Plasma Exeresis Technology for Rejuvenation of the Upper Eyelid
Chrisanthi Karapantzou1,2*, Joao Pedro Vale3, Frank Haubner4, Martin Canis5
1University ORL Department, Ludwig-Maximilians University Munich, Germany
2Interbalcan Medical Hospital, ORL Department, Thessaloniki, Greece
3Belage Clinic, Lisbon, Portugal
4University ORL Department, Ludwig-Maximilians University Munich, Germany
5University ORL Department, Ludwig-Maximilians University Munich, Germany
*Corresponding Author: Chrisanthi Karapantzou, University ORL Department, Ludwig-Maximilians University Munich, Germany.
Received: 26 January 2022; Accepted: 04 February 2022; Published: 10 February 2022
Article Information
Citation: Chrisanthi Karapantzou, Joao Pedro Vale, Frank Haubner, Martin Canis. Plasma Exeresis Technology for Rejuvenation of the Upper Eyelid. Archives of Clinical and Medical Case Reports 6 (2022): 78-90.
View / Download Pdf Share at FacebookAbstract
Background: One of the common aesthetic and functional surgical interventions is the upper eyelid blepharoplasty. It offers satisfying results, but is associated to some non-reversible complications. An non-surgical method for rejuvenation of the eyelid, is the usage of Plexr®. Based on plasma exeresis technology, it allows precise sublimation of epidermal and superficial dermal layers, without adverse events. This intrinsic plasma exeresis induces an immediate lifting effect of the treated skin.
Methods: Objective of this clinical observational study, is to assess the long-term results in a 60 patients cohort (9 male, 51 female), where bilateral plasma blepharoplasty was performed under local anesthesia, in a period of 18 months. All participants were subjected to 2 interventions with Plexr®. 32 patients were treated in the ORL Department of the Interbalcan Medical Hospital in Thessaloniki and the rest of the cohort in the ORL University Department of the LMU in Munich. They were treated by the same physician, for the same indication: upper eyelid dermatochalasis, without lipoptosis. Photographs were taken prior to each session and after the second procedure. Parameters that were evaluated, were the reduction of the flaccened eyelid skin, the duration of post-treatment oedema, the development of wound healing and pain perception. Patient satisfaction was rated at 6 months, 12 months and 18 months post- procedure.
Results: A very good general satisfaction rate with long-lasting results was reached, while no relevant adverse effects were reported. The treatment combined a quick, well tolerated procedure with a low downtime, compared to surgical blepharoplasty.
Conclusions: Plasma technology is an effective method to rejuvenate the upper eyelid and manage
Keywords
<p>Eyelids; Medical blepharoplasty; Plasma exeresis technology; Plasma skin rejuvenation</p>
Article Details
1. Introduction
Various natural intrinsic and extrinsic factors lead to skin aging, affecting the periorbital and especially the upper eyelid areas, even in younger patients. All these processes result in eyelid thinning, drooping and wrinkling. Upper blepharoplasty is for these indications a common facial aesthetic and functional surgical intervention, although the proper technique and optimal design of the excision keep remaining a point of controversial scientific discussion. The surgical procedure offers satisfying results, but is associated to some non reversible complications and prolonged recovery times, because of bruising, oedema and pain. An alternative therapeutic approach is the non surgical, medical blepharoplasty, based on the innovative method of plasma exeresis technology (Table 2). The usage of Plexr® device allows a punctual, precise sublimation of epidermal and superficial dermal layers, causing a skin retraction without the appearance of severe adverse events. Further, Plexr® facilitates the management of various dermal pathologies, through its remodeling and lifting effect in cases of skin laxity or hypertrophy (fine perioral-, neck wrinkles, cheloids, various scars). Parallel to that, it might be used as a minimal traumatic extraction tool for benign neoformations of the skin and mucosa (superficial skin neoplasms, naevi, cysts, oral fibromas) (Figure 1). The main idea behind plasma exeresis has been described analytically in literature, with emphasis on heat transfer on the treated tissue, as its most important mechanism of function [1]. This phenomenon bases on a voltage difference between the cordless Plexr® device and the subject’s skin or mucosa. A small electrical arc, a lighting of short duration, is generated when it just reaches the surface of application, from a distance of 1mm. Through this electrical signal a sublimation of the fluids contained on the superficial epidermal layer is generated, without affecting deeper layers [2]. From histopathological aspect, it has been proved, that Plexr® spots respect the basal membrane of the skin, without penetrating it [1]. Clinical studies confirm that only one month later, collagen type III is formed, supporting the structural mechanics of skin. This observation supports the fact, that plasma exeresis leads to a desired skin lifting and retraction through quick wound healing, minimizing this way the infection risk, too [3]. Testing the hypothesis, that this noninvasive technique could be used as a sufficient and safe alternative method to surgical upper blepharoplasty, in cases of moderate dermatochalasis of the eye lids is of great interest.
2. Results
A total of 60 patients with moderate upper blepharochalasis were treated using plasma exeresis technology (Plexr® device). All patients were evaluated on 3 different intervals: 6 months, 12 months, 18 months posttreatment, in order to control long-term results and subjective satisfaction, too (Figures 2,3 and 5). During the procedure pain sensation was extremely low. Minimal, tolerable discomfort was described by 60% of our patients. The majority of our subjects experienced a very brief, slight sensation of heat during the application, but the surrounding tissue was never affected. Scabs occured immediately at the treated area and lasted from 5-14 days (Figure 4). Patients were advised to apply twice a day an antibiotic creme during the first days, so we didn’t document any infection during the first days, where this might be expected. Further, they applied daily an anti-UV tinted moisturizer until the healing of the scrabs was completed and the mild skin irritation disappeared. Sun exposure without necessary protective measurements should generally be avoided for 1 month, due to skin hyperpigmentation danger. None of our patients reported any dyschromia appearance on the treated areas. Eyelid swelling was common in all patients, occurring at the end of the procedure and resolving within 3-5 days. Skin retraction could be achieved directly after each session, peaking after several days (around 14 days). We performed on the participants of this study 2 sessions with an interval of 28 days between them, in order to optimize our results, keeping in mind that after every treatment, there is estimated to get an improvement of 30%, as described in literature [1, 2]. Serious adverse events were not observed. One female patient described a possible allergic reaction to the prescribed antibiotic creme, as she developed eye redness, tearing, a burning sensation on her eyelids and an acute exacerbation of her eyelid oedema. She was supported by oral intake of 10 mg rupatadine tablets once a day for one week and applied local an aloe vera gel. All this discomfort could be controlled, without affecting the very good outcome of her blepharoplasty. Although she didn’t apply any antibiotic crème after her second session, no inflammation was reported. We measured the results of our procedures in terms of the margin-crease distance, using a millimeter ruler, in order to document its post-operative increase. The average pre-operative margin-crease distance was 1,3 mm, while the average postoperative measurement was 3,5 mm - 6 months and 3,2 mm - 18 months after. Our questionnaire revealed that 95% of the patients would undergo the non-surgical blepharoplasty again. 40% reported functional and cosmetic reasons for deciding to get Plexr®. With the assistance of this qualitative questionnaire, which was handed out 6, 12 and 18 months after completing the second Plexr® session, we were able to collect data about various parameters. First of all we investigated the extent of post-procedure pain, measured on a scale of 0 to 10 (where 0 reflected absence of pain and 10 the worst pain ever experienced). Our patient cohort reflected moderate pain with an average of 3 on the suggested scale from 0 to 10. Participants were also asked to assess their subjective satisfaction on these 3 intervals on a scale from 0% to 100% (0%=dissatisfaction, 100%=total satisfaction), resulting an average satisfaction rate of 100% in 66,6% (n=40) of the participants, 80% in 25% (n=15) participants and 60% in 8,3% (n=5) patients. In the second interval of 12 months after the second blepharoplasty, the satisfaction rate was estimated in 100% by 58,3% (n=35) subjects, 80% in 33,3% (n=20) and 50% in 8,3% (n=5) cases (Sheme 1,2). The longterm results of 18 months remained constant in comparison to the 12 months results. In the series of patient photographs taken in all of the 3 intervals of interest, there could be documented a visible, very pleasant improvement after the novel introduced blepharoplasty approach with plasma exeresis.
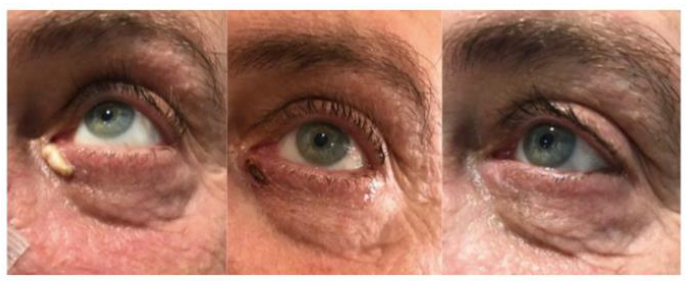
Figure 1: Xanthelasm extraction with the usage of Plexr®. (A) A preoperative photograph, (B) Photograph 5 days post-procedure, (C) Photograph 10 days post-treatment.
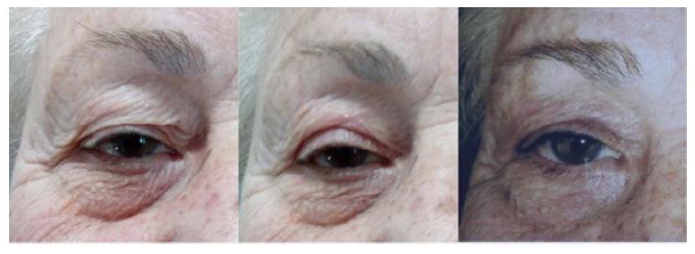
Figure 2: 82 year old patient with eyelid blepharochalasis. (A) A preoperative photograph, (B) Status 28 days post-procedure, (C) Photograph 18 months after two Plexr® sessions.
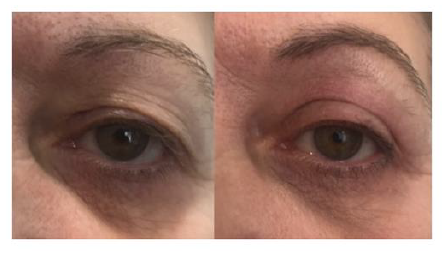
Figure 3: 65 year old patient with moderate blepharochalasis. (A) Status pre-treatment, (B) Photograph 2 months post-treatment.
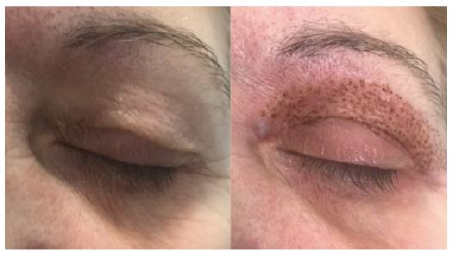
Figure 4: Patient with upper eyelid blepharochalasis. (A) Photograph prior to Plexr® blepharoplasty, (B) Scrubs, redness and dermal lifting, immediately after.
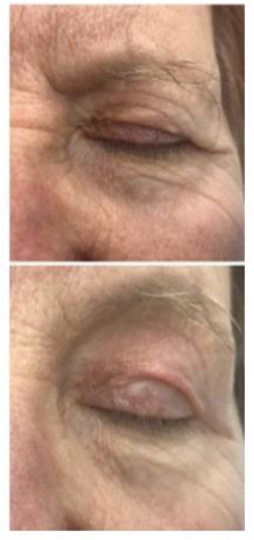
Figure 5: Results 18 months after two Plexr® sessions.
|
1. Palpebral lipoptosis |
|
2. Periocular botulinum toxin or filler injection within 6 months |
|
3. Immunsuppression |
|
4. Prior surgical eye lid procedures |
|
5. Abnormal eye lid conditions: ectropion, entropion, facial nerve palsy, eyelid dystopias |
|
6. Severe browptosis |
|
7. Infection of the eye or periorbital area |
Table 1: Exclusion criteria of plasma exeresis blepharoplasty candidates in this study.
|
Plexr Blepharoplasty |
Surgical Blepharoplasty |
|
Indication: Mild/moderate dematochalasis, without lipoptosis |
Indication: Mainly in moderate/severe dermatochalasis with & without lipoptosis |
|
Anesthesia type: Local anesthetic creme, applied 30 minutes prior to the procedure |
Anesthesia type: General/local anesthesia via injection |
|
Duration of procedure: 10-20 minutes |
Duration of procedure: 1-2 hours |
|
Recovery time: -no stitches |
Recovery time: - stitches in both lids for a week |
|
Complications: -without any major complications, |
Complications: - major complications and |
|
In moderate cases optimization of outcome after 2 - 3 sessions (the earliest 28 days after each session) possible |
Revision operation only in case of complications (rarely) needed |
|
Cost: low |
Cost: Higher than the Plexr blepharoplasty |
Table 2: Comparison of plexr blepharoplasty and surgical blepharoplasty.
Scheme 1: Clinical Investigation questionnaire after Plexr blepharoplasty
3. Clinical Investigation Questionnaire after Plexr Blepharoplasty
Personal data:
Date:
Date of PLEXR application:
Session number:
Signature:
Please respond to the following questions regarding your experience after Plasma exeresis upper blepharoplasty.
- Did you undergo the above procedure because of an aesthetic reason?
- Did you undergo the above procedure because of a functional reason?
- Did you undergo the above procedure because of both reasons (aesthetic and functional)?
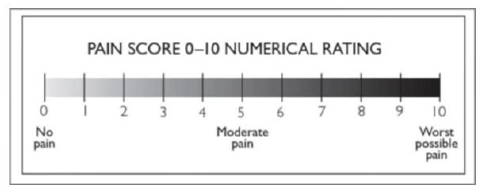
- Please mark your post-procedure (first 14 days) pain perception on the following Numerical Rating Scale.
- Did you experience any complication after the treatment? In case of positive response please Name the symptom/ problem you experienced.
- How long after the treatment dis the scabs persist?
- How long after the treatment did you experience eyelid swelling?
- How long after the treatment did you observe a skin sensitivity of the eyelid or skin persisting skin redness?
- Did you experience any remaining skin discoloration after the treatment?
- Would you undergo this specific treatment again?
- Please mark on a rating scale from 0 to 100% your subjective satisfaction rate after the procedure on the three different intervals (A,B,C)
(A) Satisfaction rate 6 months after medical blepharoplasty

(B) Satisfaction rate 12 months after medical blepharoplasty

(C) Satisfaction rate 18 months after medical blepharoplasty

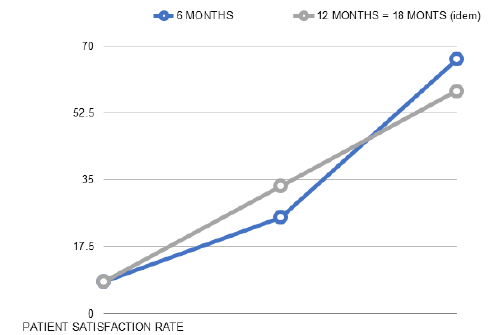
Scheme 2: Patient satisfaction rate.
4. Discussion
The functional improvement and rejuvenation of the periorbital skin laxity and the upper eyelid dermatochalasis especially, are a true challenge in choosing a proper therapeutic method for this unpleasant condition. Not only technical questions rise the difficulty of the most suitable treatment concept, but also the important anatomical position of the eyes in the center of the face. Pointing out the main indication that can be assessed with Plexr®, we can summarize the condition of moderate excess skin on upper eyelids without lipoptosis and with possible co-existing, fine peri-ocular wrinkles. Medical blepharoplasty with plasma exeresis generates a skin lifting accurately, without any bleeding, incisions or surgical sutures. This technique is associated with less pain, swelling and downtime, compared to the gold standard of surgical blepharoplasty. Potential and irreversible skin harm is avoided as it isn’t as invasive as traditional laser devices, either. Compared to the plasma exeresis technique, CO2 - Lasers, as well as fractional lasers, might cause more serious and permanent side effects when applied on the periorbital area. Such undesired situations are corneal and scleral burns, loss of vision, ectropion, scarring, infection and often hyper- or hypopigmentation [4]. When applying Plexr®, no special corneal protection special protective eye covering is needed, as during Laser-treatments. Pain perception is easily reduced by the usage of local anesthetic cremes prior to each session. Severe swelling of the eyelid is observed during the first 3-5 days. Further, the majority of our patients reported an important improvement of the sensation of heavy, droopy eyelids in the first post-procedure days, despite the swelling. Plexr® application shows promising remodeling effects and an early onset of wound healing, due to a direct affection on fibroblasts, through sublimation. The applied micro spot technique has in general the advantage of reducing the reepithelialization of treated tissue to a few days only, minimizing this way the infection risk associated to delayed epithelial healing [5]. Our patient cohort experienced a clinically improved appearance, without any serious adverse events (Fig.2, Fig.3, Fig.5). There exist only a few sources in literature referring to plasma technology for upper blepharoplasty, which include 10 to 25 participants. So an attempt of an analytic comparison to the results of other working groups is possible, but with a reference to a smaller amount of treated eyelids. Despite the number of involved patients, all other authors describe the absence of major complications, while having parallels very promising, long lasting results on the treated skin areas. The largest study so far, published by Tsioumas and his working group, was conducted over 2 years. They report about 1000 treated subjects, receiving all a medical Plexr® blepharoplasty. The excess skin sublimation was estimated in 30% in the end of each treatment. 800 amongst this study’s subjects achieved 100% of the desired result in 3 sessions and 200 patients in 2 sessions [1]. Despite the numerous participants and documented treatments, no undesirable effects were reported, proving Plexr® blepharoplasty to be a low cost, minimal invasive and safe, novel approach for blepharochalasis [1,2]. Rossi et al evaluated the clinical improvement and collagen remodeling of upper blepharochalasis after plasma exeresis. In a pilot study, they were able to document very promising effects on the upper eyelid collagen, viewed under Reflectance confocal microscopy (RCM), which is a non invasive tool for ‘’in vivo’’ dermal imaging. Based on the clinical improvement of patient’s appearance without having adverse phenomenons, they suggest plasma technology as a valid solution in the management of eyelid dermatochalasis [6]. Baroni A. and Giroux PA et al, two different working groups, published both in 2019 their experience with the usage of plasma radiofrequency ablation technology for medical blepharoplasty [7,8]. Both scientific assessments proved good tolerability for the patients, optimal cosmetic results with no major adverse events and a high patient satisfaction rate [7,8]. Our experience is associated to a high patient satisfaction rate even 18 months after the first two sessions, mild pain sensation and well tolerated post-procedure swelling. The complex structure and function of the eyelids have an existing potential for complications. Through the non invasive character of the plasma exeresis method, various phenomenons that could arise with the surgical technique like: Ecchymosis, wound dehiscence, scar abnormalities, irreversible asymmetries, overcorrections,persisting epiphora, ptosis, diplopia and ocular injury can be avoided [9].
5. Materials and Methods
Object of this clinical observational study was to assess the aesthetic and functional longterm results in a cohort of 60 patients (9 male, 51 female) with an age range from 23-86 years, where bilateral plasma blepharoplasty was performed under local anesthesia, in a time period of 18 months (Figure 2,3,5). All participants were subjected to two interventions of plasma exeresis, with a hand operated Plexr® soft surgery device, after signing an informed consent. They have been always treated by the same physician and for the same indication: moderate, functionally disturbing and aesthetic unpleasant dermatochalasis. This clinical entity creates in most subjects one or more folds of excess skin on the upper eyelid. Severe dermal elasticity loss cases, result not only a cosmetic deficit, but also a functional visual field obstruction, mainly on then lateral parts of the eye lids, especially in the elderly. Cases of palpebral lipoptosis were excluded, as this is a situation, which typically requires a surgical indication. Other exclusion criteria included periocular botulinum toxin injection or filler application within 6 months, immunosuppression, prior surgical eye lid procedures, abnormal eyelid conditions like ectropion, entropion, facial nerve palsy, eye lid dystopias, severe brow ptosis and persisting infection of the eye or surrounding skin (Table 1). Medical and ophthalmologic history including chronic systemic entities and medication were documented to ensure an optimal pre-procedure evaluation. Moreover, the quality and quantity of lax upper-eyelid skin, were always considered. All patients underwent a two session plan with Plexr®, respecting a 28 day treatment-free interval, between each application. Parameters that were evaluated, were the reduction of the flaccened eyelid skin, the duration of post-treatment edema, the development of wound healing and pain perception. Further, we evaluated the patient satisfaction rate at 6 months, 12 months and 18 months post-procedure. Plexr®, which stands for ‘’plasma exeresis’’ creates an ion- electron- rich energy (plasma), which leads to a sublimation of the epidermis. The terminus sublimation describes the physical and direct transition from solid to the gaseous state. Plasma exeresis technology is applied on previous desinfected skin with a special hand-controlled pen, that ionizes the air between its terminal needle and the tissue planned for treatment, in order to generate a radius of microplasma. The microprocessor inside the device allows the application of precise signals, reproducing exactly the amount of plasma needed to have a sublimation effect. The operation device should not contact the skin in order to produce ionization gas, otherwise the procedure will get interrupted. Therefore its tip must be held in 1 mm away from tissue, in order to generate an immediate, visible retraction. Direct improvement and shrinking of the treated area are achieved, without any bleeding or skin incision. The total amount of retracted skin is estimated to be around 30% per session [1,2]. During Plexr® blepharoplasty the doctor asks the patient to open and close the eyes, so excess skin can be identified and treated. So a series of Plexr® shots can be targeted effectively. Small scrabs result and heal within 6-14 days. Patients should always be advised to not pick or scratch on them. The level and intensity of pain experienced by the patients can be controlled, as well as their tolerability and cooperation supported, when an anesthetic creme (lidocaine/prilocaine) is applied 30 minutes prior to the procedure. In our study both eyelids were treated in one session and revised after 28 days. After the application our patients were instructed to apply twice a day and for 5 days in total, smoothly, a thin layer of an antibiotic creme. Additionally they were advised to apply on daily basis a high - 50o UV-protecting creme when going out, in order to minimize the risk of skin discoloration during recovery time and for a period of 4 weeks after each session. All subjects we included in this study returned for a 6 month-12 months-18 months evaluation. Photographs were taken in frontal projection using the same camera, lighting and positioning.
6. Conclusions
The therapeutic gold standard for upper eyelid dermatochalasis has been conventional surgical blepharoplasty since years. Lately, noninvasive procedures promise none scarring, immediate results in cases of moderate blepharochalasis, without lipoptosis. One of these approaches is the usage of plasma exeresis technology, through a Plexr® device. It induces a plasma voltaic arc, causing retraction and remodeling of the epidermis and superficial dermis [1, 2, 6]. This well tolerated method gives long-lasting results with a high satisfaction rate, low downtime and a very low complication rate. Moreover, the procedure is performed under local anesthesia in the office and outside the operating rooms. This fact is translated into lower treatment costs than in invasive blepharoplasty. Instant results control and direct lifting effect during each session, together with the possibility of verbal communication with the patient, allow the optimization of the outcome for both, patients and practicioners. In our study we evaluated 60 patients in total, who were all treated with Plexr®, for the indication of moderate skin laxity on their upper eyelids over a period of 18 months. All patients underwent two sessions, within an interval of 28 days, with the majority reporting very satisfying functional and aesthetic results.
Author Contributions
Conceptualization, C. Karapantzou and F. Haubner.; methodology C. Karapantzou; software C. Karapantzou validation C. Karapantzou; formal analysis F. Haubner; investigation C. Karapantzou; resources C. Karapantzou; data curation C. Karapantzou and F. Haubner.; writing—original draft preparation, C. Karapantzou; writing—review and editing, C. Karapantzou; visualization, F. Haubner; supervision M. Canis; project administration M. Canis; All authors have read and agreed to the published version of the manuscript.
Funding
This research received no external funding.
Institutional Review Board Statement
Ethical review and approval were given from the Ethics Commission of the Interbalcan Medical Hospital, Thessaloniki Greece. Informed Consent Statement: Informed consent was obtained from all subjects involved in the study. Written informed consent has been obtained from the patients to publish this paper.
Data Availability Statement
Data supporting reported results can be found in the patient archive of the ORL University Department LMU Munich and in the patient archive of the ORL Department of the Interbalkan Hospital in Thessaloniki Greece as the first author works in both Departments.
Conflicts of Interest
The authors declare no conflict of interest.
References
- Tsioumas G. Sotiris, Georgiadis Nikolaos, Georgiadou Irini, Plexr: The Revolution in Blepharoplasty. Pinnacle Medicine & Medical Sciences 1 (2014): 423-427.
- Sotirios TG, Natia S. Non - Invasive Blepharoplasty with Plasma Exeresis (Plexr) Pre/Post Treatments. J Aesthet Reconstr Surg 4 (2018): 6.
- Asgari M, Latifi N, Heris HK, et al. In vitro fibrillogenesis of tropocollagen type III in collagen type I affects its relative fibrillar topology and mechanics. Sci Rep 7 (2017): 1392.
- Lieberman D, Quatela V, Upper lid blepharoplasty - a current perspective; Clin Plast Surg 40 (2013): 157-165.
- Pham M. MIXTOSX, Aesthetic trends (2007): 35-37.
- Rossi E, Farnetani F, Trakatelli M, et al. Clinical and Confocal Microscopy Study of Plasma Exeresis for Nonsurgical Blepharoplasty of the Upper Eyelid: A Pilot Study, Dermatol Surg 44 (2018): 283-290,
- Baroni A. Non - surgical blepharoplasty with the novel plasma radiofrequency ablation technology, Skin Res Technol 2019.
- Giroux PA, Hersant B, SidAhmed-Mezi M, et al. The Outcomes Assessment of the Plasma Blade Technology in Upper Blepharoplasties: A Prospective Study on a Series of 25 Patients, Aesthetic Plast Surg 43 (2019): 948-955.
- Oestreicher J, Mehta S. Complications of Blepharoplasty, Prevention & Management, Plastic Surgery International 2012 (2012).


 Impact Factor: * 5.3
Impact Factor: * 5.3 Acceptance Rate: 75.63%
Acceptance Rate: 75.63%  Time to first decision: 10.4 days
Time to first decision: 10.4 days  Time from article received to acceptance: 2-3 weeks
Time from article received to acceptance: 2-3 weeks 
