Successful Endoscopic Management of Obstructive Jaundice in Von Hippel-Lindau Disease Caused by Multiple Pancreatic Serous Cystadenomas’ Extrinsic Compression - A Case Report
Hunter Benvenuti MD1, Mandeep Singh MD2, Amir H Fathi MD, FACS1*
1Department of Surgery, University of California San Francisco (UCSF), Fresno Medical Education program, Fresno, CA, USA
2Advanced Gastroenterology and Hepatology Associates, Fresno, CA, USA
*Corresponding Author: Dr. Amir H Fathi, Assistant Clinical Professor of Surgery, Department of Surgery, University of California, San Francisco, Fresno Medical Education Program, 2335 E. Kashian Lane, Suite 220, Fresno, CA 93701, USA
Received: 03 March 2020; Accepted: 16 March 2020; Published: 03 April 2020
Article Information
Citation: Hunter Benvenuti, Mandeep Singh, Amir H Fathi. Successful Endoscopic Management of Obstructive Jaundice in Von Hippel-Lindau Disease Caused by Multiple Pancreatic Serous Cystadenomas’ Extrinsic Compression - A Case Report. Archives of Clinical and Medical Case Reports 4 (2020): 280-284.
View / Download Pdf Share at FacebookAbstract
Serous cystadenomas of the pancreas are a common entity in patients with von Hippel-Lindau (vHL) disease. However, to date, only thirteen cases of pancreatic cystic lesions causing obstructive jaundice in vHL patients have been reported in the literature, and these were the result of distal CBD stricture. In this study, we present a rare first case report of multiple large pancreatic serous cystadenomas causing obstructive jaundice via extrinsic compression of the mid CBD in a 27-year-old female with vHL. Biliary decompression has been successfully achieved with ERCP and stent placement, with serial stent exchanges every 2 months. Given the patient’s young age and the morbidity associated with total pancreatectomy, we have elected to pursue a more conservative approach to her biliary obstruction via serial stent exchanges until they are no longer successful at achieving decompression, at which point we will proceed with surgical intervention such as biliary bypass or total pancreatectomy.
Keywords
Multiple Pancreatic Serous Cystadenomas; Pancreatic cystic lesions
Multiple Pancreatic Serous Cystadenomas articles, Pancreatic cystic lesions articles
Multiple Pancreatic Serous Cystadenomas articles Multiple Pancreatic Serous Cystadenomas Research articles Multiple Pancreatic Serous Cystadenomas review articles Multiple Pancreatic Serous Cystadenomas PubMed articles Multiple Pancreatic Serous Cystadenomas PubMed Central articles Multiple Pancreatic Serous Cystadenomas 2023 articles Multiple Pancreatic Serous Cystadenomas 2024 articles Multiple Pancreatic Serous Cystadenomas Scopus articles Multiple Pancreatic Serous Cystadenomas impact factor journals Multiple Pancreatic Serous Cystadenomas Scopus journals Multiple Pancreatic Serous Cystadenomas PubMed journals Multiple Pancreatic Serous Cystadenomas medical journals Multiple Pancreatic Serous Cystadenomas free journals Multiple Pancreatic Serous Cystadenomas best journals Multiple Pancreatic Serous Cystadenomas top journals Multiple Pancreatic Serous Cystadenomas free medical journals Multiple Pancreatic Serous Cystadenomas famous journals Multiple Pancreatic Serous Cystadenomas Google Scholar indexed journals Pancreatic Serous Cystadenomas articles Pancreatic Serous Cystadenomas Research articles Pancreatic Serous Cystadenomas review articles Pancreatic Serous Cystadenomas PubMed articles Pancreatic Serous Cystadenomas PubMed Central articles Pancreatic Serous Cystadenomas 2023 articles Pancreatic Serous Cystadenomas 2024 articles Pancreatic Serous Cystadenomas Scopus articles Pancreatic Serous Cystadenomas impact factor journals Pancreatic Serous Cystadenomas Scopus journals Pancreatic Serous Cystadenomas PubMed journals Pancreatic Serous Cystadenomas medical journals Pancreatic Serous Cystadenomas free journals Pancreatic Serous Cystadenomas best journals Pancreatic Serous Cystadenomas top journals Pancreatic Serous Cystadenomas free medical journals Pancreatic Serous Cystadenomas famous journals Pancreatic Serous Cystadenomas Google Scholar indexed journals Cystadenomas articles Cystadenomas Research articles Cystadenomas review articles Cystadenomas PubMed articles Cystadenomas PubMed Central articles Cystadenomas 2023 articles Cystadenomas 2024 articles Cystadenomas Scopus articles Cystadenomas impact factor journals Cystadenomas Scopus journals Cystadenomas PubMed journals Cystadenomas medical journals Cystadenomas free journals Cystadenomas best journals Cystadenomas top journals Cystadenomas free medical journals Cystadenomas famous journals Cystadenomas Google Scholar indexed journals Pancreatic cystic lesions articles Pancreatic cystic lesions Research articles Pancreatic cystic lesions review articles Pancreatic cystic lesions PubMed articles Pancreatic cystic lesions PubMed Central articles Pancreatic cystic lesions 2023 articles Pancreatic cystic lesions 2024 articles Pancreatic cystic lesions Scopus articles Pancreatic cystic lesions impact factor journals Pancreatic cystic lesions Scopus journals Pancreatic cystic lesions PubMed journals Pancreatic cystic lesions medical journals Pancreatic cystic lesions free journals Pancreatic cystic lesions best journals Pancreatic cystic lesions top journals Pancreatic cystic lesions free medical journals Pancreatic cystic lesions famous journals Pancreatic cystic lesions Google Scholar indexed journals Pancreatic articles Pancreatic Research articles Pancreatic review articles Pancreatic PubMed articles Pancreatic PubMed Central articles Pancreatic 2023 articles Pancreatic 2024 articles Pancreatic Scopus articles Pancreatic impact factor journals Pancreatic Scopus journals Pancreatic PubMed journals Pancreatic medical journals Pancreatic free journals Pancreatic best journals Pancreatic top journals Pancreatic free medical journals Pancreatic famous journals Pancreatic Google Scholar indexed journals treatment articles treatment Research articles treatment review articles treatment PubMed articles treatment PubMed Central articles treatment 2023 articles treatment 2024 articles treatment Scopus articles treatment impact factor journals treatment Scopus journals treatment PubMed journals treatment medical journals treatment free journals treatment best journals treatment top journals treatment free medical journals treatment famous journals treatment Google Scholar indexed journals cancer articles cancer Research articles cancer review articles cancer PubMed articles cancer PubMed Central articles cancer 2023 articles cancer 2024 articles cancer Scopus articles cancer impact factor journals cancer Scopus journals cancer PubMed journals cancer medical journals cancer free journals cancer best journals cancer top journals cancer free medical journals cancer famous journals cancer Google Scholar indexed journals Von Hippel Lindau articles Von Hippel Lindau Research articles Von Hippel Lindau review articles Von Hippel Lindau PubMed articles Von Hippel Lindau PubMed Central articles Von Hippel Lindau 2023 articles Von Hippel Lindau 2024 articles Von Hippel Lindau Scopus articles Von Hippel Lindau impact factor journals Von Hippel Lindau Scopus journals Von Hippel Lindau PubMed journals Von Hippel Lindau medical journals Von Hippel Lindau free journals Von Hippel Lindau best journals Von Hippel Lindau top journals Von Hippel Lindau free medical journals Von Hippel Lindau famous journals Von Hippel Lindau Google Scholar indexed journals pancreatectomy articles pancreatectomy Research articles pancreatectomy review articles pancreatectomy PubMed articles pancreatectomy PubMed Central articles pancreatectomy 2023 articles pancreatectomy 2024 articles pancreatectomy Scopus articles pancreatectomy impact factor journals pancreatectomy Scopus journals pancreatectomy PubMed journals pancreatectomy medical journals pancreatectomy free journals pancreatectomy best journals pancreatectomy top journals pancreatectomy free medical journals pancreatectomy famous journals pancreatectomy Google Scholar indexed journals Surgery articles Surgery Research articles Surgery review articles Surgery PubMed articles Surgery PubMed Central articles Surgery 2023 articles Surgery 2024 articles Surgery Scopus articles Surgery impact factor journals Surgery Scopus journals Surgery PubMed journals Surgery medical journals Surgery free journals Surgery best journals Surgery top journals Surgery free medical journals Surgery famous journals Surgery Google Scholar indexed journals
Article Details
1. Introduction
Von Hippel Lindau (vHL) disease is an autosomal dominant inherited disorder characterized by the mutation in the VHL gene, which results in the formation of multiple tumors and cysts throughout the body, notably the brain, kidneys, and pancreas. The range of manifestations of vHL disease is extensive. About 40 different lesions in 14 different organs have been described. These include retinal and central nervous system (CNS) hemangioblastomas, endolymphatic sac tumors, renal cysts and tumors, pancreatic cysts and tumors, pheochromocytomas, and epididymal cystadenomas [1]. Over 70% of patients with vHL have a propensity to develop multiple pancreatic cysts2. Obstructive jaundice has been reported in association with vHL as a result of either extrinsic compression of the distal CBD or inflammatory stricture. Attempting conservative management for these cysts via biliary decompression with stents has been described as the standard of care, as these lesions have no malignant potential, and biliary bypass and total pancreatectomy carry considerable degrees of morbidity and mortality. Thus, here we present a case report of the conservative management of a mid CBD stricture due to extrinsic compression from large pancreatic serous cystadenomas in a patient with vHL.
2. Case Presentation
A 27-year-old female was referred to the HPB (Hepato- Pancreatico-Biliary) surgery service at our tertiary referral hospital, Community Regional Medical Center (CRMC) in Fresno, CA, for evaluation of symptomatic cholelithiasis. Subsequently, she was admitted with nausea, vomiting and oral intake intolerance. Detailed history and physical examination revealed, history of diabetes, obesity, depression and intermittent post-prandial nausea and vomiting, worse with greasy foods. On laboratory workup, she had a mild elevation in transaminases and mild leukocytosis, and normal total bilirubin and lipase. On US abdomen imaging, she had possible small gallstones, normal gallbladder wall, and CBD dilation to 12.9 mm. On HIDA imaging, she had decreased gallbladder ejection fraction of 15%, consistent with biliary dyskinesia.
Further work-up including abdominal imaging which revealed bilateral kidney masses. These masses were biopsied by interventional radiology, revealing bilateral renal cell carcinomas (RCC). Imaging also showed multiple pancreatic serous cystadenomas throughout the entire gland. The pattern of distribution was very suggestive of vHL disease (Figure 1). Laboratory work up included tumor markers to rule out pancreatic malignancies were all negative including Chromogranin A and CA 19-9. Renal biopsy samples were further analyzed by Foundation One CDx, next generation genomic sequencing (Foundation Medicine) revealing vHL disease. This finding prompted further testing including brain MRI which was negative for central nervous system (CNS) hemangioblastomas or endolymphatic sac tumors.
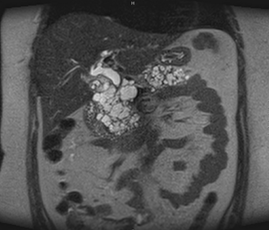
Figure 1: MRCP with biliary ductal dilatation and multiple pancreatic serous cystadenomas.
Based on her significant symptomatology, she underwent laparoscopic cholecystectomy with intraoperative ultrasound, revealing near-complete replacement of the pancreatic parenchyma with cysts. She tolerated the procedure well and was discharge home post-operatively. She is also status post robotic partial nephrectomy to address her RCCs.
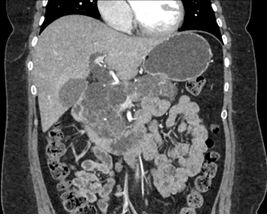
Figure 2: CT scan with proximal CBD dilation due to mid CBD compression by large pancreatic cysts.
Four months later, she re-presented to CRMC for evaluation of obstructive jaundice. She complained of severe epigastric abdominal pain radiating to her back, as well as acholic stools. On laboratory workup, she had elevated transaminases and a total bilirubin of 2.4 (direct 1.7), with a normal lipase. On CT imaging, she was found to have a dilated proximal CBD to 16 mm likely due to extrinsic compression of a short-segment mid CBD by innumerable large pancreatic cysts (Figure 2). She underwent endoscopic retrograde cholangiopancreatography (ERCP) with sphincterotomy and 6-French plastic stent placement by GI. She tolerated the procedure well and was discharge home after normalization of her LFTs and resolution of symptoms (Figure 3).
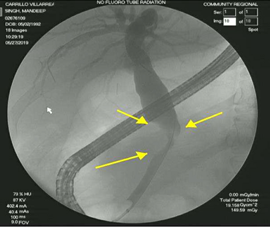
Figure 3: Initial ERCP with stenting of mid CBD stricture.
Since that time, the patient has undergone serial ERCPs every 2 months, with removal and replacement of the temporary biliary stents. Her symptoms of biliary obstruction have resolved with this conservative management. However, the mid CBD stricture has persisted despite repeated stent placements (Figure 4).
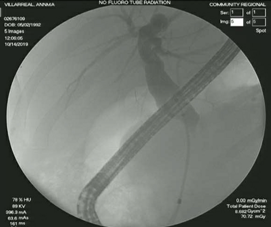
Figure 4: 6-month follow up of ERCP with stent exchange.
3. Discussion
Cystic lesions of the pancreas carry no malignant potential in vHL, and as a result, these patients do not require operative resection unless they develop biliary obstructive symptoms that cannot be managed via endoscopic stent placement [2, 3]. While there have only been thirteen cases of obstructive jaundice developing in vHL patients as a result of extrinsic distal biliary compression by pancreatic cysts, to date, this is the first report of mid biliary compression by pancreatic cysts [4-10].
This patient serves as a successful example of management of biliary obstruction in vHL disease by endoscopic decompression, sphincterotomy and stent placement with serial stent exchanges. This approach is especially beneficial in younger patients, as the morbidity and mortality associated with surgical biliary bypass or total pancreatectomy have the potential to severely limit the longevity and quality of life in these populations [11]. Furthermore, given the advances in endoscopic interventions as well as surveillance modalities for potential malignancy, conservative management in these cases constitutes a safe and effective plan of care. Thus, we present a rare case report of multiple serous cystadenomas of the pancreas causing mid CBD obstruction with jaundice in a vHL patient, which has been successfully managed with endoscopic decompression with stenting.
Conflict of Interest Statement
Authors do not have any conflict of interest “None Declared” in this research.
Author Contribution Statement
All authors contributed to the conception, design, or data analysis of this work; contributed to drafting or critical revision of the intellectual content of this work; and give final approval of the version to be published. All authors agree to be accountable for this work.
References
- Melmon KL, Rosen SW. Lindau's Disease. Review of the Literature and Study of a Large Kindred. Am J Med 36 (1964): 595-617.
- Hammel PR, Vilgrain V, Terris B, et al. Pancreatic involvement in von Hippel-Lindau disease. The Groupe Francophone d'Etude de la Maladie de von Hippel-Lindau. Gastroenterol 119 (2000): 1087-1095.
- Charlesworth M, Verbeke CS, Falk GA, et al. Pancreatic lesions in von Hippel-Lindau disease? A systematic review and meta-synthesis of the literature. J Gastrointest Surg 16 (2012): 1422-1428.
- Beerman MH, Fromkes JJ, Carey LC, et al. Pancreatic cystadenoma in Von Hippel-Lindau disease: an unusual cause of pancreatic and common bile duct obstruction. J Clin Gastroenterol 4 (1982): 537-540.
- Boujaoude J, Samaha E, Honein K, et al. A benign cause of obstructive jaundice with von Hippel-Lindau disease. A case report and review of the literature. JOP 8 (2007): 790-794.
- Cheng TY, Su CH, Shyr YM, et al. Management of pancreatic lesions in von Hippel-Lindau disease. World J Surg 21 (1997): 307-312.
- Deboever G, Dewulf P, Maertens J. Common bile duct obstruction due to pancreatic involvement in the von Hippel-Lindau syndrome. Am J Gastroenterol 87 (1992): 1866-1868.
- Fellows IW, Leach IH, Smith PG, et al. Carcinoid tumour of the common bile duct--a novel complication of von Hippel-Lindau syndrome. Gut 31 (1990): 728-729.
- Gallego Sanchez JA, Pereira Arias JG, Larrinaga Simon J, et al. Renal carcinoma and von Hippel-Lindau disease. Actas Urol Esp 22 (1998): 428-430.
- Issar SK, Kumar N, Sachdeva AK, et al. von Hippel Lindau syndrome presenting as obstructive jaundice with involvement of pancreas in two siblings. T Trop Gastroenterol 17 (1996): 30-32.
- Zakaria HM, Stauffer JA, Massimo R, et al. Total pancreatectomy: Short- and long-term outcomes at a high-volume pancreas center. World J Gastrointest Surg 8 (2016): 634-642.


 Impact Factor: * 5.3
Impact Factor: * 5.3 Acceptance Rate: 75.63%
Acceptance Rate: 75.63%  Time to first decision: 10.4 days
Time to first decision: 10.4 days  Time from article received to acceptance: 2-3 weeks
Time from article received to acceptance: 2-3 weeks 
