Buschke-Löwenstein Tumor: About an Observation and Review of Literature
Article Information
Nada Lahmidani*, Sara Bahja, Ibrahimi Sidi Adil, Mohammed El Abkari
Department of Gastroenterology, University Hospital Hassan II fez, University Sidi Mohammed Ben Abdallah, Fes, Morocco
*Corresponding Author: Lahmidani Nada, Department of Gastroenterology, University Hospital Hassan II fez, University Sidi Mohammed Ben Abdallah, Fes, Morocco
Received: 05 November 2020; Accepted: 30 December 2020; Published: 14 January 2021
Citation: Nada Lahmidani, Sara Bahja, Ibrahimi Sidi Adil, Mohammed El Abkari. Buschke-Löwenstein Tumor: About an Observation and Review of Literature. Archives of Clinical and Medical Case Reports 5 (2021): 100-105.
View / Download Pdf Share at FacebookAbstract
Buschke - Löwenstein tumor is an uncommon disease associated with human papillomavirus infection. It occurs most often in pubescent male subjects with sexual activity. It is located at the level of the external genitalia. The diagnosis is based on the histological study and the treatment is essentially surgical with complete and wide excision in order to avoid recurrence. The prevention of this tumor is based on the treatment of condylomata acuminata as a sexually transmitted disease.
Keywords
Buschke-Löwenstein tumor; Papillomavirus; Condylomata acuminate; Large surgery
Article Details
1. Introduction
The Buschke-Löwenstein tumor (BLT) or giant condyloma acuminata (GCA) is a rare nosological entity described by Buschke and Löwenstein in 1925 [1]. It is an ill-defined epithelial tumor that develops in the external genitalia and in the anorectal region following a sexually transmitted viral infection whose causal agent is the papillomavirus (HPV) often non-oncogenic (HPV 6 and 11) [2]. It is distinguished from condyloma acuminata by its more marked proliferation and deep penetration into the underlying tissues which can then be repressed, and from squamous cell carcinoma by the absence of histological invasion and metastases [1-3]. It is characterized by its degenerative potential and its recurrence after treatment [1-4]. Management is often the subject of controversy: abstention from treatment, surgical excision, electrocoagulation-excision, CO2 laser, immunotherapy. A consensus seems to be emerging for the surgical option.
2. Patients
- Patient information: Mr A.K a 68-year-old patient current heavy smoker with a past history of surgery in 1970 for anal abscess. His history of the disease goes back 20 years before his admission by the appearance of a para anal condylomatous mass associated with proctalgia of moderate intensity and progressive aggravation with defecating and non-defecating bleeding of low abundance with recent weight loss and anorexia.
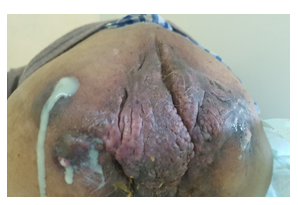
- Clinical findings: Clinical examination on admission finds a conscious patient who is hemodynamically and respiratory stable, dehydrated and malnourished; the lymph node areas are free; the abdominal examination was normal; the examination of the anal margin objectified a greyish giant papillomatous mass para anal in the left side, irregular measuring 15 cm long axis with the presence of 6 external fistulous orifices bringing back pus and stool whose catheterization finds a path to the anal canal. Anuscopy showed a large internal fistulous orifice "figure 1"
- Diagnostic Assessment: Biologically; the blood count objectified anemia at 9.8 g / dl microcytic hypochromic; PNN-predominant 17850 hyperleukocytosis; the CRP is 104 and the ionogram was correct. Serologies of HIV, HBV, HCV, TPHA-VDRL were negative. A thoraco-abdomino-pelvic CT scanner was performed objectifying a left paranal mass, necrotic, enhanced in a heterogeneous manner after contrast, poorly limited measuring 57x40mm.It was associated with an infiltration of neighboring fat with a few collections of hypodense bilateral para-anal abscesses with a wall enhanced after communicating contrast between it for some fistulized to the skin measuring for the largest 70x60mm
- Therapeutic Interventions: Surgical excision of the process was performed with Ciprofloxacin-type antibiotic therapy 200 mg * 2 / day + Metronidazole 500 mg * 3 / day . Showing an appearance of benign fibro epithelial BLT,
- Follow up and outcomes: The course was marked by the installation of severe sepsis and hyponatremia at 121 with neurological disorder, hence his admission to intensive care; patient was intubated ventilated sedated, put on drug based on norepinephrine at 0.3g / kg / min; the patient died 2 days later.
3. Discussion
This observation illustrates the difficulties in the management of these rare tumors with an aggressive local extension potential. BLT is a relatively rare disease whose nosological classification is difficult between benign lesion, lesion with malignant potential or carcinomatous lesion [1]. It was originally described as a giant condyloma due to the lack of metastases but the possibility of progression to an invasive tumor classifies this tumor as a border line tumor [5]. Some authors consider it to be an early form of verrucous carcinoma [6]. The Buschke-Löwenstein tumor is inconstantly associated with human papillomavirus (HPV) infection. Papillomaviruses are viruses without an envelope and the structure of their capsid makes them extremely resistant in the external environment which facilitates their direct transmission by skin or mucous membrane contact, but also their indirect transmission by genital secretions, surfaces, linen. soiled or hands [7, 8]. Papillomaviruses specifically infect multi-layered epithelia such as the skin and genital or oral mucous membranes [9]. The annual incidence of buschke lowenstein tumor is 0.1%. It occurs at any age after puberty and predominates between the 4th and 6th decades [4, 5, 10, 11].
Infection can affect both sexes but is frequently seen in males [5, 12]. Transmission of TBL occurs primarily through the sexual route but also through water, linen, gloves and '' other contaminated materials given that the virus is resistant to environmental conditions.The incriminated risk factors are: poor anorectal hygiene, pregnancy with a risk of 3 times more frequent, multiparity, homosexuality, The multiplicity of partners, immunosuppression, smoking and alcohol [13, 14]. TBL is most often located in the genitals. In men, BLT is localized in 81% to 94% of cases in the penis and in 10% to 17% of cases in the anorectal region. In women, the location is essentially vulvar in 90% of cases, unlike the anorectal location, which remains less frequent [10]. The tumor is always preceded by grayish or pink condylomatous lesions, progressively evolving to take on a papillomatous, irregular appearance [3, 4]. It is distinguished from condyloma acuminata by its size, its development on the surface and in depth, and its potential to push back neighboring tissues [12, 15].
Symptoms are related to the deep infiltration: pain, bleeding, pruritus and purulent discharge secondary to the formation of fistulas complicating bacteremia. The clinical examination should include examination of the external genitalia, perineal and anal region, and inguinal lymph node areas for inflammatory lymphadenopathy secondary to superinfection of the tumor. It should be supplemented by an anoscopy, rectoscopy, pelvic examination, pelvic computed tomography or magnetic resonance imaging in order to assess local invasion of the tumor and to guide further management. The search for other sexually transmitted infections such as HIV, HBV, HCV, TPHA-VDRL, Chlamydia trachomatis and Nesseria gonorrhoeae is systematic. The precise diagnosis of TBL is based on the histological examination of a large surgical biopsy so as not to wrongly conclude to a condyloma or a seborrheic keratosis. This histological examination shows a perfectly limited squamous cell tumor characterized by considerable epithelial hyperplasia sometimes pseudo-epitheliomatous, hyperacanthosis, hyperpapillomatosis and koilocytes which are pathognomonic markers of HPV infection, however their presence is not constant. The basement membrane remains intact, which proves the benignity of the tumor [10, 15, 16].
The Buschke-Lowenstein tumor poses the problem of differential diagnosis. Indeed, certain tumoral lesions such as squamous cell or infectious epitheliomas such as syphilis in its secondary form, verrucous and vegetative tuberculosis, Nicolas Favre's disease, donovanosis or inguinal granuloma, ano-genital amoebiasis, balanitis keratotic and micaceous pseudo-epitheliomatous and Bowen's disease in its condylomatous dyskeratotic form can clinically mimic BLT [12, 14, 17]. The rarity of BLT explains the lack of consensus regarding its treatment. However, surgical excision appears to be the treatment of choice for the majority of authors [3, 11, 18].The surgical treatment of BLT is based on complete and large or even mutilating excision of the lesion in order to reduce the risk of local recurrence, which remains important even in the event of clinically and histologically complete excision. Therefore, incomplete surgical excision indicates surgical revision [19]. In perianal locations, resection with preservation of the sphincter and reconstruction is performed as often as possible, but heavier interventions such as amputation of the rectum or abdominoperineal amputations are sometimes necessary.Patients with extensive lesions with several fistulas and / or superinfection may require a temporary discharge colostomy [3, 12, 18]. Chemotherapy can be used but it remains without real contribution, it is especially indicated preoperatively in order to reduce the tumor volume and reduce the aggressiveness of the surgical act [19].
Radiotherapy is controversial. It is used preoperatively to reduce tumor mass, or as a last resort for non-operable tumors. For some authors, the combination of radiotherapy with neoadjuvant chemotherapy could give remarkable results for degenerated TBL; For others, chemotherapy and radiotherapy should only be given in unresectable or recurrent TBL since their effectiveness has not been fully documented[12, 15, 20] .Topical topicals (podophyline, 5FU), electrocoagulation, cryotherapy, and laser destruction widely used in the treatment of banal condyloma are ineffective in the treatment of BLT [20]. As in other sexually transmitted infections (STIs), partner management is essential. He who must be examined, to look for clinical lesions of HPV or other STIs. Look for other STIs such as HIV, syphilitis, hepatitis B (HBV), and Chlamydia, so microbiological samples should be taken in case of urethritis, vulvovaginitis and associated cervicitis. When treating this tumor, it is necessary to provide for the protection of sexual intercourse [5] .The natural progression can be towards a local invasion, a single or multiple local recurrence or a malignant transformation into invasive squamous cell carcinoma which varies from 5 to 42%, it can be complicated by fistulization in neighboring organs, necrosis, anal stenosis or hemorrhage [15-20].
4. Conclusion
TBL is a rare mucocutaneous disorder caused by condylomatous epithelial proliferation of viral origin, the causative agent of which is papillomavirus (especially types 6 and 11).Although the clinical appearance of the tumor is quasi-specific, the precise diagnosis of TBL is based on histological examination of a large biopsy or the surgical specimen. The treatment must be early, it is essentially surgical requiring a large resection. Its prevention is based on the treatment of condylomas acuminata, the fight against sexually transmitted diseases and vaccination against HPV 6, 11, 16, 18.
Conflicts of Interest
No conflict of interest for authors
Authors Contributions
Collecting DATA and drafting article: Nada Lahmidani , Sara Bahja; Revising the manuscript: Ibrahimi Sidi Adil, Mohammed El Abkari
References
- Kasmaoui El, Lezrak M, Ameur A, et al. Tumeurs de Buschke Loewenstein à localisation génitale, À propos de quatre observations. Ann Urol (Paris) 36 (2002): 211-216.
- Norman L, Sykes JR. Condyloma accuminatum. Intern J Dermatol 34 (1995): 297-230.
- Lévy A, Lebbe C. Prise en charge des tumeurs de BuschkeLöwenstein. Ann Urol (Paris) 40 (2006): 175-178.
- Gillard P, Vanhooteghem O, Richert B, et al. Tumeur de Buschke-Löwenstein. Ann Dermatol Venereol 132 (2005): 98-99.
- Mlle Bennani Hajar. Tumeurs De Buschke-Lowenstein (à propos de 16 cas et revue de littérature) (2018).
- Anadolu R, Boyvat A, Calikoglu E, et al. Buschke-Löwenstein tumour is not a low-grade carcinoma but a giant verruca. Acta Derm Venereol 79 (1999): 253-254.
- Sophie Alain, Sébastien Hantz, François Denis. Papillomavirus: les virus et la physiopathologie de l’infection (2010).
- Précis de biopathologie analyses médicales spécialisées, Biominis (2012).
- Edith Akom, Sylvie Venne. L’infection Au Virus Du Papillome Humain (VPH) (2012).
- Elmejjad A, Dakir M, Tahiri M, et al. Le condylome acuminé géant - tumeur de Buschke Lowenstein (à propos de 3 cas). Prog Urol 13 (2003): 513-517.
- Qarro A, Ait Ali A, Choho A, et al. Tumeur de BuschkeLowenstein à localisation anorectale (À propos de trois cas). Ann Chir 130 (2005): 96-100.
- Rabiil R, Jouall A, Bellabidia B, et al. Condylome acumin scrotal geant: A propos d’un cas. Ann Urol (Paris) 35 (2001): 67-70.
- Noureddine Njoumi, Mohamed Tarchouli, Moulay Brahim Ratbi, et al. La tumeur de Buschke-Lowenstein anorectale : à propos de 16 cas et revue de la littérature (2013).
- Hsu-Cheng Juan, Maw-Chang Sheen, Tsung-Yi Huang, et al. Giant condyloma acuminatum of penis with cancer Transformation. Formosan Journal of Surgery (2011).
- Tytherleigh MG, Birtle AJ, Cohen CE, et al. combined surgery and chemoradiation as a treatment for the Boschke-Lowenstein tumour. Surgeon 4 (2006): 378-383.
- Meli S, Sebastio N, Azzolini N, et al. Buschkelowenstein tumor: report of 2 clinical cases, Acta Biomed Ateneo Parmense (2000).
- Jongen J, Reh M, Bock JU, et al. Perianal precancerous conditions (Bowen disease, paget disease, carcinoma in situ, Buschke-Lowenstein tumor), Kongressbd Dtsch Ges chir Kongr (2001).
- Michael WT, Chao, Peter Gibbs. Squamous Cell Carcinoma Arising in a Giant Condyloma Acuminatum (BuschkeLowenstein Tumour). Asian J Surg 28 (2005): 238-240.
- Mougin C, Dalstein V, Pretet JL, et al. Epidémiologie des infections cervicales à papillomavirus. Presse Med 30 (2001): 1017-1023
- Ali Sbai M, Balti W, Dhahak S, et al. Buschke Lowenstein tumor: unusual bilateral localization. Tunis Med 87 (2009): 627-629.


 Impact Factor: * 3.1
Impact Factor: * 3.1 CiteScore: 2.9
CiteScore: 2.9  Acceptance Rate: 11.01%
Acceptance Rate: 11.01%  Time to first decision: 10.4 days
Time to first decision: 10.4 days  Time from article received to acceptance: 2-3 weeks
Time from article received to acceptance: 2-3 weeks 
