Desmoid Fibromatosis Presenting as An Omental Mass: A Case Report
Aljalabneh Basim1*, Shenjere Patrick3, O'Dwyer ST1,2
1Department of Surgery, Colorectal and Peritoneal Oncology Centre, The Christie Hospital NHS Foundation Trust, UK
2MAHSC Professor of Surgery, University of Manchester, UK
3Department of Pathology, The Christie Hospital NHS Foundation Trust, UK
*Corresponding Author: Aljalabneh Basim, Department of Surgery, Colorectal and Peritoneal Oncology Centre, The Christie Hospital NHS Foundation Trust, UK
Received: 28 December 2020; Accepted: 09 February 2021; Published: 15 December 2021
Article Information
Citation: Aljalabneh Basim, Shenjere Patrick, O'Dwyer ST. Desmoid Fibromatosis Presenting as An Omental Mass: A Case Report. Archives of Clinical and Medical Case Reports 5 (2021): 950-956.
View / Download Pdf Share at FacebookAbstract
Intra-abdominal desmoid fibromatosis (IADF) is a rare condition, comprising 8-15% of all presentations of desmoid fibromatosis (DF), most commonly arising from the small bowel mesentery. We report the case of a 34 year old male, who presented with a 7.4 x 6.5 cm right iliac fossa mass arising from the omentum. Percutaneous biopsy was inconclusive and the working diagnosis was desmoplastic small round cell cancer of appendiceal or urachal origin. He underwent a diagnostic debulking procedure; a dominant omental mass was removed and 2-3 mm peritoneal nodules on the distal small bowel mesentery and a bulky mass around the root of the superior mesenteric vessels were noted. Histopathological, immunohistochemical and gene mutation analysis confirmed IADF as the definitive diagnosis. We review the literature of this rare presentation and discuss challenges in diagnosis and subcategorization of DF.
Keywords
Fibromatosis; Desmoid; Omentum
Fibromatosis articles; Desmoid articles; Omentum articles
Fibromatosis articles Fibromatosis Research articles Fibromatosis review articles Fibromatosis PubMed articles Fibromatosis PubMed Central articles Fibromatosis 2023 articles Fibromatosis 2024 articles Fibromatosis Scopus articles Fibromatosis impact factor journals Fibromatosis Scopus journals Fibromatosis PubMed journals Fibromatosis medical journals Fibromatosis free journals Fibromatosis best journals Fibromatosis top journals Fibromatosis free medical journals Fibromatosis famous journals Fibromatosis Google Scholar indexed journals COVID-19 articles COVID-19 Research articles COVID-19 review articles COVID-19 PubMed articles COVID-19 PubMed Central articles COVID-19 2023 articles COVID-19 2024 articles COVID-19 Scopus articles COVID-19 impact factor journals COVID-19 Scopus journals COVID-19 PubMed journals COVID-19 medical journals COVID-19 free journals COVID-19 best journals COVID-19 top journals COVID-19 free medical journals COVID-19 famous journals COVID-19 Google Scholar indexed journals Desmoid articles Desmoid Research articles Desmoid review articles Desmoid PubMed articles Desmoid PubMed Central articles Desmoid 2023 articles Desmoid 2024 articles Desmoid Scopus articles Desmoid impact factor journals Desmoid Scopus journals Desmoid PubMed journals Desmoid medical journals Desmoid free journals Desmoid best journals Desmoid top journals Desmoid free medical journals Desmoid famous journals Desmoid Google Scholar indexed journals Temporal lobe epilepsy articles Temporal lobe epilepsy Research articles Temporal lobe epilepsy review articles Temporal lobe epilepsy PubMed articles Temporal lobe epilepsy PubMed Central articles Temporal lobe epilepsy 2023 articles Temporal lobe epilepsy 2024 articles Temporal lobe epilepsy Scopus articles Temporal lobe epilepsy impact factor journals Temporal lobe epilepsy Scopus journals Temporal lobe epilepsy PubMed journals Temporal lobe epilepsy medical journals Temporal lobe epilepsy free journals Temporal lobe epilepsy best journals Temporal lobe epilepsy top journals Temporal lobe epilepsy free medical journals Temporal lobe epilepsy famous journals Temporal lobe epilepsy Google Scholar indexed journals Omentum articles Omentum Research articles Omentum review articles Omentum PubMed articles Omentum PubMed Central articles Omentum 2023 articles Omentum 2024 articles Omentum Scopus articles Omentum impact factor journals Omentum Scopus journals Omentum PubMed journals Omentum medical journals Omentum free journals Omentum best journals Omentum top journals Omentum free medical journals Omentum famous journals Omentum Google Scholar indexed journals treatment articles treatment Research articles treatment review articles treatment PubMed articles treatment PubMed Central articles treatment 2023 articles treatment 2024 articles treatment Scopus articles treatment impact factor journals treatment Scopus journals treatment PubMed journals treatment medical journals treatment free journals treatment best journals treatment top journals treatment free medical journals treatment famous journals treatment Google Scholar indexed journals CT articles CT Research articles CT review articles CT PubMed articles CT PubMed Central articles CT 2023 articles CT 2024 articles CT Scopus articles CT impact factor journals CT Scopus journals CT PubMed journals CT medical journals CT free journals CT best journals CT top journals CT free medical journals CT famous journals CT Google Scholar indexed journals MRI articles MRI Research articles MRI review articles MRI PubMed articles MRI PubMed Central articles MRI 2023 articles MRI 2024 articles MRI Scopus articles MRI impact factor journals MRI Scopus journals MRI PubMed journals MRI medical journals MRI free journals MRI best journals MRI top journals MRI free medical journals MRI famous journals MRI Google Scholar indexed journals surgery articles surgery Research articles surgery review articles surgery PubMed articles surgery PubMed Central articles surgery 2023 articles surgery 2024 articles surgery Scopus articles surgery impact factor journals surgery Scopus journals surgery PubMed journals surgery medical journals surgery free journals surgery best journals surgery top journals surgery free medical journals surgery famous journals surgery Google Scholar indexed journals Torticollis articles Torticollis Research articles Torticollis review articles Torticollis PubMed articles Torticollis PubMed Central articles Torticollis 2023 articles Torticollis 2024 articles Torticollis Scopus articles Torticollis impact factor journals Torticollis Scopus journals Torticollis PubMed journals Torticollis medical journals Torticollis free journals Torticollis best journals Torticollis top journals Torticollis free medical journals Torticollis famous journals Torticollis Google Scholar indexed journals
Article Details
1. Case Report
Our patient is a 34 year old Caucasian male. He initially presented with four months history of diarrhea and weight loss. Clinical examination revealed a right sided lower abdominal mass and a CT scan noted an omental mass in the right iliac fossa measuring 7 x 2 cm with stranding and nodularity in the surrounding tissues. A colonoscopy and an oesophagogastroscopy were clear of any abnormality. An initial USS guided biopsy was inconclusive. His medical history included depression and anxiety although he was not on any medication. His only surgical history was a hand tendon repair at the age of 4. He has no family history of Familial Adenomatous Polyposis (FAP) and/or Gardner syndrome and there was no history of abdominal trauma.
After a 12 month period of observation he was referred to our hospital with progressive abdominal pain and mass in the RIF. A second CT scan demonstrated a 6.8 x 2.7 cm (axial) x 7.5 cm (craniocaudal) mass arising within the omentum, with soft tissue nodules extending along the anterior abdominal wall peritoneum to the level of the urinary bladder. In addition, there were areas of abnormal soft tissue nodularity in the left upper quadrant and tissue surrounding the superior mesenteric vessels. There were no size significant abdominal or pelvic lymph nodes and no free fluid. No source of a primary neoplasm was identified. Tumor markers: CEA, CA15.3 and CA19.9 were within normal ranges. A pathology review of the previous biopsy showed findings suggestive of a sclerotic process and a diagnosis of desmoid fibromatosis was proposed, but definitive diagnosis was not possible on the limited tissue available. Given the rarity of omental disease associated with DF, concerns remained that this could represent peritoneal surface malignancy. Following a Multidisciplinary team (MDT) discussion it was greed that a formal resection of the omental mass would relieve symptoms and confirm a definitive diagnosis.
He underwent a laparotomy were the omental mass was confirmed and removed. Diffuse nodular deposits along the distal small bowel mesentery and thickened tissue around the superior mesenteric vessels at the root of the mesentery were confirmed. Nodularity extended along the peritoneum to the dome of the bladder along the line of the urachus and this was excised en bloc. His appendix appeared grossly normal but was removed to exclude primary appendiceal pathology. He recovered well and was discharged without complications 5 days following surgery.
Histopathology demonstrated features of a desmoid-type abdominal fibromatosis (Figure 1a) with most areas showing near total hyalinisation (Figure 1b). The urachal tissue and appendix were normal. The lesional cells were positive for smooth muscle actin (SMA) (Figure 1c), whilst Desmin, ALK1, DOG1, CD117, and Beta-catenin nuclear staining were all negative. CTNNB1 gene mutation analysis by PCR and restriction enzyme digestion (exon 3) was negative for the 3 most common substitutions (p.T41A, p.S45P and p.S45F).
Follow up 6 months after surgery noted that his symptoms had settled. Consideration has been given to treatment with Cox 2 inhibitors but the patient has elected for surveillance rather than active treatment. He has been referred for genetic assessment and counseling.
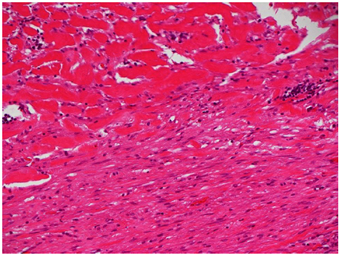
Figure 1a: Fibromatosis showing transition between a cellular region (bottom half) and a paucicellular hyalinised area (top half). The cellular region comprises long sweeping fascicles of bland looking spindle cells.
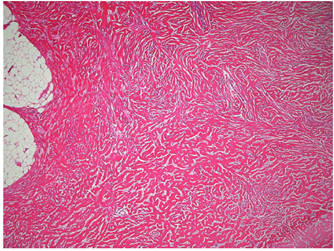
Figure 1b: Paucicellular region with keloid-like collagen bands.
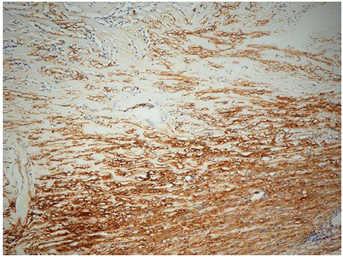
Figure 1c: The spindle cells are positive for SMA.
2. Discussion
Desmoid fibromatosis (DF) is a rare, locally aggressive condition that comprises 0.03% of all neoplasms commonly presenting in the soft tissues of the trunk and limbs in the 25-35 year age group [1-4]. DF accounts for <1% of intra-abdominal tumors when it is described as Intra-abdominal fibromatosis (IAF), and arises most commonly within the small bowel mesentery; retroperitoneal fibromatosis is a second notable site. IAF has a 2:1 predilection towards younger females, possibly due to estrogen influence [1, 2, 5, 6]. Although its course is often indolent it is unpredictable, and can lead to fatal outcomes due to local progression in the mesentery leading to enteric dysfunction and malnutrition [1, 7]. Risk factors include previous trauma, abdominal surgery, pregnancy and family history of DF. Although usually sporadic, specific genetic profiles are associated with IAF namely Familial Adenomatosis Polyposis (FAP) and Gardner Syndrome due to APC germline mutations [8, 9].
Diagnosis is usually established by histopathological examination, however it can be challenging to exclude other spindle cell tumours including gastrointestinal stromal tumors (GIST), hence immunohistochemistry is commonly employed to assist with defining the cellular subtypes [10, 11]. IAF stains positive for vimentin and SMA, and nuclear beta-catenin staining supports the diagnosis. Desmin, cytokeratins, and S-100 are usually negative. Next-generation mutation analysis sequencing is reported to be highly sensitive (92%) and specific (100%) for the detection of CTNNB1 mutations in sporadic desmoid-type fibromatosis and may be used to direct therapy with COX 2 selective inhibitors [12-16]. FAP/Gardner’s syndrome related tumours harbor mutations in the APC tumour suppressor gene and do not have CTNNB1 gene alterations [15]. Table 1 shows the most common histological differential diagnoses and their immunohistochemical staining profiles [17-19].
|
Immunohistochemistry |
IAF* |
GIST** |
Leiomyosarcoma |
Solitary Fibrous Tumour |
|
Β-catenin |
Positive |
Negative |
Negative |
Negative |
|
CD 117 |
Negative |
Positive in 95% |
Negative |
Negative |
|
CD 34 |
Negative |
Positive in 70% |
Negative |
Positive |
|
STAT6 |
Negative |
Negative |
Negative |
Positive |
|
Smooth muscle actin (SMA) |
Positive in 75% |
Positive in 63% |
Positive |
Negative |
|
Desmin |
Positive in 50% |
Positive in 8% |
Positive |
Negative |
|
DOG1 |
Negative |
Positive |
Negative |
Negative |
*Intra-abdominal Fibromatosis
** Gastrointestinal Stromal Tumour
Table 1: Outline of immunohistochemical discriminators for distinguishing sarcomas, IAF and fibrous tumours.
Treatments for IAF include observation, COX 2 selective inhibitors, systemic anthrax-cycline based chemotherapy, and radiotherapy. However as some cases spontaneously resolve asymptomatic patients should undergo a period of observation once diagnosis has been established. Surgery should be directed towards diagnosis and reserved for symptom relief as radical resection is likely to result in a poor quality of life. Active surveillance showed similar 2-year event free survival compared to surgery [20, 21]. The role of selective COX 2 inhibitors has been studied in tumors with COX 2 expression, as it can potently induce anti-tumor responses by both COX-2 dependent and independent mechanisms, on the basis of CTNNB1 and APC mutations, as they are part of the Wingless/WNT signaling pathway which results in accumulation of β-catenin which triggers COX 2 contributing to tumorigenesis [16].
To date, only 7 cases of omental IADF have been reported [22-28]. As in this case, patients usually present with vague abdominal symptoms and an abdominal mass. Imaging with CT and US can be helpful in defining the anatomy and determining multifocal deposits but diagnosis requires histopathological and immunochemical analysis. Differential diagnosis includes mesenteric panniculitis and sclerosis, retroperitoneal fibrosis and gastrointestinal stromal tumors [22].
This case presented a diagnostic challenge relating to its presentation as a predominant omental mass and inconclusive pathology at biopsy. Clinically a urachal primary with peritoneal metastases was a more likely diagnosis than IAF. At laparotomy in the absence of a definitive diagnosis concern remained that the patient had peritoneal malignancy with unresectable disease around the mesenteric root hence it was judged best to obtain definitive pathology rather than undertake more radical surgery.
The second challenge was that the immuno-staining profile did not conform to that expected in IAF. DF usually shows nuclear staining with beta catenin (80%) which was not the case here. This resulted in the need for gene mutation analysis for CTNNB1 which was also negative. CTNNB1 mutation is seen in 90-95% of cases of sporadic desmoid tumours. The lack of CTNNB1 mutation is seen in DF related to Gardner’s syndrome with the APC gene mutation [17]. This raises the possibility of an APC genetic mutation in the absence of clinical FAP/Gardner’s syndrome in our patient, hence genetic assessment with APC mutation analysis and counseling is warranted and ongoing.
3. Conclusion
There are only 7 prior cases of omental IADF reported in the literature. More common causes of an omental mass include metastases from gastric, colorectal, ovarian and appendiceal cancers which must be excluded with such a presentation. Diagnosis required tissue for immunohistochemistry which although often derived from nonsurgical intervention, surgical biopsy with limited resection may be necessary. Once diagnosed, non-surgical treatments can directed toward patients' symptoms and more sophisticated genetic markers may be helpful in directing therapy.
References
- Sakorafas GH, Nissotakis C, Peros G. Abdominal desmoid tumors. Surg Oncol 16 (2007): 131-142.
- Eastley NC, Hennig IM, Esler CP, et al. Nationwide trends in the current management of desmoid (aggressive) fibromatosis. Clin Oncol (R Coll Radiol) 27 (2015): 362-368.
- Eastley N, Aujla R, Silk R, et al. Extra-abdominal desmoid fibromatosis-a sarcoma unit review of practice, long term recurrence rates and survival. Eur J Surg Oncol 40 (2014): 1125-1130.
- Plukker JT, van Oort I, Vermey A et al. Aggressive fibromatosis (non-familial desmoids tumour): therapeutic problems and the role of adjuvant radiotherapy. Br J Surg 82 (1995): 510-514.
- DeVita V T, Lawrence TS, Rosenberg SA, et al. Cancer: Principles and Practice of Oncology. Lippincot Williams and Wilkins. 8th Edn. 2: (2008).
- Kreuzberg B, Koudelova J, Ferda J, et al. Diagnostic problems of abdominal desmoid tumors in various locations. European Journal of Radiology 62 (2007): 180-185.
- Colombo C, Miceli R, Le Pechoux C, et al. Sporadic extra abdominal wall desmoid-type fibromatosis: surgical resection can be safely limited to a minority of patients. Eur J Cancer 51 (2015): 186-192.
- Walczak BE, Rose PS. Desmoid: the role of local therapy in an era of systemic options. Current Treatment Options in Oncology 14 (2013): 465-473.
- Clark SK, Neale KF, Landgrebe JC, et al. Desmoid tumours complicating familial adenomatous polyposis. British Journal of Surgery 86 (1999): 1185-1189.
- Penel N, Coindre JM, Bonvalot S et al. Management of desmoid tumours: A nationwide survey of labelled reference centre networks in France. Eur J Cancer 58 (2016): 90-96.
- Huss S, Nehles J, Binot E et al. β-catenin (CTNNB1) mutations and clinicopathological features of mesenteric desmoid-type fibromatosis. Histopathology 62 (2013): 294-304.
- Wang WL, Nero C, Pappo A, et al. CTNNB1 genotyping and APC screening in pediatric desmoid tumors: a proposed algorithm. Pediatr Dev Pathol 15 (2012): 361-367.
- Colombo C, Bolshakov S, Hajibashi S et al. Difficult to diagnose' desmoid tumours: a potential role for CTNNB1 mutational analysis. Histopathology 59 (2011): 336-340.
- Crago AM, Chmielecki J, Rosenberg M, et al. Near universal detection of alterations in CTNNB1 and Wnt pathway regulators in desmoid-type fibromatosis by whole-exome sequencing and genomic analysis. Genes Chromosomes Cancer 54 (2015): 606-615.
- Aitken SJ, Presneau N, Kalimuthu S, et al. Next-generation sequencing is highly sensitive for the detection of beta-catenin mutations in desmoid-type fibromatoses. Virchows Arch 467 (2015): 203-210.
- Shanshan Yang, Xufu Wang, Haiping Jiang, et al. Effective treatment of aggressive fibromatosis with celecoxib guided by genetic testing, Cancer Biology & Therapy 18 (2017): 757-760.
- b-Catenin (CTNNB1) mutations and clinicopathological features of mesenteric desmoid-type fibromatosis Histopathology 62 (2013): 294-304.
- Giovanni Li Destri, Maria Jessica Ferraro, Martina Calabrini, et al. Desmoid-Type Fibromatosis of the Mesentery: Report of a Sporadic Case with Emphasis on Differential Diagnostic Problems. Case Reports in Medicine (2014): 7.
- Marek Wronski,Bogna Ziarkiewicz-Wroblewska, Maciej Slodkowski. Mesenteric fibromatosis with intestinal involvement mimicking a gastrointestinal stromal tumour. Radiol Oncol 45 (2011): 59-63.
- The management of desmoid tumours: A joint global consensus-based guideline approach for adult and paediatric patients The Desmoid Tumor Working Group1 European Journal of Cancer 127 (2020): 96e107.
- Kasper B, Baumgarten C, Garcia J, et al. An Update On The Management Of Sporadic Desmoid-Type Fibromatosis: A European Consensus Initiative Between Sarcoma Patients Euronet (Spaen) And European Organisation For Research And Treatment Of Cancer (Eortc) / Soft Tissue And Bone Sarcoma Group (Stbsg). behalf of the Desmoid Working Group.
- Channabasappa kori, Pradyumn singh, Neelesh Jain, et al. Giant Omental Fibromatosis Presenting as Pelvic Mass. Journal of Clinical and Diagnostic Research 9 (2015): XD06-XD08.
- Anthony C. Disher, Mahua Biswas. Atypical desmoid tumour of the abdomen: A case report. Journal of the National Medical Association 85 (1993): 309-331.
- Y Pakosy, M Sahin. Omental fibroma: CT AND USG finding. European Radiol Journal 8 (1998): 1422-1424.
- Domenico Iusco, Enrico Donadei, Giuseppe Sgobba, et al. Giant fibroma of the lesser omentum: report of a rare case. Acta Biomed 76 (2005): 42-44.
- Masanori Ono, Kyoko Tanaka, Nana Ikezawa. Fibroma of the Omentum Resembling an Ovarian Tumourin the Pelvis. Keio J Med 58 (2009): 234-236.
- Ahmed T, Hussain MM, Ahmed SU. A 30 year old female with lower abdominal lump. Mymensingh Med J 20 (2011): 138-144.
- Iusco D, Donadei E, Sgobba G, et al. Giant fibroma of the lesser omentum: report of a rare case. Acta Biomed 76 (2005): 42-44.


 Impact Factor: * 5.3
Impact Factor: * 5.3 Acceptance Rate: 75.63%
Acceptance Rate: 75.63%  Time to first decision: 10.4 days
Time to first decision: 10.4 days  Time from article received to acceptance: 2-3 weeks
Time from article received to acceptance: 2-3 weeks 
