Use of Multiple Perineural Adjuncts in Quadratus Lumborum Block and Lumbosacral Plexus Block to Provide Anesthesia for Hip Fracture Repair: A Case Report
LL Lee1, A Chan2*, JTK Wong3
1Louis Lam Lee, MBChB, Resident in Department of Anesthesia and Operating Theatre Services, Tuen Mun Hospital (TMH), 23 Tsing Chung Koon Road, Tuen Mun, New Territories, HKSAR
2Anyon Chan (Corresponding author); MBChB; Resident in Department of Anesthesia and Operating Theatre Services, Tuen Mun Hospital (TMH), 23 Tsing Chung Koon Road, Tuen Mun, New Territories, HKSAR
3Jeffery Tak-kin Wong, MBChB, FHKCA, Associate Consultant in Department of Anesthesia and Operating Theatre Services, Tuen Mun Hospital (TMH), 23 Tsing Chung Koon Road, Tuen Mun, New Territories, HKSAR
*Corresponding Author: Anyon Chan, MBChB, Resident in Department of Anesthesia and Operating Theatre Services, Tuen Mun Hospital (TMH), 23 Tsing Chung Koon Road, Tuen Mun, New Territories, HKSAR
Received: 20 April 2022; Accepted: 05 May 2022; Published: 16 May 2022
Article Information
Citation: LL Lee, A Chan, JTK Wong. Use of Multiple Perineural Adjuncts in Quadratus Lumborum Block and Lumbosacral Plexus Block to Provide Anesthesia for Hip Fracture Repair: A Case Report. Archives of Clinical and Medical Case Reports 6 (2022): 374-380.
View / Download Pdf Share at FacebookKeywords
<p>Dexmedetomidine; Dexamethasone; Meperidine; Nerve block; Lumbosacral plexus; Hip fractures; Case report</p>
Article Details
1. Introduction
Hip fracture is common among the elderly with multiple co-morbidities, and early surgery was shown to improve mortality and morbidity [1]. General or neuraxial anesthesia may be risky or even contraindicated in some of these patients, for instance, those with severe cardio-pulmonary diseases or chronic anticoagulation. Regional anesthesia (RA) is an attractive alternative as it offers advantages such as improved analgesia and avoidance of adverse effects from general anesthesia or neuraxial anesthesia [2]. Recently, a combination of Quadratus Lumborum Block (QLB) and lumbar Erector Spinae Plane (ESP) block has been reported as the main anesthetic method for a patient undergoing hemiarthroplasty [3]. With the current rekindled enthusiasm of regional anesthesia in hip fracture surgery, we would like to discuss a case with use of Lumbar Plexus Block (LPB), sacral plexus block (SPB) and QLB as the main anaesthetic method for a patient having gamma nail procedure. Multiple adjuncts including epinephrine, dexamethasone, dexmedetomidine, dextrose, meperidine and sodium bicarbonate were added to supplement the effect of Local Anesthetics (LA). Verbal consent was obtained from the patient’s son for the case to be published. The case report was written according to the CARE (Case Report) guideline [4].
2. Case Presentation
A 93-year-old Chinese lady (body weight 42.8 kg) suffered from a trochanteric fracture of her right femur and was arranged to undergo gamma nail insertion. Her medical history included dementia, hypertension, myocardial infarction with percutaneous coronary intervention done, congestive heart failure with a reduced ejection fraction of 20%, atrial fibrillation on Apixaban and chronic kidney disease. General anesthesia was considered to be detrimental because of the poor cardiac reserve, while neuraxial anesthesia carried a risk of vertebral hematoma with the use of oral anticoagulant and renal impairment. Hence, regional anesthesia was employed as the main anesthetic method. Apixaban was withheld 3 days before the operation. Risks of RA including bleeding, nerve injury and Local Anaesthesic Systemic Toxicity (LAST) were explained to the patient's son as the patient was demented and could not understand the risks. Before commencing RA, arterial line was inserted for close blood pressure monitoring. The patient was then placed in the left lateral decubitus position. The LA mixture was prepared by adding 4 mg dexamethasone, 40 μg dexmedetomidine, 50 mg meperidine, 2 mL 8.4% sodium bicarbonate and 5.6 mL 5% dextrose solution to 15 mL 0.5% levobupivacaine and 15 mL 2% lignocaine with 1:200000 epinephrine, resulting in a total of 40 mL clear solution. LPB was first performed with the “Shamrock Method” [5], and a curved probe (Fujifilm Sonosite Edge; 2-5 MHz) was placed transversely on the lower flank to identify the lumbar spine. A 10 cm Pajunk Sonoplex® needle was inserted in an in-plane manner and 20 mL of the mixture was deposited in the lumbar paravertebral space which was confined by the neuroforamen medially, psoas major anteriorly and erector spinae posteriorly (Figure 1). SPB was then performed with the parasacral approach [6], and 10 mL was injected beneath the piriformis muscle in an out-of-plane fashion (Figure 2). Finally, QL1 block was performed with a linear probe (6-15 MHz) placed laterally above the iliac crest, and 10 mL was injected on the transversalis fascia plane between the transversus abdominis and the quadratus lumborum muscles (Figure 3). Total block time was 25 minutes, and time of block onset was 5 minutes, as demonstrated by pain-free passive movement of the operated hip. Twenty five μg of intravenous fentanyl was given prophylactically prior to the start of the operation. The patient was hemodynamically stable and did not complain of pain throughout the surgery and in the Post-Anesthetic Care Unit (PACU). She was prescribed regular oral paracetamol and tramadol for postoperative analgesia. Upon follow-up 24 hours after RA, the patient reported mild pain at rest and upon movement according to verbal rating scale. Even though Apixiban was resumed, there was no swelling or bruising at the injection sites suggesting hematoma formation. She was able to flex her hip up to 45 degrees and walk with a frame with assistance.
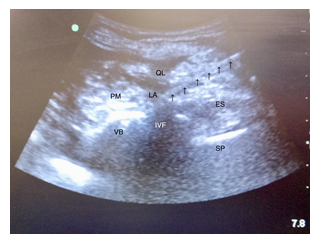
Figure 1: The sonographic image of lumbar plexus block. ES, erector spinae; IVF, intervertebral foramen; LA, local anesthetics; PM, psoas major; QL, quadratus lumborum; SP, spinous process; VB, vertebral body; arrows pointing to the needle.
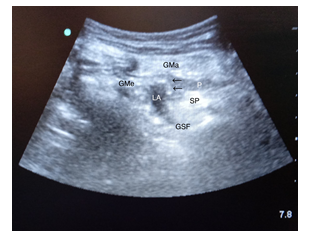
Figure 2: The sonographic image of sacral plexus block. GMa, gluteus maximus; Gme, gluteus medius; GSF, greater sciatic foramen; LA, local anesthetics; P, piriformis; SP, sacral plexus; arrows pointing to the needle.
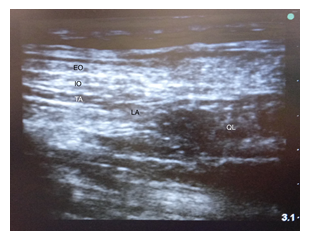
Figure 3: The sonographic image of quadratus lumborum block. EO, external oblique; IO, internal oblique; LA, local anesthetics; TA, transversus abdominis; QL, quadratus lumborum.
3. Discussion
Patients suffering from hip fractures are commonly elderly with multiple comorbidities. Although regional block seems to be the best option for hip fracture surgery given its minimal physiological perturbation, they are seldom the only mode of anesthesia (1.4% in a systemic review from Whiting) [7]. There are several challenges that prevent widespread use of regional block as the sole anesthetic method. The hip joint is innervated by the lumbar plexus (L2-L4) and the sacral plexus (L4-S1) [8], while the superior aspect of the skin incision involves the subcostal (T12) and iliohypogastric (L1) nerves [9]. With LPB and SPB being deep blocks, they may be associated with severe complications like psoas hematoma [10]. However with the advent of high-resolution ultrasound machine, LPB can be accomplished by depositing LA posterior to the psoas muscle instead of in the psoas muscle as proposed by Chayen [11], which potentially lessens the risk of psoas hematoma. Another problem of performing hip fracture surgery under regional block alone is the delayed block onset. A case series by Petchara revealed that the onset time for combined lumbosacral plexus block was around 20 to 30 minutes, which occasionally required additional LA infiltration at the incision site [12]. In our case, the onset time was 5 minutes which was comparable to spinal anesthesia [13]. Sodium bicarbonate was shown to hasten the onset of both sensory and motor block by 2 minutes when ropivacaine was used for supraclavicular Brachial Plexus Block (BPB), which was explained by increasing the unionised fraction of LA [14]. Other than the opioid receptor mediated systemic effect, meperidine also independently blocks sensory and motor nerve conduction [15]. Perineural meperidine was demonstrated by Oztürk to quicken the onset of motor block and improve the motor block quality of lidocaine in axillary BPB [16]. While the analgesic mechanisms of dextrose are manifold [17], a randomised controlled study by Lim suggested that use of 5% dextrose instead of normal saline shortened the onset time of analgesia in supraclavicular BPB [18]. Postoperative analgesia is also of paramount importance in patient undergoing hip fracture repair, as optimal pain control allows early mobilisation which reduces delirium [19] and length of stay [20]. Dexmedetomidine is a unique adjunct that can both speed up block onset and prolong block duration [21], while dexamethasone is also another promising candidate. A systematic review by Sehmbi showed that perineural dexmedetomidine and dexamethasone extended the analgesic duration of supraclavicular block by 294 and 258 minutes respectively [22], while a randomised control trial by Zhang demonstrated a further lengthened analgesic duration when both perineural dexmedetomidine and dexamethasone were used instead of using either one of them [23]. However, perineural dexmedetomidine can cause sedation, bradycardia and hypotension. A dose of 50-60 μg should be adopted in order to strike a balance between the risks and benefits [21]. One may also argue that protracted motor block can delay postoperative mobilization and rehabilitation, but this did not happen in our case. Dexamethasone and dexmedetomidine exhibit differential prolongation of analgesia over motor block (518 minutes vs 294 minutes for dexamethasone, 318 minutes vs 258 minutes for dexmedetomidine) [22], which explains why our patient experienced long-lasting analgesic effect while still being able to actively mobilize. Other problems like incompatibility and neurotoxicity should also be looked out for. To date, this is the only case report that demonstrates the use of 6 perineural adjuncts in combined QLB, LPB and SPB is feasible and can bring about favorable clinical outcomes. Information garnered from postoperative follow-up also gave an insight into how perineural adjuncts may affect the course of recovery. The generalizability of this case report is limited by the fact that only one patient was included, and there was no control case to compare the onset and duration of regional block without using any adjuncts. Optimal doses of the perineural adjuncts are yet to be defined, requiring additional research. Last but not least, the patient in this case report had dementia, which limited the clinical assessment of the effect of the regional block.
4. Conclusion
Use of multiple perineural adjuncts including dexamethasone, dexmedetomidine, dextrose, epinephrine, meperidine and sodium bicarbonate in combined QLB, LPB and SPB was associated with fast onset time, adequate intraoperative anesthesia and satisfactory post-operative analgesia for patients undergoing hip fracture repair, with no major complication noted in our case.
References
- Simunovic N, Devereaux PJ, Sprague S, et al. Effect of early surgery after hip fracture on mortality and complications: systematic review and meta-analysis. CMAJ 182 (2010): 1609-1616.
- Bugada D, Bellini V, Lorini LF, et al. Update on Selective Regional Analgesia for Hip Surgery Patients. Anesthesiol Clin 36 (2018): 403-415.
- Tulgar S, Ermis MN, Ozer Z. Combination of lumbar erector spinae plane block and transmuscular quadratus lumborum block for surgical anaesthesia in hemiarthroplasty for femoral neck fracture. Indian J Anaesth 62 (2018): 802-805.
- Riley DS, Barber MS, Kienle GS, et al. CARE guidelines for case reports: explanation and elaboration document. J Clin Epidemiol 89 (2017): 218-235.
- Sauter AR, Ullensvang K, Niemi G, et al. The Shamrock lumbar plexus block: A dose-finding study. Eur J Anaesthesiol 32 (2015): 764-770.
- Ben-Ari AY, Joshi R, Uskova A, et al. Ultrasound localization of the sacral plexus using a parasacral approach. Anesth Analg 108 (2009): 1977-1980.
- Whiting PS, Molina CS, Greenberg SE, et al. Regional anaesthesia for hip fracture surgery is associated with significantly more peri-operative complications compared with general anaesthesia. Int Orthop 39 (2015): 1321-1327.
- Tomlinson J, Ondruschka B, Prietzel T, et al. A systematic review and meta-analysis of the hip capsule innervation and its clinical implications. Sci Rep 11 (2021): 5299.
- Nielsen TD, Moriggl B, Barckman J, et al. Cutaneous anaesthesia of hip surgery incisions with iliohypogastric and subcostal nerve blockade: A randomised trial. Acta Anaesthesiol Scand 63 (2019): 101-110.
- Dauri M, Faria S, Celidonio L, et al. Retroperitoneal haematoma in a patient with continuous psoas compartment block and enoxaparin administration for total knee replacement. Br J Anaesth 103 (2009): 309-310.
- Chayen D, Nathan H, Chayen M. The psoas compartment block. Anesthesiology 45 (1976): 95-99.
- Petchara S, Paphon S, Vanlapa A, et al. Combined Lumbar-Sacral Plexus Block in High Surgical Risk Geriatric Patients undergoing Early Hip Fracture Surgery. Malays Orthop J 9 (2015): 28-34.
- Danelli G, Baciarello M, Di Cianni S, et al. Effects of baricity of 0.5% or 0.75% levobupivacaine on the onset time of spinal anesthesia: a randomized trial. Can J Anaesth 55 (2008): 50501-50506.
- Kour L, Sharma G, Tantray SH. Evaluation of Addition of Sodium Bicarbonate to Dexamethasone and Ropivacaine in Supraclavicular Brachial Plexus Block for Upper Limb Orthopedic Procedures. Anesth Essays Res 15 (2021): 26-31.
- Oztürk E, Beyazova M, Kaya K, et al. Perineural meperidine blocks nerve conduction in a dose-related manner: a randomized double-blind study. Acta Anaesthesiol Scand 53 (2009): 783-787.
- Saryazdi H, Yazdani A, Sajedi P, et al. Comparative evaluation of adding different opiates (morphine, meperidine, buprenorphine, or fentanyl) to lidocaine in duration and quality of axillary brachial plexus block. Adv Biomed Res 4 (2015):232.
- Lam SKH, Reeves KD, Cheng AL. Transition from Deep Regional Blocks toward Deep Nerve Hydrodissection in the Upper Body and Torso: Method Description and Results from a Retrospective Chart Review of the Analgesic Effect of 5% Dextrose Water as the Primary Hydrodissection Injectate to Enhance Safety. Biomed Res Int 2017 (2017): 7920438.
- Lim HJ, Hasan MS, Chinna K. Faster onset time of supraclavicular brachial plexus block using local anesthetic diluted with dextrose. Braz J Anesthesiol 66 (2016): 341-345.
- Kenyon-Smith T, Nguyen E, Oberai T, et al. Early Mobilization Post-Hip Fracture Surgery. Geriatr Orthop Surg Rehabil 10 (2019): 2151459319826431.
- Craigven SHS, Rehena S, Kenny TXK, et al. Shorter acute hospital length of stay in hip fracture patients after surgery predicted by early surgery and mobilization. Arch Osteoporos 16 (2021): 162.
- Vorobeichik L, Brull R, Abdallah FW. Evidence basis for using perineural dexmedetomidine to enhance the quality of brachial plexus nerve blocks: a systematic review and meta-analysis of randomized controlled trials. Br J Anaesth 118 (2017): 167-181.
- Sehmbi H, Brull R, Ceballos KR, et al. Perineural and intravenous dexamethasone and dexmedetomidine: network meta-analysis of adjunctive effects on supraclavicular brachial plexus block. Anaesthesia 76 (2021): 974-990.
- Zhang P, Liu S, Zhu J, et al. Dexamethasone and dexmedetomidine as adjuvants to local anesthetic mixture in intercostal nerve block for thoracoscopic pneumonectomy: a prospective randomized study. Reg Anesth Pain Med 44 (2019): 10.


 Impact Factor: * 5.3
Impact Factor: * 5.3 Acceptance Rate: 75.63%
Acceptance Rate: 75.63%  Time to first decision: 10.4 days
Time to first decision: 10.4 days  Time from article received to acceptance: 2-3 weeks
Time from article received to acceptance: 2-3 weeks 
