Challenges in COVID-19 in Patients with Haematological Malignancies: Case Report of a Patient with Mantle Cell Lymphoma
Sebastian Knorz1,2*, Susanne Wiebecke1, Petra Schulze1, Sven Schimanski2, Susanne Strifler2, Tobias Gassenmaier3, Erdwine Klinker4, Benedikt Weissbrich5, Hartwig Klinker1
1Department of Internal Medicine II, Division of Infectious Diseases, University Hospital Wuerzburg, Germany
2Department of Internal Medicine II, Division of Haematology, University Hospital Wuerzburg, Germany
3Department of Diagnostic and Interventional Radiology, University Hospital Wuerzburg, Germany
4Department of Transfusion Medicine, University Hospital Wuerzburg, Germany
5Institute for Virology and Immunobiology, University of Wuerzburg, Germany
*Corresponding Author: Dr. Sebastian Knorz, Department of Internal Medicine II, Division of Infectious Diseases, University Hospital Wuerzburg, Oberduerrbacher Str. 6, 97080 Wuerzburg, Germany
Received: 01 August 2021; Accepted: 13 August 2021; Published: 31 August 2021
Article Information
Citation: Sebastian Knorz, Susanne Wiebecke, Petra Schulze, Sven Schimanski, Susanne Strifler, Tobias Gassenmaier, Erdwine Klinker, Benedikt Weissbrich, Hartwig Klinker. Challenges in COVID-19 in Patients with Haematological Malignancies: Case Report of a Patient with Mantle Cell Lymphoma. Archives of Clinical and Medical Case Reports 5 (2021): 599-609.
View / Download Pdf Share at FacebookAbstract
Introduction: Patients with haematological malignancies after chemotherapy are immunocompromised and therefore highly susceptible to Covid-19 disease. Case presentation: The case report presents a patient with mantel cell lymphoma who experienced a severe Covid-19 disease. Simultaneously, a pulmonary thromboembolism and a cerebral bleeding were detected, thereafter a cytomegalovirus reactivation. A therapy with convalescent plasma showed just an intermediate effect on the patient´s prolonged positivity for SARS-CoV-2. Conclusion: The management of COVID-19 disease in patients with haematological malignancies is a complex challenge due to the diverse impairment of the immune system. In addition to the underlying disease, opportunistic infections are of great relevance.
Keywords
<p>Covid-19; SARS-CoV-2; Mantel cell lymphoma; Pulmonary thromboembolism; Bleeding; Cytomegalovirus; Convalescent plasma</p>
Article Details
1. Introduction
Since the beginning of 2020 the new coronavirus SARS-CoV-2 has been a challenge to many health care systems all over the world. However, despite a lot of cases, little is known about the clinical characteristics in patients with chronic pre-existing diseases. Early data from China already suggested that patients with cancer have a high vulnerability in the current pandemic and severe outcomes from the Covid-19 infection [1]. This also includes patients with haematological malignancies. Due to the underlying disease and often intensive chemotherapy, this specific group of patients is immunocompromised and therefore highly susceptible to infections. Also, having been infected, the clinical course is often prolonged compared to a patient with a competent immune system [2]. So far, a standard therapy for a SARS-CoV-2 infection has not been established. Apart from a need-based oxygen therapy there has been a demand for a specific treatment early in the pandemic. Therapies with chloroquine/hydroxychloroquine, cytokine inhibitors, and JAK-inhibitors were suggested to avoid overwhelming inflammatory responses of the body [3]. However, gaining more experience with Covid-19 diseases, the recommended therapy changed several times. The latest meta-analysis could show positive effects for systemic glucocorticoids especially among critical ill patients [4]. Furthermore, remdesivir has been regarded as a potential antiviral medication. But whereas there is a WHO guideline for the use of glucocorticoids [5], data for remdesivir in worldwide conducted randomized clinical trials stayed contradictory and therefore a recommendation has not been published by the WHO [6, 7]. Already early in the pandemic, case reports from China introduced the successful treatment of critical ill patients by using convalescent plasma [8-10]. Convalescent plasma is blood plasma which contains antibodies for SARS-CoV-2 and was acquired from a patient who could clear the virus. In the early period of the pandemic, it was introduced as a therapeutic option, but the latest clinical trials showed partly contradictory data [11, 12]. Therefore, the use of convalescent plasma has not been established in guidelines yet.
However, so far, there is limited knowledge in the therapy of Covid-19 in immunocompromised patients with haematological malignancies. In the following, we present the clinical course of a patient with mantle cell lymphoma and Covid-19.
2. Case Presentation
A 54-year-old male patient was admitted to our ICU from a peripheral hospital on May 5 2020 with Covid-19 disease and a medical history of a classical nodular mantle cell lymphoma. After the diagnosis of this disease in May 2019 the patient had received an alternating therapy of each 3 chemotherapeutic cycles of R-CHOP (rituximab, cyclophosphamide, doxorubicine, vincristine, prednisolone) and R-DHAB (rituximab, dexamethasone, cytarabine, cisplatin). The stem cell mobilization with G-CSF and the stem cell apheresis was followed by a high dose chemotherapy according to the BEAM protocol (carmustine, etopoide, cytarabine, melphalan) and autologous stem cell transplantation in December 2019. Staging examinations in February 2020 showed complete remission. A consolidating therapy with rituximab every two months was recommended by the tumorboard and started.
During the rehabilitation program the patient was tested positive for SARS-CoV-2 on April 02 2020. Due to mild symptoms and no respiratory impairment the patient could be discharged home and was treated symptomatically with mucolytic medication by a general practitioner. On April 20, he was admitted to a peripheral hospital again with a reduced general health condition, fever and shortness of breath. A CT scan showed multifocal, bilateral and peripheral ground glass opacities consistent with Covid-19 pneumonia (Figure 1). The laboratory results showed a new leukopenia and thrombocytopenia and elevated ferritin and Il-6 levels. One day after admission the patient worsened and was transferred to the ICU where endotracheal intubation was necessary. With further progression of the COVID-19 disease the patient was transfered to our university hospital.
On admission to the ICU the patient was stable on pressure-controlled ventilation and low dose catecholamines. The laboratory results showed aspects of hyperinflammation with CRP 50.67 mg/dl (reference value 0-0.5 mg/dl), Il-6 517.8 pg/ml (reference value 0-7 pg/ml) and ferritin 23,986 µg/l (reference value 30-400 µg/l) and the blood cell count a leukopenia (3,900/µl), a thrombocytopenia (16,000 /µl) and an anemia (9.0 g/dl), respectively. On May 05 and 07 tocilizumab was applied and on May 05, 06 and 10 convalescent plasma with a total antibody ratio of 5.4 (retrospectively determined, see Table 1 for detailed information about the transfused convalescent plasma). In the follow-up SARS-CoV-2 antibody measures in the patient´s blood plasma, the detected levels stayed below the benchmark for positive results. Also the Il-6 levels rose steadily. After around one week the respiratory situation improved and the inflammation markers decreased spontaneously. Extubation was considered. Due to a prolonged wake-up and rising d-dimers a CT-scan was performed which showed an extended pulmonary embolism and in parallel a bleeding in the subarachnoid space (Figure 2 and 3). A heparine perfusor was initiated and the thrombocytes were consequently transfused to levels above 50,000/µl. These steps stabilized the patient and extubation was possible.
Fortunately, regarding the cerebral bleeding, no focal neurologic signs occurred. In the further course, there was a painful swelling of the right leg and the need of erythrocyte transfusions increased. For detection of a bleeding source, a CT angiography was performed, revealing an active bleeding in the dorsal right thigh musculature (Figure 4). Surgery was necessary three times during the ICU stay and one more time after the transfer to the infectious disease unit on May 29. Furthermore, a coil embolization of peripheral blood vessels was done twice.
|
Convalescent plasma Product |
Date of transfusion |
Antibody ratio (sample/ negative control) according to EUROIMMUN (reference values: <0.8 negative; >0.8 to <1.1 borderline; > 1.1 positive) |
|
1 |
05/05/2020 06/05/2020 10/05/2020 |
 5.4 5.4 |
|
2 |
09/07/2020 09/07/2020 10/07/2020 |
 10.0 10.0 |
Table 1: Summary of the transfused convalescent plasma. Blood plasma was collected from a previous Covid-19 patient. Each apheresis process allowed to acquire three samples as part of one product. Methods of production are analogous of those of fresh frozen plasma. Permission was given according to the German Medicinal Products Act (AMG).
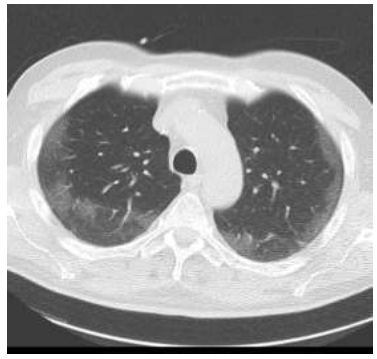
Figure 1: Low dose CT scan of the lung showing multifocal, bilateral and peripheral ground glass opacities consistent with Covid-19 pneumonia.
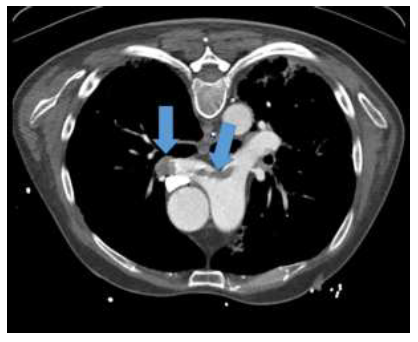
Figure 2: CT scan of the lung showing extended pulmonary embolism. Blue arrows demonstrate the emboli.
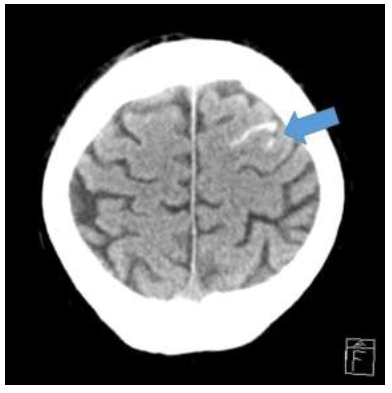
Figure 3: Cranial CT scan. The arrow marks the bleeding in the subarachnoid space.
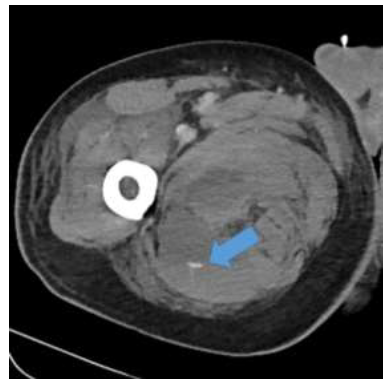
Figure 4: CT angiography of the right thigh. The arrow shows an active bleeding in the dorsal right thigh musculature.
When admitted to the infectious disease ward, the patient was clinically cardiopulmonary stable with no i.v. medication but the heparine perfusor. The oxygen demand was around 6 liters, the inflammation markers still high (CRP 16.47 mg/dl) and the oropharyngeal swabs still highly positive. No fever occurred. However, in the further course body temperatures more than 38.5 °C could be measured again and the general condition of the patient got worse again. New, an atypical pneumonia could be detected in another CT scan and additionally a CMV reactivation via PCR from the blood with 3.6 x 102 copies/ml. We initiated an antiviral therapy with valganciclovir to treat the lung manifestation of this opportunistic infection and an antibiotic therapy as we considered bacterial superinfection. This improved the respiratory situation and the inflammation markers decreased. Due to the persistent pancytopenia a bone marrow puncture was done. Fortunately, it showed together with the already implemented CT imaging no signs of a relapse of the mantle cell lymphoma
In the further course, the patient stabilized clinically and on the laboratory results. He stayed free of fever. At subcutaneously applied enoxaparine no bleeding occurred any more. Oxygen was just needed on demand. However, the weekly taken oropharyngeal swabs on SARS-CoV-2 showed ongoing positive results. The analysis of the lymphocyte subpopulations showed a complete B-cell depletion and a highly reduced number of T-helper cells (17.3 % of all lymphocytes). In consent with the patient we decided to apply convalescent plasma again on July 9 twice and on July 10. This time, the antibody ratio of the product was 10.0 (see Table 1 for detailed data). In the following, adequate antibody levels of SARS-CoV-2 could be detected. The oropharyngeal swabs revealed negative results for the first time for three months. However, when the antibody levels decreased and showed negative results again, the oropharyngeal swabs turned positive again. A viral culture was tried to gain but due to the low virus load in the swabs not possible. Performing daily physiotherapy, the clinical condition of the patient, though, improved increasingly with no supplementary oxygen being necessary any more. We could discharge the patient from hospital into domestic quarantine on August 06 with a final positive oropharyngeal swab, but no clinically symptoms. At the end of September, when the patient presented for a check-up, swabs were still positive. The patient had been free of symptoms and no member of his household had been infected. Finally, at another check-up on November 25, the oropharyngeal swab showed a negative result. At further two-monthly performed check-ups at our outpatient clinic the patient presented in steadily improving health condition. A lung function test showed aspects of a slight restriction, whereas a CT-scan demonstrated an improvement of the pulmonary infiltrates with residual changes of the lung parenchyma. However, clinically, a reduced function of the patient´s right leg stayed which is a result from the recurrent bleedings in the right thigh musculature.
3. Discussion
The described case shows a couple of interesting aspects in the treatment of Covid-19 in a haematological patient. On the basis of the inflammation parameters ferritin, interleukin-6 and CRP Figure 5 allows an overview of the patient´s clinical course.
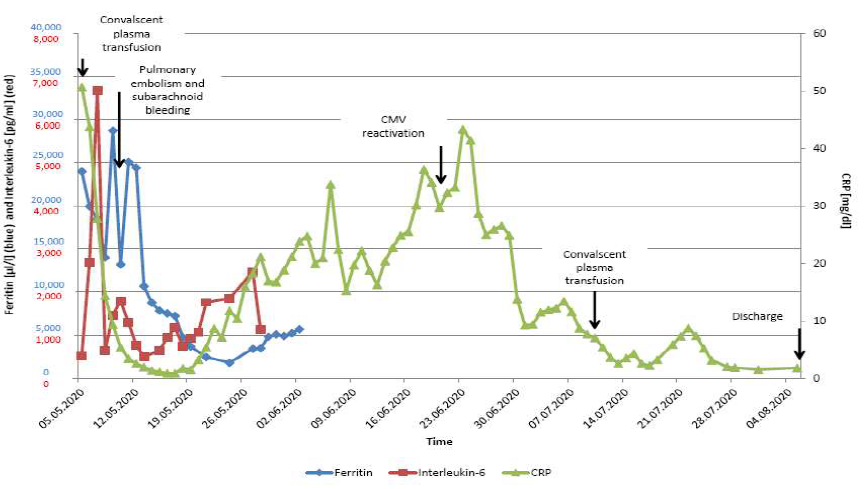
Figure 5: Overview of the inflammation parameters during the in-patient stay. Ferritin and interleukin-6 were just measured during the acute period of the Covid-19 disease. (Reference values: ferritin 30-400 µg/l, interleukin-6 0-7 pg/ml, CRP 0-0.5 mg/dl).
First of all, the case demonstrates the dilemma of thromboembolic events versus bleedings on a Covid-19 patient with a haematological disease. On one hand, patients after intensive chemotherapy often have a compromised haemogram with low thrombocytes. On the other hand, it is known that patients with Covid-19 have a higher risk of venous thromboembolism. A study from China on ICU patients with Covid-19 showed a prevalence of lower extremity venous thrombosis of as high as 25% [13]. A better outcome and a lower mortality was described using an anticoagulant therapy as low molecular weight heparin or unfractionated heparin [14, 15]. In the present case, the patient experienced an extended pulmonary embolism and a subarachnoid bleeding at the same point of time. To our knowledge, this kind of complication has not been described yet in a Covid-19 patient with a haematological disease and low thrombocytes. The event can be seen within the context of haemostaseologic changes induced by SARS-CoV-2. In literature, a Covid-19 associated coagulopathy has been described [16], but more research is necessary to better understand pathomechanisms which can induce a pulmonary embolism even in low thrombocytes. In the described case, in the further course, the necessary anticoagulation was responsible for recurrent bleedings and consecutive surgery in the right groin. In this regard, the described case shows, how difficult the anticoagulatory management of a haematological patient with Covid-19 and reduced thrombocytes after chemotherapy may be.
Furthermore, the case demonstrates, how important it is to consider additional infections in an immunocompromised haematological patient with Covid-19. When the patient had stabilized from the Covid-19-pneumonia, new pulmonary infiltrates were detected in a CT scan and a relevant CMV viremia could be found in parallel. Introducing valganciclovir, the patient improved clinically again. Thus, the case shows that opportunistic viral reactivations may occur simultaneously to a SARS-CoV-2 infection in an immunocompromised patient and consequently must not be neglected. So far, to the best of our knowledge, no study for investigating SARS-CoV-2 infections and simultaneous cytomegalovirus reactivations in haematological patients has been implemented yet. For that reason, research is needed to fill this lack of knowledge. The probably most interesting aspect of the case is the therapeutic management of the patient´s SARS-CoV-2 infection and his clinical outcome. At the period of the patient´s acute disease a therapy with glucocorticoids or remdesivir has not been established yet and so just experimental therapies were possible. Whereas the cytokine inhibitors and the convalescent plasma that was applied during the patient´s ICU stay didn´t seem to have an effect on the clinical course, measurable antibody levels could not be detected until convalescent plasma was applied for a second time.
However, a successful treatment in critical ill patients has been described [8-10, 12]. In the present case, it is likely that due to the lower antibody levels of the first blood product and longer intervals between transfusions no SARS-CoV-2 antibody levels could be measured. Interestingly, the oropharyngeal swabs turned negative when we had transfused convalescent plasma for the second time. Antibodies could be measured. This time, a blood product with a higher number of antibodies was used. Neutralizing effects on the virus could be observed. However, when the SARS-CoV-2- antibodies decreased again in the patient´s serum, the swabs turned slightly positive again whereas the patient stayed clinically asymptomatic. Figure 6 demonstrates the described observations between the serological antibody levels and PCR tests of oropharyngeal swabs graphically. We assume that due to the patient´s compromised immune system with missing B-cells and a highly decreased number of T-helper-cells no functional immunological response of the body was possible and therefore the virus persisted after the acute infection. Thus, the transfusion of convalescent plasma just had an intermediate effect on the virus replication, whereas it didn´t manage to eliminate the virus and probably didn´t have an effect on the patient´s clinical course. We assume that patients like the presented one with long-term positive swabs are not infectious for the environment as no member of the patient´s family got positive results for SARS-CoV-2. But more research on this topic is necessary. Long-term positivity to SARS-CoV-2 in Covid-19 patients has been demonstrated [17]. Also, abnormal antibody responses and a decreased ability to clear SARS-CoV-2 have been described in patients with haematological malignancies in another study [2]. However, there is still limited knowledge about the effectiveness of viral clearance in immunocompromised patients. Future research needs to gain more information.
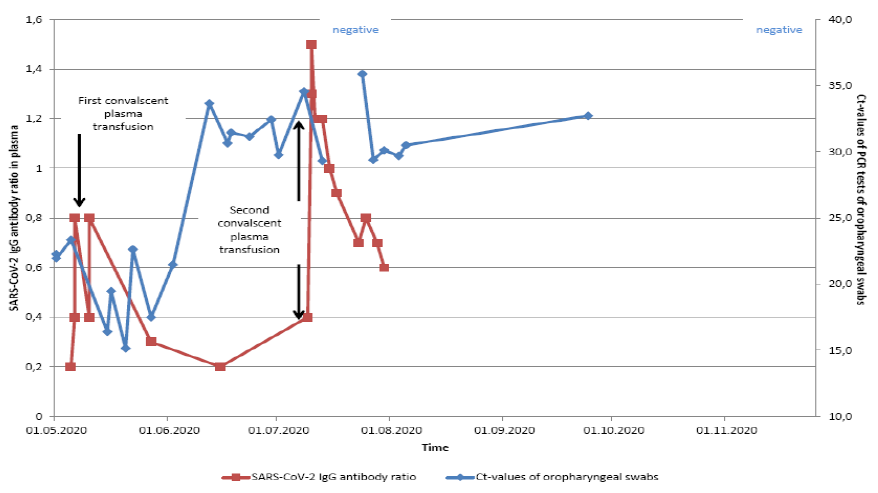
Figure 6: Overview of the SARS-CoV-2 antibody ratio in the patient´s plasma samples and the Ct-values of PCR tests of oropharyngeal swabs. Before the second convalescent plasma transfusion antibody levels showed persistent negative results (reference values: <0.8 negative; >0.8 to <1.1 borderline; > 1.1 positive) and partly low Ct-values (Ct shortens cycle threshold: an amplification cycle that determinates exponential increase in a real-time-PCR). After the second convalescent plasma transfusion significantly positive antibody levels could be measured and the oropharyngeal swabs showed negative results on July 15 and 17. When the antibody levels decreased, Ct-values of the swabs turned positive again, whereas the patient stayed clinically asymptomatic. On November 25, a negative oropharyngeal swab could be detected.
4. Conclusion
This case demonstrates some challenges a haematologist might experience treating a patient with a haematological malignancy and Covid-19. As patients after intensive chemotherapy are heavily immunocompromised, they are especially vulnerable to a SARS-CoV-2 infection. Thus, another opportunistic viral infection like the cytomegalovirus may occur simultaneously to SARS-CoV-2 in addition. Due to low thrombocytes, the anticoagulation therapy in haematological patients after chemotherapy is a challenge in particular as thrombembolisms and bleedings might occur. And finally, convalescent plasma as a therapeutic option supporting viral clearance might not have prolonged effects due to the patients´ compromised immune
system.
Conflict of Interest
The authors declare not to have any conflict of interest.
References
- Dai M, Liu D, Liu M, et al. Patients with Cancer Appear More Vulnerable to SARS-CoV-2: A Multicenter Study during the COVID-19 Outbreak. Cancer Discov 10 (2020): 783-791.
- Wu Y, Chen W, Li W, et al. Clinical characteristics, therapeutic management, and prognostic factors of adult COVID-19 inpatients with hematological malignancies. Leuk Lymphoma 25 (2020): 1-11.
- Zhang W, Zhao Y, Zhang F, et al. The use of anti-inflammatory drugs in the treatment of people with severe coronavirus disease 2019 (COVID-19): The Perspectives of clinical immunologists from China. Clin Immunol 214 (2020): 108393.
- WHO Rapid Evidence Appraisal for COVID-19 Therapies (REACT) Working Group, Sterne JAC, Murthy S, et al. Association Between Administration of Systemic Corticosteroids and Mortality Among Critically Ill Patients With COVID-19: A Meta-analysis JAMA 324 (2020): 1330-1341.
- Corticosteroids for COVID-19 - Living Guidance (2020).
- Beigel JH, Tomashek KM, Dodd LE, et al. ACTT-1 Study Group Members. Remdesivir for the Treatment of Covid-19 - Final Report. N Engl J Med 383 (2020): 1813-1826.
- WHO Solidarity Trial Consortium, Pan H, Peto R, et al. Repurposed Antiviral Drugs for Covid-19 - Interim WHO Solidarity Trial Results. N Engl J Med (2020): NEJMoa2023184.
- Ye M, Fu D, Ren Y, et al. Treatment with convalescent plasma for COVID-19 patients in Wuhan, China. J Med Virol (2020).
- Shen C, Wang Z, Zhao F, et al. Treatment of 5 Critically Ill Patients With COVID-19 With Convalescent Plasma. JAMA 323 (2020): 1582-1589.
- Zhang B, Liu S, Tan T, et al. Treatment With Convalescent Plasma for Critically Ill Patients With Severe Acute Respiratory Syndrome Coronavirus 2 Infection. Chest 158 (2020): e9-e13.
- Li L, Zhang W, Hu Y, et al. Effect of Convalescent Plasma Therapy on Time to Clinical Improvement in Patients with Severe and Life-threatening COVID-19: A Randomized Clinical Trial. JAMA 324 (2020): 460-470.
- Salazar E, Christensen PA, Graviss EA, et al. Treatment of Coronavirus Disease 2019 Patients with Convalescent Plasma Reveals a Signal of Significantly Decreased Mortality. Am J Pathol 190 (2020): 2290-2303.
- Cui S, Chen S, Li X, et al. Prevalence of venous thromboembolism in patients with severe novel coronavirus pneumonia. J Thromb Haemost 18 (2020): 1421-1424.
- Tang N, Bai H, Chen X, et al. Anticoagulant treatment is associated with decreased mortality in severe coronavirus disease 2019 patients with coagulopathy. J Thromb Haemost 18 (2020): 1094-1099.
- Nadkarni GN, Lala A, Bagiella E, et al. Anticoagulation, Bleeding, Mortality, and Pathology in Hospitalized Patients With COVID-19. J Am Coll Cardiol 76 (2020): 1815-1826.
- Connors JM, Levy JH. COVID-19 and its implications for thrombosis and anticoagulation. Blood 135 (2020): 2033-2040.
- Wang X, Huang K, Jiang H, et al. Long-Term Existence of SARS-CoV-2 in COVID-19 Patients: Host Immunity, Viral Virulence, and Transmissibility. Virol Sin 6 (2020): 1-10.


 Impact Factor: * 5.3
Impact Factor: * 5.3 Acceptance Rate: 75.63%
Acceptance Rate: 75.63%  Time to first decision: 10.4 days
Time to first decision: 10.4 days  Time from article received to acceptance: 2-3 weeks
Time from article received to acceptance: 2-3 weeks 
