Severe Shiga Toxin Producing E. coli Hemolytic Uremic Syndrome in a Child with COVID-19
Mattia Parolin1, Margherita Nosadini2, Davide Meneghesso1, Germana Longo1, Nicola Bertazza Partigiani1, Alessandro Mazza3,4, Elisa Benetti1*
1Pediatric Nephrology, Dialysis and Transplant Unit, Department of Women’s and Children’s Health, University-Hospital, Padua, Italy
2Pediatric Neurology Unit, Department of Women’s and Children’s Health, Padua University Hospital, Padua, Italy
3Pediatric Intensive Care Unit, Department of Women’s and Children’s Health, Padua University Hospital, Padua, Italy
4Pediatric Emergency Unit, Department of Women’s and Children’s Health, Padua University Hospital, Padua, Italy
*Corresponding Author: Elisa Benetti, Pediatric Nephrology, Dialysis and Transplant Unit, Department of Women’s and Children’s Health, Padua University Hospital, Padua, Italy.
Received: 09 June 2022; Accepted: 15 July 2022; Published: 08 August 2022
Article Information
Citation: Mattia Parolin, Margherita Nosadini, Davide Meneghesso, Germana Longo, Nicola Bertazza Partigiani, Alessandro Mazza, Elisa Benetti. Severe Shiga toxin producing E. coli hemolytic uremic syndrome in a child with COVID-19. Archives of Clinical and Medical Case Reports 6 (2022): 577-581.
View / Download Pdf Share at FacebookAbstract
Background: Thrombotic Microangiopathy (TMA) is one of the hallmarks of Shiga toxin-producing E. coli hemolytic uremic syndrome (STEC+HUS), but it is also described in coronavirus-19 disease (COVID-19).
Case: A 5-year-old girl was admitted to our Emergency with severe neurological involvement in STEC+HUS. She experienced encephalopathy, status epilepticus and respiratory distress that required nasotracheal intubation. Parents also reported fever and respiratory symptoms in the previous days. SARS-Cov2 PCR was positive both in nasopharyngeal swab and bronchoalveolar lavage. Based on the severe Central Nervous System (CNS) involvement and the concomitant COVID-19, we managed the patient both for HUS and SARS-Cov2 infection administering dexamethasone, eculizumab and a whole blood adsorber during renal replacement therapy. The patient gradually improved until complete renal and neurological recovery.
Discussion: In HUS, the severity of acute kidney injury is mainly related to the magnitude of TMA. Moreover, the activation of alternative complement pathway, triggered by Shiga toxin, is linked to the severity of both renal and neurological disease. C3 consumption in our patient could be associated with the degree of CNS involvement, although additional features such as electrolyte imbalances and dehydration were lacking. Since COVID-19 can lead to TMA via complement activation, we speculated on the role of SARS-Cov2 in transforming STEC infection into HUS and exacerbating TMA, thus supporting the use of therapies rarely used in STEC+HUS.
Conclusion: The case described could provide further evidence on the similarities of TMA pathophysiology in HUS and COVID-19.
Keywords
<p>Thrombotic Microangiopathy; COVID-19; SARS-Cov2; <em>E. coli</em></p>
Article Details
Abbreviations:
AKI- Acute Kidney Injury; CNS- Central Nervous System; COVID-19- Coronavirus Disease 2019; HUS- Hemolytic Uremic Syndrome; SARS-Cov2- Severe Acute Respiratory Syndrome Coronavirus 2; STEC- Shiga toxin-producing E. coli; STX- Shiga Toxin; TMA- Thrombotic Microangiopathy
1. Introduction
The term Hemolytic Uremic Syndrome (HUS) is currently used to describe the association of Acute Kidney Injury (AKI), non-immune hemolytic anemia and thrombocytopenia. This triad is the consequence of a Thrombotic Microangiopathy (TMA) mainly located in the renal vasculature [1, 2]. Depending upon the triggering factors, HUS can be classified as hereditary or acquired [3]. Shiga toxin-producing E. coli (STEC) accounts for about 90% of the total cases of HUS in the pediatric population [4]. Despite renal and hematological involvement, that are mandatory for the diagnosis, other organs can be involved such as central nervous system (CNS), liver, pancreas, heart and gastrointestinal tract. CNS involvement can represent a life-threatening condition, as well as worsening the outcome, potentially causing serious long-term disability [5]. Although in STEC+HUS TMA is mainly the direct consequence of Shiga Toxin (STX) action on the renal microvascular endothelium, evidence shows that STX may also directly contribute to alternative pathway complement activation [6], in particular in severe cases of STEC+HUS [7]. Similarly, SARS-Cov2 severe infection can lead to TMA, also via complement activation [8]. We describe a severe course of STEC+HUS occurred in a pediatric patient with coronavirus-19 disease (COVID-19).
2. Case Presentation
A previously healthy 5-year-old girl was admitted to our Emergency with encephalopathy, status epilepticus and a 5-day history of fever, bloody diarrhea, mild dehydration, rhinitis and cough. Glasgow coma scale was 4, oxygen saturation was below 80% with severe respiratory distress, coarse rales at auscultation and blood pressure 100/65mmHg (50-90thpercentile).
Considering the impaired consciousness, the severe respiratory distress and the ineffectiveness of first-line anti-seizure medications, an endotracheal tube was placed in order to optimize the therapy and protect the airways. Oxygen saturation raised to 90%. Blood tests revealed microangiopathic hemolytic anemia (Hb 10.5g/dl) with schistocytes in peripheral blood smear, thrombocytopenia (PTLs 44,000mm/c), and stage III anuric AKI with serum creatinine 620umol/L and BUN 45mmol/L, compatible with HUS. Moreover, lactate dehydrogenase was increased (3600U/L) as well as D-dimer (3400ug/L), while serum C3 level was 0.7g/L (normal range 0.9-1.8g/L). Sodium was 126mmol/L without other electrolyte imbalances and C-reactive protein was 110mg/L (normal <6mg/L). Chest x-ray showed mild interstitial disease, while cerebral MRI revealed symmetric cytotoxic edema in the thalami and globi pallidi (figure 1). Stool culture was positive for STEC-O56 STX2 producer, confirming a diagnosis of STEC+HUS. However, SARS-Cov2 screening nasopharyngeal swab was positive and the virus was also found in the bronchoalveolar lavage (BAL) as well as in a rectal swab. Due to the disease severity and the SARS-Cov2 coexistence, the patient was managed both for HUS and COVID-19. Daily PBCs and PLTs transfusions were administered for the first three days after admission. Considering the severe neurological involvement, a dose of 600mg of eculizumab was promptly administered the first day, with partial improvement of the neurologic status, making extubation possible the day after, even if non-invasive ventilation was required for several days. Three total eculizumab doses were administered using the schedule for complement-mediated HUS. Considering the SARS-Cov2 positivity in the BAL and the need for non-invasive ventilation, suggesting the hypothesis that coronavirus could play a role in TMA development, intravenous corticosteroids (dexamethasone 0.15mg/kg/day) were started. At the same time, renal replacement therapy (RRT) with continuous veno-venous hemofiltration was performed both for renal impairment and fluid overload control. Moreover, in the attempt to reduce the cytokine storm and remove STX, two treatments with a whole blood adsorber were performed. Six days after admission, kidney function began to improve with spontaneous diuresis and a decrease in BUN and creatinine until complete normalization after two weeks. After extubation, the consciousness level persisted depressed for one week, and then it gradually improved until complete recovery in three weeks. Together with the progressive recovery of the ability to interact, the patient reported important visual loss and headache. Complete eye review with optic nerve function assessment showed only mild bilateral papilledema. A cerebral MRI with angiography excluded intracranial hypertension and blood vessel defects, and reported complete resolution of the cytotoxic edema in the thalami and globi pallidi. Visual acuity gradually improved in one month, until complete recovery. The genetic evaluation for complement mutations was negative.
3. Discussion
To our knowledge, this is the first report describing the association of severe STEC+HUS and COVID-19. The disease course, in particular the neurological involvement, was very severe in our patient. Impaired consciousness, status epilepticus and strokes are considered severe neurological complications and are reported in only 10% of patients with STEC+HUS [9]. On the other hand, severe AKI is more frequent, since it occurs in over half of pediatric patients with STEC+HUS, requiring RRT in the acute phase of the disease [10]. The severity of renal involvement correlates with TMA magnitude. STX plays a central role in this process, because it can cause direct damage to glomerular endothelial cells, leading to microvascular thrombosis [11]. Moreover, STX can also activate complement alternative pathway, both in renal endothelial cells and fluid phase [7, 12]. Complement contribution appears to be not only kidney restricted; in particular, C3 consumption has been linked to the severity of CNS involvement as well as kidney injury [13]. In our patient, C3 level was decreased, suggesting a remarkable alternative complement pathway activation, probably contributing to the severe disease course. However, the typical thrombotic microangiopathic lesions of HUS that are found in renal vessels are not frequently observed in the brain endothelium [11]. Autoptic evaluations in patients who died from CNS complications in STEC+HUS showed evidence of TMA in less than 35% of cases, while different lesions are reported with a higher incidence, such as intracranial hemorrhage or brain swelling [14]. Surely, the pathophysiology of CNS involvement is less well known than that of the kidney. Some evidence suggests that brain endothelium might react to STX in different ways [11]. Furthermore, the severity of neurological complications appears to be the result of a combination of injuries rather than a unique effect of STX. In particular, several reports [5,10,15] suggest that both frequency and severity of CNS involvement are also due to the degree of dehydration at admission, electrolyte imbalances (mainly sodium) and hypertension. However, in our patient the fluid status and electrolytes were only mildly altered and blood pressure was at the 90thpercentile for sex, age and height. Considering the magnitude of neurological involvement, we promptly administered eculizumab, a C5 inhibitor of complement cascade, in the attempt to reduce complement-related injury. The first successful use of eculizumab in STEC+HUS with severe neurological involvement was reported in a small case series in 2011 [16]. However eculizumab has been shown to be more effective when given early after diagnosis and in patients without rapidly progressing HUS and multiple organ involvement, suggesting a role in preventing complement-mediated effect in CNS rather than in the blockade of early toxic effects of STX [17].
In our patient, the severity of STEC+HUS could be, at least in part, related to the concomitant SARS-Cov2 infection. Indeed, it is interesting how complement activation and related TMA are currently recognized as part of SARS-Cov2 infection, similarly to HUS. Recent acquisitions, both in adults and children with severe COVID-19, suggest how the deposition of the terminal complement complex C5b9 in kidneys and the elevated levels of lactate dehydrogenase, low haptoglobin and schistocytes in the blood smear are similar to complement-mediated HUS [18]. Furthermore, an indirect confirmation of this similitude derives from the report of two cases of complement-mediated HUS relapse triggered by COVID-19 [19,20]. SARS-Cov2 appears to have a sort of renal tropism, probably due to the relatively high expression of angiotensin converting enzyme 2 (ACE2) receptors on podocytes and tubular epithelial cells [21]. ACE2 receptors are also found both in nasal goblet and ciliated epithelial cells as well as oligodendrocytes, representing a possible pathway to CNS infiltration. In addition, SARS-Cov2 can reach the brain through hematogenous dissemination [22]. As in the kidney, COVID-19 causes endothelial injury and subsequent TMA also in the brain, as shown in brain tissue [23]. Finally, high levels of cytokines such as IL-1, IL-6, IL-12, TNFα, INFγ, could also contribute to neurotoxicity [22]. A remarkable secretion of inflammatory cytokines is also reported in STEC+HUS and it contributes both to the development of the disease and to CNS involvement [24]. These data suggest that STEC+HUS and COVID19 may share a common pathophysiology. The patient described in our report presented STEC+HUS with both renal and severe CNS involvement, complicated by SARS-Cov2 infection. Both diseases show a marked tendency to TMA development, also via activation of the alternative complement pathway. In this way, SARS-Cov2 could have exacerbated the magnitude of STEC+HUS-related TMA, justifying the use of Covid-19 specific therapies such as corticosteroids in the attempt to mitigate the virus-related TMA, as well as using eculizumab and whole blood adsorbers directed against both SARS-Cov2 and STEC+HUS. Moreover, STEC infections trigger HUS in only 6-9% of the patients [25] and COVID-19 may also have played a possible role in facilitating the escalation from gastrointestinal infection to HUS, not only in its severity. STEC-HUS is usually managed in a conservative and supportive way, but eculizumab can be considered in case of severe neurological involvement, although data are inconclusive regarding its effectiveness [5, 26]. Furthermore, some reports suggest its use and efficacy in COVID-19 related distress syndrome [27, 28]. Moreover, whole blood adsorbers are rarely employed in STEC+HUS [29] but they can have a rationale in SARS-Cov2 critical patients, considering the hyperinflammatory features of the disease [30]. In conclusion, with the inherent limitation of a case report, our case could represent further indirect evidence of the similitudes of COVID-19 and HUS, mainly concerning the TMA process, also providing a possible indication for timely use of eculizumab and whole blood adsorbers in this association.
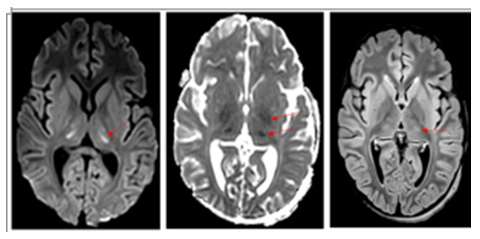
Figure 1: cerebral MRI at onset showed (a) cytotoxic edema in the thalami (DWI), (b) mild cytotoxic edema in the globi pallidi (ADC map) and (c) mild hyperintense lesions in the thalami (FLAIR). Courtesy of Dr. Ignazio D'Errico.
Contributors’ Statement
Mattia Parolin, Margherita Nosadini, Davide Meneghesso, Germana Longo, Nicola Bertazza Partigiani, Alessandro Mazza and Elisa Benetti equally contributed to data collection, literature review, and manuscript drafting and revision. All authors approved the final manuscript as submitted and agree to be accountable for all aspects of the work.
Disclosure Statement
The authors report no disclosures. The manuscript has not been published elsewhere.
References
- Noris M, Remuzzi G. Hemolytic uremic syndrome. J Am Soc Nephrol 16 (2005): 1035-1050.
- Kaplan BS, Meyers KE, Schulman SL. The pathogenesis and treatment of hemolytic uremic syndrome. J Am Soc Nephrol 9 (1998): 1126-1133.
- Aigner C, Schmidt A, Gaggl M, et al. An updated classification of thrombotic microangiopathies and treatment of complement gene variant-mediated thrombotic microangiopathy. Clin Kidney J 12 (2019): 333-337.
- Ardissino G, Salardi S, Colombo E, et al. Epidemiology of haemolytic uremic syndrome in children. Data from the North Italian HUS network. Eur J Pediatr. 2016 175 (2016): 465-473.
- Giordano P, Netti GS, Santangelo L, et al. A pediatric neurologic assessment score may drive the eculizumab-based treatment of Escherichia coli-related hemolytic uremic syndrome with neurological involvement. Pediatr Nephrol 34 (2019): 517-527.
- Morigi, M, Galbusera M, Gastoldi S, et al. Alternative pathway activation of complement by Shiga toxin promotes exuberant C3a formation that triggers microvascular thrombosis. J. Immunol. 187 (2011): 172-180.
- Noris M, Mescia F, Remuzzi G. STEC-HUS, atypical HUS and TTP are all diseases of complement activation. Nat Rev Nephrol 8 (2012): 622-633.
- Diorio C, O McNerney K, Lambert M, et al. Evidence of thrombotic microangiopathy in children with SARS-CoV-2 across the spectrum of clinical presentations. Blood Adv 4 (2020): 6051-6063.
- Brown CC, Garcia X, Bhakta RT, et al. Severe Acute Neurologic Involvement in Children With Hemolytic-Uremic Syndrome. Pediatrics 147 (2021): e2020013631.
- Ylinen E, Salmenlinna S, Halkilati J, et al. Hemolytic uremic syndrome caused by Shiga toxin-producing Escherichia coli in children: incidence, risk factors, and clinical outcome. Pediatr Nephrol 35 (2020): 1749.
- Trachtman H, Austin C, Lewinski M, et al. Renal and neurological involvement in typical Shiga toxin-associated HUS. Nat. Rev. Nephrol 8 (2012): 658-669.
- Orth D, Khan AB, Naim A, et al. Shiga toxin activates complement and binds factor H: evidence for an active role of complement in hemolytic uremic syndrome. J. Immunol 182 (2009): 6394-6400.
- Netti GS, Santangelo L, Paulucci L, et al. Low C3 Serum Levels Predict Severe Forms of STEC-HUS with Neurologic Involvement. Front Med (Lausanne) 7 (2020): 357.
- Gallo EG, Gianantonio CA. Extrarenal involvement in diarrhoea associated haemolytic-uraemic syndrome. Pediatr Nephrol 9 (1995): 117-119.
- Angela Bauer, Loos S, Werhman C, et al. Neurological involvement in children with coli O104:H4-induced hemolytic uremic syndrome. Pediatr Nephrol (2014): 1607-1615.
- Lapeyraque AL, Malina M, Fremeaux-Bacchi V et al. Eculizumab in severe Shiga-toxin-associated HUS. N Engl J Med 364 (2011): 2561-2563.
- Pape L, Hartmann H, Bange FC, et al. Eculizumab in Typical Hemolytic Uremic Syndrome (HUS) With Neurological Involvement. Medicine (Baltimore) 94 (2015): e1000.
- Afzali B, Noris M, Lambrecht BN, et al. The state of complement in COVID-19.Nat Rev Immunol (2021): 1-8.
- Mat O, Ghisdal L, Massart A, et al. Kidney thrombotic microangiopathy after COVID-19 associated with C3 gene mutation. Kidney Int. Rep 6 (2021): 1732-1737.
- Ville S, Le Bot S, Chapelet-Debout S, et al. Atypical HUS relapse triggered by Covid-19. Kidney Int 99 (2020): 267-268.
- Wan Y, Shang J, Graham R, et al. Receptor recognition by the novel coronavirus from Wuhan: an analysis based on decade-long structural studies of SARS coronavirus. J Virol 94 (2020): e00127-20.
- Ghazal A, Gallo Marin B, Kathcur NJ, et al. Neurological Involvement in COVID 19 and Potential Mechanisms: A Review. Neurocritical care 34 (2021): 1062-1071.
- Hernández-Fernández F, Sandoval Valencia H, Barbella Aponte RA, et al. Cerebrovascular disease in patients with COVID-19: neuroimaging, histological and clinical description. Brain 143 (2020): 3089-3103.
- Shimizu M. Pathogenic functions and diagnostic utility of cytokines/chemokines in EHEC-HUS. Pediatr Int (2020): 308-315.
- Gerber A, Karch H, Allerberger F, et al. Clinical course and the role of shiga toxin-producing Escherichia coli infection in the hemolytic-uremic syndrome in pediatric patients, 1997-2000, in Germany and Austria: a prospective study. J Infect Dis 186 (2002): 493.
- Walsh PR, Johnson S. Eculizumab in the treatment of Shiga toxin haemolytic uraemic syndrome. Pediatr Nephrol 34 (2019): 1485.
- Pitts TC. Soliris to Stop Immune-Mediated Death in COVID-19 (SOLID-C19) A Compassionate-Use Study of Terminal Complement Blockade in Critically Ill Patients with COVID-19-Related Adult Respiratory Distress Syndrome. Viruses 13 (2021): 2429.
- Djillali A, Heming N, grimaldi Bensouda L, et al. Eculizumab as an emergency treatment for adult patients with severe COVID-19 in the intensive care unit: A proof-of-concept study . Eclinical Medicine 28 (2020): 100590.
- Bottari G, Lorenzetti G, Severini F, et al. Role of Hemoperfusion With CytoSorb Associated With Continuous Kidney Replacement Therapy on Renal Outcome in Critically III Children With Septic Shock. Front Pediatr 9 (2021): 718049.
- Ruiz Rodriguez JC, Molnar Zsolt, Deliargyris EN, et al. The Use of CytoSorb Therapy in Critically Ill COVID-19 Patients: Review of the Rationale and Current Clinical Experiences. Crit Care Res Pract (2021).


 Impact Factor: * 5.3
Impact Factor: * 5.3 Acceptance Rate: 75.63%
Acceptance Rate: 75.63%  Time to first decision: 10.4 days
Time to first decision: 10.4 days  Time from article received to acceptance: 2-3 weeks
Time from article received to acceptance: 2-3 weeks 
