Inverted-T Reduction Mammoplasty with Superomedial Pedicle for Gigantomastia - A Case Series
Romaisa Shamim Khan, Nauman Ahmed Gill*
Department of Plastic Surgery, Services Hospital, Lahore, Pakistan
*Corresponding author: Nauman Ahmed Gill, Department of Plastic Surgery, Services Hospital, Lahore, Pakistan
Received: 04 July 2021; Accepted: 12 July 2021; Published: 17 September 2021
Article Information
Citation: Romaisa Shamim Khan, Nauman Ahmed Gill. Inverted-T Reduction Mammoplasty with Superomedial Pedicle for Gigantomastia - A Case Series. Journal of Surgery and Research 4 (2021): 478-483.
View / Download Pdf Share at FacebookAbstract
Background
Gigantomastia, defined as >1500 g excess tissue per breast, is a relatively rare, physically and psychologically disabling condition. It has traditionally been approached with breast amputation and free nipple grafting. Disadvantages of this technique include uneven nipple-areolar complex (NAC) pigmentation, NAC necrosis, and complete loss of lactation. Newer techniques have been described to reduce these large breasts, while avoiding the disadvantages associated with free nipple grafting. The aim of this study was to share our experience of utilizing the superomedial pedicle technique with inverted-T mammoplasty in patients with gigantomastias.
Materials and methods
A retrospective review of all patients with gigantomastia who underwent inverted T-reduction mammoplasty with superomedial pedicle technique at Dept. of Plastic Surgery, Services Hospital, Lahore between January 2013 to December 2016 was performed. Patient demographics, preoperative breast measurements, perioperative data and post procedure patient satisfaction were analyzed. Exclusion criteria were a reduction mammoplasty weight of less than 1500 grams per breast.
Results
A total of 14 patients were included in this study. The average age at the time of surgery was 29.5 years. The average body mass index was 23.4kg/m2. Average breast resection weight was -1770 for the right and 1737g for the left breast. Average NAC transposition was 12.2cm for the right breast and 12.0cm for the left breast. Two patients developed epidermolysis of the NAC which improved with time. One patient had partial NAC necrosis. Two patients experienced partial wound dehiscence. All patients reported satisfaction with breast shape and projection.
Conclusion
Our study shows that inverted-T reduction mammoplasty with supero-medial pedicle is a safe and effective treatment modali
Keywords
<p>Gigantomastia, Reduction mammoplasty, Superomedial pedicle, Nipple-areola complex (NAC)</p>
Article Details
1. Introduction
The literal meaning of gigantomastia is excessively large breasts. The exact mechanism of its development is not well understood. Genetics, and an increased sensitivity to female hormones is thought to play a role [1,2]. It can be classified as gestational (onset in pregnancy), Juvenile (onset at puberty triggered by sex hormones), drug-induced, and Idiopathic which is the most common type. Excessively large breasts cause many functional problems for the patient, including backache, skin maceration and fungal infection [3]. Additionally, it is a significant cause of emotional embarrassment to the patient, who often find it difficult to buy appropriate clothing. As a result they start avoiding social gatherings. In the literature, different cut-off values have been stated to define the norms, as well as to define what constitutes gigantomastia. The most commonly used systems classify the excessive growth with respect to the amount of breast tissue requiring reduction. Excessive breast tissue <1500 grams per breast is termed macromastia. Where the excess breast tissue amounts to >1500 grams per breast it is labelled as gigantomastia [4]. Reduction mammoplasty is the surgical treatment for enlarged breasts4. Several different surgical techniques are described in textbooks for breast reduction in macromastia. All of these share a basic common principle, which is that the NAC is carried on a pedicle of tissue, while the desired amount of breast tissue is removed from the remaining breast. The techniques differ in the type of pedicle utilized and is named accordingly [5-7]. In the cases of gigantomastia, breast amputation, with free NAC graft had been recommended by some surgeons. Though this technique is versatile in leaving behind the desired amount and shape of breast tissue, often the nipple graft does not produce an aesthetically pleasing result. Complications associated with free NAC grafts range from uneven pigmentation to total NAC loss. Also, this results in complete loss of lactation [8]. The superomedial pedicle conserves the NAC and reduces the morbidity associated with breast amputation and NAC graft, and can be considered the treatment of choice for gigantomastia [9-11]. In the present case series, we share our experience of inverted T reduction mammoplasty with superomedial pedicle for gigantomastia.
2. Materials and Methods
A retrospective review was performed of all patients who presented with gigantomastia at the department of plastic surgery at Services Hospital Lahore between January 2013 and December 2016.
2.1 Inclusion criteria: All patients who underwent Inverted-T reduction mammoplasty with superomedial pedicle, in which the excised breast tissue weighed 1500 grams and above were included in the study.
2.2 Exclusion criteria: Patients with comorbid conditions such as peripheral vascular disease, Ischemic heart disease, uncontrolled HTN and DM were excluded.
After obtaining informed consent, patient demographics including age, weight, and BMI were recorded. The patient’s charts were reviewed in detail. Preoperative breast measurements, resection weight per breast (measured per-operatively) and post-operative complications, specifically wound dehiscence and NAC appearance, were noted. Breast measurements were again taken at 1 month post-op. Mid-clavicle to nipple distance was measured pre-and post-operatively. NAC transposition was calculated as the difference between these two readings. All patients completed at least 6 months of follow-up. Patient satisfaction was assessed on two parameters, ‘projection’ and NAC appearance, at 6 months. This was done on a scale of 1 (very dissatisfied) to 5 (very satisfied). All data was entered on excel sheets and analyzed using SPSS v 20.
3. Results
A total of 14 patients were included in the study. Mean age was 29.5 years (SD=8.2), and mean BMI was 23.4kg/m² (SD=1.7). There were 2 patients with juvenile gigantomastia, the remaining were idiopathic. The per-operative resection parameters are depicted in table 1.
|
Resection weight (grams) mean(SD) |
NAC transposition (cm) mean (SD) |
|
|
Right breast |
1770 (135) |
12.2 (2.9) |
|
Left breast |
1737 (191) |
12.0 (2.3) |
Table 1: Resection parameters
The modal score for patient satisfaction was 4 (satisfied) with regard to both breast shape and Nipple appearance. None of the patients reported being dissatisfied with the result (figure 1). Complications were encountered in five patients, the details of which are elaborated in table 2. A few of our results are shown in figure 2 with pre and post op outcomes.
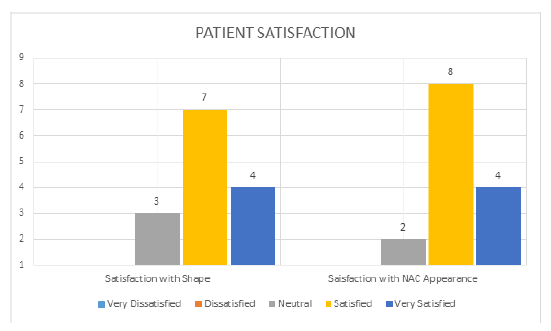
Figure 1: Patient satisfaction
|
Complication |
N |
Management |
|
NAC epidermolysis (1 unilateral, 1 bilateral) |
2 |
Conservative |
|
Partial NAC necrosis, (unilateral) |
1 |
Conservative |
|
Wound dehiscense |
2 |
1 managed conservatively |
Table 2: Complications and their management
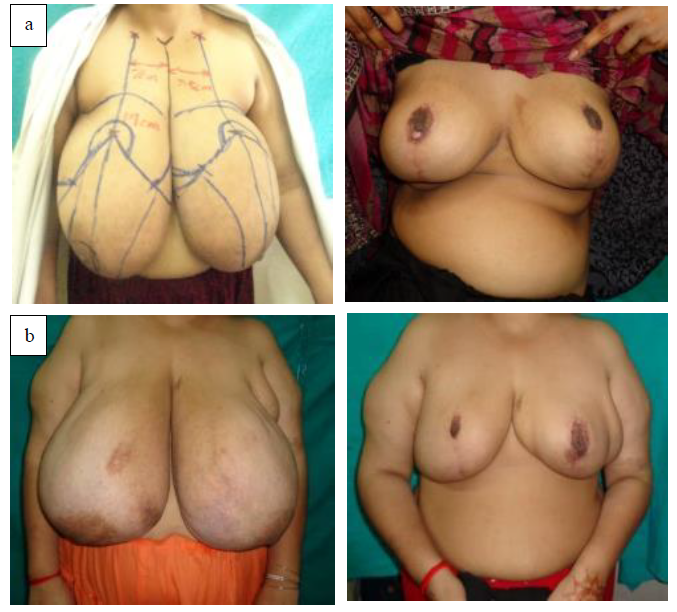
Figure 2: Pre and post op outcomes of two of our patients with gigantomastia.
4. Discussion
Large breasts cause significant functional problems for the patient, they are also a cause of psycho-social embarrassment [1,2]. Breast enlargement is treated surgically with reduction mammoplasty. There are several techniques described with regards to which pedicle is used and what incision is given. In all these techniques, the NAC is carried on a pedicle of tissue that maintains its blood supply. Excessively large breasts, also termed Gigantomastia, have traditionally been surgically treated with breast amputation. In this procedure, the excessive tissue is removed in a wise pattern excision. The NAC is then harvested from the excised tissue and placed at the desired position as a graft. There are certain complications of free nipple grafting: partial/complete graft loss, uneven pigmentation, and complete absence of lactation. As the NAC is the most prominent part of the breast, an aesthetically pleasing and natural looking NAC is paramount to the self-confidence of such patients.
In this study, we present our series of patients with gigantomastia who instead of breast amputation, underwent inverted T reduction mammoplasty with superomedial pedicle. All were operated upon by a single surgeon. Our technique involves raising skin flaps of only 2cm thickness, as it has been demonstrated that the blood vessels supplying the breast skin are travelling within 2 cm of the skin surface [12,13]. An inverted T scar pattern was used as it better allows ease of resection medially and laterally.
The mean age of patients in our study was 28 years. This is similar to mean age quoted in other studies on patients with gigantomastia. Mean BMI was 23.4kg/m2. This value is slightly higher than that seen in other studies [9]. The mean resection weight was 1770 for right breast and 1737 for the left. This value is higher than seen in most studies where superomedial pedicle reduction mammoplasty is done. Similarly mean NAC transposition is somewhat higher than documented for superomedial pedicle [9,10]. The reason for this difference is likely that for this particular study we deliberately included patients with more than 1500gm excess tissue per breast. Though all patients documented improvement in physical symptoms of fatigue and back pain, this was not objectively assessed. This however is an invariable outcome of any procedure that will reduce breast size [14,15]. Of more interest was patient satisfaction with breast shape and NAC appearance. Most of the patients were satisfied with both parameters studied. A few reported being ‘neutral’. Wound dehiscence at the T-junction was encountered in 2 out of 14 patients (14%). This rate is similar to that seen in other studies [16]. NAC epidermolysis was seen in 2 of 14 patients (14%). It settled completely with time in both patients. Partial necrosis of NAC was seen in 1 patient (7%), and this too is comparable to other studies.
5. Conclusion
Inverted T reduction mammoplasty using the superomedial pedicle is a safe and effective surgical technique for treatment of gigantomastia. It may be superior to breast amputation with respect to the NAC appearance.
References
- Noczynska A, Wasikowa R, Myczkowski T. Hypersensitivity of estrogen receptors as a cause of gigantomasty in two girls. Polski merkuriusz lekarski: organ Polskiego Towarzystwa Lekarskiego 11 (2001): 507-509.
- Ohlsén L, Ericsson O, Beausang-Linder M. Rapid, massive and unphysiological breast enlargement. European Journal of Plastic Surgery 19 (1996): 307-313.
- Baker SB, Burkey BA, Thornton P, et al. Juvenile gigantomastia: presentation of four cases and review of the literature. Annals of plastic surgery 46 (2001): 517-526.
- Dancey A, Khan M, Dawson J, et al. Gigantomastia- a classification and review of the literature. Journal of Plastic, Reconstructive & Aesthetic Surgery 61 (2008): 493-502.
- Dex EA, Asplund O, Ardehali B, et al. A method to select patients for vertical scar or inverted-T pattern breast reduction. Journal of plastic, reconstructive & aesthetic surgery 61 (2008): 1294-1302.
- Wettstein R, Christofides E, Pittet B, et al. Superior pedicle breast reduction for hypertrophy with massive ptosis. Journal of plastic, reconstructive & aesthetic surgery 64 (2011): 500-507.
- Deventer PV, Graewe FR. Enhanching pedicle safety in mastopexy and breast reduction procedures: the posteroinferomedial pedicle, retaining the medial vertical ligament of Würinger. Plast Reconstr Surg 126 (2010): 786-793.
- Agbenorku P. Nipple-areolar complex (NAC) composite grafts in the management of macromastia: review of complications. Nigerian Journal of Surgical Research 8 (2006).
- Altuntas ZK, Kamburoglu HO, Yavuz N, et al. Long-term changes in nipple-areolar complex position and inferior pole length in superomedial pedicle inverted ‘t’scar reduction mammaplasty. Aesthetic plastic surgery 39 (2015): 325-330.
- Fernandez S, Coady L, Cohen-Shohet R, et al. Comparative outcomes and quality analysis of inverted-T and pure vertical scar techniques in superomedial pedicle reduction mammaplasty. Annals of plastic surgery 76 (2016): 328-331.
- Khalil HH, Malahias M, Shetty G. Triangular lipodermal flaps in wise pattern reduction mammoplasty (superomedial pedicle): A novel technique to reduce T-junction necrosis. Plastic Surgery 24 (2016): 191-194.
- Van Deventer PV, Graewe FR. The blood supply of the breast revisited. Plastic and reconstructive surgery 137 (2016): 1388-1397.
- Mon O’Dey D, Prescher A, Pallua N. Vascular reliability of nipple-areola complex- bearing pedicles: an anatomical microdissection study. Plastic and reconstructive surgery 119 (2007): 1167-1177.
- Spector JA, Singh SP, Karp NS. Outcomes after breast reduction: does size really matter ? Annals of Plastic Surgery 60 (2008): 505-509.
- Ogunleye AA, Leroux O, Morrison N, et al. Complications after reduction mammaplasty: a comparison of wise pattern/inferior pedicle and vertical scar/superomedial pedicle. Annals of plastic surgery 79 (2017): 13-16.
- Ulusal BG, Alper I. In pursuit of effective volume reduction and enhanced aesthetics for treatment of gigantomastia using superior dermoglandular pedicle. Aesthetic plastic surgery 42 (2018): 412-421.


 Impact Factor: * 4.2
Impact Factor: * 4.2 Acceptance Rate: 72.62%
Acceptance Rate: 72.62%  Time to first decision: 10.4 days
Time to first decision: 10.4 days  Time from article received to acceptance: 2-3 weeks
Time from article received to acceptance: 2-3 weeks 