Effectiveness of Structured Training Programme Regarding Adult Basic Life Support on Knowledge of Nurses` in Zoba Maekel and National Referral Hospitals, Eritrea, 2018
Filmon Abraham Ghirmai1*, Ghidey Ghebreyowhanness Weldeghiorgis2, Teklu Tsegay Bahlebi3, Eyasu Habte Tesfamariam1
1Asmara College of health Sciences, School of Nursing, Asmara, Eritrea
2Dean Asmara College of Health Sciences, Asmara, Eritrea
3Orrota Medical Surgical National Referral Hospital, Emergency department, Asmara, Eritrea 4Asmara College of Health Sciences, School of public Health, Asmara, Eritrea
*Corresponding Author: Filmon Abraham Ghirmai, Asmara College of health Sciences, School of Nursing, Asmara, Eritrea.
Received: 29 August 2022; Accepted: 07 September 2022; Published: 17 October 2022
Article Information
Citation: Filmon Abraham Ghirmai, Ghidey Ghebreyowhanness Weldeghiorgis, Teklu Tsegay Bahlebi, Eyasu Habte Tesfamariam. Effectiveness of Structured Training Programme Regarding Adult Basic Life Support on Knowledge of Nurses` in Zoba Maekel and National Referral Hospitals, Eritrea, 2018. Archives of Clinical and Medical Case Reports 6 (2022): 693-701.
View / Download Pdf Share at FacebookAbstract
Background: In Eritrea nurses provide most of the health care in the primary, secondary and tertiary level health facilities. The rate of trauma and medical emergencies are on the increase so nurses should have adequate and updated knowledge on Basic Life Support in order to be able to implement effective interventions in cardiac arrest situations.
Aim: The objective of this study was to assess the effectiveness of structured training programme regarding Adult Basic Life Support on knowledge of nurses.
Method: A quasi-experimental single group, pretest-posttest and retest design was utilized. Forty (40) nurses’ participated in the study. Structured and modified questionnaire was used to collect data. Data were analyzed using the Statistical Package for Social Sciences (SPSS) Version 22.0 program. Frequencies, percentages, mean and standard deviation was used to describe the data. One way repeated measures of ANOVA was used to check the possible change in knowledge of the nurses at preintervention, immediate and three months’ after intervention. A p-value < 0.05 was considered to be statistically significant.
Results: The findings showed an acquisition of Adult Basic Life Support knowledge among the study participants following a four hour Basic Life Support training programme. Before training, the mean score of the study participant on knowledge questions was 9.58/20 and none of the respondents got a pass mark. Immediately after the training the mean score of the study participants was increased to 15.9/20 and 55.0% of the study participant got a passing mark. Significant deterioration from the immediate training score was found three months following Basic Life Support training as score was decreased to 14.9 and 40% of the respondents got a pass
Keywords
<p>Basic Life Support; Cardiopulmonary Resuscitation; Knowledge; Nurses; Training</p>
Article Details
Abbreviations: ACLS- Advanced Cardiac Life Support; ALS- Advanced Life Support; AHA- American Heart Association; BCLS- Basic Cardiac Life Support; BLS- Basic Cardiac Life Support; BSN- Bachelor of Science in Nursing; CPR- Cardio Pulmonary Resuscitation; EMS- Emergency Medical Service; MoH- Ministry of Health; ICN- International Council of Nurses; ICU- Intensive Care Unit; ERC- European Resuscitation Council.
1. Background
In the last 45 years, BLS has elevated from experimental technique to a clinically universal life saving procedure. As a result all health care professionals are expected to know and be proficient with the steps [1]. Many countries have guidelines on how to provide basic life support (BLS) which are formulated by professional medical bodies in those countries. The guidelines outline algorithms for the management of a number of conditions, such as cardiac arrest, choking and drowning. The American Heart Association and European Resuscitation Council establish the standards for BLS and are actively involved in teaching Basic Cardiac Life Support (BCLS) and Advanced Cardiac Life Support (ACLS) to health professionals. The American Heart Association recommends that nurses and physicians working with patients be certified in BCLS and ACLS. Certification involves attending formal classes and passing cognitive and motor skill tests. Basic life support is a first line of response to a cardiac arrest in the interim before defibrillation and advanced life support are available and it’s timely provision can save a precious life [2,3]. Both the European Resuscitation guidelines and the American Heart Association recommend that all hospital staff with patient contact should have regular resuscitation training. However, in Eritrea, there is no regulatory mandate for nurses to attend BLS instruction or re-certification programmes. This situation is unique and therefore, it is conceivable, that nurses may be receiving the majority of their BLS training during the early stages of an educational programme. In the clinical setting, nurses are the first people to see cases of cardiac arrest therefore, they should be the first to initiate and perform BLS without losing time [4]. It was considered amongst the duties of all healthcare team members to possess BLS knowledge and skills [5, 6]. Having the cognitive knowledge that is necessary for the effective performance of BLS in cardiac arrest situations makes someone to be competent in BLS [7], this study further defines BLS competency as encompassing both the acquisition and retention of CPR cognitive knowledge. Health care professionals have varied level of BLS knowledge even in the developed countries. Inadequate level of BLS knowledge amongst nurses was found in studies conducted in United States of America (USA) [8], the United Kingdom (UK) [7], Finland [9] and Ireland [3]. Similar trend was also observed in countries like Bahrain [10], Greece [11], Nigeria [12] South Africa [13] and Ethiopia [14] but to our knowledge no previous study has been conducted in Eritrea to determine the effect of BLS training on the knowledge of nurses. Studies conducted to assess the effect of training on the knowledge of nurses’ towards BLS showed improvements in the cognitive knowledge of nurses [1, 3, 12, 15]. From the literature it is also clear that the cognitive knowledge of BLS cannot be acquired or retained easily by nurses. Studies report different levels of cognitive knowledge in individual BLS knowledge and skill components that vary dramatically along a continuum from 0% to 100% [1, 3, 4, 16]. BLS retention is defined as retaining the cognitive knowledge that helps to perform BLS effectively at a certain point in time after BLS training [17]. The retention of CPR knowledge is a key factor in determining BLS competence [7]. However, there is universal evidence to suggest that BLS knowledge is poorly retained across populations [1, 3, 7, 16, 18]. A review of studies on CPR retention revealed that there was a significant deterioration in the level of knowledge of nurses from the immediate after training [1, 3, 19]. The purpose of this study was to evaluate the effectiveness of structured training programme regarding adult basic life support on knowledge of nurses` in Zoba Maekel and the two national referral hospitals, Eritrea, 2018, with the following objectives: [I] to assess nurses knowledge toward Adult BLS before taking the course, [II] to determine the effect of attending adult BLS course on the knowledge of nurses towards adult BLS [III] to evaluate the level of retention of the cognitive knowledge.
1.1 Study Setting
The study was conducted in all Zoba Maekel Health facilities and the two National Referral Hospitals (ORROTTA and HALIBET).
Zoba Maekel is one of the six zones of Eritrea and is found in the center of the country. In Zoba Maekel there are 37 health facilities that range from zonal referral hospitals to health station. Orotta and Halibet hospitals are national referrals which provide medical and surgical services to patients from all zones of Eritrea.
1.2 Study Design
A quasi-experimental single group pretest intervention posttest and retest after three months was done.
1.3 Study Subjects
The target population comprised all nurses (degree nurse, diploma nurse and associate nurses) working in all Zoba Maekel health facilities and the two National Referral Hospitals.
1.4 Sample Size and Sampling Technique
The sample size was calculated using G*power software after considering the effect size (medium=0.25), type I error (0.05), power (0.80), correlation among measurements (0.55), and sphericity (ε=0.5) of one group followed up at three time points. Depending on those parameters the calculated sample size was 40 nurses. After sample size was calculated, strata were formed by virtue of the level of health facilities (National Referral Hospitals, Zonal Referral Hospitals, Community Hospitals, Health center and Health Station). Finally, samples were randomly selected from each stratum, proportionately distributed as per nurses’ level (Degree, Diploma nurse, and Associate nurse). All nurses who were willing and randomly selected were included in the study.
1.5 Data Collection Tool
Structured questionnaire was used to collect data. The questionnaire was adopted [1,3] and was modified. The questionnaire contains two parts. Part one has demographic characteristics such as age, gender, marital status, work experience, academic qualifications, work department, frequency of Basic Life Support done in their setting and any formal BLS training attended. Part two is a written examination containing 20 multiple choice questions with a single best answer for each and a minimum score of 17(85%) is required to pass the examination [1,3,20].
1.6 Reliability and Validity
The 2015 Guidelines of BLS specified by the European Resuscitation Council was followed. The content validity of the instrument was enhanced through evaluation by two nurse researchers, two anesthetists, critical care clinical specialist and a statistician.
1.7 Data Collection Procedure
During the pre-test phase first, each respondents completed multiple-choice questionnaire. After this, certified BLS instructors provided a four-hour BLS training session [1]. The post-test was conducted immediately after the BLS training. Then the re-test was conducted three months after the first training. This time frame was considered as an appropriate delay between intervention and re-testing as it was previously used in a similar study [1, 3, 20]. The CPR training programme consisted of a 4 hours theory and practical course based on the European Resuscitation Council 2015 guidelines. This included theory class on heart disease, risk factors and epidemiology of heart disease, the steps in adult Basic Life support one-rescuer and demonstrations of the steps in adult Basic Life support.
1.8 Data Management
Data were analyzed using the Statistical Package for Social Sciences (SPSS) Version 22.0 program. Frequency, percentages, mean and standard deviation was used to describe the data. To investigate the effect of training on the changes in knowledge, scores of the nurses at pre, immediate post and 3 months after intervention, repeated measures ANOVA was utilized. A p-value < 0.05 was considered to be statistically significant in all the analysis.
1.9 Ethical Consideration
Permission to collect data was granted from the Ministry of Health research committees; Eritrea, from Zoba Maekel branch office, from the two National Referral hospitals and from the Research and Ethics Committee of the College of Health Sciences. A covering letter was attached to each questionnaire, explaining the details of the study. Participation was voluntary and informed written consent was provided by each participant. The right to decline or to withdraw from the study at any stage without incurring any penalty was explained. All data were coded and kept locked up, accessible only to the researchers and the statistician.
2. Results
2.1 Demographic Characteristics of Study Participants
|
Variable |
Number |
Percent |
|
Gender |
||
|
Male |
15 |
37.5 |
|
Female |
25 |
62.5 |
|
Age (Mean=32.7, SD=6.8, Min.=23 and Max.=52) |
||
|
Less than 30 |
20 |
50 |
|
30 to 39 |
11 |
27.5 |
|
Greater or equal 40 |
9 |
22.5 |
|
Place of Work |
||
|
National Referral Hospital |
16 |
40 |
|
Zonal Referral Hospital |
8 |
20 |
|
Community Hospital |
8 |
20 |
|
Health Center |
6 |
15 |
|
Health Station |
2 |
5 |
|
Qualification |
||
|
Associate Nurse |
16 |
40 |
|
Diploma Nurse |
15 |
37.5 |
|
Degree Nurse |
9 |
22.5 |
|
Work Experience median=6, IQR=6 |
||
|
Less than 4 years |
14 |
35 |
|
5 to 10 years |
17 |
42.5 |
|
Greater or equal to 11 years |
9 |
22.5 |
|
Department |
||
|
Adult |
27 |
67.5 |
|
Pediatric |
6 |
15 |
|
Maternity |
7 |
17.5 |
Table 1: Socio-demographic characteristics of the study participants (n=40).
Abbreviations: SD- Standard Deviation; Min- Minimum; Max- Maximum; IQR- Interquartile Range.
Table 1 shows the demographic characteristics of the study participants. Female nurses contributed 62.5% (n=25) of the sample while male nurses contributed 37.5% (n=15) of the sample. The mean age of the respondents was 32.7 years (SD=6.8) and half (n=20) of the respondents were less than 30 years, followed by 27.5% (11) nurses of ages between 30 to 39, and 22.5% (9) were 40 years old or older. Most of the study participants, (40%, n=16) were from national referral hospitals, followed by zonal referral hospitals (20%, n=8), community hospitals (15%, n=6), health centers (15%,n=6), and health stations (5%, n=2). The academic qualification of the respondents shows that, most respondents 40% (16) were trained in certificate level, 37.5% (15) were diploma nurse and the remaining 22.5% (9) had possessed bachelor’s degrees in nursing science. Less than half (42.5% n=17) of the respondents possessed 5-10 years of work experience, 35% (14) had less than 4 years of work experience, 22.5%(9) were having greater than or equal to eleven years of work experience. The respondents were from three working departments; such that 67.5% (27) from Adult Medical-Surgical Department, 17.5% (7) nurses from maternity and 15% (6) nurses from pediatric department. Table 2 shows majority, 67.5% (27) of the study participants did not attend any pre-service training, on the other hand 70% (27) of the respondents attended formal training about BLS in their hospital. In order to determine the frequency of BLS attempts, the respondents were asked how often they had performed CPR in their clinical settings. The results on table 2 shows that 40% (16) of the respondents had never participated in resuscitation attempts at all, 30% (12) were performing annually, 22.5% (9) respondents were performing BLS on a monthly basis, 5% (2) on a daily basis and the remaining 2.5% (1) were performing on weekly basis.
|
Variable |
Frequency |
Percent |
|
BLS Class in college |
||
|
Yes |
13 |
32.5 |
|
No |
27 |
67.5 |
|
BLS Training in hospital |
||
|
Yes |
28 |
70 |
|
No |
12 |
30 |
|
Frequency of BLS Performance |
||
|
Never |
16 |
40 |
|
Daily |
2 |
5 |
|
Weekly |
1 |
2.5 |
|
Monthly |
9 |
22.5 |
|
Annually |
12 |
30 |
Table 2: Background of study participants on Basic Life Support (n=40).
Abbreviations: BLS- Basic Life Support.
2.2 Knowledge of Respondents regarding Adult Basic Life Support
Knowledge of the nurses under this study was assessed using a questionnaire that had mainly 3 domains, namely, general knowledge in BLS, steps in BLS, and chest compression in BLS. The number of items in the domains of general knowledge, steps in BLS, and chest compression were 9, 6 and 5 respectively.
Knowledge of Study Participants on the Domain Related to General Knowledge about Basic Life Support
Before intervention, 42.5% of the respondents correctly knew CPR abbreviation and only 5% of the respondents correctly identified the steps in initiating CPR. However, the percentage of knowledge for both CPR abbreviation and steps in initiating CPR steadily increased to 95% immediately after intervention, even though, slight decline had occurred 3 months later. Considerable improvement in the knowledge of the respondents immediately after intervention on brain survival without oxygen (55% to 97.5%), how to recognize someone in need of CPR (67.5% to 85%), and best way to give mouth to mouth ventilation (67.5% to 82.5%) was observed. Even though much difference in percentage was not observed immediately after intervention, increase in proportion of respondents regarding the knowledge of the goal of CPR (72.5% to 90%), and about the maneuver not used to open the airway (62.5% to 95%) was observed 3 months after the intervention. Paradoxically, immediate after training, a decrease in percentage was observed on respondents who correctly knew the benefit of minimizing interruptions during compression.
|
General knowledge |
Pre-intervention n (%) |
Immediate Post n (%) |
3 months later n (%) |
|
|
CPR Abbreviation |
||||
|
Correct |
17(42.5%) |
38(95%) |
36(90%) |
|
|
Incorrect |
23(57.25%) |
2(5%) |
4(10%) |
|
|
Brain survival without oxygen |
||||
|
Correct |
22(55%) |
39(97.5%) |
31(77.5) |
|
|
Incorrect |
18(45%) |
1(2.5%) |
9(22.5%) |
|
|
The organ that cannot survive without oxygen |
||||
|
Correct |
25(62.5%) |
29(72.5%) |
31(77.5%) |
|
|
Incorrect |
15(37.5%) |
11(27.5%) |
9(22.5%) |
|
|
The goal of CPR |
||||
|
Correct |
30(75%) |
29(72.5%) |
36(90%) |
|
|
Incorrect |
10(25%) |
11(27.5%) |
4(10%) |
|
|
Steps for initiating CPR |
||||
|
Correct |
2(5%) |
38(95%) |
29(72.5%) |
|
|
Incorrect |
38(95%) |
2(5%) |
11(27.5%) |
|
|
How to recognize someone in need of CPR |
||||
|
Correct |
27(67.5%) |
34(85%) |
29(72.5%) |
|
|
Incorrect |
13(32.5%) |
6(15%) |
11(27.5%) |
|
|
Benefit of minimizing interruptions during compression |
||||
|
Correct |
31(77.5%) |
22(72.5%) |
23(57.5%) |
|
|
Incorrect |
9(22.5%) |
18(27.5%) |
17(42.5%) |
|
|
Best way to give mouth to mouth ventilation |
||||
|
Correct |
27(67.5%) |
33(82.5%) |
32(80%) |
|
|
Incorrect |
13(32.5%) |
7(17.5%) |
8(20%) |
|
|
Maneuver not used to open the airway |
||||
|
Correct |
22(55%) |
25(62.5%) |
38(95%) |
|
|
Incorrect |
18(45%) |
15(37.5%) |
2(5%) |
|
Table 3: Responses of study participants on domains related to general knowledge about Basic Life Support (n=40).
Abbreviations: CPR- Cardiopulmonary Resuscitation.
2.3 Knowledge of Respondents on the Domain Related to Steps on BLS
Before intervention more than 50% of study participants failed to answer what the next step is after patient lie unconscious (52.5%), what to do next if patient has no response (75.0%), what to do next after 30 compressions and two breaths (62.5%) and fail to arrange steps in correct order (90.0%). Immediate after intervention, marked improvement was recorded in identifying next step after 30 compressions and two breaths (37.5% to 95.0%),what to do next after patient lie unconscious (47.5% to 82.5%) and what to do if patient has no response (25.0% to 57.5%) even though there was some reduction three month after intervention. On putting the steps on correct sequence, even though marked improvement was seen after intervention (10.0% to 45.0%) still less than half of the study participants can correctly order it. Before intervention the number of respondents who knew on what to do if patient is breathing but unresponsive was 62.5% and after intervention it was increased to 87.5%. After training, slight decrease was observed in the number of respondents who knew what to do if no scene of danger (55.0% to 52.5%).
|
Steps on BLS |
Pre-intervention n (%) |
Immediate Post n (%) |
3 months later n (%) |
|
|
What you will do next if no scene of danger |
||||
|
Correct |
22(55%) |
21(52.5%) |
20(50%) |
|
|
Incorrect |
18(45%) |
19(47.5%) |
20(50%) |
|
|
What you will do next if patient lie unconscious in safe place |
||||
|
Correct |
19(47.5%) |
33(82.5%) |
27(67.5) |
|
|
Incorrect |
21(52.5%) |
7(17.5%) |
13(32.5%) |
|
|
Putting in correct sequence |
||||
|
Correct |
4(10%) |
18(45%) |
21(52.5%) |
|
|
Incorrect |
36(90%) |
22(55%) |
19(47.5%) |
|
|
What will you do next if patient do not have response |
||||
|
Correct |
10(25%) |
23(57.5%) |
16(40%) |
|
|
Incorrect |
30(75%) |
17(42.5%) |
24(60%) |
|
|
What will you do next after 30 compression and 2 breaths |
||||
|
Correct |
15(37.5%) |
38(95%) |
34(85%) |
|
|
Incorrect |
25(62.5%) |
2(5%) |
6(15%) |
|
|
what will you if victim starts breathing but is unresponsive |
||||
|
Correct |
25(62.5%) |
35(87.5%) |
38(95%) |
|
|
Incorrect |
15(37.5%) |
5(12.5%) |
2(5%) |
|
Table 4: Knowledge of respondents on the domain related to steps on Basic Life Support (n=40).
2.4 Knowledge of Study Participants on the Domain Related to Compression During BLS
Before intervention 65.0% of the respondents correctly knew the compression to ventilation ratio, but on the position of hand during compression, depth of compression, rate of compression, and maximum interruption during compression, the number of respondents who correctly knew were 42.5%, 40.0%, 20.0% and 30.0% respectively. Immediate after training, on all items that asses’ respondents’ knowledge on compression, good improvement was seen in the number of participants who responded correctly. Three month after intervention, slight decrease was observed in the number of participants who responded correctly to most of these items.
|
Compression |
Pre-intervention n (%) |
Immediate Post n (%) |
3 months later n (%) |
|
Hand position during compression |
|||
|
Correct |
17(42.5%) |
35(87.5%) |
36(90%) |
|
Incorrect |
23(57.5%) |
5(12.5%) |
4(10%) |
|
Compression to ventilation ratio |
|||
|
Correct |
26(65%) |
40(100%) |
38(95%) |
|
Incorrect |
14(35%) |
0(0%) |
2(5%) |
|
Depth of chest compression |
|||
|
Correct |
16(40%) |
32(80%) |
32(80%) |
|
Incorrect |
24(60%) |
8(20%) |
8(20%) |
|
Rate of chest compression |
|||
|
Correct |
8(20%) |
38(95%) |
35(87.5%) |
|
Incorrect |
32(80%) |
2(5.0%) |
5(12.5%) |
|
Maximum interruption during compression |
|||
|
Correct |
12(30%) |
29(72.5%) |
28(70.0%) |
|
Incorrect |
28(70%) |
11(27.5%) |
12(30.0%) |
Table 5: Respondents knowledge on the domain related to compression during BLS (n=40).
2.5 Overall Knowledge Status
The pass mark for the knowledge is a score of 85% or above. Accordingly, none of the study participants got a passing mark on knowledge about Basic Life Support before the intervention. However, 55.0% (n=22) and 40% (n=16) of the participants got a passing mark right after intervention and 3 months later, respectively.
2.6 Effect of Intervention on Knowledge of Study Participants Through Time
A one way repeated measures ANOVA was conducted to look over the contribution of an educational intervention on the knowledge scores of the study participants through time. Total of 40 participants were taken in the study and no missing data was found at the three time periods. The average knowledge scores at time 1(prior to the intervention), Time 2 (following the intervention) and Time 3 (three month after intervention) were 9.58 (SD±2.81), 15.9 (SD±3.53), and 14.88 (SD±3.63) respectively (Table 6). Mauchly’s test indicated that there was an evidence of sphericity (Mauchly’s W=0.88, p=0.089). Hence, assuming sphericity, significant effect for time (p<0.001) was found using univariate ANOVA. Moreover, significant effect for time (Wilks’ Lambda=0.189, F (2, 38) = 81.3, p<0.001), was observed using multivariate ANOVA (Multivariate partial eta squared =0.811).
|
Time Period |
N |
Mean (SD) |
Test of Sphericity |
Wilk’s Lambda |
RANOVA p-value |
|
|
Time 1 (pre-intervention) |
40 |
9.58(2.81) |
Mauchly’s W=0.88 |
Wilk’sλ=0.189 F(2,38)=81.3 |
||
|
Time 2 (Post intervention) |
40 |
15.9(3.53) |
p=0.089 |
p<0.0001 |
<0.0001 |
|
|
Time 3 (3-month followup) |
40 |
14.88(3.63) |
partial eta squared=0.811 |
Table 6: Comparison of participants’ level of knowledge at Time 1, Time 2 and Time 3 (n=40).
Furthermore, Bonferroni post-hoc test revealed that the knowledge of study participants have significantly higher at immediate post intervention than pre-intervention (p<0.001), 3 months later than pre-intervention (p<0.001), and immediate post intervention than 3 months later (p =0.025). In addition, a significant linear trend in the level of knowledge was observed across the three time periods (p<0.001).
|
Post-hoc Comparison |
Mean Difference (95% CI) |
p-value |
p-value for Trend |
|
|
Immediate post and pre-intervention |
6.33(5.08-7.57) |
<0.001 |
<0.001 |
|
|
3 months later and pre-intervention |
5.30(4.07-6.53) |
<0.001 |
||
|
Immediate post and 3 months later |
1.03 (0.10-1.95) |
0.025 |
Table 7: Post-hoc comparison for the knowledge of study participants (n=40).
As shown in figure 2, immediate after intervention there was marked improvement in knowledge of study participants while three months after intervention it shows slight decrement.
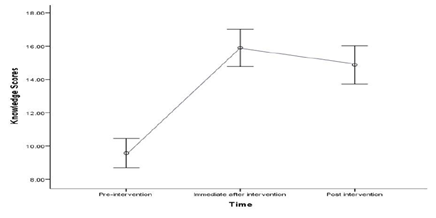
Figure 2: Error plot for Knowledge.
3. Discussion
Knowledgeable nurses can implement effective BLS interventions to save patients’ lives. This study’s findings emphasize on the importance of increasing the BLS knowledge of nurses, as no one passed the BLS pre-test and significant deterioration was seen three months after the training.
3.1 Knowledge of Study Participants on Basic Life Support
In this study, as it is shown in table 3, less than half of the study participants correctly answered CPR abbreviation and steps to initiate CPR before training was given. This clearly indicate that majority of the nurses were not familiar with the resuscitation procedure. In contrast to this, a study done in Nigeria by [12] on dental students, found that all the respondents knew the full abbreviation of CPR. As reflected in table 5, more than one third of the respondents failed to know the position of the hand during compression and depth of compression. This could be because the study participants were not updated with the latest resuscitation protocols as the guideline is updated every five years. As shown in table 5, the pre-test knowledge of the study participants indicated that majority of the respondents did not know the correct compression/ventilation ratio, the compression rate, maximum interruption during compression, when to start compression and what to do next after 30 compression and 2 breaths. These are critical skills for increasing the survival rate of patients because the primary determinant of a successful neurological outcome is the maintenance of adequate circulatory and respiratory support during prolonged cardiac arrest – something that is only achieved by continual chest compressions. Ignorance about these steps reduces the patient’s chances of survival during resuscitation [1]. This result was consistent with a similar research done in Ireland [3] and in Botswana [1]. As indicated in figure 1, the study participants lacked BLS knowledge in the pre-test as no one got a passing mark. This finding is consistent with previous studies [1, 3, 7, 19]. After the CPR training programme, as shown in table 3, more than 90% of the respondents knew the abbreviation of CPR and steps to initiate CPR. This marked increment could be attributed to the effect of training. Immediate after intervention, as indicated in table 5, on all items that assess respondents’ knowledge on the domain related to compression, good improvement was seen in the number of participants who responded correctly. This shows that nurses should be trained with updated guidelines to be equipped with current theories and practices. Following the CPR training program, as shown in figure 1, there was a significant acquisition in respondents’ CPR cognitive knowledge as 55% of the study participants got a passing mark, which supports the findings of [1, 3, 7, 15]. While this showed a positive training effect, it is of concern that over one third of respondents did not meet the pass standard following BLS instruction. This may be attributed to information overload (because the training was new to most of the respondents), and individual capacity of the respondents (some of the respondents were associate nurses and were old age) following the training programme, which may have negatively influenced respondents’ performance. Three month after training, as indicated in figure 1, significant deterioration was seen in the respondents’ CPR cognitive knowledge as the number of respondents who got a passing mark reduced from 55% to 40%. Other related studies also documented similar findings [1, 3, 7, 15]. As shown in table 6, a significant effect of intervention on knowledge of the respondents was shown through time. When the mean score between the pre-test & immediate post-test, immediate post & retention test and pretest & retention test was compared statistically significant difference was found. These findings indicate that it is imperative for the respondents to receive regular, periodic in-service CPR courses, updating nurses on the latest CPR techniques, technologies and developments. The ability of nurses to perform BLS and to maintain their CPR skills and knowledge are indispensable professional requirements of all nurses working in healthcare settings [21].
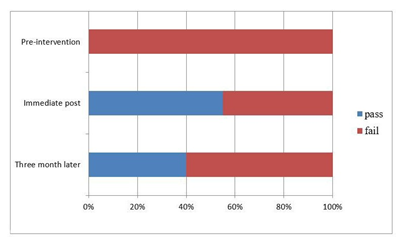
Figure 1: Knowledge Status of respondents through time (n=40).
Strengths and Limitations
The major limitations of this study were the small population and sample size, in addition to the study being conducted in one geographical location, in Zoba Maekel. This prevents making inferences about similar populations of nurses in Eritrea.
4. Conclusion
The acquisition and retention of BLS knowledge is largely dependent on training and frequency of CPR instruction [20] and the findings from this study strongly supports this. Ultimately, the goal is to prepare nurses who are competent and confident in the event of a cardiac related emergency. It is recommended that the provision of an ongoing structured programme of basic life support is necessary. This is particularly fundamental in the critical years of an undergraduate nursing programme and critical to Eritrean nurses due to lack of mandatory requirements for CPR instruction.
Declarations
Ethics Approval and Consent to Participate
This study was approved by the Ministry of Health ethical committee. Participation in this study was voluntary. Written consent was sought. Submission of responses to the questionnaire was considered to constitute implied consent. The voluntary nature of participating in the research was made explicit and unambiguous in the cover letter. The investigators did not coerce or entice anyone to complete the questionnaire. Any participant could decline to return the questionnaire.
Consent for Publication
Not applicable.
Availability of Data and Materials
Most of the data supporting our findings is contained within the manuscript, and all others, excluding identifying/confidential respondent data should, will be shared upon request.
Competing Interests
The authors declare that they have no competing interests.
Funding
Fund is secured by the government of Eritrea (Ministry of Finance) through National Higher Education and Research Institute, Eritrea (NHERI). The institute usually provides fund to thesis for completion of masters’ degree.
Authors’ Contributions
GAF contributed to concept development, proposal writing, data collection analysis and interpretation, manuscript drafting and preparation and final writing, WGG contributed to concept development, proposal writing, analysis and interpretation. BTT contributed to concept development, proposal writing, data collection and manuscript drafting, and THE contributed to research proposal writing, analysis and interpretation. All authors read and approved the final manuscript.
Acknowledgments
We express our gratitude to Asmara college of Health Sciences and the Ministry of Health, Eritrea, for granting us the permission to conduct the study. We wish to express our sincere appreciation to Dr. Ghimja Fesssehaye, Associate Dean of research and post graduate study in Asmara College of Health Sciences, for the technical assistance and Mr. Andom Yohannes, Head School of Nursing, for his support guidance and valuable comments. We thank all nurses who sacrificed their time and energy to participate in the study.
References
- Rajeswaran L, Ehlers VJ. Cardiopulmonary resuscitation knowledge and skills of registered nurses in Botswana. Curationis 37 (2014): 1-7.
- Yunus M, Mishra A, Karim HM, et al. Knowledge, attitude and practice of basic life support among junior doctors and students in a tertiary care medical institute. Int J Res Med Sci 3 (2015): 3644.
- Madden C. Undergraduate nursing students’ acquisition and retention of CPR knowledge and skills. Nurse education today 26 (2006): 218-227.
- Terzi B, Düzkaya DS. Evaluation of basic life support training program provided for nurses in a university hospital. International Journal of Medical Research & Health Sciences 6 (2017): 70-76.
- Etkinliginin AP. Degerlendirilmesi. TAF Preventive Medicine Bulletin 12 (2013): 151-156.
- Özdogan M, Agalar F, Eryilmaz M, et al. Prehospital life support in trauma patients: basic or advanced trauma life support. Ulus Travma Acil Cerrahi Derg 12 (2006): 87-94.
- Broomfield R. A quasi-experimental research to investigate the retention of basic cardiopulmonary resuscitation skills and knowledge by qualified nurses following a course in professional development. Journal of Advanced Nursing 23 (1996): 1016-1023.
- Dane FC, Russell-Lindgren KS, Parish DC, et al. In-hospital resuscitation: association between ACLS training and survival to discharge. Resuscitation 47 (2000): 83-87.
- Hopstock LA. Cardiopulmonary resuscitation; use, training and self-confidence in skills. A self-report study among hospital personnel. Scandinavian journal of trauma, resuscitation and emergency medicine 16 (2008): 18.
- Marzooq H, Lyneham J. Cardiopulmonary resuscitation knowledge among nurses working in Bahrain. International Journal of Nursing Practice 15 (2009): 294-302.
- Passali C, Pantazopoulos I, Dontas I, et al. Evaluation of nurses’ and doctors’ knowledge of basic & advanced life support resuscitation guidelines. Nurse education in practice 11 (2011): 365-369.
- Owojuyigbe AM, Adenekan AT, Faponle AF, et al. Impact of basic life support training on the knowledge of basic life support in a group of Nigerian Dental Students. Nigerian Postgraduate Medical Journal 22 (2015): 164.
- Govender K, Rangiah C, Ross A, et al. Retention of knowledge of and skills in cardiopulmonary resuscitation among healthcare providers after training. South African Family Practice 52 (2010): 459-462.
- Tsegaye W, Tesfaye M, Alemu M. Knowledge Attitude and Practice of Cardiopulmonary Resuscitation and associated factors in Ethiopian University Medical Students. J en Practice 3 (2015): 206-210.
- Goswami R, Kanika, Sembian N. Effectiveness of Training Program on Knowledge and Practices Regarding Basic Life Support (BLS) Among Nursing Students. Int J Clin Anesthesiol 3 (2015): 1046-1050.
- Adekola OO, Menkiti DI, Desalu I. How much do we Remember after CPR Training?–Experience from a Sub-Saharan Teaching Hospital. Analg Resusc: Curr Res S1 4 (2013): 5-6.
- Greig M, Elliott D, Parboteeah S, et al. Basic life support skill acquisition and retention in student nurses undertaking a pre-registration diploma in higher education/nursing course. Nurse education today 16 (1996): 28-31.
- Handley AJ, Koster R, Monsieurs K, et al. European Resuscitation Council Guidelines for Resuscitation 2005: Section 2. Adult basic life support and use of automated external defibrillators. Resuscitation 67 (2005): S7-23.
- Nori JM, Saghafinia M, Motamedi MK, et al. CPR training for nurses: how often is it necessary?. Iranian Red Crescent Medical Journal 14 (2012): 104.
- Berden HJ, Willems FF, Hendrick JM, et al. How frequently should basic cardiopulmonary resuscitation training be repeated to maintain adequate skills?. BMJ: British Medical Journal 306 (1993): 1576.
- Hamilton R. Nurses’ knowledge and skill retention following cardiopulmonary resuscitation training: a review of the literature. Journal of advanced nursing 51 (2005): 288-297.
- Sherman M. The new American Heart Association cardiopulmonary resuscitation guidelines: should children and adults have to share?. Current opinion in paediatrics 19 (2007): 253-257.
- Resuscitation Council of Southern Africa. Basic Life Support for healthcare providers (2005).
- Monsieurs KG, Nolan JP, Bossaert LL, et al. European resuscitation council guidelines for resuscitation 2015 section 1. Executive summary. Resuscitation.-Limerick, 1972, currens 95 (2015): 1-80.


 Impact Factor: * 5.3
Impact Factor: * 5.3 Acceptance Rate: 75.63%
Acceptance Rate: 75.63%  Time to first decision: 10.4 days
Time to first decision: 10.4 days  Time from article received to acceptance: 2-3 weeks
Time from article received to acceptance: 2-3 weeks 
