Breast Lump: An Uncommon Metastasis of Prostate Cancer
Prashant Kumar Chauhan, Mayank Jain*, Pramod Adiga, Shivalingaiah M
Department of Urology, Institute of Nephrourology, Victoria hospital Campus, Bengaluru 560002, Karnataka, India
*Corresponding Author: Dr. Mayank Jain, Department of Urology, Institute of Nephrourology, Victoria hospital Campus, Bengaluru 560002, Karnataka, India
Received: 07 May 2020; Accepted: 01 June 2020; Published: 08 July 2020
Article Information
Citation: Prashant Kumar Chauhan, Mayank Jain, Pramod Adiga, Shivalingaiah M. Breast Lump: An Uncommon Metastasis of Prostate Cancer. Archives of Clinical and Medical Case Reports 4 (2020): 624-628.
View / Download Pdf Share at FacebookAbstract
Prostate carcinoma is the second most common cancer in men. Prostatic adenocarcinoma can metastasize to anywhere in the body. It is seen more commonly to lymph node, bone, lung, liver, breast, eyes, kidney, muscle, pancreas, spleen and rarely to adrenal or breast. Prostate carcinoma in form of breast metastasis is extremely rare. Here we discuss a case of 73 year old male k/c/o carcinoma prostate on hormonal treatment and recently diagnosed to have castrate resistant prostatic adenocarcinoma (mCRPC); who developed a large breast lump. Histopathology revealed metastatic deposit from prostatic adenocarcinoma which was confirmed by IHC. Patient responded to docetaxel chemotherapy and is on regular follow-up.
Keywords
<p>Breast metastasis; Prostate adenocarcinoma; Castration Resistant prostate cancer; Prostate specific antigen</p>
Article Details
1. Introduction
Prostatic adenocarcinoma is the second most common primary malignancy in men after oral cancer. Carcinoma prostate can present as localised disease or metastatic disease with incidence of 80% and 20% respectively, with advent of PSA screening. Skeletal metastasis occurs more often while soft tissue metastasis is comparatively rare. Lung and liver is frequent site of soft tissue metastasis. Breast metastasis from non-mammary primary tumours is even rare, with incidence of 0.5-2.0% of all breast malignancies. In case of prostate cancer, it is even rarer [1, 2]. As per literature there is a significant increased risk of breast cancer in patients receiving oestrogen therapy for prostate cancer [3]. Likewise, patients undergoing hormonal therapy for prostate carcinoma have increased blood supply to the breast, resulting in gynecomastia, metastasis or primary malignancy. Difficulties always arise in differentiating primary lesions from metastasis clinically, although metastasis tends to be found in the subcutaneous fat, whereas primary breast cancers develop in glandular tissue [4].
2. Case Report
A 73-year-old male presented with lower urinary tracts symptoms since 6 months. Digital rectal examination revealed grade II prostatomegaly with hard nodules in right lobe. His initial PSA was >100 mg/milk Rest all blood and urine analysis revealed no abnormalities. TRUS guided 12 core prostatic biopsy confirmed prostatic adenocarcinoma with 8 cores positivity, Gleason’s score of 4 + 4 = 8, and ISUP grade group 4. Tc99 MDP Bone scan showed multiple axial bony metastasis. Subsequently patient underwent surgical castration for polymetastatic adenocarcinoma of prostate and bicalutamide 50 mg OD was started. He was asymptomatic and has shown response with falling PSA levels with nadir PSA of 1.2 ng/mL. He was on combined androgen blockade for nearly 2 years before being diagnosed with CRPC. Serum PSA rose to 49.76 ng/mL with Serum testosterone of < 0.45 nmol/L. 3 months later, he presented with a painless swelling in left breast. Swelling was a 7 × 5 cm sized, hard, immobile, and non-tender, without any underlying bone tenderness or lymphadenopathy (Figure 1). High frequency ultrasound of the left breast showed an oval shaped hypo echoic area measuring 4.6 × 2.7 × 3.5 cm in diameter with hyperaemia, more in favour of malignancy. Right breast was normal and there was no evidence of ipsilateral axillary or supraclavicular or neck lymphadenopathy. Chest X Ray also revealed a soft tissue shadow in left breast territory (Figure 2). Breast biopsy showed a malignant infiltrate with positive staining for PSA. PSMA PET-CT showed ill-defined heterogeneous tracer avid lesion 2.8 × 3.2 × 2.5 cm in right lobe of the prostate with diffuse skeletal metastasis with a soft tissue component 6.3 × 7.9 × 5.3 cm infiltrating overlying left serratus anterior muscle. Surprisingly, these results were consistent with metastatic adenocarcinoma of the prostate involving the left breast (Figure 3). Patient is undergoing docetaxel chemotherapy with significant reduction in size of breast lump.
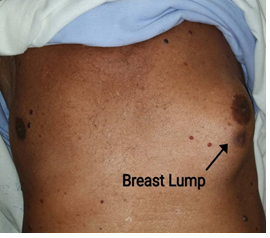
Figure 1: Clinical Image: Large breast lump.
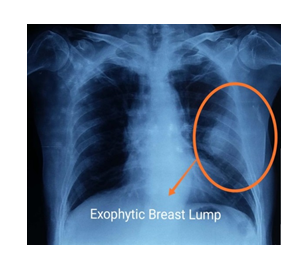
Figure 2:CXR showing exophytic left breast mass.
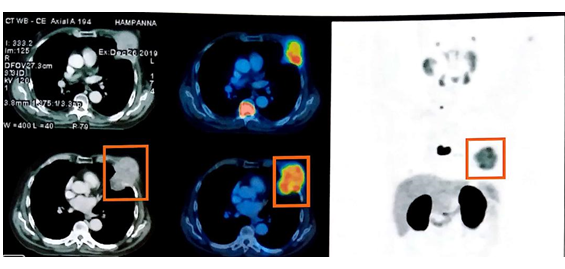
Figure 3: PSMA PET scan: Tracer avid lesion in left upper chest involving left anterolateral wall (max SUV 15).
3. Discussion
Carcinoma prostate presenting with breast metastasis is rarely reported in literature. There is no clear predisposing factors correlating with the development of breast metastasis from carcinoma prostate; and there have been few cases of breast metastasis from carcinoma prostate without any prior hormonal treatment [5]. As per literature, hormonal therapy for carcinoma prostate could predispose to breast metastasis due to an imbalance of oestrogen levels as a result of increased secretion of luteinizing hormones in initial phase [6]. In the past Oestrogen therapy, which was considered the main treatment of carcinoma prostate, has also been attributed to the development of breast metastasis [2, 7]. Bland et al stated that oestrogen causes proliferative changes in the breast with development of both ducts and periductal stroma [8]. Though our patient was not treated with oestrogen, bicalutamide increases testosterone level by blocking negative feedback to luteinizing hormone and thus increased level of oestrogen by aromatization of testosterone, and that can lead to gynaecomastia.
There are only few cases of carcinoma prostate metastasized to breast, as metastatic tumours to the breast arising from non-mammary cancer are rare [1, 2]. Prostate carcinoma on the other hand metastasizes more commonly to the bones, lung, liver, pleura and rarely to adrenal gland, eyes, breast, and kidney [4]. This rare occurrence of breast metastasis is believed to be due to the large areas of fibrous tissue with a relatively poor blood supply within in the breast[9]. Valerie Lima et al (2020) reported a case whose initial presentation was breast lump with infiltrating ductal carcinoma on HPE and on further evaluation it came to be PSAP (prostate specific acid phosphatase) positive metastasis from prostate carcinoma [10]. Hiren Mandaliya et al. (2015) reported case of carcinoma prostate with breast metastasis, staining positive for PSA and consistent with metastatic adenocarcinoma of the prostate [11].
The treatment and prognosis of primary carcinoma of the male breast and metastatic prostatic carcinoma, differs widely. While the primary male breast carcinoma is conventionally managed by wide local excision or mastectomy with axillary node clearance; On the other hand, in metastatic prostatic carcinoma surgical intervention is inappropriate and systemic chemotherapy shows good response. So, it is important to differentiate primary and secondary carcinoma. Histopathological examination of breast lump including PSA and PSAP stains on IHC (immunohistochemistry) would certainly help to differentiate the nature of the pathology [12-14].
4. Conclusion
Breast metastasis for primary adenocarcinoma is very rare. But due increased use of hormonal therapy and resurgence of oestrogen therapy metastatic carcinoma breast should always be kept as differential diagnosis of hard breast lump. Increased awareness and recognition of the rare entity described here is of utmost importance to differentiate it from gynecomastia as well as primary and secondary carcinoma; as treatment and prognosis varies widely, with medical management being the ideal treatment modality.
References
- Feder JM, De paredes ES, Hogge JP et al. Unusual breast lesions: radiologic-pathologic correlation. Radiographics 19 (1999): S11-26.
- Lee UJ, Jones JS. Incidence of prostate cancer in male breast cancer patients: a risk factor for prostate cancer screening. Prostate Cancer Prostatic Dis 12 (2009): 52-56.
- Thellenberg C, Malmer B, Tavelin B, et al. Second primary cancers in men with prostate cancer: an increased risk of male breast cancer. J Urol 169 (2003): 1345-1348.
- Sandison AT. Metastatic tumors in the breast, Br. J. Surg 47 (1959): 54.
- Mostofi FK. Grading of prostatic carcinoma. Cancer Chemother Rep 59 (1975): 111-117.
- Hartley LC, Little JH. Bilateral mammary metastases from carcinoma of the prostate during oestrogen therapy. Med J 1 (1971): 434-436.
- Moldwin RM, Orihuela E. Breast masses associated with adenocarcinoma of the prostate. Cancer 63 (1989): 2229-2233.
- Bland KI, Buchanan JB, Wiseberg BF, et al. The effects of exogenous estrogen replacement therapy of the breast: Breast cancer risk and mammographic parenchymal patterns. Cancer 45 (1980): 3027-3033.
- Mun SH, Ko EY, Han BK, et al. Breast metastases from extramammary malignancies: typical and atypical ultrasound features. Korean J Radiol 15 (2014): 20-28.
- Valerie Lima, Felycette Gay Martinez-Lapus, Kenny Jun Demegillo. Breast Metastasis From Castrate-Resistant Prostatic Adenocarcinoma Mimicking as a Second Primary: A Case Report. World J Oncol 11 (2020): 37-40.
- Mandaliya H, Sung J, Hill J, et al. Prostate cancer: cases of rare presentation and rare metastasis. Case Rep Oncol 8 (2015): 526-529.
- Sahoo S, Smith RE, Potz JL, et al. Metastatic prostatic adenocarcinoma within a primary solid papillary carcinoma of the male breast. Arch Pathol Lab Med 125 (2001): 1101-1103.
- Green LK, Klima M. The use of immunohistochemistry in metastatic prostatic adenocarcinoma to the breast. Hum Pathol 22 (1991): 242-246.
- Cheng CW, Chan LW, Ng CF, et al. Breast metastasis from prostate cancer and interpretation of immunoreactivity to prostate-specific antigen. Int J Urol 13 (2006): 463-465.


 Impact Factor: * 5.3
Impact Factor: * 5.3 Acceptance Rate: 75.63%
Acceptance Rate: 75.63%  Time to first decision: 10.4 days
Time to first decision: 10.4 days  Time from article received to acceptance: 2-3 weeks
Time from article received to acceptance: 2-3 weeks 
