Stent Placement in the Hepatic Artery with Anatomical Variant for Treatment of A Massive Ulcer Bleeding
Van Dijk B MD1*, de Vos tot Nederveen Cappel WH MD PhD1, van Hasselt BAAM MD2, van Westreenen HL MD PhD3, Nieuwenhuijs VB MD PhD3
1Gastroenterology and Hepatology at Isala Hospital, Zwolle, The Netherlands
2Interventional radiology at Isala Hospital, Zwolle, The Netherlands
3Abdominal surgery at Isala Hospital, Zwolle, The Netherlands
*Corresponding Author: Van Dijk B, Gastroenterology and Hepatology at Isala Hospital, Zwolle, The Netherlands
Received: 25 August 2021; Accepted: 20 September 2021; Published: 21 October 2021
Article Information
Citation: Van Dijk B, de Vos tot Nederveen Cappel WH, van Hasselt BAAM, van Westreenen HL, Nieuwenhuijs VB. Stent Placement in the Hepatic Artery with Anatomical Variant for Treatment of A Massive Ulcer Bleeding. Archives of Clinical and Medical Case Reports 5 (2021): 721-723.
View / Download Pdf Share at FacebookAbstract
A 54-year-old man, presented with melaena after a recent bowel perforation resulting in sigmoid resection. The gastroduodenoscopy showed a large clot and active bleeding in the postpyloric duodenum without the opportunity of obtaining endoscopic hemostasis. A diagnostic angiography was attempted, but no blush was seen. The next day radiologic coiling took place. Unfortunately long term hemostasis was not achieved. A second gastroscopy was performed and a postpyloric ulcer with a large pulsating blood vessel was seen. Hemostasis was attempted by both endoscopic clipping and radiological coiling of the target vessels. An angiography with coiling was attempted. It was technically impossible to coil all the vessels due to an anatomic variation. In order to prevent to sacrify the hepatic artery by coiling the entire hepatic artery, we successfully tried a unique approach to place a radiologic covered stent in the common hepatic artery to cover the origin of the gastroduodenal artery.
Keywords
<p>Hemorrhage; Vascular malformations; Artery; Gastrointestinal; Arterial intervention; Radioembolization; Stenting; Stent graft</p>
Article Details
1. Case Report
A 54-year-old man, presented with melaena after a recent scrotal hernia correction complicated by bowel perforation resulting in sigmoid resection. The gastroduodenoscopy showed a large clot and active bleeding in the postpyloric duodenum without the opportunity of obtaining endoscopic hemostasis.
A CT-angiography was performed and demonstrated a blush into the duodenum. A diagnostic angiography was attempted, but no blush was seen. The next day, the patient was hypotensive and radiologic coiling took place. Unfortunately long term hemostasis was not achieved; fluid resuscitation and blood transfusions were needed to stabilize the patient. A second gastroscopy was performed and a postpyloric ulcer with a large pulsating blood vessel was seen. Endoscopic treatment with adrenaline and the goldprobe was performed, which provoked recurrent bleeding. Hemostasis was attempted by both endoscopic clipping and radiological coiling of the target vessels.
An angiography with coiling was attempted. It was technically impossible to coil all the vessels due to an anatomic variation (shown in figure 1). The short origin of the gastroduodenal artery arose from the common hepatic artery which was displaced to the superior mesenteric artery. In order to prevent to sacrify the hepatic artery by coiling the entire hepatic artery, we successfully tried a unique approach to place a radiologic covered stent (Gore Viabahn 8 × 50 mm, shown in Figure 2) in the common hepatic artery to cover the origin of the gastroduodenal artery. Eight weeks later an outpatient gastroscopy showed a healed ulcer.
Stenting is not the initial therapy, but should be considered if endoscopic treatment or coiling cannot arrest the bleeding and surgery is detrimental.
References
None.
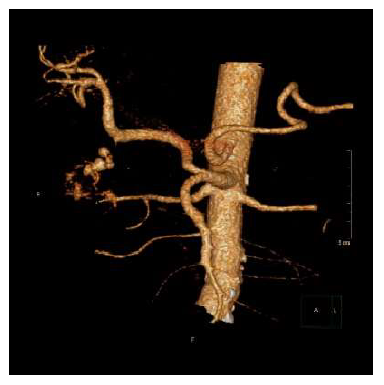
Figure 1: 3D reconstruction of the anatomical variation of the vascular supply.
1 Truncus coelicus; 2 Superior mesenteric artery; 3 Common hepatic artery; 4 Right renal artery
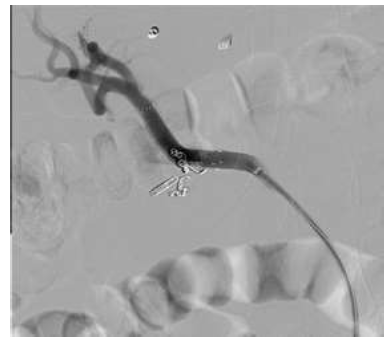
Figure 2: Hemostasis achieved with the Covered stent (Gore Viabahn, 8 × 50 mm).


 Impact Factor: * 5.3
Impact Factor: * 5.3 Acceptance Rate: 75.63%
Acceptance Rate: 75.63%  Time to first decision: 10.4 days
Time to first decision: 10.4 days  Time from article received to acceptance: 2-3 weeks
Time from article received to acceptance: 2-3 weeks 
