Human Parainfluenza Serotype 3 Viral Myocarditis Complicated with Ventricular Tachycardia
Chanceline Formisano1, Alain Kenfak Foguena2, Valery S Effoe3, James Tataw Ashu2*
1Medicentre Tavannes, Grand-Rue 32, 2710 Tavannes (Be), Switzerland
2Hopital du Jura bernois SA, Moutier, Beausite 49 2740 Moutier (Be), Switzerland
3Division of Cardiology, Morehouse School of Medicine, Atlanta, Georgia USA
*Corresponding Author: Dr. James Tataw Ashu, Hopital du Jura bernois SA, Moutier, Beausite 49 2740 Moutier (Be), Switzerland
Received: 13 December 2020; Accepted: 11 January 2021; Published: 18 January 2021
Article Information
Citation: Chanceline Formisano, Alain Kenfak Foguena, Valery S Effoe, James Tataw Ashu. Human Parainfluenza Serotype 3 Viral Myocarditis Complicated with Ventricular Tachycardia. Archives of Clinical and Medical Case Reports 5 (2021): 156-161.
View / Download Pdf Share at FacebookAbstract
Background: Viral myocarditis is a leading cause of mortality and cardiovascular morbidity. Its clinical manifestation is heterogeneous varying from asymptomatic courses to presentations with ventricular arrhythmias, heart failure and cardiogenic shock. Right ventricular endomyocardial biopsy is the gold standard in confirming the diagnosis; however, this may not be readily available in some clinical settings. For identification of the viral causative agent, the expanded use of polymerase chain reaction (PCR) techniques may facilitate precise viral genomic diagnosis and improve outcomes.
Case presentation: We report a case of a 56 -year-old female patient who presented to the hospital with chest pain mimicking an acute coronary syndrome and stable monomorphic ventricular tachycardia. She had a medical history notable for permanent pacemaker placement due to high-degree atrioventricular block, Brugada-like syndrome and venous thromboembolic disease. Her high-sensitivity troponin was elevated, evidence of myocardial injury, and an echocardiogram showed an ejection fraction of 55% with no wall motion abnormalities. She was managed with IV Amiodarone with subsequent cardioversion. Coronary angiography performed after cardioversion ruled out ischemia as the cause of her ventricular tachycardia. Examination of the nasopharyngal swap by PCR showed a Human Parainfluenza Virus type 3 (HPIV-3), the most likely culprit for her myocardial injury. The presumptive diagnosis of myocarditis complicated with ventricular tachycardia was made after ruling out other common etiologies.
Conclusion: This case illustrates a mild presentation of myocarditis and the diagnostic challenge that may ensue due to the lack of specificity of their clinical presentation and the limitation to perform biopsies or cardiac magnetic resonance imaging.<
Keywords
<p>Myocarditis; Ventricular tachycardia; Type three Parainfluenza</p>
Article Details
1. Introduction
Myocarditis is defined as the inflammation of the heart muscle according to clinical and histopathological criteria.
The disease can be of infectious origin either (viral, bacterial or mycotic) or non-infectious (inflammatory, intoxication, autoimmune, drug related) [1]. The clinical presentation is variable and the gold standard for diagnosis is via a myocardial biopsy. However, this procedure is invasive and carries some degree of risk. As such, the diagnosis can be presumed based on the clinical presentation coupled with noninvasive testing such as a cardiac magnetic resonance imaging test [2].
The progression of this condition, in milder forms, is most favorable without sequelae, but one quarter of the patients will develop long-term cardiomyopathy and another quarter will require a heart transplant [1].
2. Case Description
A 56-year-old female patient presented to the hospital with sudden onset of retrosternal severe pressure-like chest pain aggravated by breathing radiating to the left shoulder and jaw, associated with palpitations and NYHA functional Class III dyspnea. She mentioned having had dry cough without fever or Coryza symptoms in the 72 hours preceding her hospital visit. Notable medical history included Steinert myotonic dystrophy with repeated episodes of cardiac conduction disorders, including high degree atrioventricular block and Brugada-like syndrome for which she had a permanent pacemaker (DDD mode) implanted 3 years prior. A recent device interrogation showed a normal functioning device. No structural heart disease had been reported on previous echocardiograms. Otherwise, she had been on acenocoumarol (a warfarin derivative) for a previous lower limb deep vein thrombosis.
On admission, her vital signs were: respiratory frequency of 26 breaths / min, oxygen saturation of 95% on 4 liters of supplemental oxygen through a nasal cannula, blood pressure of 103/71 mmHg, heart rate of 220 beats/min and temperature of 37.0°C. her physical examination was significant only for mild wheezing and distended jugular veins. A 12-lead electrocardiogram (ECG) revealed ventricular tachycardia (VT) (Figure 1). Her condition was managed as stable monomorphic VT with intravenous infusion of 150 mg of Amiodarone. A repeat ECG following cardioversion revealed a sinus rhythm, left bundle branch block and a first-degree AV block (Figure 2). Owing to the constellation of cough, dyspnea, hypoxemia and in a context of type 2 respiratory failure (pH 7.39, PCo2 50 mmHg, P02 65.6 mmHg, bicarbonate 28.3 mmol/l, Chloride 109 mmol/l) and subsequent fever, she was commenced on empirical antibiotic therapy with intravenous Co-Amoxicillin for suspected community-acquired pneumonia. An elevated high-sensitivity cardiac troponin (2500 ng/l) suggested myocardial injury. She underwent left heart catheterization with coronary angiography, which was unremarkable for ischemia. Transthoracic echocardiogram revealed a globally normal left ventricle with an ejection fraction of 55% with normal sizes of the left atrium as well as the right cavities. Chest CT was negative for an infectious focus and pulmonary embolism. Blood cultures were negative.
Thereafter, she was admitted in our intermediary care unit for cardiac monitoring awaiting other results. Due to persistent dyspnea with hypoxemia and hypercapnia, she underwent non-invasive ventilation (NIV). Subsequently, three days after admission a respiratory panel of her nasopharyngeal swab (NPS) sample taken for microbiological studies was positive through polymerase chain reaction (PCR) for Human para influenza virus serotype 3 (HPIV-3). Antibiotic therapy was stopped, and symptomatic treatment was pursued with a slowly favorable course.
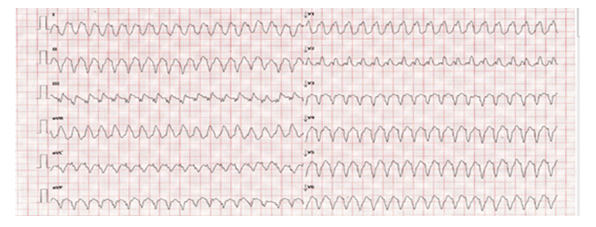
Figure 1: initial electrocardiogram showing ventricular tachycardia.
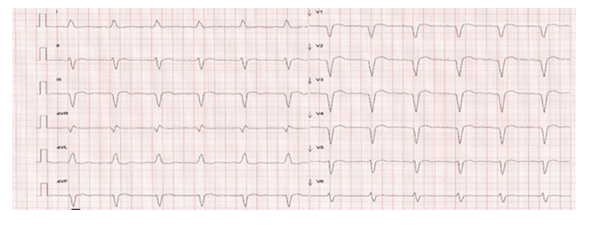
Figure 2. Electrocardiogram after 150 mg of Amiodarone. Left bundle branch bloc and first degree AV block.
3. Discussion
In our case, the diagnosis of acute viral myocarditis was challenging owing to her non-specific clinical presentation and the absence of more specific imaging modalities, such as cardiac MRI, and endomyocardial biopsy [1]. Although a positive diagnosis is made by right ventricular endomycoardial biopsy preceded most often by cardiac MRI criteria, some of these tools may not be readily available in all clinical settings. In addition, the diagnostic value of viral serologies is limited because of lack of specificity and difficult interpretation. The diagnosis of acute myocarditis should be suspected whenever a patient presents with evidence of myocardial injury, or heart failure otherwise unexplained by ischemia or other cardiac structural abnormalities.
In our case, the absence of flu like symptoms days before consulting probably explains in part the absence of the initial suspicion of acute (infectious) myocarditis. However, she presented with acute myocardial injury evidenced by a continuous rise in high-sensitivity cardiac troponins, without evidence of coronary stenosis on angiography, suggesting that her elevated troponin was attributable primarily to myocarditis and VT. Interrogation of our patient’s pacemaker did not reveal any explanation for her VT. The next logical step would have been a cardiac MRI, but in the absence of an MRI, myocarditis was the most likely diagnosis to explain her clinical picture especially with the identification of a cardiotropic virus, human para influenza type 3 PCR.
Cases of acute myocarditis related to Human Parainfluenza Virus (HPIV) previously reported in the existing literature have been established based only serology [2-4]. However, as expected its interpretation may be difficult in the clinical setting since there is inadequate specificity. To the best of our knowledge, very few cases of HPIV 3 myocarditis have been reported in literature. Wilks D et al. reported a case of myopericarditis associated with HPIV-3 based on clinical presentation and a throat smear culture [5]. Romero-Gomez et al. [6] demonstrated the presence of HPIV-3 in the cardiac tissue of a 12-year-old patient who presented with acute myocarditis in the context of the 2009 H1N1 epidemic with an unfavorable evolution, which led to a heart transplant. Cardiac biopsy was mandatory for a positive etiologic diagnosis. This case illustrates once again the difficulty of obtaining an etiologic diagnosis of acute myocarditis based solely on peripheral samples.
A positive diagnosis of acute myocarditis is based on histological damage to the heart muscle according to the Dallas criteria [7] complemented by immunohistochemical evidence and PCR examination to distinguish the lymphocyte populations and the evidence of the causal germ. However, myocardial biopsy remains a highly invasive procedure that cannot be performed in all patients or by all teams, which is why the American Heart Association/American College of Cardiology/European Society of Cardiology have defined the cases in which myocardial biopsy is indicated:
- heart failure refractory to standard therapy,
- worsening of the ejection fraction despite optimization of the pharmacological treatment,
- hemodynamically significant arrhythmia,
- heart failure with rash, fever or eosinophilia,
- past history of vascular collagenosis,
- Cardiomyopathy in the presence of known amyloidosis, sarcoidosis or hemochromatosis or in the absence of an identifiable cause (such as a myocardial infarction).
- any unexplained cardiomyopathy [8]
In our patient, besides VT, we had no other indication to proceed to biopsy based on the above criteria especially after a satisfactory evolution on beta-blockers. Indirect diagnostic methods remain of interest in the presence of suggestive clinical and paraclinical signs. These methods allow the detection of viral particles in peripheral blood, throat, urine or stool. Molecular biology techniques are the most widely used (PCR and RT-PCR) [9, 10].
In summary, as we discuss in this case, in the absence of cardiac MRI or endomyocardial biopsy, an indirect diagnosis of acute myocarditis can be made based on the presence of suggested clinical findings (elevated cardiac troponin, VT) and evidence of a cardiotropic pathogenic agent (HPIV-3).
References
- Pollack A, Kontorovich A, Fuster V, et al. Viral myocarditis-diagnosis, treatment options, and current controversies. Nat Rev Cardiol 12 (2015): 670-680.
- Grist NR, Bell EJ. A six year study of coxsackievirus B infections in heart disease. Journal of Hygiene 73 (1974): 165-172.
- Grodzicka-Krolak H, Horbowska-Marzec H, Malkowska E. The search for a viral etiology of myocarditis]. Przeglad Epidemiologiczny 43 (1989): 388-392.
- Novikov IuI, Stulova MA: [Viral myocarditis (the etiologic, clinical, diagnostic and treatment problems)]. Terapevticheskii Arkhiv 57 (1985): 49-56.
- Wilks D, Burns SM. Myopericarditis associated with parainfluenza virus type 3 infection. Eur. J. Clin. Microbiol. Infect. Dis 17 (1998): 363-365.
- Romero-Gomez MP, Guereta L, Pareja-Grande J, et al. Myocarditis caused by human parainfluenza virus in an immunocompetent child initially associated with 2009 influenza (H1N1) virus. J Clin Microbiol 49 (2011): 2072-2073.
- Laurent Andréolettia, Nicolas Lévêque, Camille Boulagnon, et al. Viral causes of human myocarditis. Arch Cardiovasc Dis 102 (2009): 559-568.
- Cooper LT, Baughman KL, Feldman AM, et al. The role of endomyocardial biopsy in the management of cardiovascular disease: a scientific statement from the American Heart Association, the American College of Cardiology, and the European Society of Cardiology endorsed by the Heart Failure Society of America and the Heart Failure Association of the European Society of Cardiology. Eur Heart J 28 (2007): 3076-3093.
- Laurent Andréolettia, Nicolas Lévêque, Camille Boulagnon, et al. Viral causes of human myocarditis. Arch Cardiovasc Dis 102 (2009): 559-568.
- Uwe Kühl, Heinz-Peter Schultheiss. Viral myocarditis, Swiss Med Wkly 144 (2014): w14010.


 Impact Factor: * 5.3
Impact Factor: * 5.3 Acceptance Rate: 75.63%
Acceptance Rate: 75.63%  Time to first decision: 10.4 days
Time to first decision: 10.4 days  Time from article received to acceptance: 2-3 weeks
Time from article received to acceptance: 2-3 weeks 
