A Case Report on Charcot Marie Tooth Disease, and the Role of Vitamin C in this Disease
Madeeha Subhan Waleed1, Waleed Sadiq2*
1Ayub Medical College, Pakistan
2Department of Medicine, Staten Island University Hospital, New York, USA
*Corresponding Author: Dr. Waleed Sadiq, Department of Medicine, Staten Island University Hospital, New York, USA
Received: 03 April 2020; Accepted: 20 April 2020; Published: 18 May 2020
Article Information
Citation: Madeeha Subhan Waleed, Waleed Sadiq. A Case Report on Charcot Marie Tooth Disease, and the Role of Vitamin C in this Disease. Archives of Clinical and Medical Case Reports 4 (2020): 451-455.
View / Download Pdf Share at FacebookAbstract
Charcot Marie tooth is a heredity disease. There is peripheral nerve demyelination, weakness and impaired motor function. No current medications improve neuropathy in subjects with Charcot-Marie-Tooth disease type 1A. We present to you a case of young Asian male with Charcot Marie tooth showing no improvement with three months treatment with ascorbic acid and folate.
Keywords
<p>Charcot Marie Tooth, Polyneuropathies, Pes cavus, Ascorbic acid</p>
Article Details
1. Introduction
Charcot Marie tooth disease or hereditary motor and sensory neuropathy is the most common inherited disease of the peripheral nervous system. It affects approximately 1/2500 individuals [1]. The typical phenotype of an individual suffering from Charcot Marie tooth includes sensory and motor polyneuropathies along with variable sensory manifestations, decreased or absent tendon jerks and skeletal abnormalities such as pes cavus, hammer toes and scoliosis [2-4]. In severe cases the patients become wheelchair bound and respiratory insufficiency occurs, but usually it is a slowly progressive disease compatible with life although the quality of life is always compromised.
2. Case Presentation
A previously healthy 23 year old male presented to the emergency department with one week history of headache and dizziness. The headache was gradual in onset, sharp in character, involving complete head, persisted throughout the day and was relieved with painkillers. There was no associated photophobia, phonophobia, nausea or aura. He also had dizziness which aggravated with movement. It was sudden in onset and occurred along with headache. It was relieved when he lied down and closed his eyes. The patient reported progressive bilateral weakness of lower limbs that later involved bilateral upper extremities as well for 7 months. Nothing aggravated the weakness and it was relieved by rest. He also had speech difficulty but comprehension was fine. He reported multiple falls since three years. He also complained of tremors in all the extremities. Tremors affected the lower left extremity the most. Moreover, he had needle like sensations involving umbilicus, upper left limb and fingers. Regarding past medical history he had undergone laparoscopic appendectomy and septoplasty two years back and recovered fine. His father reported that at times he also had involuntary grinding of teeth and squinting since birth. His vaccination history is up to date and he is a nonalcoholic and a nonsmoker. He is a shopkeeper by profession. His mother is diabetic and his parents had a consanguineous marriage. His siblings are fine. On examination his blood pressure was 120/80 mmHg, pulse was 78 beats per minute. On cardiovascular and respiratory exam heart sounds were normal with normal vesicular breathing and no sign of respiratory compromise was noted. Abdomen was nontender without hepatosplenomegaly. On Nervous system exam; he was alert and oriented to time place and person. His score on MMSE was 30/30. Cranial nerves were grossly intact. Romberg sign was positive. Fine touch and two point discrimination was impaired throughout bilaterally in upper and lower extremity. The gait was broad based gait and feet had hammer toe deformity. Dysdiadochokinesia was negative. Motor power in lower limbs was 3/5 bilaterally and 5/5 in both upper extremities. Reflexes were 2+ in the lower extremities and 3+ in the upper extremities. He has pes cavus (Figure 1).
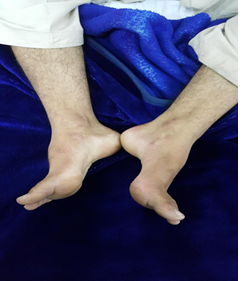
Figure 1: pes cavus.
Appropriate investigations were ordered, CT Brain was normal, nerve conductions studies and electromyography were consistent with CMT. He was started on 1 mg cobalamin, 1 gram folic acid and Vitamin C 2 gram/day for three months. Upon follow up three months later, nerve conduction studies and electromyography were repeated and there was no improvement.
2.1 Laboratory workup at presentation
|
Compound |
Unit |
|
Hemoglobin |
14.8 g/dl |
|
RBC |
3.7 × 10^6 /uL |
|
WBC |
13.7 × 10^3 /uL |
|
Platelets |
156 × 10^3 /uL |
Urine R/E: normal
2.2 Complete metabolic profile
|
Metabolic Profile |
Unit |
|
Sodium |
136 mmol/l |
|
Potassium |
4.4 mmol/l |
|
Chloride |
103 mmol/l |
|
Urea |
36 mg/dl |
|
Creatinine |
0.9 mg/dl |
|
Glucose |
120 mg/dl |
|
ALT |
26 U/l |
|
Alkaline Phosphatase |
407 U/l |
|
Total bilirubin |
0.6 mg/dl |
Nerve Conduction Studies: Hereditary sensory and motor neuropathy.
MRI: Abnormal linear vertical, symmetrical, high T2/PD and low T1 signal area involving the posterior horn of the internal capsule bilaterally. A well-defined, high T1 and T2 signal abnormality measuring approximately 1.5 cm × 1.5 cm × 1.3 cm in right petrous apex , possibly suggestive of cholesterol granuloma. Bilateral maxillary sinusitis.
CPK: normal; Antinuclear antibody: negative
2.3 Blood lipid profile
|
Cholesterol |
126 mg/dl |
|
Triglycerides |
79 g/dl |
3. Discussion
The prevalence of CMT ranges from 10-30/100,000, depending on the region of origin [5, 6]. Symptoms usually appear at infancy or early adulthood and include tremors, unsteady gait and deformity of the feet. The patient may have cramps after exercise. Positive sensory alterations are extremely rare. Foot drop can be seen on physical examination. Previous studies have documented that Charcot Marie tooth has a negative impact on life both psychologically and physically [7]. A study shows Ascorbic acid ameliorates neuropathy in CMT-1A mice [8]. This paper shows treating a mouse model of CMT1A with ascorbic acid thus showing the use of Vitamin C in CMT. European multicenter studies are underway to check the use of high doses of ascorbic acid in people suffering from CMT. A trial conducted in Italy and the United Kingdom of 138 adults receiving 1.5-g/d AA compared with 133 adults receiving placebo for 2 years showed no effect of Ascorbic acid on patients with Charcot Marie tooth [9]. This is in concordance to our patient who received high dose Vitamin C and folate but showed no improvement in nerve conduction. It states that high dosages of Vitamin C improved function and increased the numbers of myelinated peripheral nerve axons in mouse models of Charcot Marie tooth [10]. A small Dutch study of 2-g/d AA and an Australian trial of 30-mg/kg/d AA in children showed no change in nerve conduction velocity in Charcot Marie tooth [11, 12]. Hence vitamin C or folate plays no role in treatment of Charcot Marie tooth. Two hypotheses exist that how vitamin C plays role in Charcot Marie tooth disease. In vitro experiments show culture media are deficient of vitamin C; consequently when exogenous vitamin C is given it replenishes the stores and then exerts the biological effects [13, 14]. The second one state that upon vitamin C transporters, which are saturable, vitamin C can enter cells both in its reduced as well as oxidized form, ascorbic acid and dehydroascorbate, utilizing sodium-dependent transporters, also necessary for the uptake of vitamin C by the Schwann cells [15] or glucose transporters (GLUT) [16].
4. Conclusion
CMT is a heterogeneous disease both clinically and genetically. Clinical and electrophysiological data are insufficient for performing efficient molecular diagnoses of this entity. It is crucial to provide good symptomatic treatment, counseling, effective diagnosis of family members and valid prognosis to decrease morbidity as well as mortality There’s currently no cure for this disease. However treatments can help relieve symptoms, aid mobility and increase quality of life for people with the condition but more studies should be done for finding out the effective treatment for it.
References
- Skre H. Genetic and clinical aspects of Charcot–Marie–Tooth's disease. Clin Genet 6 (1974): 98-118.
- Thomas PK, Marques W Jr, Davis M, et al. The phenotypic manifestations of chromosome 17p11.2 duplication. Brain 120 (1997): 465-478.
- Marques WJ, Freitas MR, Oliveira ASB, et al. 17p duplicated Charcot–Marie–Tooth 1A: characteristics of a new population. J Neurol 252 (2005): 972-979.
- Patzko A, Shy ME. Charcot–Marie–Tooth disease and related genetic neuropathies. Continuum Lifelong Learning Neurol 18 (2012): 39-59.
- Berciano J, Combarros O. Hereditary neuropathies, Current Opinion in Neurology. 16 (2003): 613-622.
- Emery EH. Population frequencies of inherited neuromuscular diseases—a world survey. Neuromuscular Disorders 1 (1991): 19-29.
- Arnold A, Entagardt M, Younger DS. Psychosocial issues that face patients with Charcot–Marie–Tooth disease: the role of genetic counselling. J Genet Couns 14 (2005): 307-318.
- Passage E, Norreel JC, Noack-Fraissignes P, et al. Ascorbic acid treatment corrects the phenotype of a mouse model of Charcot-Marie-Tooth disease. Nat Med 10 (2004): 396-401.
- Pareyson D, Reilly MM, Schenone A, et al. CMT-TRIAAL Group; CMT-TRAUK Group. Ascorbic acid in Charcot-Marie-Tooth disease type 1A (CMT-TRIAAL and CMTTRAUK): a double-blind randomised trial. Lancet Neurol 10 (2011): 320-328.
- Passage E, Norreel JC, Noack-Fraissignes P, et al. Ascorbic acid treatment corrects the phenotype of a mouse model of Charcot-Marie-Tooth disease. Nat Med 10 (2004): 396-401.
- Verhamme C, Haan RJ, Vermeulen M, et al. Oral high dose ascorbic acid treatment for one year in young CMT1A patients: a randomised, double-blind, placebo-controlled phase II trial. BMC Med 7 (2009): 70.
- Burns J, Ouvrier RA, Yiu EM, et al. Ascorbic acid for Charcot-Marie-Tooth disease type 1A in children: a randomised, double-blind, placebo-controlled, safety and efficacy trial. Lancet Neurol 8 (2009): 537-544.
- Smith AR, Visioli F, Hagen TM. Vitamin C matters: increased oxidative stress in cultured human aortic endothelial cells without supplemental ascorbic acid. FASEB Journal 16 (2002): 1102-1104.
- Halliwell B, Whiteman M. Measuring reactive species and oxidative damage in vivo and in cell culture: how should you do it and what do the results mean? British Journal of Pharmacology 142 (2004): 231-255.
- Gess B, Lohmann C, Halfter H, et al. Sodium-dependent vitamin C transporter 2 (SVCT2) is necessary for the uptake of l-ascorbic acid into Schwann cells. Glia 58 (2010): 287-299.
- Michels AJ, Hagen TM, Frei B. A new twist on an old vitamin: human polymorphisms in the gene encoding the sodium-dependent vitamin C transporter 1. American Journal of Clinical Nutrition 92 (2010): 271-272.


 Impact Factor: * 5.3
Impact Factor: * 5.3 Acceptance Rate: 75.63%
Acceptance Rate: 75.63%  Time to first decision: 10.4 days
Time to first decision: 10.4 days  Time from article received to acceptance: 2-3 weeks
Time from article received to acceptance: 2-3 weeks 
