Favism in the Elderly
Carme Gomila Sintes1, Sara Bernal2,3, Ester Rojas2, Pilar Leoz Alegretti4, Matias Nicolas Flores Orella1, Antonio Jorge Betbesé Roig5
1Critical Care Unit, Hospital de la Santa Creu i Sant Pau, 08041 Barcelona, Spain
2Genetics Department and Sant Pau Biomedical Research Institute, Hospital de la Santa Creu i Sant Pau, 08041 Barcelona, Spain
3Rare Diseases Network Biomedical Research Center (CIBERER ), Instituto de Salud Carlos III, 28029 Madrid, Spain.
4Hematology Department, Hospital de la Santa Creu i Sant Pau, 08041 Barcelona, Spain
5Critical Care Unit and Sant Pau Biomedical Research Institute, Hospital de la Santa Creu i Sant Pau, 08041 Barcelona, Spain
*Corresponding Author: Carme Gomila Sintes, Critical Care Unit, Hospital de la Santa Creu i Sant Pau, Barcelona, Spain
Received: 17 May 2022; Accepted: 09 June 2022; Published: 08 August 2022
Article Information
Citation: Carme Gomila Sintes, Sara Bernal, Ester Rojas, Pilar Leoz Alegretti, Matias Nicolas Flores Orella, Antonio Jorge Betbesé Roig. Favism in the Elderly. Archives of Clinical and Medical Case Reports 6 (2022): 582-585.
View / Download Pdf Share at FacebookAbstract
G6PD deficiency is an X-linked, hereditary genetic disorder. G6DP gene is located on the long arm of this chromosome (Xq28). The most common clinical manifestations are neonatal jaundice and acute hemolytic anemia, which in most patients is triggered by an exogenous agent (infection, ingestion of fava beans (favism) or exposure to an oxidative drug). Favism is most frequently diagnosed in children below 5 years of age, whereas its diagnose in adulthood is relatively uncommon, even more in the elderly. We outline a case of an elderly male who required admission to the Intensive Care Unit because of a severe hemolysis and acute kidney injury after fava beans ingestion.
Keywords
Glucose-6-phosphate dehydrogenase deficiency; favism; elderly; hemolytic anemia; acute kidney injury
Glucose-6-phosphate dehydrogenase deficiency articles; favism articles; elderly articles; hemolytic anemia articles; acute kidney injury articles
Glucose-6-phosphate dehydrogenase deficiency articles Glucose-6-phosphate dehydrogenase deficiency Research articles Glucose-6-phosphate dehydrogenase deficiency review articles Glucose-6-phosphate dehydrogenase deficiency PubMed articles Glucose-6-phosphate dehydrogenase deficiency PubMed Central articles Glucose-6-phosphate dehydrogenase deficiency 2023 articles Glucose-6-phosphate dehydrogenase deficiency 2024 articles Glucose-6-phosphate dehydrogenase deficiency Scopus articles Glucose-6-phosphate dehydrogenase deficiency impact factor journals Glucose-6-phosphate dehydrogenase deficiency Scopus journals Glucose-6-phosphate dehydrogenase deficiency PubMed journals Glucose-6-phosphate dehydrogenase deficiency medical journals Glucose-6-phosphate dehydrogenase deficiency free journals Glucose-6-phosphate dehydrogenase deficiency best journals Glucose-6-phosphate dehydrogenase deficiency top journals Glucose-6-phosphate dehydrogenase deficiency free medical journals Glucose-6-phosphate dehydrogenase deficiency famous journals Glucose-6-phosphate dehydrogenase deficiency Google Scholar indexed journals COVID-19 articles COVID-19 Research articles COVID-19 review articles COVID-19 PubMed articles COVID-19 PubMed Central articles COVID-19 2023 articles COVID-19 2024 articles COVID-19 Scopus articles COVID-19 impact factor journals COVID-19 Scopus journals COVID-19 PubMed journals COVID-19 medical journals COVID-19 free journals COVID-19 best journals COVID-19 top journals COVID-19 free medical journals COVID-19 famous journals COVID-19 Google Scholar indexed journals SARS-Cov2 articles SARS-Cov2 Research articles SARS-Cov2 review articles SARS-Cov2 PubMed articles SARS-Cov2 PubMed Central articles SARS-Cov2 2023 articles SARS-Cov2 2024 articles SARS-Cov2 Scopus articles SARS-Cov2 impact factor journals SARS-Cov2 Scopus journals SARS-Cov2 PubMed journals SARS-Cov2 medical journals SARS-Cov2 free journals SARS-Cov2 best journals SARS-Cov2 top journals SARS-Cov2 free medical journals SARS-Cov2 famous journals SARS-Cov2 Google Scholar indexed journals dehydrogenase deficiency articles dehydrogenase deficiency Research articles dehydrogenase deficiency review articles dehydrogenase deficiency PubMed articles dehydrogenase deficiency PubMed Central articles dehydrogenase deficiency 2023 articles dehydrogenase deficiency 2024 articles dehydrogenase deficiency Scopus articles dehydrogenase deficiency impact factor journals dehydrogenase deficiency Scopus journals dehydrogenase deficiency PubMed journals dehydrogenase deficiency medical journals dehydrogenase deficiency free journals dehydrogenase deficiency best journals dehydrogenase deficiency top journals dehydrogenase deficiency free medical journals dehydrogenase deficiency famous journals dehydrogenase deficiency Google Scholar indexed journals Chemotherapy articles Chemotherapy Research articles Chemotherapy review articles Chemotherapy PubMed articles Chemotherapy PubMed Central articles Chemotherapy 2023 articles Chemotherapy 2024 articles Chemotherapy Scopus articles Chemotherapy impact factor journals Chemotherapy Scopus journals Chemotherapy PubMed journals Chemotherapy medical journals Chemotherapy free journals Chemotherapy best journals Chemotherapy top journals Chemotherapy free medical journals Chemotherapy famous journals Chemotherapy Google Scholar indexed journals treatment articles treatment Research articles treatment review articles treatment PubMed articles treatment PubMed Central articles treatment 2023 articles treatment 2024 articles treatment Scopus articles treatment impact factor journals treatment Scopus journals treatment PubMed journals treatment medical journals treatment free journals treatment best journals treatment top journals treatment free medical journals treatment famous journals treatment Google Scholar indexed journals CT articles CT Research articles CT review articles CT PubMed articles CT PubMed Central articles CT 2023 articles CT 2024 articles CT Scopus articles CT impact factor journals CT Scopus journals CT PubMed journals CT medical journals CT free journals CT best journals CT top journals CT free medical journals CT famous journals CT Google Scholar indexed journals favism articles favism Research articles favism review articles favism PubMed articles favism PubMed Central articles favism 2023 articles favism 2024 articles favism Scopus articles favism impact factor journals favism Scopus journals favism PubMed journals favism medical journals favism free journals favism best journals favism top journals favism free medical journals favism famous journals favism Google Scholar indexed journals hemolytic anemia articles hemolytic anemia Research articles hemolytic anemia review articles hemolytic anemia PubMed articles hemolytic anemia PubMed Central articles hemolytic anemia 2023 articles hemolytic anemia 2024 articles hemolytic anemia Scopus articles hemolytic anemia impact factor journals hemolytic anemia Scopus journals hemolytic anemia PubMed journals hemolytic anemia medical journals hemolytic anemia free journals hemolytic anemia best journals hemolytic anemia top journals hemolytic anemia free medical journals hemolytic anemia famous journals hemolytic anemia Google Scholar indexed journals acute kidney injury articles acute kidney injury Research articles acute kidney injury review articles acute kidney injury PubMed articles acute kidney injury PubMed Central articles acute kidney injury 2023 articles acute kidney injury 2024 articles acute kidney injury Scopus articles acute kidney injury impact factor journals acute kidney injury Scopus journals acute kidney injury PubMed journals acute kidney injury medical journals acute kidney injury free journals acute kidney injury best journals acute kidney injury top journals acute kidney injury free medical journals acute kidney injury famous journals acute kidney injury Google Scholar indexed journals
Article Details
Abbreviations:
G6DP: Glucose-6-phosphate dehydrogenase; ICU: Intensive Care Unit; LDH: Lactate dehydrogenase; GCS: Glasgow coma scale; AKI: Acute kidney injury; DNA: Deoxyribonucleic acid; PCR: Polymerase chain reaction; HGVS: Human Genome Variation Society; NADP: nicotinamide-adenine dinucleotide phosphate.
1. Introduction
We report a case about an elderly male who presented with severe hemolytic anemia in the context of an unknown Glucose-6-phosphate dehydrogenase (G6PD) enzyme deficiency.
2. Case Presentation
A 78-year-old male with a medical history of dyslipidemia, hyperthyroidism and peripheral artery disease was admitted in the Emergency department with a 24-hour history of dark urine without other symptoms.
Initial blood tests revealed mild normocytic anemia with hemoglobin value of 119 g/L (previous 157 g/L), reticulocyteosis and anisocytosis with excentrocites in the blood smear. No-schistocytes were found. LDH was 826 U/L, total bilirubin was 119 µmol/L (indirect bilirubin 108 µmol/L) and haptoglobin was < 0.08 g/L. Direct Coombs test was negative.
Kidney function was normal. Non-immune hemolytic anemia was suspected and patient was admitted to the Hematology ward. In 24 hours, the patient’s level of consciousness worsened (GCS 13-14), hemoglobin fell down to 54 g/L and he developed an acute kidney injury (KDIGO 3) with urea 36 mmol/L, creatinine 338 µmol/L and anuria due to its prerenal condition. In addition, he presented atrial fibrillation with rapid ventricular response (150 bpm).
The patient was transferred to the Intensive Care Unit (ICU) as prerenal AKI could not be reversed, where a hemodialysis catheter was placed and continuous renal replacement therapy was started. During his admission, three packed of red blood cells were transfused. The anamnesis was repeated and patient’s family revealed that few hours before the beginning of symptoms, the patient had ingested fava beans. Although they confirmed that he had previously consumed fava beans in the past, he never developed any symptoms. Then, a genetic study was performed to diagnose favism (see methodology). A genetic variant in the G6PD gene was identified in hemizygous state in the patient [ChrX(GRCh37):153774276T>C), it is a missense change that involves the substitution of an amino acid by other in the protein encoded by this gene [p. (His32Arg )].
According to the guidelines of the American College of Medical Genetics and Genomics (ACMG) this genetic variant in the G6PD gene is classified as pathogenic [1]. In the databases consulted (LOVD3 and ClinVar), this same genetic variant is described in other patients with G6PD deficiency [2]. This study confirmed G6PD genetic disorder.
After starting renal replacement therapy, transfusing red blood cell concentrates and performing volume replacement, the patient’s level of consciousness improved and sinus rhythm was recovered. Hemoglobin remained stable, around 80 g/L, without new transfusions. The liver profile improved progressively, up to a bilirubin of 7 µmol/L at discharge from the ICU, decreasing jaundice and normalization of the urine color. AKI persisted and the patient continued requiring intermittent hemodialysis every 48 hours. Patient was discharged to the Hematology ward 13 days after admission.
3. Methodology
3.1 DNA Extraction
Following informed consent, EDTA anticoagulated blood samples were collected. Genomic DNA was automatically extracted from peripheral leukocytes using QIAsymphony technology (Qiagen) by magnetic particles.
3.2 Mutation analysis
Primers corresponding to the complete coding sequence and intronic adjacent regions of the Glucose-6-phosphate dehydrogenase (G6PD) gene (2-13 exons) were designed according to Primer 3 v.4.1.0 software and entry NM_001360016.2 by UCSC Genome Browser on Human (GRCh37/hg19) database.
PCR amplification was performed in a final volume of 25 µL that contained 0.2 µM of each primer, 0.5 units of MyTaq™ DNA Polymerase in the recommended buffer and 150-200 ng of genomic DNA. The thermocycling conditions used were as follows: 94°C for 2min, followed by 30 cycles at 94 °C for 30s (denaturation step), 58°C for 30s (annealing primers) and 72°C for 30s, followed by a 10 min final extension step at 72°C.
When PCR amplification products were completed, any inconsumable dNTPs and primers remaining in the PCR product mixture were removed by ExoSAP digestion enzyme. After the clean-up procedure was completed, the bidirectional sequencing reaction was performed by the Sanger method using Big Dye v.1.1. Terminator chemistry.
The sequencing reactions of the fragments amplified were cleaned by a Montage SEQ96 kit on a vacuum manifold prior to their subjection to capillary electrophoresis on an ABI Prism 3500 genetic analyzer (Applied Biosystems). Sequence chromatograms were analyzed using SeqScape v.2.7 software. Mutations and genetic variants were described according to NM_001360016.2 reference sequence and the Human Genome Variation Society (HGVS) nomenclature [3].
4. Discussion
G6PD is an enzyme that catalyzes the first reaction in the pentose phosphate pathway converting glucose-6-phosphate to 6-phosphogluconolactone and reducing the cofactor nicotinamide-adenine dinucleotide phosphate (NADP) to reduced form of nicotinamide adenine dinucleotide phosphate (NADPH). Consequently, this reaction provides reduced power to all cells in the form of NADPH. NADPH enables cells to counterbalance oxidative stress that can be triggered by several oxidant agents [4] (Figure 1).
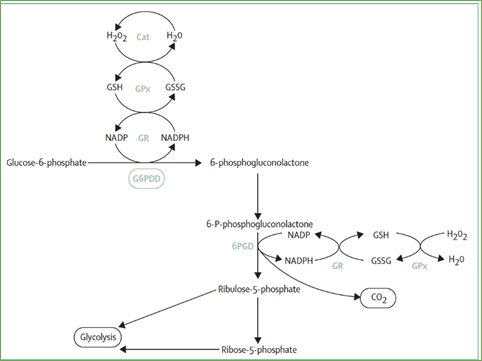
Figure 1: Pentose phosphate pathway
Since red blood cells do not contain mitochondria, the pentose phosphate pathway is their only source of NADPH; therefore, this pathway is necessary to protect the cell against oxidative damage.
G6PD deficiency is an X-linked, hereditary genetic disorder. G6PD gene is located on the long arm of this chromosome (Xq28). Then, this disease is more frequent in males and most females are heterozygotes. This genetic defect is caused by mutations in the G6PD gene, most of which are single-base substitutions leading to amino acid replacements. Rarely, a second mutation is presented. This results in protein variants, with different levels of enzyme activity, which are associated with a wide range of biochemical and clinical phenotypes. The G6PD-deficient variants are grouped into different classes corresponding with disease severity [5-6] (Table 1). Our patient was included in class II.
|
Class |
Level of deficiency |
Enzyme activity |
Prevalence |
|
I |
Severe |
Chronic nonspherocytic hemolytic anemia in the presence of normal erythrocyte function |
Uncommon; occurs across populations |
|
II |
Severe |
< 10% of normal activity |
Varies; more common in Asian and Mediterranean populations |
|
III |
Moderate |
10 - 60% of normal activity |
10% of black males in the United States |
|
IV |
Mild to none |
Normal activity (60 - 150%) |
Rare |
|
V |
None |
Increased activity (> 150%) |
Rare |
Table 1: Classification of G6PD deficiency.
Deficient G6PD alleles are distributed worldwide; a conservative estimation is that at least 400 million people carry a mutation in the G6PD gene causing deficiency [4]. The highest prevalence is reported in Africa, Mediterranean, the Middle East, Southeast Asia, and the central and southern Pacific islands. However, because of fairly recent migration, deficient alleles are nowadays quite prevalent in North and South America and in some parts of northern Europe. The most common clinical manifestations are neonatal jaundice and acute hemolytic anemia, which in most patients is triggered by an exogenous agent (infection, ingestion of fava beans or exposure to an oxidative drug).
Focusing on favism, this disease presents as an acute hemolytic anemia in a G6PD-deficient individual following the ingestion of broad beans (Vicia faba), usually 24 hours after the ingestion. It is the form of presentation most frequently associated with the Mediterranean variant of G6PD deficiency. Not all G6PD-deficient individuals undergo favism after ingestion of fava beans, and even the same individual can have an unpredictable response, suggesting that several factors affect development of the disorder (health of the patient and the amount of fava beans ingested). It occurs most frequently in children below 5 years of age, is relatively uncommon in adults [7] and extremely rare in elderly. It can be fatal. The Mediterranean-type G6PD deficiency is common in our population and usually it is not difficult to diagnose. We have reported this case because favism can be encountered in daily clinical practice but is extremely rare to be diagnosed in elderly and specially upon ICU admission. Additionally, the mutation presented in our patient seems to be more frequent in Asia [2]. As long as the family genetic study is still to be completed and as far as we know, our patient did not have any Asian genetic background. Genetic counseling is recommended to evaluate these results according to the clinical and family context. G6PD deficiency is inherited in X-linked pattern. Patient's daughters are mandatory carriers to G6PD deficiency. Heterozygous female carriers have a risk of 50% of transmitting the pathogenic variant in each pregnancy.
5. Conclusion
In summary, G6PD deficiency should be suspected in cases of Coombs-negative hemolytic anemia where the patient has an exogenous trigger (infection, drugs or fava beans). Our case presents distinctive and exceptional aspects: first, that hemolytic events due to G6PD deficiency could present with different degrees of severity in the same patient (he had ingested fava beans previously without any symptomatology); second, it appeared in the elderly; third, he required ICU admission; and last, he presented an Asiatic mutation in spite of his Mediterranean origin.
Acknowledgements
N/A
Conflict of Interest
None of the authors have any conflict of interest to report
References
- Richards S, et al. ACMG Laboratory Quality Assurance Committee. Standards and guidelines for the interpretation of sequence variants: a joint consensus recommendation of the American College of Medical Genetics and Genomics and the Association for Molecular Pathology Genet Med 17 (2015): 405-24.
- Fu C, et al. Newborn screening of glucose-6-phosphate dehydrogenase deficiency in Guangxi, China: determination of optimal cutoff value to identify heterozygous female neonates. Sci Rep 8 (2018): 833.
- den Dunnen JT, Dalgleish R, Maglott DR, et al. On behalf of the Human Genome Variation Society (HGVS), the Human Variome Project (HVP), and the Human Genome Organisation (HUGO). HGVS Recommendations for the Description of Sequence Variants: 2016 Update. Hum Mutat 37 (2016): 564-569.
- Capellini M, Fiorelli G. Glucose-6-phosphate dehydrogenase deficiency. Lancet 2008; 371:64-74
- WHO Working Group. Glucose-6-phosphate dehydrogenase deficiency. Bull World Health Organ 67 (1989): 601-611.
- Frank JE. Diagnosis and management of G6PD deficiency. Am Fam Physician 72 (2005): 1277-82.
- Belsoy MA. The epidemiology of favism. Bulletin of the World Health Organization 48 (1973): 1-13.


 Impact Factor: * 5.3
Impact Factor: * 5.3 Acceptance Rate: 75.63%
Acceptance Rate: 75.63%  Time to first decision: 10.4 days
Time to first decision: 10.4 days  Time from article received to acceptance: 2-3 weeks
Time from article received to acceptance: 2-3 weeks 
