Would You Trust a Diagnostic Procedure with 100% Specificity and 96% Sensitivity?
Lisa Van den Eeckhaut*, Jean-Claude Lemper, Sonja Rebel, Michiel Schils, Kurt Barbé, Denis Pierard, Raphael Amstutz, Ingo Beyer
Universitair Ziekenhuis Brussel, Belgium
*Corresponding Author: Dr. Lisa Van den Eeckhaut, Universitair Ziekenhuis Brussel, Belgium
Received: 08 August 2020; Accepted: 25 August 2020; Published: 18 September 2020
Article Information
Citation: Lisa Van den Eeckhaut, Jean-Claude Lemper, Sonja Rebel, Michiel Schils, Kurt Barbé, Denis Pierard, Raphael Amstutz, Ingo Beyer. Would You Trust a Diagnostic Procedure with 100% Specificity and 96% Sensitivity?. Archives of Clinical and Medical Case Reports 4 (2020): 920-923.
View / Download Pdf Share at FacebookAbstract
Nasopharyngeal swab (NPS) RT-PCR SARS-CoV-2 detection has approximately 100% specificity and 70% sensitivity. We report a case of a 94-year-old patient without significant comorbidities, who developed respiratory symptoms 7 days after being transferred for wrist-fracture rehabilitation. NPS RT-PCR for SARS-CoV-2 was negative on day 1, 7, 12 and 19 after symptom onset. No other viral or bacterial pathogens were detected, nor was there improvement with different empirical antibiotics. CT showed non-specific five-lobe involvement. She slowly recovered clinically and radiologically. SARS-CoV-2 antibody testing became available in Belgium, revealing specific IgG in this patient. Despite serial testing and a cumulative sensitivity of 96%, COVID-19 could not be detected through NPS. This underlines the precaution that should be taken in interpreting a negative test result when the clinical suspicion is high, as well as the need for detailed information about pre- and post-test probabilities in different settings.
Keywords
<p>COVID-19; Geriatric medicine; SARS-CoV-2 RT-PCR; SARS-CoV-2 IgG; SARS-CoV-2 antibodies; Test performance: Test accuracy</p> <gdiv></gdiv>
Article Details
1. Introduction
A confirmed diagnosis of active COVID-19 requires the detection of SARS-CoV-2 by RT-PCR, usually from a respiratory tract sample, most often obtained by a nasopharyngeal swab (NPS). No cross-reaction with other coronaviruses has been observed, allowing for almost 100% specificity [1]. The sensitivity of this test in symptomatic patients has been estimated at 70% [2]. Lately, there has been a rising concern about false negative test results in clinically suspect patients. To overcome this limited sensitivity, it is suggested to perform repeated testing [3]. Here we report on a symptomatic geriatric patient with four consecutive negative swabs.
2. Case Report
A 94-year-old woman was transferred to our rehabilitation facility after having spent 33 days in the Geriatric Department of a General Hospital for a wrist fracture. Her living independently at home was compromised by recurrent falls and cognitive deterioration. Significant prior history included only a right knee prosthesis and osteoporosis. She took no medication. Physical examination revealed a cognitive deficit (MMSE 19/30) and a plaster on her right wrist. Laboratory findings showed slightly increased white blood cells (WBC) and neutrophil count, and normal C-reactive protein (CRP).
Six days later the patient presented with dyspnea on exertion and cough, but no fever and normal oxygen saturation (SaO2). Lung auscultation was normal. As other COVID-19 cases had been confirmed on the ward a NPS was taken, but RT-PCR was negative for SARS-CoV-2. The patient remained clinically stable over the next days.
On day 7 after symptom onset temperature rose to 37.6°C, SaO2 was 89% and crackles were heard over the left lung. WBC were normal with slight lymphopenia, CRP elevated (46 mg/L) and chest X-ray (CXR) revealed a beginning pneumonia in the left lower lobe. A second SARS-CoV-2 RT-PCR was negative. Tests for influenza A and B and RSV were negative, sputum could not be obtained, blood cultures and Mycoplasma and Chlamydia pneumoniae were negative. Treatment with amoxicillin/clavulanate was initiated and shifted to piperacillin/tazobactam after 5 days for persistent fever and desaturation. A third RT-PCR performed on day 12 was negative.
An ACP code had been agreed upon with the family excluding CPR and ICU. However, in the absence of clinical improvement despite adding clarithromycin, and with a new CXR revealing increased left lower quadrant opacity (Figure 1), the patient was transferred for chest computed tomography (CT) on day 19. CT showed non-specific involvement of all five lobes and a fourth NPS was negative.
Over the next weeks the patient slowly recovered clinically and radiologically and was transferred to a nursing home. SARS-CoV-2 antibody testing at that time became available in Belgium and revealed specific IgG in our patient.
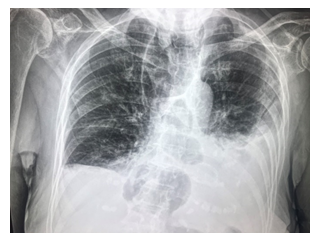
Figure 1: CXR showing extensive left lower lobe involvement and bilateral pleural effusion on day 18 after symptom onset, despite empirical treatment with three different antibiotics.
3. Discussion
This 94-year-old community-dwelling lady developed cough and dyspnea 6 days after admission, in a context of new COVID-19 cases on the ward. Four NPS on days 1, 7, 12 and 19, obtained by three different medical teams, were negative. No other viral or bacterial pathogens were detected, nor was there improvement with different empirical antibiotics. Timing dependent sensitivity has been documented [4] indicating probabilities of negative RT-PCR in our patient of 0.4, 0.3, 0.5 and 0.7 respectively. This results in a cumulative probability of 0.04 or a cumulative sensitivity of our diagnostic testing of 96%. When antibody testing became authorized in Belgium, we confirmed COVID-19 by SARS-CoV-2 specific IgG antibodies in this patient. Serial testing thus was insufficient to detect the presence of COVID-19 through NPS. When clinical suspicion is high, a negative test should not be used to stop protective measures. Highly sensitive tests and detailed information about pre- and post-test probabilities in different settings are urgently needed, for clinical and political decision making.
Declaration of Conflicts of Interest
None.
Funding
None.
Declaration of Proxy Consent
Written informed consent for publication of their clinical details and clinical images was obtained from the proxy.
References
- Sethuraman N, Jeremiah SS, Ryo A. Interpreting Diagnostic Tests for SARS-CoV-2. JAMA 323 (2020): 2249-2251.
- Watson J, Whiting PF, Brush JE. Interpreting a covid-19 test result. BMJ 369 (2020): m1808.
- Woloshin S, Patel N, Kesselheim AS. False Negative Tests for SARS-CoV-2 Infection – Challenges and Implications. N Engl J Med (2020).
- Kucirka LM, Lauer SA, Laeyendecker O, et al. Variation in False-Negative Rate of Reverse Transcriptase Polymerase Chain Reaction–Based SARS-CoV-2 Tests by Time Since Exposure. Ann Intern Med (2020): M20-1495.


 Impact Factor: * 5.3
Impact Factor: * 5.3 Acceptance Rate: 75.63%
Acceptance Rate: 75.63%  Time to first decision: 10.4 days
Time to first decision: 10.4 days  Time from article received to acceptance: 2-3 weeks
Time from article received to acceptance: 2-3 weeks 
