CT Diagnosis of Lupus Enteritis
Lokesh Singh MD1, Aruna Singh MD2*
1Department of Radio diagnosis, PGIMER, Chandigarh, India
2Department of Obstetrics and Gynecology, PGIMER, Chandigarh, India
*Corresponding Author: Aruna Singh MD, Department of Obstetrics and Gynecology, PGIMER, Chandigarh, India
Received: 23 October 2020; Accepted: 09 November 2020; Published: 02 December 2020
Article Information
Citation: Lokesh Singh, Aruna Singh. CT Diagnosis of Lupus Enteritis. Archives of Clinical and Medical Case Reports 4 (2020): 1162-1164.
View / Download Pdf Share at FacebookKeywords
<p>Lupus enteritis; Abdominal pain</p>
Article Details
1. Case Report
A 25 year old female patient was a diagnosed case of systemic lupus erythematosus with haematological, musculoskeletal, oral and dermatological manifestations. Patient was stable and remained asymptomatic for last 5 years. For last 2 months as the steroids were tapered and patient missed few doses, she developed fever, joint pains, oral ulcers, odynophagia and shortness of breath. Patient also complained of abdominal pain which was acute in onset, moderate to severe in intensity, continuous, diffuse involving whole of abdomen and relieved partially on analgesic. There were 2-3 episodes of vomiting followed by loose stools. No h/o hematemesis or melena was seen.
On examination, pulse 132 b/min, BP 140/90 mm Hg, SpO2-97% on room air, RR- 28/min. patient was conscious and alert. No pallor, icterus, cyanosis, clubbing, LAP/edema seen. On local examination-mild tenderness present over right hypochondrium. Bowel sounds were sluggish. No organomegaly/ free fluid. Initially laboratory workup showed anaemia. LFT, RFT, coagulation profile were within normal limits. Serological examination showed elevated ANA, Anti ds DNA, raised hsDNA and raised pro-BNP.
For evaluation of abdominal pain, plain X-ray of abdomen was done which was normal. Ultrasound scan of abdomen showed mild amount of free fluid in abdomen and pelvis. For further evaluation of patient, CT angiography of abdominal vessels followed by CECT of abdomen was done which showed small bowel wall thickening and enhancement giving characteristic ‘target sign’ (formed by enhancing innermost mucosa, middle non enhancing submucosa and outermost enhancing muscularis propria ± serosa) (Figure 1). There was adjacent mesenteric fat stranding with prominent mesenteric vasculature giving comb sign (Figure 1). Mild ascites was also seen. Abdominal aorta and major branches were normal in contrast opacification. Based on these characteristic features, diagnosis of lupus enteritis was kept. Patient was started on parentral high dose steroid therapy following which marked improvement was observed in symptoms.
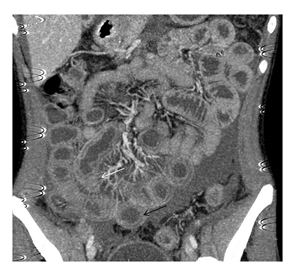
Figure 1: Coronal Post contrast CT image showing dilated and thickened small bowel loops (target sign, black arrow) with mesenteric vessel engorgement (comb sign, white arrow).
Lupus enteritis is a relatively uncommon manifestation of SLE and frequently presents as abdominal pain, diarrhoea and vomiting [1]. It most commonly involves the jejunum and ileum. Principal imaging findings seen on abdominal CT are bowel wall thickening > 3 mm also called as target sign, engorgement of mesenteric vessels also known as comb sign and increased attenuation of mesenteric fat [2]. Treatment for lupus enteritis is high-dose intravenous steroid therapy and complete bowel rest. In few cases immunosuppressants such as azathioprine or cyclophosphamide may be beneficial [3].
Conflicts of Interest
Nil
Funding
Nil
References
- Zizic TM, Shulman LE, Stevens MB. Colonic perforations in systemic lupus erythematosus. Medicine (Baltimore) 54 (1975): 411-426.
- Lee CK, Ahn MS, Lee EY, et al. Acute abdominal pain in systemic lupus erythematosus: focus on lupus enteritis (gastrointestinal vasculitis). Ann Rheum Dis 61 (2002): 547-550.
- Sultan SM, Ioannou Y, Isenberg DA. A review of gastrointestinal manifestations of systemic lupus erythematosus. Rheumatology (Oxford) 38 (1999): 917-932.


 Impact Factor: * 5.3
Impact Factor: * 5.3 Acceptance Rate: 75.63%
Acceptance Rate: 75.63%  Time to first decision: 10.4 days
Time to first decision: 10.4 days  Time from article received to acceptance: 2-3 weeks
Time from article received to acceptance: 2-3 weeks 
