Pleomorphic Adenoma of the Cheek: Case Report and Literature Review
Andrea Avagnina1, Luigi Schiraldi1, Mariana Dalaqua2, Stéphane Yerly3, Miranda Morrison1, Bassel Hallak1*, Salim Bouayed1
1Department of Otorhinolaryngology, Head and Neck Surgery, Hospital of Sion, Sion, Switzerland
2Department of Diagnostic imaging and Interventional Radiology, Hospital of Sion, Sion, Switzerland
3Department of Histocitology, Hospital of Sion, Sion, Switzerland
*Corresponding Author: Dr. Bassel Hallak, Department of Otorhinolaryngology, Head and Neck Surgery, Hospital of Sion, Sion, Switzerland
Received: 31 July 2020; Accepted: 11 August 2020; Published: 14 September 2020
Article Information
Citation: Andrea Avagnina, Luigi Schiraldi, Mariana Dalaqua, Stéphane Yerly, Miranda Morrison, Bassel Hallak, Salim Bouayed. Pleomorphic Adenoma of the Cheek: Case Report and Literature Review. Archives of Clinical and Medical Case Reports 4 (2020): 859-866.
View / Download Pdf Share at FacebookAbstract
A 56-year-old man, with good general health, was addressed by his own physician to our ENT and cervico-facial surgery department with a chief complaint of a mass in the right check. The mass has been progressively growing over the last 15 years, and has become increasingly troublesome in the last 3 months. MRI imaging suggested a vascular malformation. Patient underwent an “en-bloc” surgical excision of the mass, which revealed a pleomorphic adenoma. Pleomorphic adenomas are benin neoplasms composed of mesenchimal and epithelial components. They most frequently occur in the major salivary glands. Ectopic localisations are very rare. Here we report a case of an ectopic pleomorphic adenoma in the subcutaneous layer of the cheek and a literature review.
Keywords
Pleomorphic adenoma articles, Adenoma articles, Cheek articles, Ectopic adenoma articles
Pleomorphic Adenoma articles Pleomorphic Adenoma Research articles Pleomorphic Adenoma review articles Pleomorphic Adenoma PubMed articles Pleomorphic Adenoma PubMed Central articles Pleomorphic Adenoma 2023 articles Pleomorphic Adenoma 2024 articles Pleomorphic Adenoma Scopus articles Pleomorphic Adenoma impact factor journals Pleomorphic Adenoma Scopus journals Pleomorphic Adenoma PubMed journals Pleomorphic Adenoma medical journals Pleomorphic Adenoma free journals Pleomorphic Adenoma best journals Pleomorphic Adenoma top journals Pleomorphic Adenoma free medical journals Pleomorphic Adenoma famous journals Pleomorphic Adenoma Google Scholar indexed journals en-bloc articles en-bloc Research articles en-bloc review articles en-bloc PubMed articles en-bloc PubMed Central articles en-bloc 2023 articles en-bloc 2024 articles en-bloc Scopus articles en-bloc impact factor journals en-bloc Scopus journals en-bloc PubMed journals en-bloc medical journals en-bloc free journals en-bloc best journals en-bloc top journals en-bloc free medical journals en-bloc famous journals en-bloc Google Scholar indexed journals radiologist articles radiologist Research articles radiologist review articles radiologist PubMed articles radiologist PubMed Central articles radiologist 2023 articles radiologist 2024 articles radiologist Scopus articles radiologist impact factor journals radiologist Scopus journals radiologist PubMed journals radiologist medical journals radiologist free journals radiologist best journals radiologist top journals radiologist free medical journals radiologist famous journals radiologist Google Scholar indexed journals tumor articles tumor Research articles tumor review articles tumor PubMed articles tumor PubMed Central articles tumor 2023 articles tumor 2024 articles tumor Scopus articles tumor impact factor journals tumor Scopus journals tumor PubMed journals tumor medical journals tumor free journals tumor best journals tumor top journals tumor free medical journals tumor famous journals tumor Google Scholar indexed journals Heart defect articles Heart defect Research articles Heart defect review articles Heart defect PubMed articles Heart defect PubMed Central articles Heart defect 2023 articles Heart defect 2024 articles Heart defect Scopus articles Heart defect impact factor journals Heart defect Scopus journals Heart defect PubMed journals Heart defect medical journals Heart defect free journals Heart defect best journals Heart defect top journals Heart defect free medical journals Heart defect famous journals Heart defect Google Scholar indexed journals treatment articles treatment Research articles treatment review articles treatment PubMed articles treatment PubMed Central articles treatment 2023 articles treatment 2024 articles treatment Scopus articles treatment impact factor journals treatment Scopus journals treatment PubMed journals treatment medical journals treatment free journals treatment best journals treatment top journals treatment free medical journals treatment famous journals treatment Google Scholar indexed journals laparoscopy articles laparoscopy Research articles laparoscopy review articles laparoscopy PubMed articles laparoscopy PubMed Central articles laparoscopy 2023 articles laparoscopy 2024 articles laparoscopy Scopus articles laparoscopy impact factor journals laparoscopy Scopus journals laparoscopy PubMed journals laparoscopy medical journals laparoscopy free journals laparoscopy best journals laparoscopy top journals laparoscopy free medical journals laparoscopy famous journals laparoscopy Google Scholar indexed journals surgery articles surgery Research articles surgery review articles surgery PubMed articles surgery PubMed Central articles surgery 2023 articles surgery 2024 articles surgery Scopus articles surgery impact factor journals surgery Scopus journals surgery PubMed journals surgery medical journals surgery free journals surgery best journals surgery top journals surgery free medical journals surgery famous journals surgery Google Scholar indexed journals embryological articles embryological Research articles embryological review articles embryological PubMed articles embryological PubMed Central articles embryological 2023 articles embryological 2024 articles embryological Scopus articles embryological impact factor journals embryological Scopus journals embryological PubMed journals embryological medical journals embryological free journals embryological best journals embryological top journals embryological free medical journals embryological famous journals embryological Google Scholar indexed journals Electrocardiography articles Electrocardiography Research articles Electrocardiography review articles Electrocardiography PubMed articles Electrocardiography PubMed Central articles Electrocardiography 2023 articles Electrocardiography 2024 articles Electrocardiography Scopus articles Electrocardiography impact factor journals Electrocardiography Scopus journals Electrocardiography PubMed journals Electrocardiography medical journals Electrocardiography free journals Electrocardiography best journals Electrocardiography top journals Electrocardiography free medical journals Electrocardiography famous journals Electrocardiography Google Scholar indexed journals
Article Details
1. Introduction
In general, salivary gland tumors account for 3% of head and neck neoplasms [1]. In addition, 9 to 23% of salivary gland tumors occur in minor glands. Pleomorphic adenoma (PA) is the most common tumor of the salivary gland, and principally it presents two components, epithelial and mesenchymal components [2]. It is the most common benign neoplasm which is reported in major salivary glands. At times they can also develop in minor salivary glands of the palate [1]. We report a rare case of an ectopic pleomorphic adenoma of the right cheek which was found in the submucosal plane combined with a literature review on the subject.
2 Case Report
A 56-year-old healthy male was addressed to our ENT and cervicofacial department by his own physician following the progressive swelling of his right cheek since 15 years, a swelling that started to be increasingly troublesome in the last 3 months. There was no notion of systemic fever, localized heat or any discharge from the mass. In the patient’s history, there was no history of similar lesions or of usual ENT risk factors. On clinical examination, we found a right jugal swelling and during bimanual palpation we found a mobile, roundish, painless and well circumscribed mass of the right cheek thickness. The size was 3 cm of diameter. The rest of the clinical examination was normal.
The patient presented for the first time for above complaint in our hospital. At first we suspected a benign lesion such as epidermal cyst, a vascular or a lymphatic malformation. To complete the clinical investigation we performed an MRI of the head. The images were assessed by an experienced radiologist in the ENT sphere and they evoked as primary hypothesis a benign vasculaire malformation (hemangioma) (Figure 1, Figure 2, Figure 3).
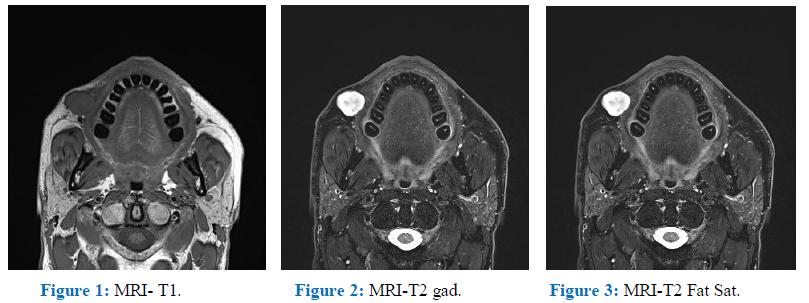
Figure 1: MRI- T1. Figure 2: MRI-T2 gad.Figure 3: MRI-T2 Fat Sat.
The patient underwent surgery under general anesthesia. The incision line was designed on the jugal mucosa, following a vertical line close to the lesion and at least 2 cm away from the labial commissure to avoid damaging the facial artery. The incision was mucosal in order to avoid postoperative scaring on the face. A mass was revealed in the submucosal layer. It was well defined from around normal soft tissues. Complete excision was successfully done and the surgical wound was closed with primary repair, carried out with an absorbable thread. Excised mass was 3 × 2 × 1 cm, firm, multilobulated and of rubbery consistency (Figure 4, Figure 5).
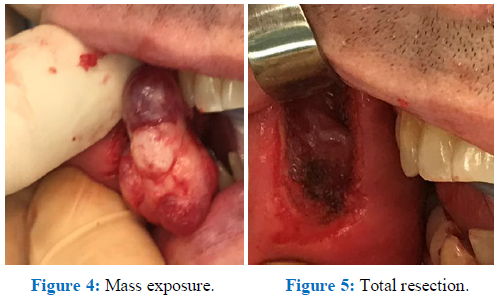
Figure 4: Mass exposure. Figure 5: Total resection.
Histopathological examination revealed a pleomorphic adenoma which presents a roughly polylobulated, biphasic, epithelial/myoepithelial and stromal architecture. The stromal component is abundant and it shows a chrondromyxoid aspect in appearance. (Figure 6, Figure 7).
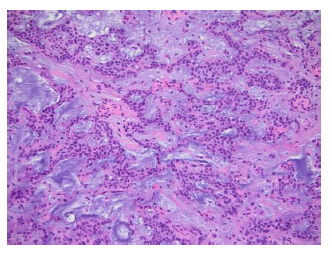
Figure 6: Histopathological examination, cross-sectional inspection of a mass (H&E, ×100).
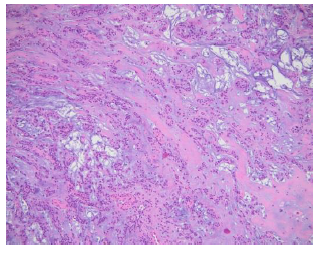
Figure 7: Pleomorphic adenoma which containsepithelial cells and myoepithelial cells with duct-like gland components (H&E, ×200).
3. Materials and Methods
Until March 2020, a systematic search of the literature was performed interrogating PubMed search engine. The following research algorhythm was used pleomorphic adenoma cheek. A prefilled excel database was used to enter the records according to a defined exclusion criteria algorithm. Exclusion criteria applied hierarchically were: (I) not concerning a pleomorphic adenoma; (II) not concerning the cheek; (III) not in English; (IV) review articles; (V) no abstract available; (VI) non-extractable data; (VII) not human. Abstracts were manually screened by AA and LS separately, and subsequently matched for accuracy. Pertinent full-text articles were retrieved and analyzed, and data were extracted on the database. The flow chart of article selection is described following the Preferred Reporting Items for Systematic Reviews and Meta-Analyses (PRISMA) statement [3].
4. Results
The initial database literature search yielded 104 records, including duplicates and non-pertinent articles. After manual screening of the abstracts, 1 record were excluded due to being a duplicate in our search. The remaining 103 articles were further assessed for eligibility. At that stage, n=23 records were not concerning pleomorphic adenoma; n=10 had a different localisation, n=7 were not in English, n=7 were reviews or editorials were excluded from data analysis; n=24 didn’t have an abstract available, n=5 had non-extractable data and n=1 was excluded because it was non human study concerning. A total of 26 [4-28] articles were identified and were included for data extraction. After exclusion, we found 79 patients including 18 females, 11 men and 50 were not available. The mean age was 39,04 ± 18,3 years old years old. The principal symptom was the cheek swelling which was present in 73 patients (92,4%). We found 56 patients (70,8%) who presented an accessory parotid gland (APG) - related tumor and 23 patients (29,2%) who revelead a minor salivary gland (MSG)-related tumor.
In the clinical assessment 5 CT scan, 6 MRI and 9 US were performed. No imaging were performed in 6 patients and for 56 patient this information was not available. Concerning the treatment, 77 (97,46%) patients received a surgical full resection, 1 (1,26%) patient was observed and about 1 patient the treatment was not available. The outcomes were satisfactory in 74 patients (93,67%) with total mass resection in 73 patients who had a surgical resection and 1 patient who was observed. Concerning 5 patients this data is not available. Only 2 patients (2,53%) presented a recurrence as a late complication.
5. Discussion
PA is the most common benign salivary gland neoplasm and it is also known as benign mixed tumor. It accounts for 60%-70% of all parotid neoplasias, 40%-60% of all submandibular neoplasias, and 40%-70% of minor salivary gland neoplasias [29, 30]. The most part of minor salivary glands are present in the oral cavity, spread between hard palate, buccal mucosa, and lips. Other sites are floor of the mouth, inferior surface of the tongue, palatoglossal folds, and tonsillar region. The prevalence is in women between fourth and sixth decade of age , male to female ratio varying from 1:1.4 to 1:1 [31]. The majority of intraoral mixed tumors have a mean size less than 3.0 cm [25]. A retrospective Mexican study showed that in minor salivary gland tumors, 64.2% are benign neoplasms and only 35.8% were malignant [32]. Usually the patient presents a solitary and slow growing firm mass. Small tumors typically form smooth, mobile, firm mass but larger tumors tend to become a multi lobular lump and may attenuate the overlying skin or mucosa [30].
In our case, an ectopic pleomorphic adenoma appeared as a painless, mobile, roundish, and well circumscribed mass of the right cheek thickness, it showed a clinical presentation similar to benign soft tissue tumors. These findings of the case are in accordance with published studies [13, 33]. The differential diagnosis of PA cheek includes buccal abscess, dermoid cyst, sebaceous cyst, neurofibroma, lipoma, mucoepidermoid carcinoma and polymorphous low grade adenocarcinoma [34]. The size, extent of lesions and the bone involvement can be assessed by imaging like CT scan, MRI and ultrasonography which are useful tools during the pre operative phase [35]. Incisional biopsy of PA is contraindicated because can predispose to a recurrence. The preferred diagnostic modality is Fine needle aspiration cytology. PA ectopically exists even in the soft tissue of the neck, lymphonodes, tongue, mandible, hypophysis, mastoid bone, thyroid, parathyroid, subcutaneous layer of the nose, and skin of the external auditory canal [2].
According to Willis and collegues, there are three hypotheses to explain this kind of heterotopias: abnormal differentiation of the local tissues (heteroplasia), abnormal persistence and development of vestigial structures andc dislocation of portion of a deficient rudiment during mass movement and development [36]. It can happen due to metaplasia, neoplastic degeneration of ectopic salivary gland tissue or to the implantation after surgical excision of the salivary gland tumor [37]. The 5% of PA’s cases can present a malignant transformation into carcinoma ex pleomorphic adenoma. Radiotherapy is not indicated as these carcinomas are usually radioresistant. An excellent prognosis was found (95%) after complete and wide excision [2]. PA can relapse in case of scattering, partial and incomplete excision or enucleation, any distant metastasis was discovered. In the literature a recurrence rate of 2-44% has been reported. The gold standard of treatment for PA is wide local surgical resection with good safety margins and follows-up for at least 3-4 years [30]. So an ectopic appearance can cause a diagnostic dilemma for surgeons and a pathological confirmation is crucial. PA is a benign tumor that mainly occurs in the salivary gland but as in this case, given the localization in the facial region an histopathological work-up is crucial inorder to exclude other differential diagnosis [5]. Three histological subtypes were found, myxoid with an high rate of stroma (80%), cellular with myoepithelial cells predominating and mixed which is the classic form.
As already mentioned above, the gold standard treatment is complete surgical resection or eventually a “wait and see” strategy can be adopted. All literature is based on case reports and small size studies which present an high level of heterogeneity in the data reported.
Declaration
We hereby declare no conflict of interest. This article has no funding. All authors approved of the final manuscript as submitted. Patient’s consent was obtained for this publication. This article was approved by the board institution committee of ethics. The availability of data and material was documented.
Contributors
AA contributed to reporting data acquisition and analysis of data. AA and SB wrote the first draft of the manuscript. MM contributed to data acquisition and proof reading. LS contributed to study design and data analysis. BH contributed to the interpretation and data analysis. SB contributed to data acquisition. MD contributed to assess MRI-images and to provide us selected photos. SY contributed to analyse the histology and to provide us selected photos. AA, SB, MM, LS, BH, contributed to the final writing and revising of the manuscript and checked for important intellectual content.
Acknowledgement
Not available for this case
References
- Eveson JW, Cawson RA. Tumours of the minor. (oropharyngeal) salivary glands: a demographic study of 336 cases. J Oral Pathol 14 (1985): 500-509.
- Ogle OE. Salivary Gland Diseases. Dent Clin North Am 64 (2020): 87-104.
- Liberati A, et al. The PRISMA statement for reporting systematic reviews and meta-analyses of studies that evaluate healthcare interventions: explanation and elaboration. BMJ 339 (2009): b2700.
- Periasamy S, Manoharan A, Garg H, et al. Pleomorphic Adenoma of the Cheek: A Case Report. Cureus 11 (2019): e5312.
- Kim YH, Yoon HW, Kim J, et al. Ectopic pleomorphic adenoma on subcutaneous plane of the cheek. Arch Craniofac Surg 20 (2019): 55-57.
- Ma H, et al. Pathology and management of masses in the accessory parotid gland region: 24-year experience at a single institution. J Craniomaxillofac Surg 46 (2018): 183-189.
- Ananthaneni A, Undavalli SB. Juvenile cellular pleomorphic adenoma. BMJ Case Rep (2013).
- Bablani D, et al. Pleomorphic adenoma of the cheek: a case report and review. J Oral Maxillofac Surg 67 (2009): 1539-1542.
- Batrani M, Kaushal M, Sen AK, et al. Pleomorphic adenoma with squamous and appendageal metaplasia mimicking mucoepidermoid carcinoma on cytology. Cytojournal 6 (2008): 5.
- Becelli R, Quarato D, Matarazzo G, et al. Surgical treatment of an extraparotid pleomorphic adenoma of minor salivary glands of the cheek. J Craniofac Surg 20 (2009): 1604-1606.
- Bialek EJ, Jakubowski W, Karpinska G. Role of ultrasonography in diagnosis and differentiation of pleomorphic adenomas: work in progress. Arch Otolaryngol Head Neck Surg 129 (2003): 929-933.
- Cohen MA. Pleomorphic adenoma of the cheek. Int J Oral Maxillofac Surg 15 (1986): 777-779.
- Dalati T, Hussein MR. Juvenile pleomorphic adenoma of the cheek: a case report and review of literature. Diagn Pathol 4 (2009): 32.
- Hamano T, et al. A case of accessory parotid gland tumor. Tokai J Exp Clin Med 29 (2004): 131-133.
- Jayaram R, Patel D, Santhanam V. Benign pleomorphic adenoma of minor salivary gland showing perineural invasion: a rare entity. Br J Oral Maxillofac Surg 53 (2015): 81-82.
- Jung YH, Hah JH, Sung MW, et al. Parotidotomy approach for a midcheek mass: a new surgical strategy. Laryngoscope 120 (2010): 495-499.
- Lee BH. Unilateral agenesis of the parotid gland associated with a pleomorphic adenoma in the ipsilateral buccal space Jpn J Radiol 28 (2010): 224-226.
- Lin DT, Coppit GL, Burkey BB, et al. Tumors of the accessory lobe of the parotid gland: a 10-year experience. Laryngoscope 114 (2004): 1652-1655.
- Panigrahi RG, et al. Juvenile pleomorphic adenoma of masticator space: The first case report. Contemp Clin Dent 4 (2013): 527-530.
- Ramachar SM, Huliyappa HA. Accessory parotid gland tumors. Ann Maxillofac Surg 2 (2012): 90-93.
- Sharma A, Deshmukh S, Shaikh A, et al. Pleomorphic adenoma of the minor salivary gland of the cheek. Singapore Med J 54 (2013): e183-184.
- Sharma N. Pleomorphic adenoma of the buccal salivary gland: magnetic resonance imaging findings with differential diagnoses. J Investig Clin Dent 3 (2012): 228-231.
- Tsegga TM, Britt JD, Ellwanger AR. Pleomorphic adenoma of the accessory parotid gland: case report and reappraisal of intraoral extracapsular dissection for management. J Oral Maxillofac Surg 73 (2015): 564-570.
- Velpula N, Annam SR, Pallepati SR, et al. Pleomorphic Adenoma of Cheek Masquerading as Fibrolipoma - Case Report with Review. J Clin Diagn Res 9 (2015): ZD13-15.
- Verma P, Sachdeva SK, Verma KG, et al. Pleomorphic adenoma of cheek: a rare case report and review of literature. Indian J Dent Res 25 (2014): 122-124.
- Vyas KC, Mathur SP. Pleomorphic salivary adenoma of cheek A case report J Laryngol Otol 98 421-423. (1984):
- Yamamoto H, Fukumoto M, Yamaguchi F, et al. Pleomorphic adenoma of the buccal gland in a child Int J Oral Maxillofac Surg 15 (1986): 474-477.
- Yasumoto M, Sunaba K, Shibuya H, et al. Recurrent pleomorphic adenoma of the head and neck Neuroradiology 41 (1999): 300-304.
- Lopes MA, Kowalski LP, da Cunha Santos G, et al. A clinicopathologic study of 196 intraoral minor salivary gland tumours. J Oral Pathol Med 28 (1999): 264-267.
- Moller K, Kohles N, Esser D. Surgery in Salivary Gland Diseases. Laryngorhinootologie 95 (2016): 709-732.
- van Heerden WF, Raubenheimer EJ. Intraoral salivary gland neoplasms: a retrospective study of seventy cases in an African population. Oral Surg Oral Med Oral Pathol 71 (1991): 579-582.
- Ledesma-Montes C, Garces-Ortiz M. Salivary gland tumours in a Mexican sample A retrospective study. Med Oral 7 (2002): 324-330.
- Rao PK, Shetty SR, Hegde D. Ectopic pleomorphic adenoma. N Am J Med Sci 4 (2012): 190-192.
- Jorge J, et al. Juvenile intraoral pleomorphic adenoma: report of five cases and review of the literature. Int J Oral Maxillofac Surg 31 (2002): 273-275.
- Kaneda T, et al. Imaging tumors of the minor salivary glands. Oral Surg Oral Med Oral Pathol 78 (1994): 385-390.
- Willis RA. Some unusual developmental heterotopias. Br Med J 3 (1968): 267-272.
- Tsukuno M, Nakamura A, Takai S, et al. Subcutaneous pleomorphic adenomas in two different areas of the face Scand. J Plast Reconstr Surg Hand Surg 36 (2002): 109-111.


 Impact Factor: * 5.3
Impact Factor: * 5.3 Acceptance Rate: 75.63%
Acceptance Rate: 75.63%  Time to first decision: 10.4 days
Time to first decision: 10.4 days  Time from article received to acceptance: 2-3 weeks
Time from article received to acceptance: 2-3 weeks 
