Sequential Use of Sarilumab and Baricitinib in Severe COVID-19 Pneumonia: A Case Report
Gagliardini Roberta*, Sacchi Alessandra, Campioni Paolo, Cicalini Stefania, Grassi Germana, Ottou Sandrine, Concetta Castilletti, Agrati Chiara, Antinori Andrea
National Institute for Infectious Diseases Lazzaro Spallanzani IRCCS, Roma, Italy
*Corresponding Author: Dr. Gagliardini Roberta, UOC Immunodeficienze Virali, INMI Lazzaro Spallanzani, IRCCS, via Portuense 292 - 00149 Rome, Italy
Received: 04 September 2020; Accepted: 12 November 2020; Published: 07 December 2020
Article Information
Citation: Gagliardini Roberta, Sacchi Alessandra, Campioni Paolo, Cicalini Stefania, Grassi Germana, Ottou Sandrine, Concetta Castilletti, Agrati Chiara, Antinori Andrea. Sequential Use of Sarilumab and Baricitinib in Severe COVID-19 Pneumonia: A Case Report. Archives of Clinical and Medical Case Reports 4 (2020): 1211-1217.
View / Download Pdf Share at FacebookAbstract
Background: Severe COVID-19 associated pneumonia patients may exhibit features of systemic hyper-inflammation. Both anti-IL-6 and anti-JAK drugs are curently under investigation for the hyperinflammatory syndrome of COVID-19 disease. Here we report a clinical case with a complete panel of cytokine levels and immunological profiling of T cell, plasmacytoid and myeloid dendritic cells.
Case Presentation: An adult patient with severe COVID-19 pneumonia and documented hyper-inflammation has been treated with antivirals and off-label sarilumab intravenously, with poor response. Subsequently, he was treated with off-label oral baricitinib for 14 days, with clinical, radiological and laboratoristic response, measured also with IL1b, IL-6, IL-8 and TNF-a levels.
Conclusions: Baricitinib was well tolerated and was able to reduce the inflammatory mediators, confirming its role in diminishing the excessive inflammatory response. This case is the first presented with an extensive characterization and shows a possible use of baricitinib as rescue therapy, after anti-IL6 treatment, for COVID-19.
Keywords
<p>Case report; Covid-19; Sars-cov2; Anti-IL6; anti-JAK; Cytokine storm</p>
Article Details
Abbrevations:
COVID-19- Coronavirus Disease 2019; ARDS- Acute Respiratory Distress Syndrome; IL- Interleukin; TNF-α- Tumor Necrosis Factor-α; IL-6R- IL-6 Receptor; CRP- C Reactive Protein; JAK- Janus Kinase; CT- Computed tomography; GGO- Ground-Glass Opacity; Iv- Intravenously; Bid- Bis in Die; LDH- Lactate Dehydrogenase; CPAP- Continuous Positive Airway Pressure; pDC- Plasmacitoid Dendritic Cells; mDC- Myeloid DC; PCR- Polimerase Chain Reaction
1. Introduction
The pandemic expansion of coronavirus disease 2019 (COVID-19) presents an extraordinary challenge to identify possible effective drugs for treatment. COVID-19 infection results in a complex disease and COVID-19 associated pneumonia may provoke respiratory failure from acute respiratory distress syndrome (ARDS) and systemic hyperinflammation with cytokine storm syndrome, probably triggered by Sars-Cov-2 itself [1]. In fact, high concentrations of cytokines were recorded in plasma of critically ill patients infected, especially IL (interleukin)-6, IL-2, IL-7, IL-10, granulocyte-colony stimulating factor, interferon-γ-inducible protein, monocyte chemoattractant protein-1, Macrophage Inflammatory Proteins 1A and Tumor Necrosis Factor-α (TNF-α), and it has been hypothesized that the cytokine storm could be associated with disease severity [2]. Consequently, possible treatment strategies should be aimed not only to eliminate the virus but also to block the hyperinflammatory syndrome [3].
Tocilizumab and sarilumab, humanized monoclonal antibodies directed against IL-6 receptor (IL-6R), block IL-6, which dysregulates the local inflammatory responses, inhibiting host innate defences against respiratory infections and leading to an exaggerated inflammatory cascades and severe tissue damage in SARS-cov-2 patients. They are both approved for use in rheumatoid arthritis, with tocilizumab also approved for cytokine release syndrome (induced by Chimeric Antigen Receptor T cell therapies). Cohort studies and press-release of randomized clinical trials showed interesting results in patients with COVID-19 pneumonia with both these drugs, with reduction in C reactive protein (CRP) levels and in mortality, but complete results are still pending [4-7]. Janus Kinase (JAK) Inhibitors works by inhibiting the JAK signal transducer and activator of transcription pathway. Among them, baricitinib has a potent anti-inflammatory activity, especially against interferon-associated inflammation and has also a possible antiviral effect, linked to the interference with SARS-CoV-2 receptor-mediated endocytosis in lung alveolar epithelial cells [8].
Hereby we report the first case of an adult patient with severe COVID-19 pneumonia that has been treated with anti-IL-6 (sarilumab) and subsequently with baricitinib, with a complete panel of cytokine levels and immunological profiling of T cell, plasmacytoid and myeloid dendritic cells, with good results.
2. Case Presentation
A 70 years old man with no relevant medical history except for hypertension was admitted to an Emergency Department after 10 days of fever and dyspnoea, and diagnosis of COVID-19 pneumonia was made. Physical examination revealed bilateral rales at lungs auscultation. Computed tomography (CT) scan showed peripheral, bilateral, ground-glass opacity (GGO) and arterial blood gas revealed severe hypoxia with PaO2/FiO2 (partial pressure of arterial oxygen/fraction of inspired oxygen) of 200 mmHg. He received oxygen supplementation with Venturi mask, corticosteroids intravenously (iv), ceftriaxone iv, lopinavir/ritonavir 400/100 bis in die (bid) plus hydrossicloroquine 400 mg bid loading dose and then 200 mg bid. Lab tests reveal systemic hyper-inflammation, with ferritin 930 ng/mL, lactate dehydrogenase (LDH) 285 U/L, CRP 12 mg/dL, d-dimer 6400 ng/mL and fibrinogen 660 mg/dl (Figure 1).
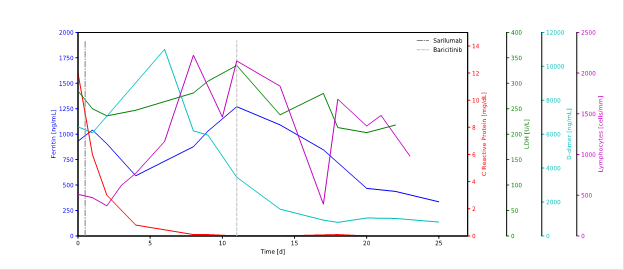
Figure 1: Evolution of inflammatory markers.
Other concomitant infections were excluded. In light of the severe respiratory failure and the high level of inflammatory markers, after 6 days from the beginning of antiviral therapy, one administration of intravenously sarilumab 400 mg off-label was administered. The day after, for a worsening of respiratory distress, respiratory support with non-invasive ventilation (continuous positive airway pressure, CPAP) was applicated.
The subsequent CT scan after 1 week showed an increase of pathological pattern with GGO and reticular and interlobular septal thickening (crazy paving) and micro-embolism was detected in pulmonary arteries proximal to the extensive ground-glass opacifications. CRP decreased to value below 1 mg/dl in 4 days, as expected after the blockage of IL-6, that is responsible of the induction of acute phase proteins such as CRP. A part for this anticipated exception, the other inflammatory markers remained elevated: ferritin 1270 ng/mL, LDH 280 U/l, d-dimer 3460 ng/mL and fibrinogen 220 mg/dl (Figure 1). Moreover, a strong increase in inflammatory cytokines was observed after sarilumab treatment reaching very high levels (Figure 2 Panel A-D). Flow cytometric analysis showed a reduction of plasmacitoid dendritic cells (pDC) after Sarilumab treatment while myeloid dendritic cells (mDC) were quite absent in the peripheral blood (Figure 2 G). A low expression of maturation markers (CD86 and CD80) was also found (Figure 2 H). T cells did not show any significant perturbation with the exception of a slight increase in CD4 effector T cells (Figure 2 E-F).
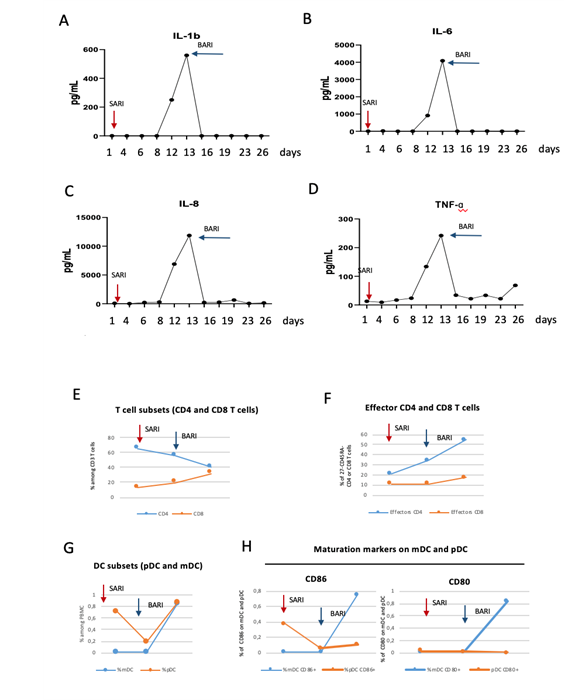
Figure 2: A-D: The levels of IL1b (A), IL-6 (B), IL-8 (C) and TNF-a (D) were quantified by using an automated ELISA assay (ELLA microfluidic analyzer, Protein Simple). E-H: Immunological profiling was performed by flow cytometry. The kinetic of the frequency of CD4 and CD8 (E), effector CD4 and CD8 T cells (F), plasmacytoid and myeloid dendritic cells (pDC and mDC, G) and their maturation markers (H) are shown before sarilumab, before baricitinib and after baricitinib.
Because of the persistence of respiratory failure and of the lack of radiological and laboratoristic improvement, off-label anti-JAK therapy with oral baricitinib 4 mg/die was started, 10 days after anti-IL-6R administration, and continued for 14 days with good tolerance and no adverse effects. Four days after anti-JAK was started, he stopped non-invasive ventilation and started oxygen supplementation with Venturi mask, definitely removed after 10 days. Pulmonary CT performed once baricitinib was stopped, revealed reduction of peripheral, bilateral lesions (GGO and crazy paving) and inflammatory markers were in the normal ranges (Figure 1 and 3). Accordingly, the levels of IL1b, IL-6, IL-8 and TNF-a showed a drastic reduction, reaching normal values (Figure 2A). The patient was discharged in good general condition and without oxygen supplementation. No further complications nor infections were observed one month after discharge.
Notwithstanding the severe clinical manifestations, he obtained a rapid clearance of viral shedding and SARS-Cov-2 polimerase chain reaction (PCR) in naso-pharingeal swab resulted negative after 10 days from the beginning of antiviral therapy. The effect of Baricitinib treatment on immune cells was analysed by flow cytometric. Results showed a decrease in CD4 T cells and a parallel increase in CD8 T cells (Figure 2E). Moreover, the frequency of effectors CD4 and CD8 T cells were substantially increased (Figure 2F). Of note a increase of both mDC and pDC was shown after Baricitinib treatment paralleled by an increase in the expression of maturation molecules mainly in mDC (Figure 2G-H), suggesting a possible improvement in their antigen presentation function. Last pulmonary CT, performed one month after discharge, showed only peripheral residual scars without GGO or crazy paving lesions (Figure 3) and the patient was asymptomatic and in good general condition at the follow-up visit.
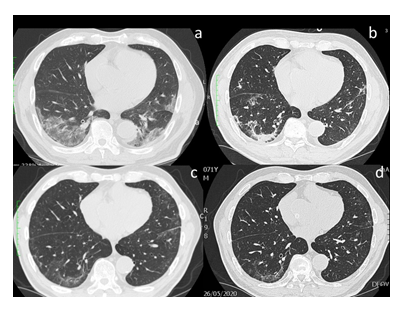
Figure 3: Evolution of lung CT scans: a) bilateral GGO; b) interstitial-reticular involvement and crazy paving after 1 week from sarilumab infusion; c) reduction of interstitial involvement after 2 weeks of baricitinib; d) one month after discharge.
3. Discussion and Conclusions
This case presents a possible use of baricitinib as rescue therapy, after an anti-IL6 treatment, for COVID-19. Both these products are not labeled for the use in Covid-19, so their use is still investigational. Baricitinib has already been explored in a small pilot study of 12 patients, showing improvement in clinical and laboratory parameters and good safety [9], but no data for its use as rescue therapy are available. A recently published paper raised doubts towards the use of baricitinib for COVID-19 patients. In fact, baricitinib cannot be initiated in patients with an absolute neutrophil count less than 1 × 109 cells/L or in patients with an absolute lymphocyte count less than 0.5 × 109 cells/L and various studies reported neutropenia and lymphopenia in patients with severe COVID-19, making this drug not suitable for many patients [10]. Other concerns were the risk of anaemia, the possible reactivation of latent infections or the detrimental impact in viral shedding, but we did not observe any of these complications in this case.
A relevant improvement in pulmonary images has been documented: the first CT scan showed peripheral, bilateral GGO; CT examination after 1 week from the beginning of sarilumab showed an increase of pulmonary lesions with interstitial-reticular involvement and crazy paving; a relevant reduction of pathological CT pictures was visible after 2 weeks from baricitinib. One month after discharge the radiological lung pattern was negative for GGO and crazy paving with periferic residual thin scars. Baricitinib was able to strongly reduce the inflammatory mediators, confirming its role in dampening the excessive inflammatory response. Moreover, we showed here that effective baricitinib treatment increased the frequency of effector T cells and the frequency and maturation molecule on mDC, suggesting a positive effect on the induction of an effective immune response. This is a single case, so further studies are mandatory in order to define if the immunological improvement could be directly driving by baricitinib or, on the other hand, could be the indirect effect of the strong reduction of inflammation. Prospective, full sample-size trials are necessary to demonstrate clinical efficacy, radiological improvement, inflammatory response and safety of anti-JAK, such as baricitinib, in COVID-19 infection.
To conclude, in this case we have illustrated a possible use of baricitinib as rescue therapy, after sarilumab iv therapy, for COVID-19 severe pneumonia.
Declarations Authors' contributions: RG was a major contributor in writing the manuscript; AS analyzed and interpreted the patient data regarding the immunological analyses; PC analyzed and interpreted the patient data regarding radiological images and revised the work; SC contributed to interpretation of data; GG analyzed and interpreted the patient data regarding the immunological analyses; OS contributed to interpretation of data; CC contributed to analysis of data and revised the work; CA analyzed and interpreted the patient data regarding the immunological analyses and revised the work; AA made substantial contributions to the conception of the work and to interpretation of data.
All authors read and approved the final manuscript.
References
- Mehta P, McAuley DF, Brown M, et al. COVID-19: consider cytokine storm syndromes and immunosuppression. Lancet 395 (2020): 1033-1034.
- Huang C, Wang Y, Li X, et al. Clinical features of patients infected with 2019 novel coronavirus in Wuhan, China. Lancet 395 (2020): 497-506.
- Sanders JM, Monogue ML, Jodlowski TZ, et al. Pharmacologic Treatments for Coronavirus Disease 2019 (COVID-19): A Review. Jama (2020).
- Regeneron and Sanofi provide update on U.S. Phase 2/3 adaptive-designed trial of KEVZARA® (sarilumab) in hospitalized COVID-19 patients (2020).
- Tocilizumab improves significantly clinical outcomes of patients with moderate or severe COVID-19 pneumonia (2020).
- Xu X, Han M, Li T, et al. Effective treatment of severe COVID-19 patients with tocilizumab. Proc Natl Acad Sci USA (2020).
- Guaraldi G, Meschiari A, Cozzi-Lepri A. et al. Tocilizumab in patients with severe COVID-19: a retrospective cohort study. The Lancet Rheumatology (2019): 30173-30179.
- Richardson P, Griffin I, Tucker C, et al. Baricitinib as potential treatment for 2019-nCoV acute respiratory disease. Lancet 395 (2020): e30-e31.
- Fabrizio Cantini, Laura Niccoli , Daniela Matarrese , et al. Baricitinib therapy in COVID-19: A pilot study on safety and clinical impact. (2020): 19-21.
- Praveen D, Puvvada RC, Janus kinase inhibitor baricitinib is not an ideal option for management of COVID-19. Int J Antimicrob Agents 55 (2020): 105967.


 Impact Factor: * 5.3
Impact Factor: * 5.3 Acceptance Rate: 75.63%
Acceptance Rate: 75.63%  Time to first decision: 10.4 days
Time to first decision: 10.4 days  Time from article received to acceptance: 2-3 weeks
Time from article received to acceptance: 2-3 weeks 
