Bilateral Pulmonary Hydatid Cyst in an 11 Year Boy: A Case Report
Dr. Maoulik Kumar, Dr. Lokesh Singh, Dr. Uma debi*, Dr. Shayeri Roy Choudhury, Dr. Vikas Bhatia
Department of Radiodiagnosis and Imaging, Postgraduate Institute of Medical Education and Research, Chandigarh, India
*Corresponding Author: Dr. Uma Debi, Department of Radiodiagnosis and Imaging, Postgraduate Institute of Medical Education and Research, Chandigarh, India
Received: 30 October 2019; Accepted: 20 March 2020; Published: 15 May 2020
Article Information
Citation: Maoulik Kumar, Lokesh Singh, Uma debi, Shayeri Roy Choudhury, Vikas Bhatia. Bilateral Pulmonary Hydatid Cyst in an 11 Year Boy: A Case Report. Archives of Clinical and Medical Case Reports 4 (2020): 435-443.
View / Download Pdf Share at FacebookAbstract
Hydatid disease, a zoonosis, most commonly caused by the parasite Echinococcus granulosus. Hydatid cysts can occur in any organ of the human body, liver followed by lung being the most common location, while in children lung involvement is more common than liver. Cough is usually the most common presenting symptoms. Other common symptoms include shortness of breath, chest pain, fever, hemoptysis or it may be asymptomatic. Pulmonary hydatid cysts grow faster as compared to those in other organs as lung tissue is elastic and compliant. Chest radiograph and Computed tomography(CT) are the most commonly used imaging modality for diagnosis of pulmonary hydatid cyst. Contrast enhanced CT is very valuable for evaluating hydatid especially complicated cyst.
Keywords
<p>Pulmonary hydatid; Pediatric; Echinococcus granulosus; Chest Xray; CT; Water lily sign</p>
Article Details
1. Introduction
Hydatidosis is zoonotic disease and parasitic infestation which can infect human beings especially in endemic areas. Its larval stage cause hydatid cyst most commonly in liver and lung. We report a case of 11 year old male with pulmonary hydatid cyst in both lung parenchyma with hydatid cyst on left side being complicated type.
2. Case History
An eleven year old male child presented to pediatric emergency with shortness of breath, cough and expectoration since one month. There was no history of fever. Chest X-ray done showed a radio-opaque intrapulmonary lesion in right lung silhouetting the right heart border and diaphragm (Figure 1). Another radiolucent lesion was seen in left hemithorax with dependent radio-opaque contents. Chest X-ray was done in supine position as well, which showed layering of the dependent contents in the left lung lesion (Figure 2). Contrast enhanced computed tomogram (CECT) chest and abdomen was done, which showed a cystic lesion in right lung and an air containing lesion in the left lung (Figure 3). The lesion in the left lung was showing dependent hyperdense membranes floating within fluid (Figure 4 and 5).
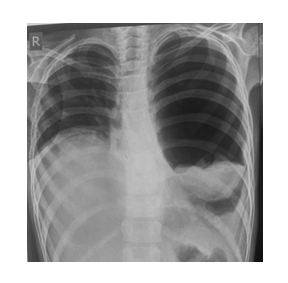
Figure 1: Chest X rayRadio-opaque intrapulmonary lesion in right lung silhouetting the right heart border and diaphragm.
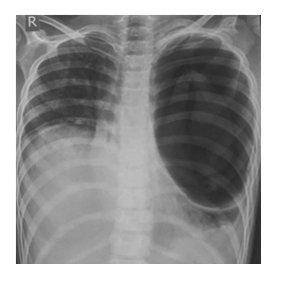
Figure 2: Supine X ray showslayering of the dependent contents in the left lung lesion.
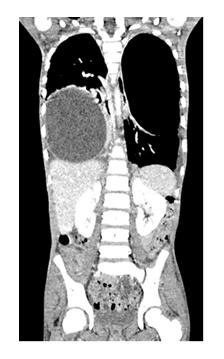
Figure 3: CECT chest and abdomen revealed a cystic lesion in right lung and an air containing lesion in the left lung.
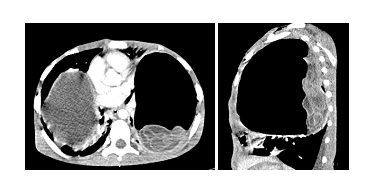
Figure 4 and 5: Left lung showed dependent hyperdense membranes floating within fluid.
3. Diagnosis
Bilateral lung hydatids with complicated left lung hydatid cyst showing “water lily” sign.
4. Discussion
Hydatidosis is zoonotic disease and it infects wild animals, domestic animals and human beings. Causative agent is the parasite Echinococcus granulosus which is the small tapeworm/ cestode with the largest larva. Its larval stage cause disease known as hydatid cyst, also known as liquid tumor. Canine animals especially dog act as definitive host where the worm becomes adult. Sheep, pigs, horses, cattle, humans are intermediate host. Humans can get infected by accidental ingestion of eggs, common source in India being infected vegetables and contaminated water [1-3]. In intermediate host, egg hatches, goes through its larval, encysted forms and develop into metacestode. The fully developed metacestode of E. granulosus is usually unilocular, subspherical shaped and fluid-filled. The cyst consists of an inner germinal or nucleated layer also known as endocyst and it is actual active parasite. It is supported externally by a tough, thick, acellular laminated layer or ectocyst which is, surrounded by host derived fibrous adventitial layer or pericyst which is nothing but inflammatory tissue reaction of host [3-5]. The cyst fluid is crystal clear, colourless, odourless and it is antigenic which if released into the host's bloodstream can cause eosinophilia and anaphylaxis [5, 6]. Hydatid cysts can occur in any organ of the human body, liver followed by lung being the most common location, while in children lung involvement is more common than liver [5-8]. It usually shows male predominance [7-12]. Though some studies have shown female predominance [6, 13].Lung hydatid disease is seen more commonly in young and middle age group [6]. In a series of 233 cases of lung hydatid, 29.6% cases were seen in pediatric age group [10]. Cough is usually the most common presenting symptoms. Other common symptoms include shortness of breath, chest pain, fever, hemoptysis or it may be asymptomatic [7- 9, 13]. Often there is history of contact with dogs [9].Our patient was 11 years old male and presented with cough and shortness of breath. In study of 120 pediatric patient by Cevik M et al, the mean age was 10.15 ± 3.93 years. Cough was presenting symptom in 80.2 % of cases and shortness of breath was seen in 22.1 % of patients while fever was present in 27.6 % of patients. Ruptured hydatid cyst at initial admission was seen in 34.2 % of cases [7].
Solitary cysts are more common than multiple, similarly unilateral localization of cyst is more common than bilateral [8, 10, 11]. It can be bilateral in 20% cases [12]. In our case cysts were bilateral and of large size. Giant hydatid cyst are usually defined by being more than 10 cm in diameter [8, 11, 13].Pulmonary hydatid cysts grow faster as compared to those in other organs as lung tissue is elastic and compliant. Larger cysts are therefore more commonly seen in the pulmonary location as compared to elsewhere [16].The right lung has been described to be more commonly involved than the left side and it has been described that it is more common in right lower lobe, with lower lobe being more commonly involved than upper lobe [8, 10, 11, 17].Peripheral location of cyst is more common than central location [11, 18]. Though simple cyst are usually more common than complicated cyst, the latter form is also a common finding [11, 17]. Pulmonary hydatid cysts can be classified into three types- unilateral solitary unilocular cyst, unilateral multiple cysts and bilateral multiple cysts. Lung hydatid can also be categorized as simple, complicated or ruptured including cystobronchial communication also [19]. Usually patients with simple hydatid cyst may present with non specific symptoms or it may be asymptomatic [20, 21]. Hydatid cyst is defined as complicated when there is rupture of cyst in the bronchus, pleural space with or without secondary infection. Patients may expectorate contents of cyst as salty sputum containing fluid, mucus and grape skin like fragments of membranes [20-22]. Chest radiograph and Computed tomography(CT) are the most commonly used imaging modality for diagnosis of pulmonary hydatid cyst [23]. Chest radiograph being the initial investigation. Commonest radiological sign include solitary well delineated round or oval homogenous opacity. Unruptured hydatid cyst appears as homogenous round to oval mass with smooth outline whereas complicated cysts (infected and /or perforated) may change the radiographic appearance of pulmonary hydatid resulting in incorrect diagnosis and delayed treatment [3, 8, 15, 20, 21].
In our case cyst on right side was simple or uncomplicated and appeared as homogenous radioopacity. CT revealed the lesion to be of cystic attenuation. Contrast enhanced CT is very valuable for evaluating hydatid especially complicated cyst [20, 21]. Hydatid cyst shows high attenuation wall and detached membranes can be seen as linear high attenuation areas in the cyst. Daughter cyst formation though rare appears as round fluid attenuation areas in the periphery of the mother cyst [22]. Hydatid may appear as cavitary lesion in case of cystobronchial communication. It may appear solid and show high attenuation value if infected. Due to solid appearance diagnosis may be difficult with difficulty in differentiating it from abscess or neoplasm [19, 20]. Rupture or perforation is the most common complication and it can be contained rupture or communicating and direct type. In contained rupture, pericyst is intact, rupture involves endocyst. If bronchi are incorporated with in pericyst, contents can escape through it, then it is termed communicating. Rupture of both adventitial and inner layer resulting in direct spillage of cyst content in pleural space, thoracic wall, hollow viscera are described as direct rupture [22]. Hydatid cysts may also be subdivided into closed/unruptured or open/ruptured type. The closed cyst is homogenous, round - ovoid, with smooth outline.When the cyst is expanding and there is communication between the adventitial layer and bronchus, various radiological findings may be seen in open cyst. Presence of pericystic emphysema is important sign seen in pre-ruptured cyst. Air may enter when there is bronchial erosion, during coughing or spontaneously and this presence of air between ectocyst and adventitial layer appears as crescent shaped radiolucency above the homogenous shadow cyst also known as crescent or meniscus sign on radiograph or CT [11, 22, 24, 25].
This peripheral radiolucency on radiograph is not specific for lung hydatid and may also be seen in cavities with fungus ball, hematoma, cavitory neoplasm like squamous cell carcinoma and tumors like bronchial adenoma ,hamartoma [25]. If there is dissection through posterior aspect of membranes, crescent of air is seen on the posterior side of lesion, which is termed inverse crescent sign usually seen on CT. Presence of small foci of intracystic air particularly at the cyst periphery is described as air bubble sign and usually demonstrable on CT [11, 22, 25, 26] . “Signet ring sign” in CT is nothing but bleb of air in the cyst wall and has been reported to be sign of impending cyst rupture [22]. Later on when there is rupture of endocyst, air fluid level may be seen with in endocyst. Air fluid level and presence of air crescent is known as Cumbo’s sign or double arch sign [3, 11, 22, 23]. When there is free connection with the bronchus , there is detachment of cyst wall from adventitia which crumbles, collapses and finally floats on cyst fluid . The presence of floating wrinkled endocyst on fluid has been described as the Camellote's or "waterlily sign" [3, 11, 22, 24, 25] . In our case, lesion on left side was complicated form with chest radiograph demonstrating dependent radiopaque contents which on CT revealed dependent hyperdense membranes floating with in the cyst fluid. The settling of endocyst in lower(most dependant) parts of cyst cavity is “mass within the cavity” sign . Expectoration of cyst contents results in empty and air filled cyst which has been named “dry cyst sign” [11, 22]. Whirl or spin sign is presence of collapsed membranes within the cyst fluid [11, 25]. Collapsed membranes of parasites can be seen on USG, CT and MRI. Contact of ectocyst with pericyst appears as parallel stripes on USG. With collapse of membranes there is disappearance of double line sign and snake or serpent sign may be seen [22, 25].When all the fluid has been expectorated, the residual solid contents comprising of membranes in the most dependent part of cavity is termed “incarcerated membrane sign” [22].
Rupture of pulmonary hydatid in the pleural cavity is uncommon, but it has been described as one of the most serious complication [27]. Rupture in pleural cavity may cause pleural effusion, empyema, pneumothorax,hydropneumothorax or pleural hydatidosis. Rupture of both adventitia and endocyst may predispose to secondary infection which appears as lung abscess. Foci of air in the hydatid or ring enhancement as seen on CT are pointer towards secondary infection and abscess [22]. Bacterial infection is one of the serious complication of rupture. Though presentation of rupture and infection of hydatid cyst may be similar ,but one important point to look for is for fever as patients having hydatid cyst are usually afebrile [6]. On contrast administration ring enhancement of pericyst may be seen on CT, MRI especially if hydatid cyst is infected which has been described as ring enhancement sign [22, 25]. Adjacent lung may shows changes of atelectasis, bronchiectasis . Hydatid cyst may cause invasion of chest wall [22]. Adjacent to the cyst, in addition to ring enhancement dense halo may be seen on CT, MRI which has been named halo sign. It is due to inflammatory infiltrates or atelectasis [22, 25].
Calcification of cyst in lung parenchyma is rare finding (0.7% in one study), so is the formation of daughter cyst in lung hydatid [6, 11, 22, 25]. Ultrasonography may be useful modality particularly in pediatric patients, if hydatid cyst is in peripheral location along chest wall, [12]. USG of liver should be done to detect hepatic hydatid cysts [6]. MRI is rarely used for imaging lung hydatid. On T1WI, cyst content appears as low or intermediate signal intensity and wall demonstrates relatively high signal intensity. On T2WI cyst wall appears as low signal intensity rim. Folded parasitic membranes may be seen. Reactive changes in adjacent lung and also changes of atelectasis may be seen [28]. In a prospective study of 28 pediatric patients of pulmonary hydatid disease, comparing non contrast MRI with fast scanning protocol with contrast CT, Sodhi et al have demonstrated comparable and good accuracy of MRI for detecting lung hydatid with better performance of MRI for demonstrating internal membranes. No requirement of contrast material and no radiation hazard are other advantages especially in pediatric age group [29]. Serologic testing or immunodiagnosis is useful to support the diagnosis. Immunoelectrophoresis or immunoglobulin G enzyme-linked immune-sorbent assay (ELISA) test is considered very sensitive test for diagnosing lung hydatid disease [6, 20, 23]. Eosinophilia may be seen, Latex agglutination test and Casoni test may be positive, however these tests are not reliable [8, 20, 21]. Complicated pulmonary hydatid cyst mimics and can sometimes be misdiagnosed as abscess ,tuberculosis, pneumonia, neoplasm or other infected pulmonary cystic lesion [20, 21, 30]. Sometimes intraparenchymal bronchogenic cyst can be a differential when there are no typical features of hydatid cyst [31, 32]. It is important to differentiate the pulmonary hydatid cyst from congenital cystic lesions of lung like bronchogenic cyst, cystic adenomatoid malformationas, congenital lobar overinflation as the treatment is different [33].
Surgery is the treatment of choice for hydatid cyst with the objective to maintain maximum viable pulmonary parenchyma especially in pediatric age group with complete excision of all viable parasite. Successful treatment of lung hydatid in pediatric cases can be achieved by cystotomy and capitonnage or only cystotomy [34, 35, 36].Capitonnage should not be performed if there is large peripheral cyst [35]. Some authors donot prefer capitonnage [14, 37, 38]. If cysts are present in both lungs median sternotomy is preferred over sequential thoracotomy [14, 39]. Various surgical techniques has been described for pulmonary hydatid cyst and surgery for lung hydatid should be individualized after considering disease severity, complication, size, expected outcome and other relevant factors. Cystotomy, closure of bronchial openings and modified capitonnage provides acceptable results in most patients [37]. Medical management with antihelmintics is useful in complex forms, disseminated form, poor surgical candidates and if there is hydatid fluid spillage preoperatively . Albendazole is the drug choice with therapy often given for 3-6 months [20, 21, 23].
5. Conclusion
Chest symptoms of pulmonary hydatid cyst are non specific and plain radiograph is the initial investigation. Though serology may play supportive role but cross sectional imaging with computed tomography remains the mainstay of diagnosis. Though at times CT diagnosis may be difficult, radiologist should be aware of imaging appearances of complicated or ruptured hydatid cyst.
References
- Bourée P. Hydatidosis: dynamics of transmission. World J Surg Jan 25 (2001): 4-9.
- Romig T, Deplazes P, Jenkins D, et al. Ecology and Life Cycle Patterns of Echinococcus Species. Adv Parasitol 95 (2017): 213-314.
- Kegel RF, Fatemi A. The ruptured pulmonary hydatid cyst. Radiology 76 (1961): 60-64.
- Thompson RC. Biology and Systematics of Echinococcus. Adv Parasitol 95 (2017): 65-109.
- Aletras HA. Hydatid cyst of the lung. Scand J Thorac Cardiovasc Surg 2 (1968): 218-224.
- Jerray M, Benzarti M, Garrouche A, et al. Hydatid disease of the lungs. Study of 386 cases. Am Rev Respir Dis 146 (1992): 185-189.
- Cevik M, Boleken ME, Kurkcuoglu IC, et al. Pulmonary hydatid disease is difficult recognized in children. Pediatr Surg Int 30 (2014): 737-741.
- Erdem CZ, Erdem LO . Radiological characteristics of pulmonary hydatid disease in children: less common radiological Eur J Radiol Feb 45 (2003): 123-128.
- El Khattabi W, Aichane A, Riah A, et al. Imaging of hydatid cyst of the lung. Rev Pneumol Clin 68 (2012): 329-337.
- Xu MQ. Hydatid disease of the lung. Am J Surg 150 (1985): 568-573.
- Akgul Ozmen C, Onat S. Computed Tomography (CT) Findings of Pulmonary Hydatid Cysts in Children and the Factors Related to Cyst Rupture. Med Sci Monit 23 (2017): 3679-3686.
- Garg MK, Sharma M, Gulati A, et al. Imaging in pulmonary hydatid cysts. World J Radiol 8 (2016): 581-587.
- Kuzucu A, Ulutas H, Reha Celik M, et al. Hydatid cysts of the lung: Lesion size in relation to clinical presentation and therapeutic approach. Surg Today 44 (2014): 131-136.
- Celik M, Senol C, Keles M, et al. Surgical treatment of pulmonary hydatid disease in children: report of 122 cases. J Pediatr Surg 35 (2000): 1710-1713.
- Ghoshal AG , Sarkar S, Saha K, et al. Hydatid lung disease: an analysis of five years cumulative data from Kolkata. J Assoc Physicians India 60 (2012): 12-16.
- Usluer O, Ceylan KC, Kaya S, et al. Surgical management of pulmonary hydatid cysts: is size an important prognostic indicator?.Tex Heart Inst J 37 (2010): 429-434.
- Hafsa C , Belguith M, Golli M, et al. Imaging of pulmonary hydatid cyst in children. J Radiol 86 (2005): 405-410.
- Onal O, Demir OF. The relation between the location and the perforation rate of lung hydatid cysts in children. Asian J Surg 41 (2018): 422-426.
- Gouliamos AD, Kalovidouris A, Papailiou J, et al. CT appearance of pulmonary hydatid disease. Chest 100 (1991): 1578-1581.
- Singh U, Kumar S, Gour H, et al. Complicated hydatid cyst and "air bubble" sign: a stepping-stone to correct diagnosis. Am J Case Rep 16 (2015): 20-24.
- Engström ELS, Salih GN, Wiese L. Seronegative, complicated hydatid cyst of the lung: A case report. Respir Med Case Rep 21 (2017): 96-98.
- Turgut AT, Altinok T, Topçu S, et al. Local complications of hydatid disease involving thoracic cavity: imaging findings. Eur J Radiol 70 (2009): 49-56.
- Kilani T, El Hammami S. Pulmonary hydatid and other lung parasitic infections. Curr Opin Pulm Med 8 (2002): 218-223.
- Grünebaum M. Radiological manifestations of lung echinococcosis in children. Pediatr Radiol 3 (1975): 65-69.
- Von Sinner WN. New diagnostic signs in hydatid disease; radiography, ultrasound, CT and MRI correlated to pathology. Eur J Radiol 12 (1991): 150-159.
- Zeyrek D, Savas R, Gulen F, et al. ''Air-bubble'' signs in the CT diagnosis of perforated pulmonary hydatid cyst: three case reports. Minerva Pediatr 60 (2008): 361-364.
- Daghfous H, Zendah I, Kahloul O, et al. Pleural complications of pulmonary hydatid disease.Tunis Med 92 (2014): 6-11.
- Von Sinner WN, Rifai A, Te Strake L, et al. Magnetic resonance imaging of thoracic hydatid disease.Correlation with clinical findings, radiography, ultrasonography, CT and pathology. Acta Radiol 31 (1990): 59-62.
- Sodhi KS, Bhatia A, Samujh R, et al. Prospective Comparison of MRI and Contrast Enhanced MDCT for Evaluation of Pediatric Pulmonary Hydatid Disease: Added Diagnostic Value of MRI. AJR Am J Roentgenol 19 (2019): 1-6.
- Zhang Q , Huang TM, Li BZ, et al. Misdiagnosis of pulmonary hydatid cyst rupture: report of 38 cases 26 (2003): 474-476.
- Malik A, Chandra R, Prasad R, et al. Imaging appearances of atypical hydatid cysts. Indian J Radiol Imaging 26 (2016): 33-39.
- Odev K, Guler I, Altinok T, et al. Cystic and cavitary lung lesions in children: radiologic findings with pathologic correlation. J Clin Imaging Sci 3 (2013): 60.
- Rashid S, Fatimi SH. Atypical pulmonary giant hydatid cyst as bilaterally symmetrical solitary cysts. Asian Cardiovasc Thorac Ann 12 (2004): 257-259.
- Yalçinkaya I, Er M, Ozbay B, et al. Surgical treatment of hydatid cyst of the lung: review of 30 cases. Eur Respir J 13 (1999): 441-444.
- Cangir AK, Sahin E, Enön S, et al. Surgical treatment of pulmonary hydatid cysts in children. J Pediatr Surg 36 (2001): 917-920.
- Do?an R, Yüksel M, Cetin G, et al. Surgical treatment of hydatid cysts of the lung: report on 1055 patients. Thorax 44 (1989): 192-199.
- Nabi MS, Waseem T. Pulmonary hydatid disease: what is the optimal surgical strategy? Int J Surg 8 (2010): 612-616.
- Turna A, Yilmaz MA, Haciibrahimo?lu G, et al. Surgical treatment of pulmonary hydatid cysts: is capitonnage necessary? Ann Thorac Surg 74 (2002): 191-195.
- Salih OK, Topcuo?lu MS, Celik SK, et al. Surgical treatment of hydatid cysts of the lung: analysis of 405 patients. Can J Surg 41 (1998): 131-135.


 Impact Factor: * 5.3
Impact Factor: * 5.3 Acceptance Rate: 75.63%
Acceptance Rate: 75.63%  Time to first decision: 10.4 days
Time to first decision: 10.4 days  Time from article received to acceptance: 2-3 weeks
Time from article received to acceptance: 2-3 weeks 
