40 Year Follow-Up of Conservatively Treated CAM Impingement of Both Hips- A Case Report
Sandeep Kashyap1, Alexander Schuh2*, Wolfgang Hönle2, Stefan Sesselmann3
1Postgraduate Institute of Medical Education & Research, Chandigarh, India
2Musculoskeletal Center, Neumarkt Hospital, 92318 Neumarkt, Germany
3Institute for Medical Technology, Ostbayerische Technische Hochschule Amberg-Weiden, Hetzenrichter Weg 15, 92637, Weiden, Germany
*Corresponding Author: Prof. Dr. Alexander Schuh, Head of Musculoskeletal Center, Neumarkt Hospital, Teaching Hospital of the University of Erlangen- Nurenberg, Nürnberger Str. 12, 92318 Neumarkt, Germany
Received: 04 September 2019; Accepted: 27 September 2019; Published: 28 November 2019
Article Information
Citation: Sandeep Kashyap, Alexander Schuh, Wolfgang Hönle, Stefan Sesselmann. 40 Year Follow-Up of Conservatively Treated CAM Impingement of Both Hips- A Case Report. Archives of Clinical and Medical Case Reports 3 (2019): 646-650.
View / Download Pdf Share at FacebookAbstract
Femoro-acetabular impingement is a recognized mechanism for the development of early degenerative changes of the hip joint. The symptoms and progression of CAM femoro-acetabular impingement may be attenuated by conservative treatment, but surgical intervention is often necessary. Nowadays there is a trend towards open or arthroscopic operative correction with the aim to remove the cause of impingement at the acetabular rim and at the femoral head neck junction- but complications do occur. Recently conservative measures in FAI have been reported, reserving surgery to symptomatic patients. We present the case of a 40 year follow- up of conservatively treated symptomatic CAM Impingement of both hips.
Keywords
<p>Femoro-acetabular impingement; Arthroscopic; Hips; Acetabular rim; Femoral headneck</p>
Article Details
1. Introduction
Hip pain in young adults can represent a diagnostic challenge. Important features to elicit from the history include developmental dysplasia, trauma or predisposing factors of avascular necrosis. Some individuals have morphological abnormalities in the shape of the femur or the acetabulum. The use of magnetic resonance imaging has helped to improve the diagnosis of soft tissue causes of hip pain, such as labral pathology. Consequently, a host of morphological abnormalities to the femoral neck and acetabulum have been termed “femoro-acetabular impingement” (FAI) [1]. Femoro-acetabular impingement is a recognized mechanism for the development of early degenerative changes of the hip joint. Global or local overcoverage by the acetabulum causes pincer femoro-acetabular impingement, and asphericity of the femoral head-neck junction causes CAM femoro-acetabular impingement. Both lead to a specific pattern of cartilage damage [2]. The aim of operative treatment of femoro-acetabular impingement is removal of the cause of impingement at the acetabular rim and at the femoral headneck junction. Surgical correction can be obtained with open or arthroscopic surgery. The symptoms and progression of CAM femoro-acetabular impingement may be attenuated by conservative treatment, but surgical intervention is often necessary. Several surgical procedures indicated for young patients without severe damage to articular surfaces have been developed to correct cam impingement by removing the osseous abnormality from the femoral head-neck junction in hope of reducing hip pain and restoring normal hip function [3, 4]. Recently, conservative measures in FAI have been reported, reserving surgery to symptomatic patients [5, 6]. We present the case of a 40 year follow- up of conservatively treated CAM Impingement of both hips.
2. Case Report
In 1972 a 25 year old football player presented himself with persisting bilateral groin pain at our private office. There was a limited range of motion of both hips. Extension / Flexion of the right hip was 0/0/130° and 0/0/120° of the left hip. Abduction /Adduction for both hips was 45/0/40°, External Rotation / Internal Rotation of both hips was 40/0/40°. Internal rotation of the flexed hip was painful. Plain radiograph of the pelvis showed a cam deformity of both hips with flattened head–neck junction and early degenerative changes (Figure 1). We recommended to avoid stop and go loads like football playing, jumping and compression loads and prescribed physiotherapy. Within 3 weeks the patient was out of any complaints. The patient stopped playing football, but was sportive performing swimming and cycling. In 1982 the patient presented himself for a x-ray examination of both hips. The patient was pain free. Extension / Flexion of the right hip was 0/0/120° and 0/0/110° of the left hip. Abduction /Adduction for both hips was 40/0/40°, External Rotation / Internal Rotation of both hips was 40/0/30°. Internal rotation of the flexed hip was painful again. Plain radiograph of the pelvis showed a CAM deformity of both hips with flattened head–neck junction and progressive degenerative changes with cystic lesions of the acetabular edge (Figure 2). Till 2011 the patient suffered from recurrent mild groin pain, which increased in October 2011. Physical examination of both hips in January 2012 revealed a limited range of motion of both hips.
Extension / Flexion of the right hip was 0/10/100° and 0/15/100° of the left hip. Abduction /Adduction for both hips was 20/0/20°, External Rotation / Internal Rotation of both hips was 20/0/0°. Internal rotation of the flexed hip was painful. Plain radiograph of the pelvis showed a cam deformity of both hips with a pistol grip deformity, cystic lesion of the left acetabular edge, osteophytes of the femoral head and joint space narrowing (Figure 3).
We prescribed physiotherapy and antiphlogistic drugs. Within 2 weeks the patient was out of complaints. We recommended x- ray examination within the next 5 years. At the latest follow-up there was no need for an operation.
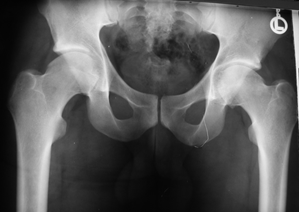
Figure 1: Plain radiograph of the pelvis (1972) at the age of 25 years showing a cam deformity of both hips with beginning degenerative changes.
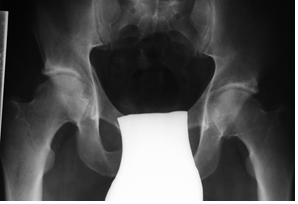
Figure 2: Plain radiograph of the pelvis (1982) at the age of 35 years showing a cam deformity of both hips with flattened head–neck junction, pistol grip deformity, cystic lesion of the acetabular edge.
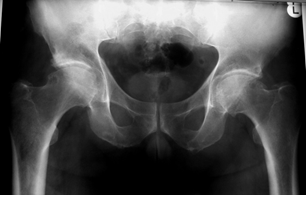
Figure 3: Plain radiograph of the pelvis (2012) at the age of 65 years showing a cam deformity of both hips with a pistol grip deformity, cystic lesion of the left acetabular edge, osteophytes of the femoral head and joint space narrowing.
3. Discussion
Cam femoro-acetabular impingement (FAI), an idiopathic progressive pathological condition of the hip in young and active adults, has been reported to affect 17% of all males and 4% of all females [4]. Usually at the limits of hip motion, the aspherical femoral head is forced against the acetabular edge, causing impingement and pain. Over time, this may lead to a labral tear or detachment and damage to articular cartilage, defects thought to be an underlying cause of hip osteoarthritis [4]. Non operative management of FAI includes modification of activities, avoiding excessive hip movement and regular non-steroidal anti-inflammatory agents can provide symptomatic relief. Discontinuation of sport or recreational activities is helpful; however, this is often unacceptable to young individuals [1]. Surgical dislocation of the hip is an established treatment of FAI and continues to be the gold standard [3]. The technique of safe surgical dislocation developed by Ganz et al. [3] preserves the femoral head blood supply and allows direct visualization of the intra-articular lesion. The technique can be combined with other procedures such as trochanteric advancement, relative femoral neck lengthening, and even femoral neck osteotomy [3, 7].
The results of surgical treatment have been good to excellent in approximately 80% of cases [2, 4]. Complications of the open technique can be intraarticular adhesions between the joint capsule and the resection area on the femoral neck, which cause persistent symptoms such as groin pain in approximately 6% of patients. Articular adhesions have also been observed after arthroscopic surgery for treatment of FAI [2]. Other complications include neurapraxia of the sciatic, pudendal, and lateral femoral cutaneous nerves [8]. Recently Papalia et al. [8] published a meta- analysis criticizing that most studies were level III-IV evidence and included only a small number of participants with limited long-term follow-ups. Papalia was unable to draw any definitive conclusion which operative procedure (open vs. arthroscopic) is most effective because the long-term consequences of residual bony impingement and secondary degeneration usually appear at mid- and long-term assessments. We follow Papalia et al. [8] that any treatment option must be measured by its long- term results. In a retrospective study Hartofilakidis G, et al. [6] examined the long-term outcome of 96 asymptomatic hips in 96 patients with a mean age of 49.3 years who had radiological evidence of FAI. 79 hips remained free of osteoarthritis for a mean of 18.5 years (10 to 40). 17 hips developed osteoarthritis at a mean of 12 years (2 to 28).
The authors concluded that a substantial proportion of hips with FAI may not develop osteoarthritis in the long-term and postulated, that in the absence of symptoms, prophylactic surgical treatment is not warranted. In a prospective study Emara K, et al. [5] examined 37 patients. Patients were instructed to adapt to their safe range of movement and perform activities of daily living with minimal friction, 27 had marked improvement of function and symptoms, 6 had partial improvement, and 4 had no improvement and underwent surgery. Conservative treatment did not improve the range of hip movement, despite improvement in function and symptoms. The authors came to the conclusion that conservative treatment for FAI achieved good early results so long as the patients can modify activities of daily living to adapt to their hip morphology. We follow Hartofilakidis G, et al. [6], that in the absence of symptoms, prophylactic surgical treatment is not warranted.
4. Conclusion
With our case we were able to show that conservative treatment can be effective even in mild symptomatic CAM impingement with good long- term results and should be kept in mind nowadays where is a trend towards operative correction of CAM Impingement.
References
- Banerjee P, Mclean CR. Femoroacetabular impingement: a review of diagnosis and management. Curr Rev Musculoskelet Med 4 (2011): 23-32.
- Beck M, Büchler L. Prevalence and Impact of Pain at the Greater Trochanter After Open Surgery for the Treatment of Femoro-Acetabular Impingement. J Bone Joint Surg Am 93 (2011): 66-69.
- Ganz R, Gill TJ, Gautier E, et al. Surgical dislocation of the adult hip. A technique with full access to the femoral head and acetabulum without the risk of avascular necrosis. J Bone Joint Surg Br 83 (2001): 1119-1124.
- Lamontagne M, Brisson N, Kennedy MJ, et al. Preoperative and postoperative lower-extremity joint and pelvic kinematics during maximal squatting of patients with cam femoro-acetabular impingement. J Bone Joint Surg Am 93 (2011): 40-45.
- Emara K, Samir W, Motasem H, et al. Conservative treatment for mild femoroacetabular impingement. J Orthop Surg (Hong Kong) 19 (2011): 41-45.
- Hartofilakidis G, Bardakos NV, Babis GC, et al. An examination of the association between different morphotypes of femoroacetabular impingement in symptomatic subjects and the development of osteoarthritis of the hip. J Bone Joint Surg Br 93 (2011): 580-586.
- Peters CL, Erickson JA. Treatment of femoro-acetabular impingement with surgical dislocation and débridement in young adults. J Bone Joint Surg Am 88 (2006): 1735-1741.
- Papalia R, Del Buono A, Franceschi F, et al. Femoroacetabular impingement syndrome management: arthroscopy or open surgery? Int Orthop 22 (2011).


 Impact Factor: * 5.3
Impact Factor: * 5.3 Acceptance Rate: 75.63%
Acceptance Rate: 75.63%  Time to first decision: 10.4 days
Time to first decision: 10.4 days  Time from article received to acceptance: 2-3 weeks
Time from article received to acceptance: 2-3 weeks 
