Solitary Splenic Metastasis of Fallopian Tube Carcinoma: A Case Report and Review of Literature
Vittore Cereda MD, PhD1*, Giuseppina Mambella MD1, Michele Moscato MD1, Domenico Campagna MD2, Mario Rosario D’Andrea, MD1
1Clinical Oncology Unit, San Paolo Hospital, Largo Donatori del Sangue 1, 00053, Civitavecchia, Rome, Italy.
2Department of Pathology, San Giovanni-Addolorata Hospital, 00184, Rome, Italy
*Corresponding Author: Vittore Cereda, Clinical Oncology Unit, San Paolo Hospital, Largo Donatori del Sangue 1, 00053, Civitavecchia, Rome, Italy
Received: 28 February 2022; Accepted: 14 March 2022; Published: 15 April 2022
Article Information
Citation: Vittore Cereda, Giuseppina Mambella, Michele Moscato, Domenico Campagna, Mario Rosario D’Andrea. Solitary Splenic Metastasis of Fallopian Tube Carcinoma: A Case Report and Review of Literature. Archives of Clinical and Medical Case Reports 6 (2022): 271-277.
View / Download Pdf Share at FacebookAbstract
Background: Solitary parenchymal splenic metastasis is an unusual event because of its anatomical, histological and physiological features. Breast, ovary, lung, gastric, colorectal cancer and melanoma are the most common tumors from which splenic metastasis may occur and this phenomenon is usually described in disseminated cancers, with a large burden of hematogenous metastases or peritoneal spread.
Case Presentation: Here we report a case of a 71-year-old female with an isolated splenic hypodense formation localized in the lower third of the spleen with extracapsular involvement and without any other evidence of secondarisms in other organs. She then performed a splenectomy, followed by histopathological examination which showed a carcinoma with a high-grade papillary growth pattern of likely ovarian origin. Ca125 levels, a pap smear test, a transvaginal ultrasound and a PET/CT scanning were found to be normal. Only a further laparoscopic bilateral adnexectomy revealed an early high-grade serous papillary carcinoma of the left fallopian tube with intratubaric growth, infiltration of the muscle layer and absence of BRCA1/2 mutations at molecular analysis. Thereafter, an adjuvant chemotherapy and radiological controls were performed, without any proof of relapse so far.
Conclusion: The reported case is, to the best of our knowledge, the first case of a solitary splenic metastasis arising from an early primary fallopian tube cancer, with no involvement of ovaries, peritoneum and/or other organs. Given the familial history of the patient, in the near future, it would be useful to include the analysis of mutations in ovarian cancer susceptibility genes through multigene panels in order to improve cancer risk management.
Keywords
<p>Isolated splenic metastasis; Fallopian tube cancer; Synchronous metastasis; Splenectomy; Hematogenous route; Hereditary susceptibility</p>
Article Details
1. Introduction
Splenic metastases from solid tumors, defined as parenchymal lesions, are considered very unusual. Historical autopsy studies have shown that the frequencies of splenic metastases are around 2.3 to 7.1 percent, but they can’t be usable for epidemiological statements because of selection bias [1,2]. On the other hand, a very interesting splenectomy specimen study reported a lower frequency of 1.3 percent [3] and even, the data collected in 2009 at the Hospital of Schwering, in Germany, found that just 59 of 6,137 metastatic cancer patients (0.96%) had splenic metastases (0.002% of all patients with malignant tumors) [4]. In this study, it has been also reported that only three out of these 59 patients had isolated splenic metastasis, without the involvement of other tissues. Indeed, majority of the cases described in the literature is part of disseminated metastatic disease and usually arise from breast, ovary, lung, gastric, colorectal cancer and skin melanoma [5], while isolated splenic metastasis is very rare [6-8].
Fallopian tube serous carcinoma develops from the transformation of the salpingeal mucosa and it has an incidence rate of 0.36 to 0.41 per 100,000 women per year, amounting to approximately 300 to 400 annual cases [9,10]. Up until now, throughout the literature, fallopian tube carcinomas are usually incorporated under the term epithelial ovarian cancer, together with primary peritoneal carcinomas, because all these three cancers have the same clinical presentation, dissemination patterns and chemosensitivity [10]. Primary fallopian tube serous carcinomas fall into the histologic type of high grade serous carcinomas, with 95% of TP53 mutations and 40% of BRCA1/2 alterations [10].
Here we describe a rare case of solitary splenic metastasis from a fallopian tube serous carcinoma. The interesting point of our report is that metastasis to the spleen from ovarian cancer, fallopian tube cancer and primary peritoneal cancer is usually a part of peritoneal spreading with multiorgan involvement and primarily occurs years after surgery [8]. In this case, splenectomy was performed without the radiological evidence of a primary gynecological malignant tumor.
2. Case Presentation
The report was conducted in accordance with the Declaration of Helsinky and a written informed consent was provided by the patient. A 71-year-old female was first clinically assessed at the Day Hospital of the Oncology Unit of S. Paolo Hospital in Civitavecchia (Rome, Italy), after performing an abdominal B-ultrasound in order to investigate an intermittent mild pain in left upper abdomen lasting for one month. Pain was non-colicky and was not associated with vomiting, diarrhea, melena, hematemesis, hematuria or serosanguinous vaginal discharge.
She had two spontaneous vaginal deliveries and she had been post-menopausal since past 25 years. No history of alcohol intake or smoke was there. Her familial history included: 1) mother deceased at the age of 87 for a colon carcinoma; 2) one sister deceased at the age of 61 for a colon carcinoma; 3) one sister with a surgery for a rectal cancer at the age of 73 and in fair performance status; 4) one sister with a surgery for a kidney cancer at the age of 50 and in good performance status. Her comorbidities were a hypertensive left ventricular hypertrophy (H-LVH) treated with indapamid, perindopril and bisoprolol for 10 years, hypercholesterolemia treated with atorvastatin for 10 years and hypothyroidism treated with 25 mcg of levothyroxine for 20 years.
Ultrasonography of abdomen revealed a not well-defined heterogeneous hypoechoic lesion in left supra renal fossa measuring 60 × 52 × 50 mm, along with light splenomegaly. On the physical examination, the abdomen became suddenly tense and the patient reported pain at touch both superficially and more in depth, expecially in the left hypochondrium. Vitals were stable. Complete blood count, renal function test, liver function test, blood sugar and serum electrolytes revealed normal parameters. A further abdominal computed tomography (CT) scan showed a large not homogeneously hypodense formation localized in the lower third of the spleen of 60x59 mm with extracapsular involvement of 10 mm at the level of the perivisceral adipose tissue at the medial margin (Figure 1). Capsular invasion was also observed at the level of the lateral margin of the described formation which was adhered to the splenic flexure of the colon. A mild abdominal and pelvic cavity effusion was also detected. No other masses were documented in abdomen and a colonoscopy did not show any suspected neoplastic lesions.
Provisional diagnosis of splenic haemangioma was made. Once we verified that chest CT scan was normal, splenectomy was performed, followed by histopathological examination. The final pathology results revealed splenic metastasis of carcinoma with a high-grade papillary growth pattern of likely ovarian origin and immunohistochemical staining demonstrated strong positivity for p53 and Ca125 (Figure 2A-2D). The review of the histological preparation carried out at another center confirmed that the splenic lesion was a secondary localization of high-grade serous ovarian carcinoma.
At the same time, the Ca15.3 antigen level was 62 U/ml (normal up to 31 U/ml), while the Ca125, CA19-9 and CEA levels were normal. Due to the results of these examinations, the patient performed a breast ultrasound, a pap smear test and a transvaginal ultrasound which were found to be normal. Furthermore, a Positron Emission Tomography – Computed Tomography (PET/CT) Scanning did not show any abnormal metabolic activity.
In agreement with the patient and the surgeon, on the basis of the histological result of the splenectomy, she underwent a laparoscopic bilateral salpingo-oophorecotmy surgery which revealed a high-grade serous papillary carcinoma of the left fallopian tube with a maximum diameter of 5 mm, intratubaric growth and infiltration of the muscle layer. The ovaries, right fallopian tube and peritoneal washing fluid were free of tumor cells. Further molecular analysis on the carcinoma did not show BRCA1/2 mutations.
After 3 weeks Ca 15.3 dropped from 62 U/ml to 29 U/ml. The patient was diagnosed with splenic metastasis of primary fallopian tube carcinoma and received chemotherapy with paclitaxel (175 mg/m2) and carboplatin (AUC 5) for 5 cycles (last cycle was not administered because of prolonged urinary infection, associated with hepatotoxicity (alanine aminotransferase” [ALT] 63 U/l, aspartate aminotransferase [AST] 102 U/l), and severe pain of the lower extremities due to worsening of a coxofemoral arthrosis). She performed a further PET scanning which just showed an aspecific increase in metabolic activity affecting the coxofemoral and glenohumeral joints and as suggested from our surgeon, she completed surgical procedures with a laparoscopic hysterectomy and total omentectomy. Histopathological examination of this surgery did not reveal the presence of tumor cells. Currently, Ca 15.3 is still normal and the patient is carefully monitored with follow-up visits and radiological controls.
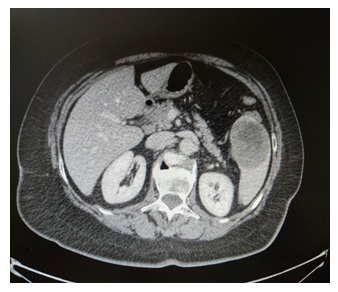
Figure 1: Abdominal computed tomography (CT). CT scan shows a large not homogeneously hypodense formation localized in the lower third of the spleen of 60x59 mm with extracapsular involvement at the medial margin
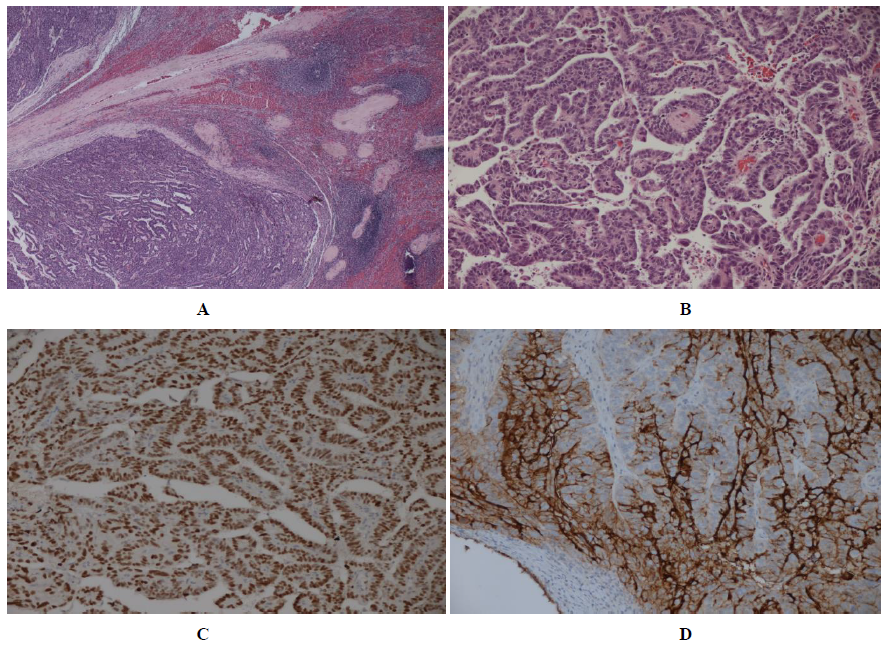
Figure 2: Histopathology and immunohistochemistry of splenic parenchyma. A: Hematoxylin and eosin stained section shows malignant carcinoma (left side) infiltrating into the splenic parenchyma (right side) (x 2.5 magnification); B: Hematoxylin and eosin stained section shows high pleomorphism of malignant cells (x 10 magnification); C:Section shows strong nuclear positivity of p53, suggesting a high proliferative index and accumulation of aberrant p53 (x 10 magnification); D:Ca-125 overexpression is detected on the membrane of carcinoma cells infiltrating the spleen ( x 10 magnification).
3. Discussion
In our view, interesting points of this case report are: 1) The spleen metastasis is isolated (rare event) and synchronous (most of them are metachronous) to a high-grade serous fallopian tube carcinoma; 2) The primary fallopian tube carcinoma was detected just after surgery and was an early-stage serous carcinoma (FIGO IA); 3) Familial history of our patients consisted of many cases of colon adenocarcinoma, suggesting a hereditary susceptibility involving genetic abnormalities, including several suppressor genes and oncogenes, such as the mismatch repair (MMR) genes, the tumor suppressor gene TP53, and several other genes involved in the double-strand breaks repair system, CHEK2, RAD51, BRIP1, and PALB2.
Splenic metastasis usually develops from breast, ovary, lung, gastric, colorectal cancer and melanoma, is mostly asymptomatic and its diagnosis is based on imaging studies [5]. It’s an unusual event because of the presence of sharp angle between the splenic artery and celiac axis [11], of the physiological rhythmic contraction of the spleen [12] and of the splenic microenvironment enriched by humoral factors and immune cells [13]. In our case, CA-125 was not increased and CT scan and PET/CT did not reveal any sign of ovarian origin. Only the histopathological examination of splenectomy favored the provisional diagnosis of primary serous gynecologic malignancy, which was further confirmed by laparoscopic bilateral adnexectomy surgery. Most of cases involving splenic metastases originates from a high burden metastastic disease through three possible routes: haematological, lymphatic (just capsular and subcapsular splenic metastases) and transcoelomic [14]. In this case, it’s not very likely that parenchymal splenic metastasis came from transcaelomic route because peritoneal spread of the disease was absent. Moreover, splenic parenchyma lacks afferent lymphatic vessels and this anatomical feature could exclude the lymphatic route from possible origins of the metastasis. This secondarism was located at the lower third of the spleen with extracapsular and perivisceral fat tissue involvement. Therefore, we may assume that the fallopian tube carcinoma metastasized from hematogenous route, even if other metastatic sites (liver, lung) were not detected.
Fallopian tube serous carcinoma is a rare disease and accounts for approximately 0.14-1.8% of female genital malignancies [10]. In the last 5 years, several studies demonstrated that precursors of ovarian cancer develop in the fimbria from occult serous tubal intraepithelial carcinoma (STIC), and only subsequently they involve the ovary [15]. This hypothesis suggests that the incidence of fallopian tube cancers may have been underestimated and explains why clinical behavior, response to surgery and chemosensitivity are similar between fallopian tube carcinoma and ovarian cancer. More than one-fifth of ovarian tumors, including fallopian tube cancers, have hereditary susceptibility, and in about 60% of cases the genetic abnormality is a germline mutation in BRCA genes [10]. In our case, the primary fallopian tube serous carcinoma did not have BRCA1/2 mutations. Nevertheless, several other suppressor genes and oncogenes have been associated with hereditary ovarian cancers [16]. In our opinion, the colon cancer familial history of our patient may suggest us an alternative mechanism of hereditary ovarian carcinogenesis, including defects in mismatch repair (MMR) genes, TP53, and several genes involved in double-strand breaks repair such as ATM, CHEK2, RAD51, BRIP1, and PALB2. In the near future, the analysis of mutations in ovarian cancer susceptibility genes, other than BRCA1/2, through multigene panels may result in more personalized cancer risk management with tailored clinical and radiological surveillance, or prophylactic surgeries.
4. Conclusion
In this report, we presented the first case of a solitary splenic metastasis originating from a very early (5 mm) primary fallopian tube cancer. Due to the rarity of this cancer, certainty of diagnosis was achieved just after a salpingo-oophorecotmy surgery, showing a small intratubaric serous carcinoma. Interesting points of discussion are the possible routes of this splenic metastasis, given the absence of other sites of spread; and the need of a multigene panel in order to analyze mutations in ovarian cancer susceptibility genes, given the familial history of the patient.
References
- Berge, T. Splenic metastases. Frequencies and patterns. Acta Pathol. Microbiol. Scand. A 82 (1974): 499-506.
- Lam, K.Y., Tang, V. Metastatic tumors to the spleen: A 25-year clinicopathologic study. Arch. Pathol. Lab. Med. 124 (2000): 526-530.
- Kraus MD, Fleming MD, Vonderheide RH. The spleen as a diagnostic specimen: a review of 10 years’ experience at two tertiary care institutions. Cancer 91 (2001): 2001-9.
- Sauer J, Sobolewski K, Dommisch K. Splenic metastases-not a frequent problem, but an underestimate location of metastases: epidemiology and course. J Vancer Res Clin Oncol 135 (2009): 667-671.
- Comperat E, Bardier-Dupas A, Camparo P, Capron F, Charlotte F. Splenic metastases:clinicopathologic presentation, differential diagnosis, and pathogenesis. Arch Pathol Lab Med 131 (2007): 965-969.
- Aijaz M, Hasan M, Alam F. Isolated splenic metastasis: an unususl presentation of colonic adenocarcinoma. Arch Clin Gastroenterol 5 (2019): 27-30.
- Karni D, Kopelman D, Abu Hatoum O. Solitary splenic metastasis of ovarian carcinoma: a case report. J Med Case Rep 17 (2014): 154.
- Lv M, Li Y, Luo C, Liu P, Yang J. Splenic metastasis of ovarian clear cell adenocarcinoma: a case report and review of the literature. Exp Ther Med 7 (2014): 982-986.
- Rexhepi M, Trajkovska E, Ismaili H, Besimi F, Rufati N. Primary fallopian tube carcinoma: a case report and literature review. Open Acces Maced J Med Sci 5 (2017): 344-348.
- Stasenko M, Filipova O, Tew WP. Fallopian Tube Carcinoma. J Oncol Pract 15 (2019): 375-382.
- Sappington SW. Carcinoma of the spleen: its microscopic frequency: a possible etiologic factor. JAMA 78 (1922): 953-955.
- Kettle EH. Carcinomatous metastases in the spleen. J Pathol Bacteriol 17 (1912): 40-46.
- Klein B, Stein M, Kuten A, Steiner M, Barshalom D, et al. Splenomegaly and solitary spleen metastasis in solid tumors. Cancer 60 (1987): 100-102.
- Sugarbaker PH, Hoskins ER. Splenic metastases-hematogenous disease or invasive peritoneal implants? Case reports of two patients. Int J Surg Case Rep 72 (2020): 266-270.
- Labidi-Galy SI, Papp E, Hallberg D, Niknafs N, Adleff V, et al. High grade srous ovarian carcinomas originate in the fallopian tube. Nat Commun 8 (2017): 1093.
- Nielsen FC, van Overeem Hansen T, Sorensen CS. Hereditary brest and ovarian cancer: new genes in confined pathways. Nat Rev Cancer 16 (2016): 599-612.


 Impact Factor: * 5.3
Impact Factor: * 5.3 Acceptance Rate: 75.63%
Acceptance Rate: 75.63%  Time to first decision: 10.4 days
Time to first decision: 10.4 days  Time from article received to acceptance: 2-3 weeks
Time from article received to acceptance: 2-3 weeks 
