melanocytes. SKMCH&RC is the only dedicated cancer setup of Pakistan which receives patients all over Pakistan especially from the Northern areas of Pakistan and Punjab. During the last two decades, 269 patients were diagnosed with cutaneous malignant melanoma. Ninety-eight (36%) patients were histologically diagnosed as cases of primary MMM owing to fact they are less frequently occurring melanomas which has been established in other studies as well [1]. However, this number is significant. It is important to study patterns of this disease in our population because MMMs are more common in Asians [8]. Mucosal surfaces of head and neck, anal canal and female genital tracts are the commonest sites of origin. Although previous studies suggested that head and neck is the most common site out of all but our population under study shows 59.1% cases of PMM of anal canal followed by head and neck 19.4%, while 14.1% patients were of PMM of female genital tract [9]. By this data, we can say MMMs of anal canal is more prevalent mucosal melanoma out of all other kinds in this region. Male predominance has been observed in melanomas of the larynx, oral cavity, esophagus and biliary tract. Female predominance has been established in melanomas originating anorectal region and urethra [10]. This study reported that overall males were more affected with male to female ratio 3:2 in both head and neck melanomas as well as anorectal melanomas. Symptoms vary with the site of origin such as per rectal bleeding, altered bowel habits and perineal pain in anorectal mucosal originating cancers. Epistaxis, nasopharyngeal mass were the commonest symptoms in patients with head and neck mucosal melanomas. Most of the patients with melanoma of female genital tract had per vaginal discharge, per vaginal bleeding and vaginal mass. The variable presentation of these cancers has been supported by other studies as well [10-15]. Mean age at the time of presentation is 53 years while most patients present at sixth decade of life. MMM is not clinically identifiable at early stages, symptoms appear late and most of the patients presents at late stages. Median duration of symptoms in our population is 8 months. High number of cases presents with metastasis although this has not been established if there were any occult metastasis before the start of treatment. That is why one cannot comment if the current treatment is enough to control the spread of cancer cells by only studying high number of reported cases with metastasis. Mainstay of treatment is surgical resection with or without radiation although targeted radiotherapy has been proved beneficial in many cases but overall survival rate remained unaffected [16]. Most of patients come with recurrences i.e. 38.5% in anorectal, 26.3% in head and neck, 41.6% in gynecological PMMs. This study is limited as data is not enough to prove if recurrence is due to inadequate tumor resection or insufficient adjuvant or neoadjuvant therapy, hence we cannot comment on which treatment modality is better. MMMs shows worst prognosis despite sufficient treatment. This study supports that overall survival is not good for this specific disease. Out of all melanomas head and neck melanomas shows worst prognosis with mean survival of 10 months following anorectal melanomas with 22 months and anorectal melanomas with 25 months mean survival. It shows vague site specific symptoms in most cases that is why proper workup is essential not to hold off treatment process, which can pitch in and leave us to deal with few number of metastasis carcinomas. There are a few limitations of this study such as the retrospective nature which does introduce an element of bias associated with such studies. This is the first study from Pakistan reporting the clinicopathological characteristics, recurrence rate and prognosis of MMM. This study will pave the way for future research which will benefit professionals treating MMM. Primary MMM is a rare disease of aggressive nature. The prognosis of the disease varies in patients with different anatomical site. Despite of the adequate management which includes surgery, chemotherapy and radiotherapy, still the risk of local or distant recurrence is high. The study reports poor overall prognosis. This study cannot be used as a guideline for the management of disease, however this is the first study from this region which can be used as a reference point for future studies.Keywords
Article Details
1. Introduction
2. Methodology
3. Results
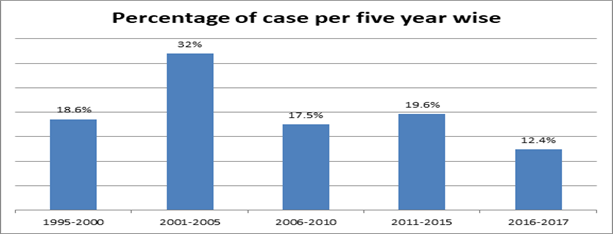
4. Discussions
5. Conclusion
References
Article Views: 1986
Journal Statistics




Discover More: Recent Articles


