Dermal Sinus with an Associated Dumbbell Dermoid Cyst: A Case Report
Hayden Scott1*, Olusoji A. Afuwape2, Grace Rice1, Sagar Mehta4,5, Tomoko Tanaka2,3
1College of Medicine, University of Arkansas for Medical Sciences, Little Rock, AR, USA
2Department of Neurosurgery, University of Arkansas for Medical Sciences, Little Rock, AR, USA
3Division of Pediatric Neurosurgery, Arkansas Children’s Hospital, Little Rock, AR, USA
4Department of Plastic and Reconstructive Surgery, University of Arkansas for Medical Sciences, Little Rock, AR, USA
5Division of Plastic and Reconstructive Surgery, Arkansas Children’s Hospital, Little Rock, AR, USA
*Corresponding Author: Hayden Scott, College of Medicine, University of Arkansas for Medical Sciences, Little Rock, AR, USA
Received: 01 September 2021; Accepted: 16 September 2021; Published: 15 October 2021
Article Information
Citation: Hayden Scott, Olusoji A. Afuwape, Grace Rice, Sagar Mehta, Tomoko Tanaka. Dermal Sinus with an Associated Dumbbell Dermoid Cyst: A Case Report. Archives of Clinical and Medical Case Reports 5 (2021): 699-703.
View / Download Pdf Share at FacebookKeywords
<p>Dermoid cyst; Dermal sinus; Neurosurgery</p>
Article Details
1. Introduction
Dermoid cysts are benign growths that develop from ectodermal components [1]. Similar to a simplistic teratoma, these dermoid cysts are often composed of sebum, keratin, and hair [2, 3]. Dermoid cysts typically present along midline of the head and neck with limited record of cases involving the infratemporal fossa [4]. One review describes less than 20 cases of dermoid cysts occurring in the lateral frontotemporal region with a sinus tract and bony involvement. Of the 20 cases described, only seven had intracranial extension [5]. Another larger series reviewed a total of 280 cases involving orbital and periorbital dermoid and epidermoid cysts, and found that the periorbital location accounted for more than 50% of all cases reported in the head and neck region [6]. Notably, dermoid cysts with extension into the temporal fossa were only seen in 5.7% of the cases in the series. Additionally, subperiosteal dermoid cysts were most destructive due to bony invasion [6].
2. Case Report
We describe an 8-year-old male with a history of recurrent drainage since near birth from the left lateral periorbital region who was followed by his PCP and had now developed headaches that centered around the lesion. The patient was initially referred to General Surgery and a contrasted CT scan was obtained revealing of a 2 cm lytic lesion with sclerotic borders invading the lateral orbital wall along with soft tissue enhance overlying the defect (Figure 1B-D). This lesion was further characterized with an MRI prior to referral for Neurosurgery evaluation. MRI findings were notable for a diffusion restricting T2 hypertintense lesion associated with an overlying soft tissue enhancing lesion superior to the temporalis muscle with concerns for inflammatory changes within the muscle itself (Figure 1A) which was concerning for a dermoid cyst.
The patient was taken to the operative theater as a combined case between Neurological and Plastics Craniofacial surgery. An incision was made at the margins of the discolored skin (Figure 2A) and excised revealing of a stalk-like fibrotic stalk that appeared to extend through the soft tissue into the lateral orbital wall of the sphenoid wing to connect to a large cystic mass (Figure 2B). Thick yellow content was easily expelled with manipulation of the mass and this fluid was sent for culture (Figure 2C). The margins of cyst were delineated from the underlying bone and the entire lesion including the stalk was grossly resected (Figure 2D). The cavity was cauterized to ensure no tissue remnants to avoid recurrence. A vascularized fascial graft was excised and used to fill the bony defect prior to closure.
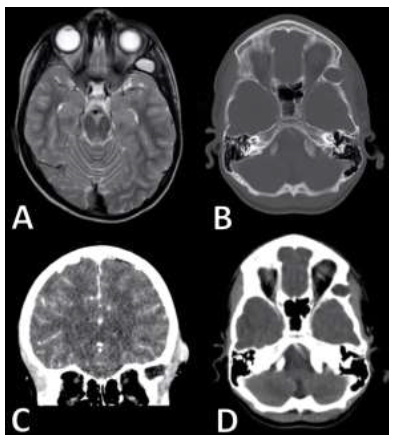
Figure 1: A: T2 Axial MRI findings notable for a diffusion restricting T2 hypertintense lesion associated with an overlying soft tissue enhancing lesion superior to the temporalis muscle with concerns for inflammatory changes within the muscle itself.
B: Axial CT, bone windowed; C: coronal contrasted CT; D: Axial CT imaging revealing of a 2 cm lytic lesion with sclerotic borders invading the lateral orbital wall along with soft tissue enhance overlying the defect.
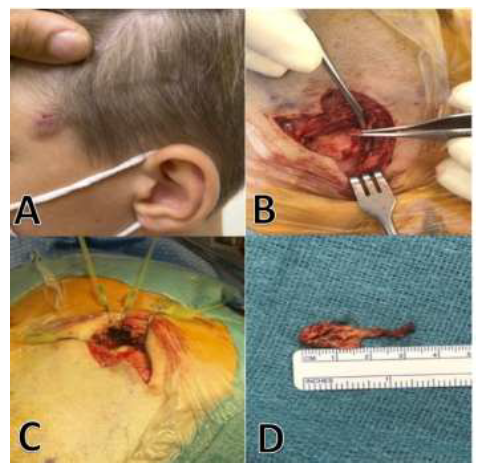
Figure 2: Patient findings including: A). Cutaneous lesion B).Sinus tract C). Purulent cyst content D). Dermoid cyst capsule.
3. Discussion
Dermoid cysts arise from sequestered ectodermal tissue during neural tube closure and are typically found at suture lines involving the head and neck. Most of the lesions present in the nasoglabellar, occipital and frontotemporal regions. Though these lesions can be associated with intracranial, intradural extension, frontotemporal dermoid cysts are typically extracranial on presentation. Dermal sinus tracts also arise from defects in neurulation and are commonly located along midline in both thoracolumbar and cranial regions. It is hypothesized these arise during apposition of embryonic tissue and periosteum and as such are commonly identified in the occipital and nasoglabellar regions. A frontotemporal dermoid cyst with an associated dermal sinus tract is quite rare but has been previously described in the literature. Furthermore, we could identify only one other report of a bilobed frontotemporal dermoid cyst with an associated dermal sinus tract [7]. We present another case of a bilobed frontotemporal dermoid cyst with a dermal sinus tract and recommend early referral to a Neurological Surgery specialist after workup that includes, at minimum, a sophisticated thin slice CT with 3D reconstruction. Here we present a case of a bilobed pterional dermoid cyst with an associated dermal sinus tract which is rare despite the growing literature on frontotemporal dermoid cysts [7-9]. However, this lesion's location and presentation is more consistent with prior descriptions of primary temporal fossa dermoid cysts that could potentially behave differently than frontotemporal dermoid cysts which primarily develop anterior to the frontozygomatic suture. Dermoid cysts anterior to the frontozygomatic suture typically present as a painless, mobile mass without bony involvement amenable to simple gross resection. Primary temporal dermoid cysts have been associated with anterior displacement of temporalis, bony remodeling, intracranial extension, pain with mastication and bilobed lesions. Meyer et al. (1999) described primary temporal fossa dermoid cysts in 5 patients with common characteristics comprising of originating in the temporal fossa, displacing the temporalis with associated underlying bony erosion [10]. In this series, only one patient had an associated draining sinus tract indicative of the rarity of temporal dermoid cysts with associated dermal sinus tracts. The bony erosion associated with draining dermoid cysts in this region can potentially extend intracranially though neither report noted meningitis as a presenting symptom [8-10].
In a series of 280 cases of periorbital and orbital dermoid cysts, only 16 (5.7%) lesions were found to be bilobed and all of which involved the temporal fossa6. Similarly, other reports of bilobed dermoid cysts have arisen in the temporal fossa and one of which was associated with a draining sinus tract [7, 11]. Taken together, dermoid cysts within the temporal fossa are associated with findings not easily discerned on routine physical examination. Though some reports have noted good outcomes after resection of simple lesions without preoperative imaging, there are increasing reports noting the extensive involvement of frontotemporal dermoid cysts. We propose that preoperative imaging be obtained for all lesions concerning for a dermoid cyst to guide operative planning and ensure an appropriate multidisciplinary approach is utilized when warranted. Prior studies have noted physical exam findings that are more concerning for extensive involvement including immobility, drainage, erythema or concern for intraorbital extension. In this case, the patient had an immobile, erythematous draining lesion at time of presentation. However, imaging was delayed until the patient complained about headaches and pain with chewing. It is likely earlier imaging would have identified the lesion with potentially less invasive features.
The deep culture that was obtained intraoperatively reportedly demonstrated skin flora, supporting the observed finding that the cutaneous lesion appeared to extend completely and invade the left lateral orbital wall forming a sinus tract with an associated bilobed pterional dermoid cyst. The aforementioned case series suggests early removal of all dermoid cysts resulting in bone changes along with imaging to rule out dumbbell or subperiosteal extension, such as the dumbbell cyst seen in our report [6].
4. Conclusion
The lateral frontotemporal region with a sinus tract with dumbbell dermoid cyst is rare. Due to its infrequency, preoperative evaluation may be misguided for potential adverse outcomes. Therefore, early thin sliced head/orbital CT with 3D reconstruction along with referral to neurosurgery and/or cranofocial plastic surgery is recommended. This case highlights the importance of preoperative imaging for all lesions concerning for a dermoid cyst as a guide for operative planning and ensure optimal management. Preoperative imaging can be revealed extent of bony erosion, abnormal lesion shape and intracranial or intraorbital extension. Finally, in agreeance with the reported literature, we recommend early removal of dermoid cysts in their entirety when possible, which too can be dependent on appropriate preoperative planning in the setting of extensive adjacent involvement.
Conflicts of Interest
The authors declare that there are no conflicts of interest.
References
- Shareef S, Ettefagh L. Dermoid Cyst. Brain Imaging with MRI CT An Image Pattern Approach. (2021): 153-154.
- HS U, AR D, R D, RM I. Dermoid cyst of the infratemporal fossa. J Laryngol Otol 116 (2002): 150-152.
- TM T, A G, KJ H, SL B. Dermoid cyst of the infratemporal fossa: case report and review of the literature. J Neurol Surg reports 75 (2014): e33-e37.
- AN S, H K, T M, et al. An Infratemporal Dermoid Cyst That Expanded the Foramen Ovale: A Case Report. World Neurosurg 116 (2018): 305-308.
- Vega RA, Hidlay DT, Tye GW, et al. Intradiploic dermoid cyst of the lateral frontotemporal skull: Case report and review of the literature. Pediatr Neurosurg 49 (2013): 232-235.
- Pushker N, Meel R, Kumar A, et al. Orbital and periorbital dermoid/epidermoid cyst: a series of 280 cases and a brief review. Can J Ophthalmol 55 (2020): 167-171.
- AS B, SM S, A L. Frontotemporal Dermal Sinus Tract with 2 Connected Intradiploic Dermoid Cysts: A Rare Case and Review of the Literature. World Neurosurg 127 (2019): 350-353.
- SW H. Deep frontotemporal dermoid cyst presenting as a discharging sinus: a case report and review of literature. Br J Plast Surg 51 (1998): 255-257.
- C Y, DW L. A Rare Presentation of a Dermoid Cyst with Draining Sinus in a Child: Case Report and Literature Review. Pediatr Dermatol 33 (2016): e244-e248.
- DR M, AM L, RP Y, JV L. Primary temporal fossa dermoid cysts. Characterization and surgical management. Ophthalmology 106 (1999): 342-349.
- D N, E A, NR S. Craniectomy for a bilobed dermoid cyst in the temporal fossa and greater wing of the sphenoid bone. Pediatr Neurosurg 45 (2009): 46-48.


 Impact Factor: * 5.3
Impact Factor: * 5.3 Acceptance Rate: 75.63%
Acceptance Rate: 75.63%  Time to first decision: 10.4 days
Time to first decision: 10.4 days  Time from article received to acceptance: 2-3 weeks
Time from article received to acceptance: 2-3 weeks 
